Renal Insufficiency
Renal Insufficiency. Department of Pathophysiology, Shandong University School of Medicine 薛冰. INDEX. Acute renal failure(ARF) Chronic renal failure(CRF). Functions of the Kidney. 1.Excretion. Remove waste product from the body ; Regulate electrolyte and acid-base balance.

Renal Insufficiency
E N D
Presentation Transcript
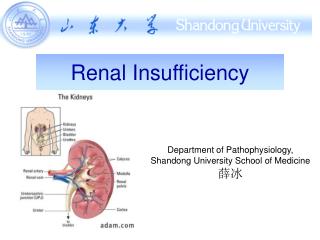
Renal Insufficiency Department of Pathophysiology, Shandong University School of Medicine 薛冰
INDEX • Acute renal failure(ARF) • Chronic renal failure(CRF)
Functions of the Kidney 1.Excretion Remove waste product from the body; Regulate electrolyte and acid-base balance. 2. Endocrine Produce renin、EPO、and prostaglandins Active VitD3 Inactivate gastrin、PTH.
Renal insufficiency Dysfunction of excretion and endocrine Diseases Symptoms and signs Edema, hypertension, oliguria, polyuria, proteinuria, anemia, osteodystrophy.
Causes 1. Primary renal diseases Primary glomerular diseases, Primarytubulardiseases, Interstitial nephritis, et al. 2. Secondary renal lesion Circulatory system diseases, immunity diseases, metabolic diseases, hematopathy(血液病), et al.
Definition Etiology & classification Pathogenesis Alteration of Metabolism and Function Prevention & Treatment Part I Acute Renal Failure(ARF)
I Definition • Acute renal failure (ARF) is defined as a precipitous and significant (>50%) decrease in glomerular filtration rate (GFR) over a period of hours to days, with an accompanying accumulation of nitrogenous wastes in the body. water intoxication, azotemia, hyperkalemia, metabolic acidosis
Morbidity and mortality • 急性肾衰竭迄今为止仍是威胁人类生命的危重病症,第二次世界大战时其死亡率高达91%,越南战争时期由于透析技术的应用,其死亡率降为68%。近年来单纯急性肾衰竭的死亡率为7%~23%,而复杂性急性肾衰竭的死亡率仍高达50%~80%。急性肾衰竭的死亡率取决于原发病的严重程度,以往的研究表明,急性肾衰竭的病因不同,其死亡率有明显差别,如缺血性原因者死亡率为30%,而中毒性原因者死亡率仅为10% .
II Etiology and Classifications 1.causes Prerenal ~ Intrarenal ~ Postrenal ~ 2. urine volume Oliguric ~ (<400ml/day) Nonoliguric ~ (>400ml/day) 3. renal lesion functional~ organic ~ obstructive ~
adrenal gland renal pelvis ureter urinary bladder Causes and classification • Pre-renal (~70% of cases) functional renal failure; prerenal azotemia • Intra-renal (~25% of cases) parenchymal renal failure • Post-renal (<5% of cases) postrenal azotemia
Cause and classification (I) Prerenal failure - Diseases that compromise renal perfusion • Decreased effective arterial blood volume - Hypovolemia (ECF↓ 50% → RBF ↓ 90-95%) Congestive heart failure (CO ↓ 40 % → RBF ↓ 72 %) sepsis (vasodilatation)
pathogenesis of pre-renal ARF pre-renal factors shock caused by haemorrhage 、infection、AHF、 serious anaphylactic reaction and others (hepatorenal syndrome ) ADHeffective blood volume Ald BP decrease kidney perfusionrenal blood vessel contraction renal blood flow Glomerular EFP GFR urine
Characteristics of prerenal ARF (A)Decreased perfusion without cellular injury (B) Intact renal tubular and glomerular functions (C)Reversible if underlying cause is corrected in time. ( Hypovolemia, Renal hypoperfusion, Hypotension) • early stage: functional~ late stage: organic ~ (D) Characteristics of urine: oliguria, specific gravity , sodium , urinary sediment(-)
Cause and classification • (II) Intrarenal failure - Diseases of the renal parenchyma(肾实质), specifically involving the renal tubules, glomeruli, interstitium • Vascular diseases • Interstitial diseases • Acute glomerulonephritis • Diseases in tubules Acute tubular necrosis (ATN)
Diseases in tubules:Acute tubular necrosis (ATN)(80%) ■Long time of renal ischaemia shock, dehydration, hemorrhage denaturalization ■Renal poisoning: Extrinsic:chemical agents (carbon tetrachloride四氯化碳) heavy metals (mercury水银) X-ray contrast medium biological toxin :some mushroom, snake venomsdrugs : sulfonamides磺胺药物, kanamycin卡那霉素 Intrinsic:hemoglobin, myoglobin,uric acid
Difference between pre-renal and intrarenal ARF Pre-renal Intra-renal Urine specific gravity > 1.020 < 1.015 Urine osmotic pressure(mmol/L) > 500 < 350 Urine sodium(mmol/L) < 20 > 40 Ucr/Scr > 40:1 < 20:1 Urinary sediment(±) (+) Urine protein (-) +~++++ Mannitol testurine volume urine volume(-)
renal pelvis ureter urinary bladder Cause and classification • (III) Postrenal failure - Diseases causing urinary obstruction from the level of the renal tubules to the urethra • Tubular obstruction from crystals • Ureteral(输尿管) obstruction
Characters of Post-renal ARF 1) intact renal tubular and glomerular functions 2) reversible if underlying cause is corrected in time (To rule out the obstruction quickly is very important.)
III Pathogenesis of ARF Most of the manifestations of ARF are caused by the decreased urine volume. Waste substance↑ The basic pathogenesis of ARF is to explain the reasons of decreased urine volume.
efferent arteriol • GFR and tubular reabsorption are the main factors to determine the urine volume. • Glomerular-tubular balance • 1% excrete • Decreased GFR and increased reabsorption in tubule will lead to decreased urine volume. GFR
Pathogenesis of ARF(induced by ATN) (I) Changes of renal hemodynamics (effects on glomerular function) (II) Effects of tubular injury (III) Glomerular Kf↓
(I) Changes of renal hemodynamics 1 Decreased renal blood flow
Renal blood flow: 20%~30% of cardiac output(1200 ml/min). Inferior vena cava Adrenalgland Kidney Aorta Ureter Bladder Urethra
10 out 18 in Blood hydrostatic pressure(BHP) 60 mmHg out Colloid osmotic pressure(COP) -32 mmHg in Capsular pressure(CP) -18 mmHg in Net filtration pressure(NFP) 10 mmHg out Net Filtration Pressure 60 out BHP 32 in COP NFP CP
1)Decreased renal blood presure (A)Decreased systemic pressure (B)Increased tubular pressure • Systemic BP<80mmHg • Renal artery BP is decreased Obstruction of urinary tract Glomerular hydrostatic pressure is decreased Increased Bowman’s capsule pressure Glomerular effective filtration pressure is decreased Decreased urine volume Glomerular hydrostatic pressure Glomerular colloidosmotic pressure efferent arteriole Afferent arteriole Bowman’s capsule pressure
BP < 80mmHg CO RBF BP (50-70mmHg) GFR (1/2 – 2/3) BP(40mmHg) GFR = 0
2) Renal vasoconstriction (A)Increased activity of sympathetic system Shock and trauma (low CO) Baroreceptor in aortic arch and carotid sinus Increased activity in sympathetic system Contraction of renal artery Constriction of afferent arteriole RBF decrease Decreased urine volume
(B)Increased activity of renin-angiotension system Ischemia and poisoning Low renal artery pressure Injury of proximal tubule and reduced Na+ reabsorption Increased Na+ in the distal tubule stimulate the Macula densa Stimulate the release of renin from the juxtaglomerular apparatus Constriction of afferent artery(AII) Decreased GFR
(C) unbalance of endothelin and NO Injury of endothelium of renal vessels by hypoxia, acidosis Constriction of afferent arteriole Increased synthesis and release of endothelin decreased synthesis and release of NO Decreased effective filtration pressure and GFR Decreased urine volume
(D) Decreased production of vasodilatory prostaglandins (PGE2) • Kidney is the main organ to produce PGE2. • The role of PGE2 is dilating blood vessels. • The production of PGE2 is reduced before the development of ARI caused by gentamycin(庆大霉素)poisoning.
3)Renal vessel obstructionA swelling of endothelial cell ischemia Na+ - K+ - ATPase Renal toxic substances cell membrane permeability calcium pump dysfunction free radical endothelial cellular injury B microthrombus formation in renal vessel Cell edema Calcium overload
(I) Changes of renal hemodynamics 2. Renal blood flow re-distribution renal cortex ischemia GFR renal medulla hyperemia Renal tubular injury
(II) Renal tubular injury • 1 Morphologic changes • ①morphologic change
Red blood Cell Cast Muddy Brown Cast White blood Cell Casts
② character of renaltubule cell damage A.Necrotic lesion tubulorrhexis lesion( renal poisoning and renal ischemia persistently ) :involve all renal tubule,especially loop of Henle. focal necrosis of nephron, epithelial cell necrosis basement membrane is destroyed nephrotoxic lesion (Renal poisoning): involve proximal tubule, all Nephron damage , epithelial cells necrosis, basement membrane is integrity B.Apoptotic lesion: distal tubule
细胞损伤机制(了解) 缺血、中毒 ADP、毒物 OFR生成↑ 清除↓ GSH ↓ ATP ↓ Na+、K+-ATP酶↓Ca2+-ATP酶↓ 线粒体Ca2+↑ 细胞内钠水潴留 胞浆内游离钙↑ 磷脂酶活性↑ 细胞内Ca2+超载 PGs、LTs 细胞水肿 脂质过氧化 细胞损伤 (坏死;凋亡)
2 Effect of tubular injury 1)Tubule obstruction 2)Loss of tubule integrity: initial urine back-leakage
1)Tubule obstruction Reduced urine volume Long time of renal ischemia Renal poisoning Injury of proximal tubule cells ( necrosis) Detach from basement membrane and slough into the tubule lumen and become impacted (tube cast) Tubule obstruction Increase Bowman’s capsule pressure
Denuded tubular membrane Injured tubular cells Obstruction from debris and necrotic cells Urine flow
②Loss of tubule integrity (passive back-leakage) Severe ischemia and poisoning of tubule Epithelial cell necrosis and loss of tubule integrity (become leaky) Back leaking of urine to peritubular interstitial space high interstitial pressure Press the tubule Press blood vessels ↑ intratubular pressure ↓ RBF Decreased urine volume
(III) Glomerular Kf↓ Glomerular lesion filtration surface area Glomerular permselectivity GFR 43
IV Clinical Course and manifestation Two types of ARF: oliguric(<400ml/d) ARF nonoliguric (>400ml/d) ARF.
Clinical Course and manifestation 1 Oliguric phase(days~weeks) Manifestations: a) changes of urine b) azotemia c) metabolic acidosis d) hyperkalemia e) Water intoxication (I) oliguric ARF
A changes of urine (a) reduced urine volume: less than 400 ml /24h (oliguria) less than 100 ml/24h (anuria) Mechanism:RBF decrease, renal tubule obstruction and urine back-leakage (b) urine sediment investigation: In prerenal ARF: (- or +?) In ATN: (+) contain : RBC, WBC, epithelial cells and casts
(c) specific gravity and osmolality: ATN: Low specific gravity =1.010~1.015 (N:1.015-1.025) Osmolality of urine = or < plasma Cause: The ability of concentration and dilution is lost in ATN. Pre-renal AFR:
(d) urinary Na+ concentration: In pre-renal ARF with normal reabsorption of tubule, urine [Na+] <20 mmol/L In ATN, urine [Na+] >40 mmol/L Actually, during oliguria, the amount of sodium entering Bowman’s capsule is decreased, the [Na+] in urine is elevated because of deficient tubular reabsorption of sodium.
Hypervolemic hyponatremia Fluid retention Cell edema B Water intoxication (Hypotonic hypervolemia, dilutional hyponatremia ) Causes: (a) oliguria with more water intake (b) increased production of metabolic water (catabolism) (c) Transfuse fluid↑
C Azotemia (NPN>40 mg/dl) (a) Concept of azotemia: increased concentration of nonprotein nitrogens (NPN) in the blood. (normal: 20~35 mg/dl) The nonproteins include urea, uric acid, creatinine etc. (b) Reasons : a) oliguria b) increased catabolismof proteins.