LICHEN PLANUS (LP)
LICHEN PLANUS (LP). Overview Lichen planus is an inflammatory disease that affects the skin and the oral mucosa. Cause

LICHEN PLANUS (LP)
E N D
Presentation Transcript
Overview Lichen planus is an inflammatory disease that affects the skin and the oral mucosa. Cause The cause of lichen planus is not known; however, there are cases of lichen planus-type rashes (known as lichenoid reactions) occurring as allergic reactions to medications for high blood pressure, heart disease and arthritis. These lichenoid reactions are referred to as lichenoidmucositis (of the mucosa) or dermatitis (of the skin). Lichen planus has been reported as a complication of chronic hepatitis c virus infection and can be a sign of chronic graft-versus-host disease of the skin.
It has been suggested that true lichen planus may respond to stress, where lesions may present on the mucosa or skin during times of stress in those with the disease. Lichen planus affects women more than men (at a ratio of 3:2), and occurs most often in middle-aged adults. Lichen planus in children is rare.
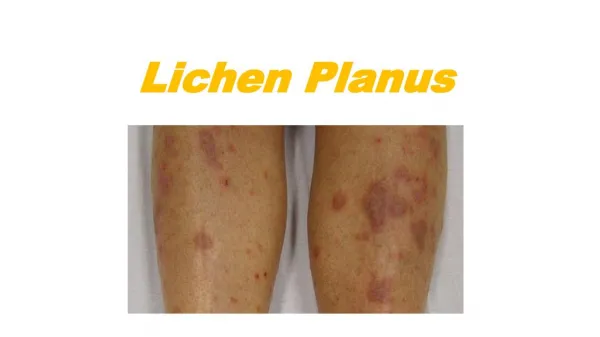
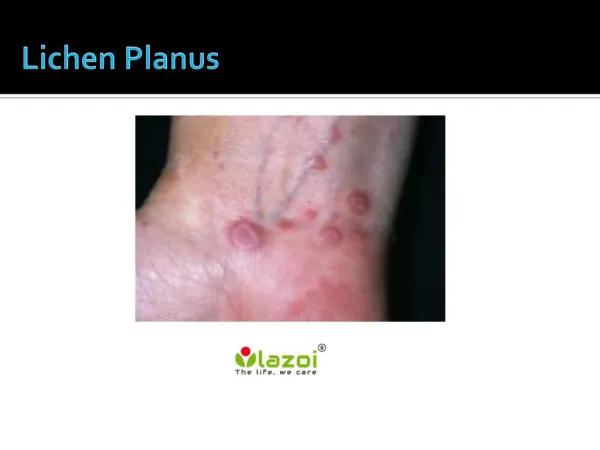
C/P • The typical rash of lichen planus is well-described by the "5 P's": well-defined pruritic, planar, purple, polygonal papules. • Flexor surfaces especially wrists, flanks, medial thighs, shins of tibia, glans penis, nails, scalp & oral mucosa. • Pruritus;rubbing than scratching. • Koebner’s phenomenon (isomorphic response). • After lesions subside, post lichen hyperpigmentation occurs.
Lichen planopilaris Lichen Planopilaris is the specific name given to lichen planus on the scalp that .may cause permanent, scarring alopecia
Oral LP Oral lichen planus may present in one of three forms. The reticular form is the most common presentation and manifests as white lacy streaks on the mucosa (known as Wickham's striae) or as smaller papules (small raised area). The lesions tend to be bilateral and are asymptomatic. The lacy streaks may also be seen on other parts of the mouth, including the gingiva (gums), the tongue, palate and lips. The bullous form presents as fluid-filled vesicles which .project from the surface
The erosive form presents with erythematous (red) areas that are ulcerated and uncomfortable. The erosion of the thin epithelium may occur in multiple areas of the mouth, or in one area, such as the gums, where they resemble desquamative gingivitis. Wickham's striae may also be seen near these ulcerated areas. This form may undergo malignant transformation.
Complications of LP • Squamous cell carcinoma in oral ulcerative lesions. • Cicatricial alopecia in scalp LP. • Postinflammatoryhyperpigmentation.
Differential Diagnosis • The clinical presentation of lichen planus may also resemble other conditions, including: • Lichenoid drug reaction • Discoid Lupus Erythematosus • Chronic Ulcerative Stomatitis • PemphigusVulgaris • Benign Mucous Membrane Pemphigoid • Oral leukoplakia • Frictional keratosis A biopsy is useful in identifying histological features that help differentiate lichen planus from these conditions.
Treatment • Currently there is no cure for lichen planus but there are certain types of medicines used to reduce the effects of the inflammation. Lichen planus may go into a dormant state after treatment. There are also reports that lichen planus can flare up years after it is considered cured. • Medicines used to treat lichen planus include: • Oral and topical steroid • Oral retinoids • immunosuppressant medications • Hydroxychloroquin • Tacrolimus • dapson
An inflammatory non-infectious scaly erythematous eruption. • An exanthematous reaction to an upper respiratory viral infection. • Highest between 15-40 years. • More prevalent in spring & autumn. Etiology Human herpes virus (HHV)-6 & -7.
C/P Primary Lesion:Herald patch • Single oval lesion with three different zones. • Starts on one side of the trunk with its longitudinal axis // to ribs.
C/P (cont.) Secondary Eruption: • Occurs after 1-2 weeks from the onset of herald patch. • Similar to herald patch, but smaller & multiple. • Distributed along long axis of ribs (Christmas tree pattern). • Located on the trunk & proximal parts of the limbs; flannel area giving picture of jacket with short sleeves. • Itching. • Spontaneously heal within 4-8 weeks. • Recurrences are not common.
DD:Tineacircinata(by CP & scraping). Treatment • Patient reassurance. • Avoid skin irritation. • Soothing lotions, e.g. calamine lotion. • Oral antihistamines, mild topical corticosteroids & UVB.