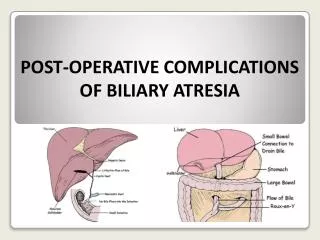
Operative complications
Operative complications. Introduction. Litigation Indemnity cover: MPS. Urologic complications. Important to know the normal urinary tract anatomy and various anomalies (3.3-11.1% of the population) encountered in clinical practice To prevent injury and complications and medicolegal problems.

Operative complications
E N D
Presentation Transcript
Introduction • Litigation • Indemnity cover: MPS
Urologic complications • Important to know the normal urinary tract anatomy and various anomalies (3.3-11.1% of the population) encountered in clinical practice • To prevent injury and complications and medicolegal problems
Causes of oliguria • Prerenal • Decreased volume • Dehydration • Blood loss • Third space sequestration • Circulatory • Septic shock • Cardiogenic shock • Postrenal • Acute obstructive uropathy • Ureteral obstruction • Urethral obstruction • Urinary extravasation • Intrinsic renal disease
Ureteric injury • Low incidence (0.4-2.5%) but serious implications of morbidity and litigation • 75% occur during gynaecologic surgery • Thought to be higher with laparoscopic surgery • Only 1/3 detected during surgery • Intraop recognition is critical for prompt repair before renal compromise occurs • Prevented by routine identification and dissection of the ureter
Risk factors for ureteric injury • Enlarged uterus • Previous pelvic surgery • Ovarian neoplasms • Endometriosis • Pelvic adhesions • Distorted anatomy • Massive bleeding
Types of ureteric injury • Ligation • Angulation • Transection • Laceration • Crush • Ischaemia • Resection
Sites of ureteric injury • Most common site during abdominal hysterectomy or adnexectomy is the pelvic brim where it lies beneath the IFP ligament • Over the iliac arteries • In the cardinal ligament at the level of the internal cervical os where the uterine artery crosses the ureter • At the anterolateral vaginal fornix as the ureter enters the bladder
Sites of injury 5. In vaginal hysterectomy: near the internal cervical os and vaginal fornices as it enters the trigone of the bladder 6. At laparoscopy near the USL esp. with endometriosis 7. Trying to control bleeding in broad ligament at caesarean hysterectomy 8. Hypogastric artery ligation
Prevention of ureteral injuries • Ureteric stenting for difficult cases e.g. Ca ovary • Adequate exposure during surgery. Identify the ureter • Avoid blind clamping of vessels • Caution when using diathermy (laparoscopy)
Diagnosing ureteric injury • 70% diagnosed postop in gynaecologic procedures
Intraoperative diagnosis • If ureters can’t be identified, use of IV methylthioninium chloride or indigo carmine can demonstrate patency • Intraop transurethral cystoscopy or abdominal telescopy may be used to show ejaculation of dye stained urine from both ureteric orifices • Cystoscopy should be considered for complex cases
Postoperative diagnosis • Symptoms are variable: Flank pain, fever, haematuria, retroperitoneal urinoma (sonar) • IVP, CT with IV contrast, retrograde ureterogram, renal u/s, cystoscopy, contrast dye tests
Treatment of ureteral injuries: principles • Tension free anastomosis • Minimal use of fine absorbable suture • Use of peritoneum or omentum to surround the anastomosis • Drain site with passive drain to prevent urine accumulation • Stent with ureteric catheter
Case • Prolonged labour • C section done • Post-op abd distension • ? Diagnosis
Bladder injury • 2 layer repair • Catheter for 10 days
Cardiovascular complications • Perioperative cardiac morbidity is the leading cause of death after anaesthesia and surgery • Includes: MI, unstable angina, CCF, dysrhythmia • Risk factors: Age, previous MI, hypertension, Diabetes • Prevention: good preop care, lab tests, ECG, CXR, cardiologist review
Haematological complications: risk factors • Alcohol abuse • Liver disease • Family h/o bleeding tendency • Prior need for transfusion • Severe menorrhagia • Frequent nosebleeds • Easy bruising • Von Willebrand’s disease • Chronic renal disease • SLE • Anticoagulant use • Antiplatelet drugs
Intraoperative bleeding: risk factors • Surgical technique: blood vessels in retroperitoneal space • Obesity • Large pelvic mass • Adhesions • Cancer • Prior radiotherapy
Blood product replacement • Red cell transfusion: whole blood, red blood cells, leukocyte-poor red cells, washed red cells • Platelet transfusion • Plasma derivatives: Cryoprecipitate-rich in Factor VIII and fibrinogen
GIT • Approached with trepidation by the gynaecologist • Important in complicated surgery like Ca ovary • Bowel injury during surgery • Postop complications: Perforation, ileus, obstruction, reexploration for bowel complications, fistulae
Others • Retained foreign bodies • Lymphoedema • Sexual dysfunction • Death