Digestive enzymes
Digestive enzymes. mirka.rovenska@lfmotol.cuni.cz. Pancreas is the major organ that synthesizes the digestive enzymes. Various organs in digestion and absorption. Small intestine is a principal site of digestion and absorption.

Digestive enzymes
E N D
Presentation Transcript
Digestive enzymes mirka.rovenska@lfmotol.cuni.cz
Pancreas is the major organ that synthesizes the digestive enzymes Various organs in digestion and absorption
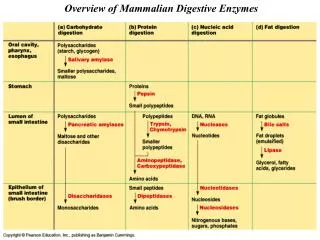
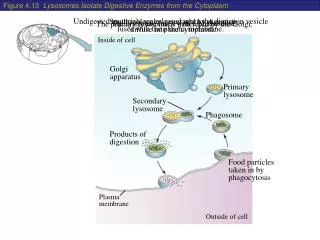
Small intestine is a principal site of digestion and absorption • Pancreatic enzymes together with bile are poured into the lumen of the descending part of the duodenum • Digestion of oligomers of AA and saccharides is accomplished by the enzymes in the luminal plasma membranes of enterocytes; these enzymes – usually glycoproteins • Hydrolysis of di- and tripeptides occurs in the cytoplasm of enterocytes …and there are 3 compartments where digestion and absorption occur:
Zymogens • Digestive enzymes are usually synthesized as larger inactive precursors – zymogens • Otherwise they would digest the tissues that synthesize them: • acute pancreatitis: premature activation of digestive enzymes produced by pancreas→ auto-digestion of pancreas; activated phospholipase A2converts lecithin to lysolecithin that can damage cell membranes
Synthesis of zymogens • Proteins destined for secretion are synthesized on polysomes of the RER • Their N-terminus contains a signal sequence→ release of the protein into ER; then, the signal sequence may be clipped off • Transport to the Golgi complex • The proteins are stored in vesicles; after stimulus, granules move to the luminal plasma membrane (PM) and fuse with PM…exocytosis
Zymogens are activated by proteolysis • Proenzymes (zymogens) are activated by proteolytic cleavage in the lumen of the GIT: • pepsinogen • trypsinogen • chymotrypsinogen • proelastase • procarboxypeptidases • prophospholipases
Activation of pepsinogen • Pepsinogen is secreted from the stomach cells • Pepsinogen is activated by the proteolytic removal of 44 AA from its N-terminus – either as an intramolecular reaction or by active pepsin • This reaction takes place at pH values below 5
chymotrypsinogen, proelastase, procarboxypeptidases, prophospholipase enteropeptidase (produced in duodenum) trypsinogen trypsin – 6 N-terminal AA chymotrypsin, elastase, carboxypeptidases, phospholipase autocatalytic activation Activation of pancreatic zymogens in the lumen of the small intestine
„Strategies“ that prevent premature zymogen activation • At pH>2, the peptide (44 AA) clipped of pepsinogen remains bound to pepsin, masking its active site; it is released by a drop of pH below 2 or by further degradation by pepsin • Pancreatic secretory trypsin inhibitor (PSTI), a small polypeptide,blocksany trypsin that is erroneously activated within the pancreas
Regulation of secretion • Through secretagogues that interact with the receptors on the surface of the exocrine cells → signal cascade leading to fusion of granules with PM • Cholecystokinin: peptide secreted by cells of small int. after stimulation by AA and peptides from gastric proteolysis, by FA, and by acid pH • Secretin: peptide secreted by cells of small int.; stimulated by luminal pH < 5
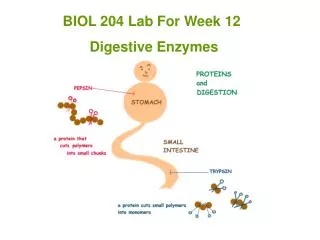
DIGESTION OF PROTEINS • By peptidases (proteases): • endopeptidases – attack internal bonds: • pepsin • trypsin • chymotrypsin • elastase • exopeptidases – cleave off 1 AA at a time from the: • C-terminus – carboxypeptidases • N-terminus – aminopeptidases
Peptidases hydrolyze the peptide bond …and differ in substrate specificity:
Pepsins • Acid in the stomach serves to kill off microorganisms and to denature proteins (denaturation makes proteins more susceptible to proteolysis) • Pepsins are acid stable and pH optimum is about 2!!! • Major products of pepsin action: larger peptide fragments and some free AA; this mix = peptone • Importance lies mainly in generation of peptides and AAs that stimulate cholecystokinin release in the duodenum
Pancreatic enzymes • trypsin • chymotrypsin • elastase • carboxypeptidases • Active at neutral pH depend on neutralization of gastric HCl by pancreatic NaHCO3 • The combined action of pancreatic peptidases results in the formation of free AA and small peptides (2-8 AA)
Intestinal peptidases • Luminal surface of intestinal epithelial cells contains endopeptidases, aminopeptidases, and dipeptidases that cleave oligopeptides released by pancreatic peptidases • Products: AA, di- and tripeptides → absorbed by enterocytes • Di- and tripeptides are hydrolyzed by intestinal cytoplasmicpeptidases • AA are absorbed into the portal blood
DIGESTION OF SACCHARIDES • 1) Polysaccharides(starch, glycogen) are attacked by -amylase, which is present in saliva and pancreatic juice (more important) • -amylase attacks the internal -1,4-glucosidic bonds products: maltose, maltotriose, -limit dextrins
2) Hydrolysis of oligosaccharides is carried out by surface enzymes of the intestinal epithelial cells – disaccharidases and oligosaccharidases • These enzymes – often exoglycosidases
Saccharide absorption • End products: monosaccharides, mainly D-glucose, D-galactose, D-fructose • These are transported by a carrier-mediated process into enterocytes and then into the blood of the portal venous system
Not everything can be digested • Many plant polymers, including celluloses, hemicelluloses, inulin, pectin, are resistant to human digestive enzymes • A small percentage of this „dietary fibre“ is hydrolyzed and then anaerobically metabolized by the bacteria of the lower intestinal tract • This bacterial fermentation produces H2, CH4, CO2, H2S, acetate, propionate, butyrate, lactate
Lactase deficiency • Experienced as milk intolerance • Cause: • a) genetic defect • b) decline of lactase activity with age • c) decline of activity due to an intestinal disease • Inability to absorb lactose accumulation andbacterial fermentation of lactose production of gas (distension of gut, flatulence); osmotically active solutes draw water into the intestinal lumen (diarrhea)
Lysozyme • Hydrolyzes -1,4-glycosidic bonds in the bacterial cell wall polysaccharide peptidoglycan • Kills only some types of bacteria
DIGESTION OF LIPIDS • Lipids – sparingly or not at all soluble in aqueous solutions • Two problems have to be overcome: • poor accessibility of the substrate to the enzyme • aggregation of products of hydrolysis to larger complexes that are hard to absorb
Lipid digestion is initiated in stomach • In the stomach, acid-stable lipase, secreted by stomach (gastric lipase) and by lingual glands (lingual lipase), converts TG mostly into FA and 1,2-diacylglycerols (small amount of monoAG is also produced) • The products possess both polar and non-polar groups act as surfactants: stabilize the water-lipid interface dispersion of the lipid phase into smaller droplets (emulsification) better availability of the substrate to the lipases. • These lipases have the unique ability to initiate the degradation of maternal milk fat globules
Pancreatic lipase • Cleaves acylglycerols mainly to FA and 2-monoacylglycerols • Requires solubilization of the substrate • Also requires colipase (secreted by the pancreas) that anchors and activates the enzyme • Absorption of resulting FA and monoAG requires bile saltsmicelles
Digestion of phospholipids • By phospholipases, especially by phospholipase A2 (requires bile acids for activity): • FA and lysophospholipids are absorbed from the bile acid micelles • In the intestinal mucosa, the absorbed lysophospholipids are reacylated with acyl-CoA
Hydrolysis of cholesterol esters • By pancreatic cholesterol esterase • The free cholesterol is transported in the bile acid micelles and absorbed through the brush border • Here, it is reacylated with acyl-CoA
Bile acid micelles solubilize lipids • Primary bile acids are synthesized by the liver and in peroxisomes, they are conjugated with glycine or taurine (H2N-CH2CH2SO3-) • A portion of the primary bile acids is subjected to the modifications by intestinal bacteria →secondary bile acids • Primary and secondary bile acids are reabsorbed by the ileum into the portal blood, taken up by the liver, and then resecreted into the bile …enterohepatic circulation
Bile acid has a hydrophobic surface and a hydrophilic surface • The most abundant bile salt in humans – glycocholate:
Bile acid micelles • Hydrophobic region of the bile salt is oriented fromthe water molecules x hydrophilic region interacts with water • Mixed micelles contain (beside bile acids) phospholipidsandcholesterol, or FAandacylglycerols; FA and phospholipids form a bilayer in the interior, bile salts occupy the edge.
Released FA and monoacylglycerols are incorporated into bile acids micelles • Micelles move lipids from the intestinal lumen to the cell surface where absorption occurs • Micelles also serve as transport vehicles for vitamins A, K • Fat malabsorption can result from pancreatic failure or lack of bile acids bulk of unabsorbed lipids is excreted with the stool…steatorrhea
Most absorbed lipids are incorporated into chylomicrons • Within the intestinal cell (after absorption): • FA of medium chain lenght(6-10C) pass into the portal blood without modification • long-chain FA (> 12C) are bound to a fatty acid binding protein in the cytoplasm and transported to ER, where they are resynthesized to TG • TG form lipid globules to which phospholipids, cholesterol (esters), and apolipoproteins adsorb – chylomicrons • chylomicrons migrate through the Golgi to the basolateral membrane, they are released, and pass into the lymphatics
DIGESTION OF NUCLEIC ACIDS • Pancreaticenzymes hydrolyze dietary nucleic acids: • ribonucleases • deoxyribonucleases • Polynucleotidasesof the small intestinecomplete the hydrolysis to nucleotides which are then hydrolyzed to nucleosides by phosphatases and nucleotidases • Nucleosides are used as such or undergo degradation by nucleosidases / nucleoside phosphorylases to free bases and pentose-1-phosphate endo- as well as exonucleases
Purine nucleosides are: • A) catabolized to uric acid • B) alternatively, purines are released and used for resynthesis of NA
Pyrimidine nucleosides are: • A) catabolized to NH4+, CO2, and β-aminoisobutyrate or β-alanine, respectively, that are partially converted to (methyl)malonyl-CoA • B) absorbed intact and utilized for the resynthesis of nucleic acids