Aggressive Angiomyxoma
Aggressive Angiomyxoma. AM Report 1/25/2010 Cat Hathaway. Epidemiology. Aggressive Angiomyxoma (AA) is a very rare tumor. It was first described in 1983 and since then only about 250 cases have been reported Women are affected more than men (1:6.6), typically in the reproductive years

Aggressive Angiomyxoma
E N D
Presentation Transcript
Aggressive Angiomyxoma AM Report 1/25/2010 Cat Hathaway
Epidemiology • Aggressive Angiomyxoma (AA) is a very rare tumor. It was first described in 1983 and since then only about 250 cases have been reported • Women are affected more than men (1:6.6), typically in the reproductive years • Genetic abnormality in chromosome 12 is found in some AA • 12q15 involving HMGA2 gene
Locations of the tumor are typically in the pelvis and perineum of women • Scrotum and inguinal area for men • Can be found in men and there are case reports of AA mimicking inguinal hernias and hydrocele • Case reports also found with AA in maxillary sinus and the larynx (1each) • No associated risk factors have been identified
Histology • These are tumors of myxoid or mesenchymal origin, i.e. connective tissue. They are typically S100 negative. • Often positive IHC for desmin, vimentin, alpha smooth muscle actin • The tumor is soft and does not have discrete borders. In fact the tumor often has soft finger like projections that extend into surrounding tissue • Appears hypocellular on pathology and is of mesenchymal cell origin. There are bland spindled and stellate cells and a background of myxoidstroma. Blood vessels are prominent • Typically estrogen & progesterone receptor +
Hypocellular background and prominent blood vessels seen on Pathology
Presentation • No specific or typical features. Often will be an asymptomatic perineal or vulvar mass. Sometimes will be a pelvic mass seen on imaging. • Sometimes can appear cystic and can be confused with Bartholin’s cyst • Very slow growing, often not noticed until the size of the tumor is quite large • Obesity can result in vulvar edema that can be mistaken for AA – although typically bilateral and involves superficial tissues as well
Clinical Features • As the tumor is not encapsulated it is difficult to resect. Local recurrence is very common (up to 70% in some series). • Metastasis is very rare. In one case series they report only 2 with metastasis to the lungs. • Can cause obstruction of bowel or of bladder/ureters if advanced peritoneal presentation. Some can develop complete obstruction of the intestinal tract
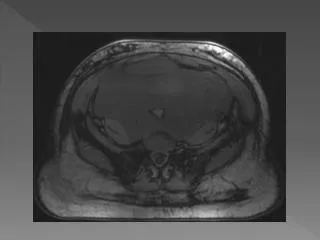
Diagnosis • Typically diagnosis is not made until surgical excision and pathology obtained • Imaging will show some characteristic findings. US shows hypoechoic mass, can appear cystic. MRI shows hypo-intense mass compared to muscle on T1 but hyperintense on T2. CT can be variable, but typically homogenous mass that sometimes has cystic components
Treatment • Surgical excision – often can be problematic as the tumor is very locally invasive. Goal is complete excision. • One series showed 50% vs 40% pts remained disease free at 10 years of those who had complete vs incomplete resection • However generally felt that recurrence is less if 1cm tumor free margins are obtained • Reportedly not life threatening, but two cases of metastasis have been reported and these patients died. • GNRH antagonists have been used with success, although these are case reports, no formal trials have been done
Treatment continued • The tumors have very low mitotic activity and slow growth rates, which is why adjuvant therapy with chemo or radiation is not typically pursued. • Only a few case reports of XRT, yielding mixed results. No cases reporting use of chemotherapy • Recurrence occurs within 3 years in 70% of the cases but can be as late as 14 years • F/u is clinical but should also include imaging studies, preferably MRI
Prognosis • Typically felt to be benign, although as mentioned before very locally invasive • Our patient did have metastatic disease and as such extensive surgical excision was not attempted • Often require repeat surgery to remove recurrent tumor. • Size at diagnosis plays a large role in prognosis
Other conditions to consider • Pseudomyxoma peritonei – there are two types, benign and malignant. Both are locally aggressive and have many relapses/recurrences. • Lipoma • Myxoid sarcoma • Intramuscular myxoma • Myxoid neurofibroma • Angiomyofibroblastoma
Bibliography • http://atlasgeneticsoncology.org/Tumors/AggresAngiomyxomaID5203.html • Haldar K, et al., Aggressive angiomyxoma: A case series and literature review, Eur J SurgOncol (2009), doi:10.1016/j.ejso.2009.11.006 • Chunyanca et al. World J SurgOncol. 2006; 4: 60. Published online 2006 September 1. doi: 10.1186/1477-7819-4-60. • Fujita Y - J Am AcadDermatol - 01-FEB-2008; 58(2 Suppl): S40-1 • Wu, et al. Scrotal aggressive angiomyxoma mimicking inguinal hernia. Asian J Androl. 2007 Sep;9(5):723-5.