Facial Trauma
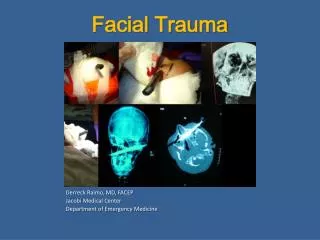
Facial Trauma. Derreck Raimo, MD, FACEP Jacobi Medical Center Department of Emergency Medicine. Anatomy of the eye. Ocular Trauma. · Six e xtraocular m uscles are responsible for all ocular movement · Controlled by cranial nerves

Facial Trauma
E N D
Presentation Transcript
Facial Trauma Derreck Raimo, MD, FACEP Jacobi Medical Center Department of Emergency Medicine
Anatomy of the eye Ocular Trauma ·Six extraocular muscles are responsible for all ocular movement ·Controlled by cranial nerves ·Ocular motility can be impaired by restriction, denervation or trauma
Anatomy of the eye Ocular Trauma ·The conjunctiva, cornea, anterior chamber, iris, lens and ciliary body are referred to as the anterior segment ·The sclera is referred to as “the white of the eye” ·The body of the eye is referred to as the globe
Ophthalmologic exam ·Inspection ·Pupils ·Movement ·Acuity ·Anterior Chamber ·Visual Fields ·Fundoscopy
Subconjunctival Hemorrhage ·Conjunctival vessels are fragile and can rupture from minor trauma ·The blood is usually bright red and appears flat ·Painless ·Requires no treatment
Corneal Abrasion ·Abrasion of the corneal epithelium usually caused by direct trauma ·Very painful, tearing, foreign body sensation ·Can only be visualized using fluorescein dye under cobalt blue light
Corneal Foreign Body ·Patients complain of a foreign body sensation following an appropriate event ·Superficial FBs can be removed using a cotton applicator ·Imbedded FBs must be removed under magnification with a 25ga needle or eye spud ·Failure to remove metallic FBs in a timely fashion may result in a rust ring
Hyphema ·Any injury to the anterior chamber can disrupt the vasculature supplying the iris or ciliary body ·Can cause pain, blurry vision and photophobia ·Initial treatment is aimed at preventing further bleeding ·Have the patient rest in the supine position with the head slightly elevated ·Use a rigid eye shield when possible
Chemical Injury ·True ocular emergency ·Identify exposure agent if possible ·Immediate copious irrigation with normal saline should not be delayed ·Can use a Morgan Lens or a liter bag of NS attached to a nasal cannula ·Alkali exposure (lye, ammonia) is worse than acid, but both can be blinding
Cyanoacrylate ·Super glue, “Crazy Glue” or Dermabond ·Accidental application to the eye is common, especially in children ·Can adhere lids together and forms clumps on the cornea or sclera ·Glue can be moistened and removed using Erythromycin ointment
Globe Rupture ·Commonly caused by penetrating trauma, but can also occur by blunt mechanisms ·Suspect when a large FB protrudes from near the globe ·Such objects should be left in place ·Avoid any manipulation of the globe, apply a rigid shield if possible ·Diagnosis suspected with teardrop shaped pupil, flattened anterior chamber or obvious aqueous humor leakage ·Diagnosis confirmed by Seidel Test
Globe Rupture Rigid Eye Shield Bulky Dressing
Traumatic Iridodialysis ·Trauma can pull the iris away from the ciliary body ·Patients complain of a “second pupil” ·Commonly associated with hyphema or lens dislocation ·No specific emergency treatment
Lens Dislocation ·Caused by a sudden blow to the globe ·Patient complains of double vision or gross blurry vision ·Must be surgically corrected
Dental Fractures ·Classified as Ellis class I, II, and III ·Class I involves the enamel only ·Class II involves the enamel and exposes underlying dentin ·Class III fractures extend into the pulp
Dental Fractures ·Ellis class I ·Involves the enamel only ·Treat pain and any underlying lacerations ·Predominantly cosmetic issue
Dental Fractures ·Ellis class 2 ·Deep enamel disruption exposes dentin ·Pulp can become infected over time ·Gauze dressing placed over tooth can ease pain if the nerve is exposed and help prevent infection
Dental Fractures ·Ellis class 3 ·Dental Emergency ·Delay in treatment by dentist can result in severe pain and abscess formation ·Noticeable pink or bloody discoloration on the fracture surface is diagnostic
Dental Subluxation ·Loosening of a tooth in its alveolar bone socket ·Unstable teeth can be temporarily immobilized with ·Gauze ·Suture material in a figure eight around adjacent tooth ·Aluminum foil ·Periodontal dressing
Dental Avulsion ·Total displacement of tooth from its socket ·Involves complete disruption of the periodontal ligament ·Successful implantation depends on the survival of periodontal ligament fibers ·Rinse tooth with saline but do not scrub ·Store in Hank’s Solution if possible if not Patients mouth > container of milk > normal saline ·Do not use water to store tooth
Nasal Trauma ·Commonly results in epistaxis ·Hold continuous pressure to soft portion of nose ·Homemade or commercial clips can be handy ·Anterior bleeds are most common ·Posterior bleeds can be life threatening
Septal Hematoma ·Uncommon complication of direct trauma to nose ·Blood accumulates between mucosal skin and underlying cartilage ·The resulting pressure on septal cartilage can lead to necrosis and deformity ·Must be drained by a surgeon
Cranial Trauma ·The scalp is comprised of 5 layers. Skin, subcutaneous tissue, galea, areolar tissue and pericranium ·The skull is comprised of eight major bones ·The scalp’s rich vascular supply causes a potential for severe blood loss from seemingly minor lacerations ·Skull fractures are classified as either basilar or of the skull convexity
Basilar Skull Fracture ·The most common type involves the temporal bone ·Commonly associated with a tear in the dura leading to a CSF leak ·Classic signs and symptoms are often absent on initial presentation but will develop gradually over the first hours of evaluation ·Raccoon Eyes are caused by bleeding from a fracture site in the anterior portion of the skull base
Basilar Skull Fracture Battle’s Sign Hemotympanum
Depressed Skull Fracture ·Commonly occurs when a large force is applied to a small area ·Classified as an open fracture if fracture lies below or near a laceration ·Wound must be explored and manipulated in a sterile fashion
Frontal Bone Fracture ·All frontal lacerations must be explored to rule out an underlying fracture ·A fracture will involve the frontal sinus ·May be part of a complex of facial fractures involving other sinuses
Maxillofacial Trauma ·Sutures at the borders of the sphenoid bone, pterygoid plate and zygomatic arch anchor the face to the skull ·The orbit consists of 7 different bones ·Orbital bones lie in close proximity to extraocular muscles, vessels and cranial nerves
Maxillofacial Trauma ·Prehospital care should concentrate on control of the airway ·Always maintain c-spine precautions ·The mouth should be cleared of any obvious debris and suctioned as needed ·Severe mandibular fractures may prevent a jaw thrust from clearing the tongue from airway, necessitating manual extraction of the tongue with a gauze pad, towel, clamp, or even a suture through the anterior tongue ·Early emergency department notification helps us to prepare
Maxillofacial Trauma ·Avoid nasotracheal intubation in patients with midface trauma because the cribiform plate may be disrupted ·Orotracheal intubations are often successful even with distorted facial anatomy ·It may be impossible to obtain an adequate seal with a BVM ·Laryngeal mask airway can be considered in a difficult airway ·When possible prepare for a surgical airway while attempting intubation ·Control bleeding with direct pressure ·Severe pharyngeal bleeding may require packing of the pharynx above a cuffed ET tube ·In LeFort fractures manual reduction may be needed to control bleeding
Maxillary Fractures ·An impact 100 times the force of gravity is required to break the midface ·Classified as LeFort fractures ·LeFort I fractures involve only the area under the nasal fossa ·LeFort II fractures involve a pyramidal area including the maxilla zygoma, nasal and ethmoid bones ·LeFort III fractures are known as craniofacial disassociation and involve the frontozygomatic suture at the base of the skull
Maxillary Fractures ·Clinically a patient will have significant facial swelling and ecchymosis ·Associated cranial injuries are common ·Airway protection ·Hemorrhage control ·Cervical immobilization
Zygoma Fractures ·Visual inspection from several angles may detect a subtle deformity ·Can be associated with orbital fractures and ocular trauma
Orbital Fracture ·Occurs when the globe sustains a direct blunt force ·In a true orbital blowout fracture this force is transmitted to the thin bones of the orbital floor resulting in a fracture ·May result in entrapment of extraocular muscles if they herniate through the fracture ·Fractures without entrapment or associated globe injury are treated conservatively
Mandibular Fracture ·Results in malocclusion or irregular contact between upper and lower teeth when mouth is closed ·A non fractured mandible should be able to hold a tongue blade between the molars tightly enough to break it off ·A unilateral condylar fracture will deviate the jaw towards the side of the fracture upon maximal opening
TMJ Dislocation ·Temporal Mandibular Joint ·Can result from direct trauma to chin while mouth is open ·Can occur in predisposed individuals during a vigorous yawn, eating or laughing ·Approximately 70% of the population can partially subluxate then spontaneously reduce the mandible
References ·Tintinalli, J., Kelen, G. D., Stapczynski, J. S. Emergency Medicine a Comprehensive Study Guide. 5th Ed. McGraw-Hill, 1985. ·Marx, J. A., et al. Rosen’s Emergency Medicine Concepts and Clinical Practice. 5th Ed. Mosby, 1998 ·Knoop, K. J., Stack, L. B., Storrow, A. B. Atlas of Emergency Medicine. 2nd Ed. McGraw-Hill, 2002