Gastric Ulcer
300 likes | 651 Vues
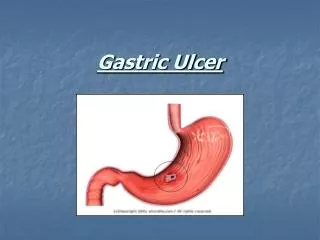
Gastric Ulcer. Even though gastric ulcer is a common disease, a diagnosis can be difficult because it has a wide spectrum of clinical presentations, ranging from : - asymptomatic to vague epigastric pain, nausea, and iron-deficiency anemia to - acute life-threatening hemorrhage.

Gastric Ulcer
E N D
Presentation Transcript
Even though gastric ulcer is a common disease, a diagnosis can be difficult because it has a wide spectrum of clinical presentations, ranging from:-asymptomatic to vague epigastric pain, nausea, and iron-deficiency anemia to -acute life-threatening hemorrhage. The normal stomach maintains a balance between: • protective factors- such as mucus and bicarbonate secretion and • aggressive factors- such as acid secretion and pepsin Gastric ulcers develop when aggressive factors overcome protective mechanisms.
Causes The two major etiological factors for pepticulcer disease (PUD) are: • Helicobacter pylori infection • nonsteroidal anti-inflammatory drug (NSAID) consumption 70% of all gastric ulcers occurring in the United States can be attributed to H pylori infection.
Helicobacter pylori • the bacterium's spiral shape and flagella facilitate its penetration into the mucous layer and its attachment to the epithelial layer • it releases phospholipase and proteases, which cause further mucosal damage • a cytotoxin-associated gene (cag A) has been isolated in approximately 65% of the bacteria • the products of this gene are associated with more severe gastritis, gastric ulcer, gastric cancer, and lymphoma
NSAID • 26% of gastric ulcers • secondary to a decrease in prostaglandin production resulting from the inhibition of cyclooxygenase.1 • the typical effects of NSAIDs are superficial gastric erosions and petechial lesions • the greatest risk of developing an ulcer occurs during the first 3 months of NSAID use • patients with H pylori infection may be twice as likely to get a bleeding peptic ulcer.
In the Celecoxib Long-term Arthritis Safety Study (CLASS), they found a significantly lower incidence of symptomatic ulcers in patients taking celecoxib for the initial 6 months as compared to patients taking ibuprofen or diclofenac • Other medications that predispose patients to gastroduodenal ulcers include potassium chloride, chemotherapeutic agents, and bisphosphonates • A rare cause of PUD is Zollinger-Ellison syndrome (gastrinoma). The hallmark of Zollinger-Ellison syndrome is : • profound hypersecretion of gastric acid • significant disruption of the mucosal integrity • Cigarette smoking- people who smoke tend to develop more frequent and recurrent ulcers and their ulcers are more resistant to therapy
Frequency • United States- it is estimated to affect 0.92% of the population or 1.6 million persons. • Epidemiological studies 1970-1985, a marked decrease in the rate of duodenal ulcer occurred, while the rate of gastric ulcer remained stable. • people with low socioeconomic status are more likely to acquire H pylori infection • individuals who are infected are 3 times more likely to develop gastric ulcer compared to those unexposed to the bacteria.
simple gastric ulcer is in decline, the incidence of complicated gastric ulcer and hospitalization has remained stable, partly due to the concomitant use of aspirin in an aging population • International • Denmark, lifetime prevalence of gastric cancer is 1.2% for men and 0.6% for women The annual incidence of gastric ulcers • Japan-1 case per 1000 population • Norway - 1.5 cases per 1000 population • Scotland - 2.7 cases per 1000 population
Mortality/Morbidity • the mortality rate is higher in patients older than 75 years(attributable to a high rate of NSAID use in this age group) • the other high-risk groups -chronicrenal insufficiency and diabetes Sex • the male-to-female ratio is 1:1 in the United States and 18:1 in India Age • the incidence of gastric ulcer increases with age • increasing NSAID use • a high prevalence of H pylori infection in persons older than 50 years
Clinical History • classic gastric ulcer pain is described as pain occurring shortly after meals, for which antacids provide minimal relief • the pain from gastric ulcer is typically located in the epigastrium;in the right upper quadrant and elsewhere • duodenal ulcer pain often occurs hours after meals and at night; relieved with food or antacids • pain with radiation to the back is suggestive of a posterior penetrating gastric ulcer complicated by pancreatitis • patients with bleeding gastric ulcers may give a history of hematemesis, melena, or episodes of presyncope • melena can be intermittent over several days or multiple episodes in a single day.
Physical • epigastric tenderness may or may not be present • right upper quadrant tenderness may suggest a biliary etiology or, less frequently, PUD • in the presence of gastric outlet obstruction, abdominal distension and succussion splash may be found • a palpable mass should raise the suggestion of a gastric malignancy • involuntary guarding is indicative of peritonitis secondary to gastric perforation • patients should be checked for melena, which is indicative of bleeding from a gastroduodenal ulcer • digital rectal examination can be easily performed in the office to check for melena.
Differential Diagnoses • Cholecystitis • Crohn Disease • Duodenal Ulcers • Gastric Cancer • Pancreatitis, Chronic • Zollinger-Ellison Syndrome • Other Problems to Be Considered • Nonulcer dyspepsia (NUD) or functional dyspepsia (a diagnosis of exclusionin the absence of any organic disease after thorough evaluation are thought to have functional dyspepsia • Crohn disease: Crohn ulceration can involve any part of the GI tract from the buccal mucosa to the rectum. Isolated Crohn ulceration of the stomach is rare, although it may cause duodenal or ileal ulcerations.
Laboratory Studies Routine laboratory tests: • complete blood cell count • iron studies, can help detect anemia. Anemia and weight loss are alarm signalsand mandate early endoscopy to rule out other sources of chronic GI blood loss.
Imaging Studies Upper GI radiography • a double-contrast barium study -benign gastric ulcers
Other Tests • H pylori testing • Invasive tests • Biopsy • Culture • Rapid urease test • Noninvasive tests • Antibody testing • Urea breath testing • Stool antigen
Procedures • Esophagogastroduodenoscopy (EGD) • endoscopy is a relatively safe procedure in experienced hands • direct visualization to obtain biopsy specimens and also to perform endoscopic therapy for bleeding ulcers • the preferred modality for the diagnosis of gastric ulcer and gastric cancer • a repeat endoscopy after 6 weeks of therapy is recommended to confirm healing of a gastric ulcer and to help definitively rule out gastric malignancy • upper endoscopy with biopsy is the most sensitive and specific method for diagnosing gastric and esophageal cancer • 7 biopsy samples obtained from the base and ulcer margins increase the sensitivity to 99%
Treatment • H pylori eradication • Bismuth, metronidazole, and tetracycline qid with H2 blockers bid • Bismuth, metronidazole, and tetracycline bid with a PPI (Helidac) • Prevacid, amoxicillin, and clarithromycin bid (PrevPac) • Prilosec, metronidazole, and clarithromycin bid • Ranitidine, bismuth, and clarithromycin with amoxicillin, metronidazole, or tetracycline bid
Endoscopic therapy • Surgical Care • Consultations • Diet
Medication • Proton pump inhibitors • Omeprazole (Prilosec) - 40 mg PO • Lansoprazole (Prevacid) - 15-30 mg PO • Rabeprazole (Aciphex) - 20 mg tab PO • Pantoprazole (Protonix) - 40 mg PO • Esomeprazole (Nexium) - 40 mg PO • Histamine H2 antagonists • Nizatidine (Axid) - 75 mg PO • Ranitidine (Zantac) - 150 mg PO
Helicobacter pylori eradication agents • Clarithromycin (Biaxin) - 250-500 mg PO • Metronidazole (Flagyl) - 250 mg PO • Bismuth subsalicylate (Pepto-Bismol) - 2 tab or 30 mL PO • Tetracycline (Sumycin) - 250 mg PO • Amoxicillin (Trimox) - 500 mg PO • Gastrointestinal agents • Sucralfate (Carafate) - 1 g PO
Complications • hemorrhage • perforation • gastric outlet obstruction • gastric malignancy • the risk is approximately 2% in the initial 3 years • H pylori infection is associated with gastric lymphoma or mucosa-associated lymphoid tissue (MALT) lymphoma • malignancy should be strongly considered in the case of a persistent nonhealing gastric ulcer
Patient Education • Instruct patients to avoid NSAIDs. • Discourage alcohol consumption and cigarette smoking because these activities impair gastric mucosal protection.