ACE Inhibitor Training
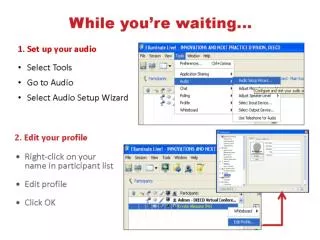
ALS PROTOCOL UPDATE EASTERN PA EMS COUNCIL PREPARED BY: DAVID K. VAN ALLEN, NREMT-P, FP-C BUREAU MANAGER, CITY OF ALLENTOWN PARAMEDICS JANUARY 2009. ACE Inhibitor Training. Captopril SL. Enalapril Injection.

ACE Inhibitor Training
E N D
Presentation Transcript
ALS PROTOCOL UPDATE EASTERN PA EMS COUNCIL PREPARED BY: DAVID K. VAN ALLEN, NREMT-P, FP-C BUREAU MANAGER, CITY OF ALLENTOWN PARAMEDICS JANUARY 2009 ACE Inhibitor Training Captopril SL Enalapril Injection
This training is not designed to replace the need of your service’s medical director to assure that you, the ALS practitioner, are trained to use this medication. This presentation is only an adjunct to other more complete training that is needed to ensure that you fully understand the uses, effects and contraindications of the medication discussed. The City of Allentown, the author, and the Eastern PA EMS Council assume no responsibility for the use or misuse of this material. All images are presumed to be free of copyright and the use of this material is strictly for non-commercial use. The author has allowed the use of this material on a free and unencumbered basis for educational purposes only as long as this message, the logo of City of Allentown, and proper citation of authorship is provided.
Objectives (focused to Congestive Heart Failure in the emergency setting) • Understand the gross epidemiology of Heart Failure • Review the basic pathophysiology of CHF • Become familiar with ACE Inhibitors • Plan a course of treatment based on BLS/ALS protocols • Interface with Medical Command through MedCom • Recognize and prepare for adverse side effects
Heart Failure Incidence and Prevalence ♥ Prevalence Worldwide – 22 million United States – 5 million ♥ Incidence Worldwide – 2 million new cases year United States – 500,000 new cases year ♥ Afflicts 10 out of every 1,000 people over age 65 in the United States (Stats from American Heart Association - 2002)
Define - Heart Failure: Heart failure, the inability of the circulatory system to meet the metabolic demands of the body. It is a multifaceted disease state involving several organs including the heart, kidney, vascular and respiratory systems - and there are several forms of heart failure with multiple etiologies. The treatment of chronic or acute heart failure is a particularly difficult therapeutic problem with no single drug or drug class adequate to provide complete relief from the symptoms of the disease. Sadly, regardless of the treatment, 50 % of individuals die within 5 years of developing CHF. In an era where morbidity and mortality from other cardiovascular diseases are decreasing, deaths from CHF are increasing. American College of Cardiology Web Site www.acc.org
Our local elderly population is higher than in some other areas. This means that we as paramedics will encounter a patient in some stage of heart failure more frequently – and often when they are experiencing emergent acute failure symptoms.
Heart Failure is caused by: • Narrowing of the coronary arteries (coronary artery disease) • Heart attack • Heart valve damage • High blood pressure • Disease of the heart muscle itself (cardiomyopathy) • Defects in the heart present at birth (congenital heart defects) • Infection of the heart valves and/or heart muscle itself (endocarditis and/or myocarditis). According to the AMERICAN HEART ASSOCIATION
Heart Failure is classified as: Class I Asymptomatic heart failureejection fraction (EF) <40% Class II Mild symptomatic heart failure with ordinary exertion Class III Moderate symptomatic heart failure with less than ordinary exertion Class IV Symptomatic heart failure at rest We often meet our patient’s when they are in Class IV heart failure!
In many cases, acute heart failure is associated with a hypertensive crisis. Correct the hypertension and you can often mitigate the emergent symptoms. Tip: CPAP works better with lowered pulmonary vascular pressures!
Fluid shift is a significant problem in the patient with acute Heart failure The acute phase of heart failure is almost always is associated with higher blood pressures resulting in fluid shift from the capillary vascular spaces to the surrounding interstitial tissue. Think of capillaries in your body as a screen door. There are holes that are big enough to naturally pass nutrients, oxygen and CO2 through the openings, but the holes are normally small enough to keep the formed elements of blood (red blood cells, etc) and plasma (90% water) from shifting out under normal pressure. It is easy to see that if you simply increase pressure, that water would pass right through!
Increased pressure in the capillaries can cause a shift of fluids into the limbs, hands, feet, toes and fingers, as well as the abdomen and lungs – depending on which side of the heart is failing!
Right sided failure vs. Left sided failure Partial failure of the right ventricle’s ability to eject its full load of blood leads to congestion of systemic capillaries. This is caused by increased venous blood pressure which pushes against the walls of small capillaries in the limbs. This excess pressure helps to generate excess fluid accumulation in the tissues of extremities by forcing plasma from the blood, past the walls of the capillaries and into the surrounding tissue. The lymphatic system becomes overwhelmed and cannot collect and remove the excess fluid. This causes swelling under the skin or peripheral edema and usually affects the dependent parts of the body first (causing foot and ankle swelling in people who are standing up, and sacral edema in people who are predominantly lying down). In progressively severe cases, ascites (fluid accumulation in the abdominal cavity causing swelling) and hepatomegaly (painful enlargement of the liver) may develop.
Right sided failure vs. Left sided failure Partial failure of the left ventricle’s ability to eject its full load of blood leads to congestion and high blood pressures in the pulmonary vasculature. The symptoms of left sided heart failure are therefore predominantly respiratory in nature. The patient will have dyspnea on exertion and in severe cases, dyspnea at rest. They may also experience breathlessness when lying flat, called orthopnea, or paroxysmal nocturnal dyspnea, which is a sudden nighttime attack of severe breathlessness. Just like in right side failure, the higher blood pressures (this time in the pulmonary circuit) cause water to leak through the capillaries surrounding the alveoli, which then fills them up reducing or stopping the ability to transfer oxygen and CO2 to the blood. This creates the sensation of trouble breathing that we so often see in these patients. Image shows enlarged heart and an significant accumulation of fluid in both lungs.
One of the goals in the emergency treatment of CHF is to reduce the systemic and therefore the pulmonary blood pressures to help get those ‘screen door’ capillary beds working correctly again. Reminder: Heart failure can affect both sides of the heart at the same time.
Nitroglycerin – Step One in reducing blood pressure. Nitro is used in the CHF patient when blood pressures are high to help bring those pressures down as quickly and as safely as possible. NTG primarily causes venous dilation which results in a reduction of pre-load to the heart. The reduction in preload helps to reduce venous return pressures to the heart and can help to lower systemic blood pressure. This helps with our ‘screen-door’ effect, and reduces workload of the heart. To be effective in the patient presenting with acute heart failure, the dosing of NTG may need to be aggressive and carefully monitored. (See PA State Protocol 5002-ALS)
ACE Inhibitors (a possible Command Only additional treatment) Recent research has shown that adding ACE Inhibitors to the emergent treatment of the patient in CHF may reduce mortality and morbidity by providing a second immediate mechanism to reduce blood pressure. ACEi does this by relaxing and dilating mainly the arterioles and thereby reducing cardiac ‘after-load’; allowing the heart to work against a lower systemic resistance. (Recall, NTG works mostly to reduce pre-load) Adding ACEi to the immediate treatment of a class IV heart failure patient may help lower blood pressure (one of the goals) and also lower the work of the heart. ACE Inhibitor therapy has a longer therapeutic life per dose, over medications such as NTG and has been a commonly used maintenance medication for patients in failure. Title: Effects of long-term enalapril therapy on left ventricular diastolic properties in patients with depressed ejection fraction. SOLVD Investigators.
ACE Inhibitors – How do they work? The renin-angiotensin-aldosterone system (RAAS) in the body plays an important role in regulating blood volume and systemic vascular resistance, which together influence cardiac output and mostly arterial pressures. As the name implies, there are three important components to this system: . renin . angiotensin . aldosterone. This system can be a potent vasoconstrictor – interrupt any portion of the system and you can cause vasodilatation and thus reduce systemic blood pressure.
The ACE inhibitor or angiotensin-converting enzyme inhibitor interrupts or blocks production of an enzyme (the ACE) that helps convert the protein angiotensin I into angiotensin II – A-II is a protein that makes blood vessels constrict and promotes retention of fluid, raising blood pressure. ACE inhibitors act to widen the blood vessels and make it easier for the heart to pump blood through the body. For a mini-review of the Renin-Angiotensin System (RAS) please see http://endo.endojournals.org/cgi/reprint/144/6/2179.pdf
Pharmacology of ACE Inhibitors • By blocking the ACE enzyme, ACE inhibitors decrease circulating levels of angiotensin II which decreases peripheral vascular resistance, and despite this fall in peripheral resistance, there is little effect on heart rate. • Drug names end in –’pril’ • Captopril • Lisinopril • Fosinopril • Quinapril • Enalapril PA State protocols allow pre-hospital use of only Captopril and Enalapril IMPORTANT! ACE INHIBITOR THERAPY IS NOT A FIRST LINE MEDICATION.
Pharmacology of ACE Inhibitors:Captopril (brand name Capoten) • First ACE Inhibitor developed for use in control of blood pressure • Widely used • Administered SL (per protocol) or PO (no IV preparations) • Dose 25mg SL – one time. • Best used for patients who are suffering hypertension with peripheral edema (right side heart failure) as the medication requires an adequate airway and moist mouth. • Onset via SL – within 5 minutes peaking in one hour. • Packaged as 12.5mg or 25mg tablets • NOT normally available in the ER for replacement. • Required to carry at least 50mg on ALS ambulances.
Pharmacology of ACE Inhibitors:Enalapril - ENALAPRILAT INJECTION (brand name Vasotec) • Second generation ACE inhibitor • Also widely used • Administered IV (per protocol) or PO • Dose 0.625mg – 1.25mg – one time. • Slow IV push – followed by flush. • Best used for patients who are suffering hypertension with pulmonary edema (left side heart failure). • Onset via IV – actions begin almost immediately peaking in 30 minutes • Packaged as 1.25mg per ml in vials of 1ml or 2ml • Normally available in the ER for replacement. • Required to carry at least 2.5mg on ALS ambulances.
Cautions of ACE Inhibitor use • Use may cause: • Hypotension (quickly in sodium or volume depleted patients) – report diuretic use, renal insufficiencies or dialysis to medical command. Starting doses for patients on diuretics is usually 0.625mg. Be prepared to provide careful fluid bolus should hypotension occur while assessing for pulmonary edema. • Angioedema (rare, but in the event of anaphylactoid response, treat with SQ Epi 1:1000) • Syncope • Cough
Contraindications of ACE Inhibitor use ACE Inhibitors are contraindicated in patients who are hypersensitive to any component of the product and in patients with a history of angioedema related to previous treatment with an angiotensin converting enzyme inhibitor and in patients with hereditary or idiopathic angioedema.
Treatment of the acute CHF patient • First do a complete assessment and uncover the medical history of the patient. • Follow PA State Protocol 5002 – ALS • Position patient for ease of breathing – usually Fowler’s • Provide high flow oxygen while assessing for edema. • Frequent repeat assessments of lung sounds are needed • If blood pressure is elevated, begin NTG treatment per protocol • Provide CPAP for those patients who qualify for the treatment • Contact Medical Command through MedCom and provide report and ETA. Advise Medical Command that you have the option of administering either Captopril SL or Enalapril IV at their discretion • Monitor airway and cardiovascular systems constantly • Rapid but safe transport to appropriate facility
Always be ready to adjust your treatments to take care of adverse condition changes. The patient in class IV heart failure is at risk for cardiac arrest. Johnny says: “You must be on your game”