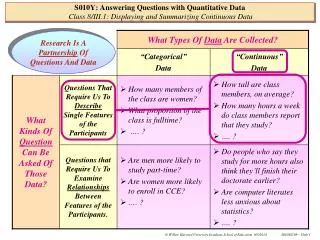
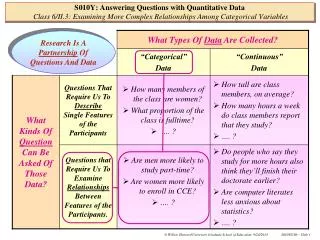
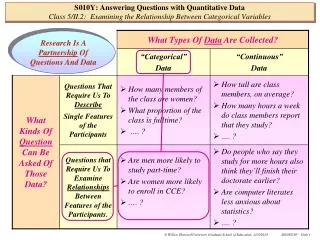
Using routinely collected data
Using routinely collected data. Dr Colin Fischbacher Information Services Division NHS National Services, Scotland. Talk outline. Potential role of routine data The current situation Primary care Secondary care Other sources Some conclusions. Why use routine data?.

Using routinely collected data
E N D
Presentation Transcript
Using routinely collected data Dr Colin Fischbacher Information Services Division NHS National Services, Scotland
Talk outline • Potential role of routine data • The current situation • Primary care • Secondary care • Other sources • Some conclusions
Why use routine data? • Considerable existing investment in data collection • Very large datasets with universal coverage • Marginal cost of adding ethnic group is relatively small • May increase profile of ethnic health inequalities
The vision: a routine system for collecting ethnic information • Based on self-definition • Collected with informed consent • Agreed categories, compatible with census • Collected once (probably in primary care) and transferable using standard data format • Collected by fully trained staff • Records everything needed for appropriate care (origin, religion, language, other?)
What could this provide? • monitoring uptake of services • targeting services • ensuring care is appropriate • policy development • performance management DOH. Collecting ethnic category data. Oct 2001
Drivers in Scotland • supporting patient focussed care • demonstrating compliance with legal obligations • investigating ethnic variations in health and health care provision
Recent developments in Scotland • Fair for all audit • ISD’s Equality and Diversity Information Programme • Diversity audit of health databases
The current situation:primary care • information on ethnicity not collected in Scotland • largely incomplete in England? • some local efforts based on mailshots • as in Liverpool – 58% coded • but very intensive (~70p/patient)
Issues in primary care • ethnicity as a clinical condition rather than a demographic characteristic • ensuring both standardisation and flexibility for data collection • availability of standard Read codes • ability to share data
The 2006 GMS contract • Includes 1 point in organisational domain for the collection of ethnic group information • . . . but does this include electronic recording? • . . . and do GP’s think it worthwhile? • . . . effect on awareness of the issue?
The current situation:secondary care • Field for ethnicity in Scottish SMR databases since 1996 • recorded in only 9.2% of hospital episodes (46.2% in one Ayrshire acute trust) • until 2004 used ethnic grouping that did not match the Census categories • “Although not mandatory it is strongly recommended that these items be completed whenever the information is available”
The current situation:secondary care • Ethnic monitoring in England • workforce (1991) patients (1995) • guidelines, training for staff • Completeness of HES variable
High HES completeness • Blackledge (BMJ 2003) reported higher incidence of heart failure among South Asians in Leicester using HES data • based on “self reported coding” for ethnicity; coverage “thorough”; validated using name search methods
Lower HES completeness • London Health Observatory review of data 1997/8 – 2000/01 found: • 37-38% ethnic group “not known” • Valid codes in around 66% of cases http://www.lho.org.uk/Download/3nhjq2aa2pnxxbmora3szquu/live/8907/EHIP_Update_4.doc
Ethnicity data incompleteness in HES (%) by Government Office Regions, England, 2003/04 Source:Indications of Public Health in the English Regions – Number 4: Ethnicity and Health. Association of Public Health Observatories, Oct 2005
Issues with HES • How are the data collected? • Can we ensure self-definition? • How often do systems default to “white”? • How well trained are staff? • Is the situation changing?
Other databases • Cancer registration (ethnic group available in 18% in Scotland) • Child health (CHI database in Scotland) – median 22% complete • Health Visitor/District Nurse databases • Lothian database said to be “100% complete” • Scottish Birth Record • Diabetes registers • GUM clinics (94% recorded)
Issues for other databases • All incomplete • Few or none match current census categories
Another “routine” source • Two health questions in the Census
Some other issues • Data standards (NCDDP in Scotland) [www.datadictionary.scot.nhs.uk] • Ambivalence among clinicians • Persistence of race as a clinical issue, eg in relation to haemo-globinopathies and diabetes
. . . some other issues • low salience in areas with small ethnic minority populations • informing patients about the reasons for collecting these data • ethnicity in the context of the wider diversity agenda
Conclusions • clear policy commitment • clear legal drivers • information vacuum • (with some variations) • ideal solution some way off • may be a place for interim approaches