Enterobacteriaceae
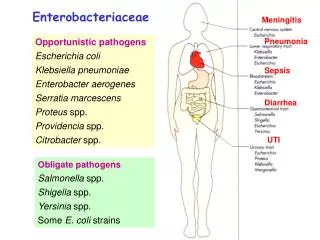
Enterobacteriaceae. Chapter 31. Introduction. “Enteric Bacteria” Gram-negative rods Ubiquitous Cause 30%-35% of all septicemias, more than 70% of UTIs, and many intestinal infections Pathogens: Normal flora – opportunistic infections Animal reservoirs Human carriers Box 31-1.

Enterobacteriaceae
E N D
Presentation Transcript
Enterobacteriaceae Chapter 31
Introduction • “Enteric Bacteria” • Gram-negative rods • Ubiquitous • Cause 30%-35% of all septicemias, more than 70% of UTIs, and many intestinal infections • Pathogens: • Normal flora – opportunistic infections • Animal reservoirs • Human carriers • Box 31-1
BOX 31-1. Common Medically Important Enterobacteriaceae • Citrobacter freundii, Citrobacter koseri • Enterobacter aerogenes, Enterobacter cloacae • Escherichia coli • Klebsiella pneumoniae, Klebsiella oxytoca • Morganella morganii • Proteus mirabilis, Proteus vulgaris • Salmonella enterica • Serratia marcescens • Shigellasonnei, Shigella flexneri • Yersinia pestis, Yersinia enterocolitica, Yersinia pseudotuberculosis
Physiology and Structure • Facultative anaerobes • Ferment glucose, are catalase positive, and oxidase negative • Lactose fermenting strains (e.g. Escherichia, Klebsiella, Enterobacter) • Non-lactose fermenting (e.g. Salmonella, Shigella, and Yersinia)
Differentiating Similar Strains Antigen detection • O polysaccharides • Part of LPS • Capsular K • Flagellar H proteins • E. coliO157:H7
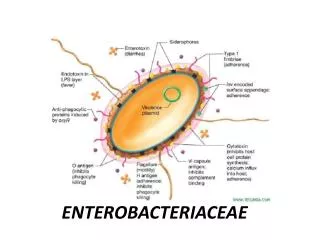
Pathogenesis and Immunity Common virulence factors • Endotoxin • Lipid A portion of LPS causes many of the systemic manifestations of infection • Capsule • Interferes with antibody binding • Capsular antigens are hydrophilic (phagocytic cell surface is hydrophobic) • Poor antigenicity • Antigenic phase variation • Capsular K and flagellar H antigens are under genetic control • Can be expressed or not expressed
Pathogenesis and Immunity • Sequestration of growth factors • Iron: Bacteria produce competitive siderophores or iron-chelating compounds, hemolysins
Escherichia coli Pathogenesis (Box 31-3) • Adhesins: Essential for colonization • Prevents the organism from being flushed out of the urinary or gastrointestinal tract • Exotoxins • Specific target tissue • Result in altered cell function or cell death
Epidemiology and Clinical Diseases • Many infections are endogenous (septicemia and UTI’s) • Septicemia-originate from UT or GI infections leading to intraabdominal infection • Neonatal meningitis, Intraabdominal infections • UTIs-originate in the colon -> contaminate urethra -> ascend into the bladder • Production of adhesins • ~80% of all community-acquired UTIs • Gastroenteritis-caused by five major groups • May include: watery diarrhea, abdominal cramps, fever, and vomiting • (Table 31-1)
Gastroenteritis (ETEC) • Estimated 80,000 cases in US travelers annually (650 million worldwide) • In small intestine; watery diarrhea, cramps, vomiting, fever • Occurs in developing countries usually in children or travelers (traveler’s diarrhea) • 1-2 day incubation, 3-4 duration • Infectious dose is high so person to person spread does not occur • Two classes of enterotoxins: heat-labile (LT-I, LT-II) and heat-stable (STa, STb) • LT-I increases secretion of chloride and inhibits absorption of sodium and chloride (the same as cholera toxin) • STa causes a hypersecretion of fluids • Both contributing to watery diarrhea • Disease similar to cholera, but milder
Gastroenteritis (ETEC) Imodium mode of action: http://en.wikipedia.org/wiki/Loperamide
Gastroenteritis (EHEC) • 73,000 cases with 60 deaths annually • In large intestine; vomiting, abdominal cramps, fever • Severity ranges from diarrhea to hemorrhagic colitis (bacterial dysentery) • 3-4 day incubation, 4-10 day duration • Infectious dose is less than 100 bacteria, O157:H7 serotype is the most common • Read text page 329 • Shiga toxins (Stx-1, Stx-2) • Bind to 28S rRNA and disrupt protein synthesis • Tissue destruction leads to the symptoms (bloody diarrhea)
Gastroenteritis (EHEC) • Spinach Outbreak Information • http://www.cdc.gov/mmwr/preview/mmwrhtml/mm55d926a1.htm • http://www.cfsan.fda.gov/~dms/spinacqa.html#howmany
Salmonella Characteristics • Similar to E. coli except no lactose fermentation • Historically there have been many different species (~2000) • All are really one species: • Salmonella enterica
Salmonella Virulence factors • Box 31-2 and 31-5 • Some bacteria can survive stomach acid • Able to enter M cells (peyer’s patches) • Cause cell death and spread to surrounding cells. • Figure
SalmonellaEpidemiology • Colonize virtually all animal species
Salmonella Diseases(Gastroenteritis) • Most common form of disease • 40,000 cases in the US in 2004 • Mostly spread by eating contaminated food (Poultry, eggs, dairy products) • Can be fecal-oral in children • Infectious dose 106 to 108 • Symptoms 6-48hrs after consumption nausea, vomiting, non-bloody diarrhea, fever, abdominal cramps • Usually ends without intervention in a week or less
Salmonella Diseases(Typhoid Fever) • Typhoid Fever • Human reservoir (person-to-person spread) • Pass through intestinal lining and engulfed by phagocytes • Replicate in liver, spleen, bone marrow • Cause fever, myalgia, gastroenteritis • Asymptomatic colonization (1-5% patients) • Story Time - “Typhoid Mary”
Salmonella Treatment • Preventative - safe food preparation • Antibiotics not recommended for enteritis • Typhoid Fever - antibiotics
Shigella • Characteristics • Gram - facultative anaerobe, rod • DNA hybridization reveals they’re actually biogroups of E. coli. • Don’t ferment lactose • Intracellular pathogen
Shigella Virulence Factors • Adhere to, invade, and replicate in M cells (Peyer’s Patches). • Spread to macrophages and cause lysis of phagocytic vacuole • They then replicate in the cytoplasm • Cause apoptosis, and release of IL-1β which attract polymorphonulear leukocytes which destroy intestinal tissue. • Shiga toxin—disrupts protein synthesis • Remember E. coli O157:H7
Shigella Epidemiology • Estimated 450,000 cases in U.S. (2003) • 150 million world wide • Spread by fecal oral route (yummy). • Primarily a pediatric disease • 70% occur in children 15 and under. • Highest risk in daycares, nurseries, custodial institutions • Low infectious dosage (~200 cells)
Shigellosis • Symptoms appear 1-3 days after ingestion • Begin with watery diarrhea. • Progress to abdominal cramps and pus in bloody stool. • Usually clears up on its own • Antibiotics are given to reduce the chance of spread • Small percentage of asymptomatic colonization
Yersinia Species • Y. pestis – causes the plague • Highly virulent pathogen causing a systemic disease • Y. enterocolitica - causes enterocolitis
Yersinia Virulence Factors • Found on plasmids • Capsule • Antiphagocytic proteins • Proteins which cause apoptosis in macrophages • Proteases which inactivate compliment proteins • Fibrinases which break down blood clots
Yersinia Epidemiology • Humans are accidental hosts • Most infections in other animals are fatal (not normal flora) • Y. enterocolitica • Reservoirrabbits, rodents, pigs, livestock • Primarily in colder climates • 90% infections associated with ingestion of contaminated meat, milk, water • Mostly in children
Yersiniaentercolitica • Symptoms include: diarrhea, abdominal pain, fever • Can mimic acute appendicitis • Usually lasts 1 to 2 weeks • Because of growth at low temperature (4°C) can spread in blood products
Yersinia pestis Epidemiology Sylvatic Plague • Reservoir is small mammals, livestock etc. • Too widespread for animal control • Can spread by eating contaminated food
Yersinia Pestis Epidemiology Urban plague • Reservoir is rats, transmitted by fleas • Rare due to good hygiene, and rat control • Three great pandemics.
Plague History • Egypt 541 AD. lasted 200yrs • Spread to most of the “old world” • Killed a majority of the population • 1320s, over 5 year period 25 million died in Europe (30-40% of population) • China 1860s spread world wide • About 10 cases in the U.S. per year • Sylvatic plague
Yersinia Diseases Bubonic Plague incubation of no more than 7 days cause bubos (swelling of lymph nodes) in groin and armpit 75% mortality in untreated cases
Yersinia Diseases Pneumonic Plague short (2-3 day) incubation fever, malaise, pulmonary signs highly infectious 90% mortality for untreated patients
Yersinia Treatment • Y. pestis–streptomycin, tetracyclines, chloroamphenicol • Enteric infections usually clear on there own • Urban plague is controlled by reducing the rodent population