Align Networks
Align Networks. Physical Therapy Management Strategies November 15, 2011 Presented by: Nicole Matoushek, MPH, PT V.P. Product Development & Matt Dougherty, V.P. Sales. Align Networks Physical Therapy Program. Align Networks Program.

Align Networks
E N D
Presentation Transcript
Align Networks Physical Therapy Management Strategies November 15, 2011 Presented by: Nicole Matoushek, MPH, PT V.P. Product Development & Matt Dougherty, V.P. Sales
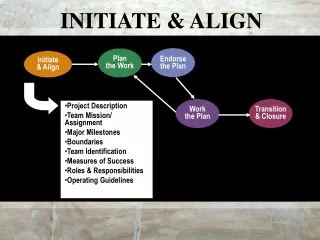
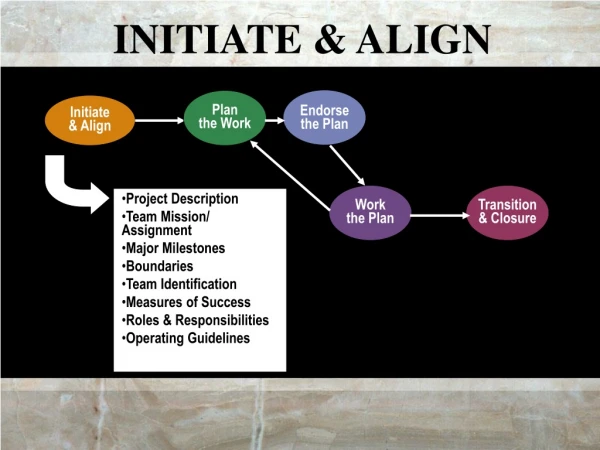
Align Networks Program Align Networks is the premier provider of physical rehabilitation services in the Workers’ Compensation industry • National network of credentialed providers • Scheduling • Visit management • Clinical oversight • EDI • Online web portal for real time claim access & easy billing
Align Networks Philosophy Align Networks believes that the front end management of the claim is necessary to deliver optimal clinical outcomes & cost savings in both our prospective and retrospective models Our philosophy has demonstrated success due to our ability to positively impact: • Clinical Outcomes • Customer Service • Provider Selection • Customer, Patient, Physician & Provider Satisfaction
Services Offered Nationally • Physical/ Occupational Therapy (75% of referrals) • Chiropractic • Industrial Rehab Services • Functional Capacity Evaluations • Work Conditioning / Hardening • Onsite Therapy Program • Job Site / Ergonomic Evaluation • Specialty Rehab Services • Certified Hand Therapy • Aquatic Therapy • Non-traditional services – massage, acupuncture, speech, vestibular therapy, wound care, gym/fitness
Most Frequent Injury Types Musculoskeletal Disorders! • MSDs represent 62% of all Workers’ Compensation claims (OSHA) • Most common: sprains, strains, CTS, fractures, contusions Ref: BLS, 2005
Musculoskeletal Disorders WHY is understanding WHAT & HOW of workplace injuries important? • MSDs are EXPENSIVE! • MSD: $20B in lost work time, W.C. Costs every year • Expected to rise to $54B in next 10 years • Indirect costs associated with every dollar spent on direct costs $3.70 $1.00 for every Direct: medical/ pharmaceutical costs Indirect: lost due to decreased productivity and absenteeism
Top 5 Leading Causes of Workplace Injuries Ref: Liberty Mutual Work Safety Index
Ergonomic Related Injuries Clinically, ergonomic work-related injuries occur when there is inadequate blood flow or tissue recovery time due to work cycles or exposure to ergonomic risk factors • Tissue damage can lead to inflammation, degeneration, loss of function (ROM, Strength), impairment, disability • Injuries: Overexertion, Repetitive Strain, Cumulative Trauma • Occurs over time with repeated exposure
What is Ergonomics? • Ergonomics: the “Science of Work” • Latin “Ergos” = work, “nomics” = science/study • Presence of one or more ergonomic risk factor can lead to an increased risk of acute & cumulative trauma injury
What are Risk Factors? A risk factor is any exposure that increases the probability of the occurrence of injury Increase an ergonomic risk factors is a multiplicative effect, not additive!
Ergonomic Risk Factors: Industrial Example: Awkward posture, repetition, sustained postures, gloves Material Handling Risk Factors: • Forceful Exertion • High Repetition • Awkward Postures & working outside of “optimal” or neutral joint postures • Sustained Postures • Contact Stress • PPE/Gloves: Increase grip needed by10% • Shift work/schedules/OT
Ergonomic Risk Factors: Office Risk Factors: • Not just in the industrial setting, they exist in the office setting too! • Common office risk factors: • Awkward positions • Static postures • High repetition/keying • Trip hazards: chair mats, electrical cords
Let’s Look At A Risk Factor Awkward Postures: Grip Strength: • Neutral joint posture= least amount of stress on tendons, ligaments and joints. Also strongest. • Loss of strength of 50% or more when working out of neutral. • Injury risk goes up!
Physical Therapy Management Strategies “You do not get injured workers well to put them back to work. You put them back to work to get them well.” - Richard Pimenthal
Pro-Active Therapy • Develop goals, treatments based on individual needs • Inherent flexibility of treatment plan • 3 x 4 weeks 1-3 x 2-4 weeks • Avoid “prescriptive care” mentality • Not all patients require exact same treatment! • Evaluate function, progress regularly (30 Days) • Modify goals, treatment as needed • Communicate findings regularly • Ensure Patient Responsibility • Involve IW, review goals with IW
Focus on Function • Include functional activities • Document objective progress • Passive treatments/modalities should be limited and used only as an adjunct to active exercise (APTA position)
Work-Specific Treatments • Goals should be objective, measurable • Focus on RTW objective • Include work-specific activities • Real tasks, tools or simulated • Refer to job description if available (Adj/Case Manager) • Job Description • Job Goal
Visit Monitoring Monitor entire episode of care; I.E.; visits attended/missed; guidelines; discharge; outcomes metrics Review patient’s RTW/SAW status & appropriateness for specialty Industrial Rehab services: • Functional Capacity Evaluation • Work Hardening/Conditioning • Ergonomic Services
Clinical Guidelines Extended durations above Clinical Guidelines may be appropriate, review clinical/patient documentation: • ODG, ACOEM, State Guideline, APTA, Other • Slower healing: advanced age, metabolic disorder, meds affect mobility/exercise tolerance • Higher surgery rates (multiple) • Co-morbidities/complications • Scarring, overweight, de-conditioned
Proactive D/Cs • APTA Definitions: Discharge vs. Discontinuation • Identify I.W.s who no longer require hands-on skilled care • Continue to improve independently? • Perform HEP independently? Gym program? • Recommend D/C of therapy services as appropriate (APTA) • Communicate with Physician/CM/Adjuster
P.T. Management Programs • Aggressive scheduling & visit management for entire episode of care; prompt I.E. & regular attendance facilitates healing, RTW & discourages counterproductive behaviors • Steerage to preferred provider based on location, services, & performance; ensures optimal outcomes • Clinical Oversight program; ensures delivery of medically necessary care; Clinical Guidelines, Peer to Peer Reviews • Industrial Rehab Specialization; identifies I.W.s eligibility for FCE/Ergonomics or WC/WH programs, maximize RTW/SAW • Data exchange: reporting & 24/7 online access for Payor; Adjuster/Case Manager; always up to date on therapy milestone updates, therapy progress & status, clinical findings, RX






![Poster Name [Align Center]](https://cdn1.slideserve.com/2804700/poster-name-align-center-dt.jpg)