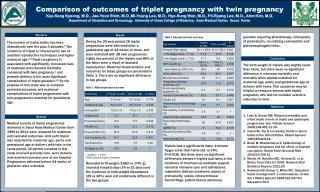
TWIN PREGNANCY
TWIN PREGNANCY. DR ANSAM AL AMAJALI FETOMATERNAL CONSULTANT KSMC. Definition (Multi-fetal Gestation) MULTIPLE PARITY -Twins (two babies) -Monozygotic(Division of 1 ova fertilized by the same sperm) - Dizygotic (Fertilization of 2 ova by 2 sperm)

TWIN PREGNANCY
E N D
Presentation Transcript
TWIN PREGNANCY DR ANSAM AL AMAJALI FETOMATERNAL CONSULTANT KSMC
Definition (Multi-fetal Gestation) MULTIPLE PARITY -Twins (two babies) -Monozygotic(Division of 1 ova fertilized by the same sperm) -Dizygotic(Fertilization of 2 ova by 2 sperm) -Triplets (three babies) -Quadruplets (four babies) I
Incidence •Twins - 1 in 100 births –African Americans: 1 in 70 –Caucasians: 1 in 88 –Japanese: 1 in 150 –Chinese: 1 in 300 •Triplets are about 1 in 7,500 births •Quadruplets are about 1 in 650,00 births
Predisposing Factors •Maternal age and parity •Maternal height and weight •Genetic and racial factors •Prior use of oral contraceptive agents •Social class •Seasonality
Causes of Multiple Gestation •Spontaneously •In Vitro fertilization –Intrauterine insemination –Assisted Hatching –GIFT, ZIFT –Frozen Embryo Transfer, Blastocyte Embryo Transfer •Fertility Drugs –Clomiphene citrate (clomid, serrophene) –Gonadotropins (GonalF, follistim, humagon)
Twins •Dizygotic twins (66% of US twins) –Dichorionic – separate chorion (placenta) –Diamniotic – separate amnion (amniotic sac)
•Monozygotic twin (33% of US twins) Ova division: •< 72 hours: Dichorionic, diamniotic •4-8 days: Monchorionic, diamniotic •8-13 days: Monochorionic, monoamniotic •> 13 days: conjoined twins
Conjoined Twins •Craniopagus •Pygopagus •Thoracopagus •Cephalopagus •Epholothoracopagus •Craniopagus •Pygopagus •Thoracopagus •Cephalopagus •Epholothoracopagus
Average age of gestation Number of babies Weeks of Gestation 1 40 weeks 2 35 1/2 weeks 3 33 weeks 4 29 ½ weeks http://www.bestdoctors.com/en/conditions/g/gestation/gestation_100200.htm
Peripartum Complications •Prematurity-major cause of neonatal death 50% of twins 90% of triplets and higher •Spontaneous abortion •Increased anomalies •Cord Prolapse •IUGR, discordant growth •Intracranial Hemorrhage •Locked Twins Description: Twins lock heads 1st twin breech, 2nd twin vertex
Problems of Prematurity •HMD/BPD •Pneumothorax •Apnea •ICH •CP •Blindness/Retinopathy •LBW •PDA •Hypertension/Hypotension
Problems of Prematurity •Bradycardia •Anemia •Hyperbilirubinemia •NEC •Metabolic disorders •Hypothermia •HIE •Hypotonia •Infections
Neonatal Management (Multiple Gestation) •Team for each fetus •Examine for prematurity and IUGR •Examine for congenital anomalies •Determine zygosity, examine placenta •Assess family support
In ICN •RDS •Apnea/Asphyxia •Hct and BP •Wt difference •NEC •Head Sono + •Glucose •Blood typing
Second Twin Risks •Asphyxia due to premature separation of placenta •Fetus papyraceous -twin fetus that died in utero, become flattened and mummified •Fetal transfusion Syndrome Placental AV shunt in monozygotic twins (~15%) Arterial twin pumps blood to other twin, starves self Other twin is bulky and plethoric •Operative or difficult delivery
Monozygotic twins (physical characteristics) •Same sex •Features alike, including teeth and ears •Hair identical •Eyes same color and shade •Skin same texture and color •Hands and feet same conformation and same size •Anthropometric values closely agree
Twin-Twin Transfusion Syndrome •Monozygotic twins share one placenta •1 placenta causes one baby to receive more blood . •One baby (donor) smaller and other larger. •Larger baby: excess urine, polyhydramnios. •Donor stops producing urine, oligohydramnios. •This can lead to pre-term delivery (~24 weeks).
Problems for Monoamnionicity Rare < 1% . •Mortality 20-50%. •Cord entanglement. •Perinatal mortality. •Preterm Delivery. •Growth restriction. •Congenital anomalies. •Conjoined twins Siamese twins * Anterior (thoracopagus). * Posterior (pygopagus). * Cephalic (craniopagus). * Caudal (ischopagus).
Problems for Monoamnionicity • 1.Acardiac twins (Reversed-Arterial Perfusion TRAP). • * rare 1:3500 births. • large A-A placental shunt between umbilical arteries in early • embryogenesis, • 75% monochorionic, diamniotic. • 25% monochorionicmonoamniotic.
Maternal Complication 1.Acute fatty liver. 2.Anemia. 3.Abnormal placentation. 4.Amniotic fluid volume abnormalities. 5.Preeclampsia. 6.Operative vaginal delivery and C-section. 7.Premature rupture of membrane. 8.Postpartum hemorrhage. 9.Umbilical cord prolapse.
Prevention (Multiple Gestation) •Moniter treatment with fertility drugs •Limit embryos transferred during IVF •Counseling risks and long-term sequelae • Fetal reduction if not against religion
Management 1.Antenatal. 2.In Labor. Antenatal Management ●Early diagnosis (mainly by ultra sound) ●Adequate nutrition:- 1- Caloric consumption increased by 300 Kcal per day. 2- Iron 60-100 mg per day. 3- Folic acid 1mg per day. ●Frequent prenatal visit:- observe maternal and fetal complications 1- Frequent ultra sound fetal growth, congenital anomalies, amniotic fluid. 2- Doppler. 3- BPP.
In Labor Management ●Trained obstetrical attendant. ●Available blood. ●Good access I.V live. ●CTG monitoring. ●Anesthetist ER C-S ●Pediatrician for each fetus. ●Mode of delivery depend on presentation.
Presentation ☻Cephalic - Cephalic 42% ☻Cephalic - Breech 27% ☻Cephalic - Transverse 18% ☻Breech - Breech 5% ☻Other 8% Management in First stage Second stage Third stage (PPH)
In Labor Management ●Ceph-ceph: NVD ●Ceph –non ceph: contraversy. ●Breech:cordprolaps,Headtrappe,Lockedtwin:c/s. ●Second twin: 10 min and no contraction. ●Non fixed p.p :abdominal manipulation ●Second twin:internalpudalic version. ●Irregular FHR,VB,larger,Bx, Trans ,contract Cx: C/S .
In Labor Management ●Trained obstetrical attendant. ●Available blood. ●Good access I.V live. ●CTG monitoring. ●Anesthetist ER C-S ●Pediatrician for each fetus. ●Mode of delivery depend on presentation.