Cardiac Physiology
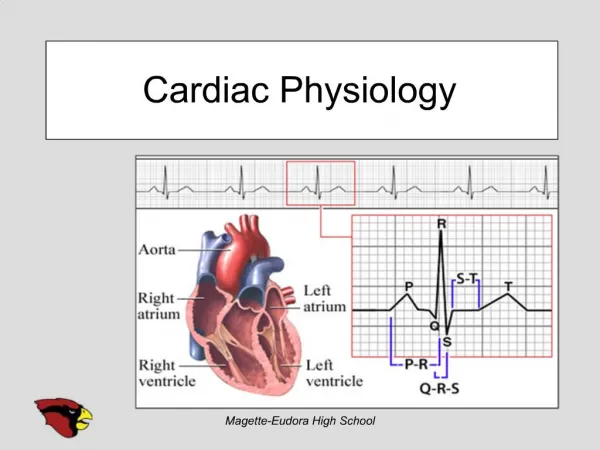
Cardiac Physiology. Dr. Meg- angela Christi Amores. The Heart. separate pumps: a right heart that pumps blood through the lungs, a left heart that pumps blood through the peripheral organs atrium and ventricle. The Heart. Cardiac muscle Striated Myofibrils with actin and myosin

Cardiac Physiology
E N D
Presentation Transcript
Cardiac Physiology Dr. Meg-angela Christi Amores
The Heart • separate pumps: • a right heart that pumps blood through the lungs, • a left heart that pumps blood through the peripheral organs • atrium and ventricle
The Heart • Cardiac muscle • Striated • Myofibrils with actin and myosin • 3 types of cardiac muscles: • atrial muscle • ventricular muscle • specialized excitatory and conductive musclefibers
The Cardiac Muscle • Syncytium • cardiac muscle fibers are made up of many individual cells connected in series and in parallel with one another via intercalated discs • form permeable "communicating" junctions • action potentials travel easily from one cardiac muscle cell to the next
The cardiac muscle • two syncytiums: • the atrialsyncytium that constitutes the walls of the two atria • the ventricular syncytium that constitutes the walls of the two ventricles • they are conducted only by way of a specialized conductive system called the A-V bundle
The cardiac Muscle • Action Potential
Action potential • Caused by opening of two types of channels: • fast sodium channels • tremendous numbers of sodium ions to enter the skeletal muscle • open for only a few thousandths of a second and then abruptly close • slow calcium channels • large quantity of both calcium and sodium ions flows through these channels to the interior of the cardiac muscle fiber, and this maintains a prolonged period of depolarization • Causes PLATEAU of action potential • are slower to open and remain open for several tenths of a second
Cardiac muscle Action Potential • after the onset of the action potential, the permeability of the cardiac muscle membrane for potassium ions decreases about fivefold • greatly decreases the outflux of positively charged potassium ions during the action potential plateau • thereby prevents early return of the action potential voltage to its resting level
Refractory period • is the interval of time during which a normal cardiac impulse cannot re-excite an already excited area of cardiac muscle • 0.25 to 0.30 second • relative refractory period of about 0.05 second during which the muscle is more difficult than normal to excite but nevertheless can be excited by a very strong excitatory signal
excitation-contraction coupling • the mechanism by which the action potential causes the myofibrils of muscle to contract • when an action potential passes over the cardiac muscle membrane, the action potential spreads to the interior of the cardiac muscle fiber along the membranes of the transverse (T) tubules
excitation-contraction coupling • T tubule action potentials in turn act on the membranes of the longitudinal sarcoplasmic tubules • release of calcium ions into the muscle sarcoplasm
excitation-contraction coupling • calcium ions diffuse into the myofibrils and catalyze the chemical reactions that promote sliding of the actin and myosin filaments along one another • Producing muscle contraction
excitation-contraction coupling • a large quantity of extra calcium ions also diffuses into the sarcoplasm from the T tubules themselves at the time of the action potential
Cardiac Cycle • cardiac events that occur from the beginning of one heartbeat to the beginning of the next • Diastole • during which the heart fills with blood • Systole • period of contraction
The atria • Primer pumps • 80 per cent of the blood flows directly through the atria into the ventricles even before the atria contract • atrial contraction usually causes an additional 20 per cent filling of the ventricles • increase the ventricular pumping effectiveness
The ventricles • Filling of ventricles • After systole, AV opens via pressure build up in atria • Emptying of ventricles • Period of Isovolumic (Isometric) Contraction • Period of Ejection • Period of Isovolumic (Isometric) Relaxation
Factors for cardiac contractility • Chemical energy • Derived mainly from oxidative metabolism of fatty acids and, to a lesser extent, of other nutrients, especially lactate and glucose
Regulation of Heart pumping • heart pumps only 4 to 6 liters of blood each minute at rest • severe exercise, the heart may be required to pump four to seven times • (1) intrinsic cardiac regulation of pumping in response to changes in volume of blood flowing into the heart • (2) control of heart rate and strength of heart pumping by the autonomic nervous system
Regulation of Heart pump • Intrinsic regulation • the Frank-Starling mechanism of the heart • intrinsic ability of the heart to adapt to increasing volumes of inflowing blood • the greater the heart muscle is stretched during filling, the greater is the force of contraction and the greater the quantity of blood pumped into the aorta
Regulation of Heart pump 2. Control of the Heart by the Sympathetic and Parasympathetic Nerves • amount of blood pumped each minute (cardiac output) often can be increased more than 100 per cent by sympathetic stimulation • the output can be decreased to as low as zero or almost zero by vagal (parasympathetic) stimulation
Other factors • Potassium and Calcium Ions • Excess potassium in the extracellular fluids causes the heart to become dilated and flaccid and also slows the heart rate • Excess of calcium causes the heart to go toward spastic contraction
Other Factors • Temperature • heat increases the permeability of the cardiac muscle membrane to ions • Increased body temperature, as occurs when one has fever, causes a greatly increased heart rate
Heart Sounds • lub, dub, lub, dub • The "lub" is associated with closure of the atrioventricular (A-V) valves at the beginning of systole(s1) • "dub" is associated with closure of the semilunar (aortic and pulmonary) valves at the end of systole (s2)
vibration of the taut valves immediately after closure • with vibration of the adjacent walls of the heart and major vessels around the heart
Shorter 2nd heart sound: semilunar valves are more taut than the A-V valves, so that they vibrate for a shorter time than do the A-V valves
Third Heart Sound • at the beginning of the middlethird of diastole • initiated by inrushing blood from the atria • Atrial Heart Sound (Fourth Heart Sound) • occurs when the atria contract, and presumably, it is caused by the inrush of blood into the ventricles
Heart Murmurs • Abnormal heart sounds • Due to abnormalities of valves • Systolic murmurs • Occur during systole • Aortic Stenosis, Mitral Regurgitation • Diastolic murmurs • Occur in diastole • Aortic Regurgitation, Mitral Stenosis