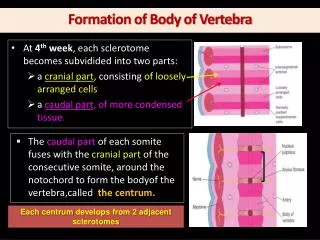
Managing Interferon-Induced Lung Disease in Melanoma Treatment
Interferon alfa therapy, commonly used as an adjuvant treatment for melanoma, can induce significant complications, including interstitial lung disease (ILD). This case study presents an 80-year-old male patient who developed symptoms of dyspnea and fever post-therapy, raising suspicion for IFN-induced ILD. Despite negative infectious and autoimmune work-ups, clinical deterioration persisted until discontinuation of interferon therapy led to improvement. It highlights the importance of recognizing ILD as a serious, albeit rare, complication of interferon therapy in melanoma management.

Managing Interferon-Induced Lung Disease in Melanoma Treatment
E N D
Presentation Transcript
When the treatment becomes the problem Sonia M. CastilloMD Mark Hamblin MD, FCCP Department of Internal Medicine University of Kansas Medical Center, Kansas City
Background • Melanoma: 5th most prevalent cancer1 • First line treatment: local excision • Interferon (IFN)alfa therapy: indicated as adjuvant treatment2 • Kim KB, Davies MA, Rapini RP, Hwu P, Bedikian AY. Chapter 39. Malignant Melanoma. In: Kantarjian HM, Wolff RA, Koller CA, eds. The MD Anderson Manual of Medical Oncology. 2nd ed. New York: McGraw-Hill; 2011. • Ascierto PA, Gogas HJ, Grob JJ et al. Adjuvant interferon alfa in malignant melanoma: an interdisciplinary and multinational expert review. Critial Reviews in Oncology/Hematology. 2013;85:149-161
Case presentation 80 year old male with malignant melanoma • 09/2011 Shave biopsy of scalp lesion • 11/2011 Excision and nodal dissection • 01/2012 Peginterferonalpha 2b • 12/2012 Shortness of breath for 6 weeks
Past Medical History • Malignant Melanoma • Hypertension Social History • Nonsmoker • No pets • No sick contacts Medications • Peginteron alfa-2b • Amlodipine
Physical exam Temp=38.2C HR=102 BP=122/58 RR=24 SO2=88% on room air • General: Well-developed male in mild respiratory distress • Cardiovascular: Tachycardic • Respiratory: Bibasilar fine crackles • Extremities: no clubbing
Initial laboratory testing • White blood cell count: 6.2 • Neutrophils: 54% • Lymphocytes: 34% • Monocytes: 12% • Arterial blood gas: 7.49/30/55/23 • B-type natriuretic peptide: 39
Chest CT Angiography Apices Mid-lung fields Lung bases
Infectious work-up • Bacterial and AFB smear and culture • Legionella urine antigen • Mycoplasma IgG and IgM • Aspergillus galactomannan • Fungitell • Histoplasma and coccidioides urine antigens • Cryptococcal serum antigen • Respiratory viral panel Negative
Autoimmune work-up • ANA • C-ANCA, P-ANCA • Anti GBM Antibody Negative
Bronchoalveolar lavage • Cell count: • Red blood cells: 1450/uL • White blood cells: 360/uL • Monocytes: 55% (Normal>85%1) • Lymphocytes: 29% (Normal=10-15%1) • Neutrophils: 16% (Normal<3%1) • Other studies: • Bacterial, mycobacterial and fungal stain and culture • Respiratory viral panel • PJP PCR • Cytology NEGATIVE 1. Meyer K, Raghu G, Baughman R et al. An Official American Thoracic Society Clinical Practice Guideline: The Clinical Utility of BronchoalveolarLavage Cellular Analysis in Interstitial Lung Disease. Am J Respir Crit Care Med Vol 185, Iss. 9, pp 1004–1014, May 1, 2012
Hospital course • Antibiotics and trial of diuresis • Non-invasive positive pressure ventilation • Unrevealing infectious work-up • Methylprednisolone 125mg IV q6hrs • No response • Discontinuation of antibiotics Clinical improvement
Follow-up CT chest 2 months later
Discussion Why did we suspect IFN-induced interstitial lung disease (ILD) on this patient? • Negative work-upfor infectious, autoimmune and malignant processes • Findings on Chest CT • Lymphocytosis on BAL cell count • Clinical deterioration despite empiric antibiotics
IFN-inducedILD • Uncommon complication (0.01-0.3%)1 • Presenting symptoms:dyspnea, dry cough,fever, fatigue, anorexia, myalgias2 • Average time of presentation: 12 weeks • Solsky J, Liu J, Peng M, Schaerer M, Tietz A. Rate of interstitial pneumonitis among hepatitis virus C infected patients treated with pegylated infeterferon. J Hepatol. 2009; 50 Suppl 1: S238. • Ji FP, Li ZX, Deng H et al. Diagnosis and management of interstitial pneumonitis associated with interferon therapy for chronic hepatitis C. World Journal of Gastroenterology. 2010;16(35):4394.
Diagnosis of IFN-induced ILD1 • Exclusion of other etiologies • Compatible chest CT • Lymphocytosis on BAL cell count • Resolution of symptoms and infiltrates after cessation of therapy 1. Ji F-P. Diagnosis and management of interstitial pneumonitis associated with interferon therapy for chronic hepatitis C. World Journal of Gastroenterology. 2010;16(35):4394.
Treatment of IFN-induced ILD • Discontinuation of IFN • Corticosteroids1 • Puente Vazquez J, Moreno Anton F, Grande Pulido E, Lopez Tarruella-Cobo S, Perez Segura P, Diaz-Rubio E. Interstitial pneumonitis and lung fibrosis during adjuvant treatment of melanoma with interferon alpha according to the Kirkwood schedule. Dermatology. 2005;210(3):247-249.
Key points IFN-induced Interstitial Lung Disease: • Uncommon complication of IFN-alfa 2b therapy, but potentially life threatening • Should be a diagnosis of exclusion
Acknowledgements • Mark Hamblin MD, FCCP Division of Pulmonary and Critical Care Department of Internal Medicine University of Kansas Medical Center, Kansas City, Kansas • Gary DoolittleMD Division of Hematology and Oncology Department of Internal Medicine University of Kansas Medical Center, Kansas City, Kansas
Questions? Thank you!
IFN-related pulmonary toxicity • Interstitial pneumonitis • BOOP • ARDS • Pleural effusion • Asthma exacerbation
Cases with other malignancies • Melanoma. Puente Vasquez et al. Dermatology 2005 • Hemangioendotelioma. Wolf et al. Clinical Toxicology 1997 • CML. Yufu et al. American Journal of Hematology 1994