Biopharmaceutics Classification System (BCS)
Biopharmaceutics Classification System (BCS). Presented By Dr. Sanaa A. El-Gizawy.

Biopharmaceutics Classification System (BCS)
E N D
Presentation Transcript
Biopharmaceutics Classification System (BCS) Presented By Dr. Sanaa A. El-Gizawy
The (BCS) has been developed to provide a scientific approach to allow for the prediction of in vivo pharmacokinetics of oral immediate release (IR) drug products by classifying drug compounds based on their solubility related to dose and intestinal permeability in combination with the dissolution properties of the dosage form
The importance of drug dissolution in the gastrointestinal tract and permeability across the gut wall barrier in the oral absorption process has been well known since the 1960s, but the research carried out to constitute the BCS has provided new quantitative data of great importance for modern drug development especially within the area of drug permeability
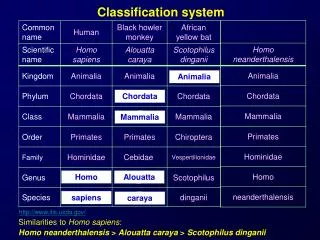
According to the BCS, drug substances are classified as follows: • Class I - High Permeability, High Solubility • Class II - High Permeability, Low Solubility • Class III - Low Permeability, High Solubility • Class IV - Low Permeability, Low Solubility
The BCS is a scientific framework for classifying drug substances based on their aqueous solubility and intestinal permeability. When combined with the dissolution of the drug product, the BCS takes into account three major factors that govern the rate and extent of drug absorption from IR solid oral dosage forms: dissolution, solubility, and intestinal permeability.
CLASS BOUNDARIES • A drug substance is considered HIGHLY SOLUBLE when the highest dose strength is soluble in < 250 ml water over a pH range of 1 to 7.5. • A drug substance is considered HIGHLY PERMEABLE when the extent of absorption in humans is determined to be > 90% of an administered dose, based on mass-balance or in comparison to an intravenous reference dose. • A drug product is considered to be RAPIDLY DISSOLVING when > 85% of the labeled amount of drug substance dissolves within 30 minutes using USP apparatus I or II in a volume of < 900 ml buffer solutions.
The benefits of knowing the BCS category of a compound • It can save both time and money—if the immediate -release, orally administered drug meets specific criteria, the FDA will grant a waiver for expensive and time-consuming bio-equivalence studies. • The aim of the BCS is to provide a regulatory tool for the replacement of certain BE studies by conducting accurate in vitro dissolution tests.
Follow; The benefits of knowing the BCS category of your compound • This step will certainly reduce timelines in the drug development process, both directly and indirectly, and reduce unnecessary drug exposure in healthy volunteers, which is normally the study population in BE studies. • It has also been reported that the application of a BCS strategy in drug development will lead to significant direct and indirect savings for pharmaceutical companies
Follow; The benefits of knowing the BCS category of your compound • BCS has been developed primarily for regulatory applications, but it has also several other applications in both the pre-clinical and clinical drug development processes and has gained wide recognition within the research-based industry
Combined with the dissolution, the BCS takes into account the three major factors governing bioavailability viz. dissolution, solubility and permeability. • This classification is associated with drug dissolution and absorption model, which identifies the key parameters controlling drug absorption as a set of dimensionless numbers viz.
Key Parameters Controlling Drug Absorption • Absorption number (An), defined as the ratio of the mean residence time to mean absorption time. • Dissolution number (Dn), defined as the ratio of mean residence time to mean dissolution time. • Dose number (D0), defined as the mass (Dose) divided by the product of (uptake volume (250 ml) and solubility of drug). D0 = Dose/(V.Cs)
Class I drugs exhibit a high absorption number and a high dissolution number. The rate limiting step is drug dissolution. • If dissolution is very rapid, then gastric emptying rate becomes the rate determining step. • e.g. Metoprolol, Diltiazem, Verapamil, Propranolol.
Class II drugs have a high absorption number but a low dissolution number. In vivo drug dissolution is then a rate limiting step for absorption except at a very high dose number. The absorption for class II drugs is usually slower than class I and occurs over a longer period of time. • In vitro- In vivo correlation (IVIVC) is usually excepted for class I and class II drugs. • e.g. Phenytoin, Danazol, Ketoconazole, Mefenamic acid, Nifedinpine.
For Class III drugs, permeability is rate limiting step for drug absorption. These drugs exhibit a high variation in the rate and extent of drug absorption. • Since the dissolution is rapid, the variation is attributable to alteration of physiology and membrane permeability rather than the dosage form factors. • e.g. Cimetidine, Acyclovir, Neomycin B, Captopril.
Class IV drugs exhibit a lot of problems for effective oral administration. Fortunately, extreme examples of class IV compounds are the exception rather than the rule and are rarely developed and reach the market. Nevertheless a number of class IV drugs do exist. e.g. Taxol.
Applications of BCS in oral drug delivery technology • Once the solubility and permeability characteristics of the drug are known it becomes an easy task for the research scientist to decide upon which drug delivery technology to follow or develop.
Class I Drugs • The major challenge in development of drug delivery system for class I drugs is to achieve a target release profile associated with a particular pharmcokinetic and/or pharmacodynamic profile. • Formulation approaches include both control of release rate and certain physicochemical properties of drugs like pH-solubility profile of drug.
Class II Drugs • The systems that are developed for class II drugs are based on micronisation, lyophilization, addition of surfactants, formulation as emulsions and microemulsions systems, use of complexing agents like cyclodextrins.
Class III Drugs • Class III drugs require the technologies that address to fundamental limitations of absolute or regional permeability. Peptides and proteins constitute the part of class III and the technologies handling such materials are on rise now days.
Class IV Drugs • Class IV drugs present a major challenge for development of drug delivery system and the route of choice for administering such drugs is parenteral with the formulation containing solubility enhancers.