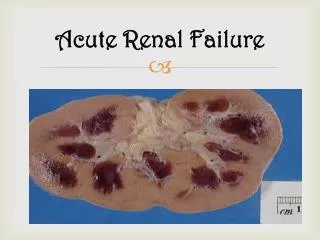
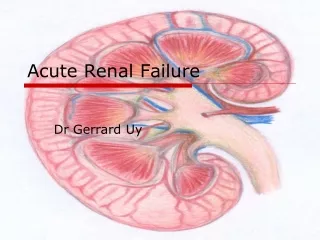
Acute Renal Failure
360 likes | 495 Vues
Acute Renal Failure (ARF) is characterized by a sudden decline in Glomerular Filtration Rate (GFR), leading to the kidneys' inability to excrete nitrogenous wastes and maintain fluid and electrolyte balance. Diagnosis is typically indicated by a 50% rise in serum creatinine. Key measurement formulas for renal function include Cockcroft-Gault and MDRD. ARF can be categorized as prerenal, postrenal, or intrarenal, each with distinct causes. Epidemiology shows ARF is common in hospitalized patients, carrying significant mortality risks, especially in those with underlying chronic kidney disease (CKD).

Acute Renal Failure
E N D
Presentation Transcript
Acute Renal Failure Jayanti Jasti, M.D. Emory Johns Creek Hospital
Definition Sudden decrease in GFR over a period of hours to days resulting in the failure of the kidney to excrete nitrogenous waste products and maintain fluid and electrolyte homeostasis. Clinically seen as rise in serum creatinine by 50% above baseline or increase by 0.5 mg/dl.
Measurement of Renal Function • Cockroft-Gault Formula GFR = (140-age in yrs) x Lean body wt(kg)/ S.Cr x 72 Adjustment made for the gender. • MDRD and modified MDRD Complicated, Laboratory reports it! Adjustment made for the gender and race. • Creatinine Clearance CrCl = U.Cr x U.vol/ S.Cr x 1440
Serum Creatinine as a marker • Steady state between creatinine production and excretion is required. • Creatinine production is dependent on muscle mass • Drugs which interfere with proximal tubular secretion of creatinine. Trimethoprim, Triamterene, Cimetidine,probenecid, amiloride etc., • Drugs which interfere with creatinine measurement in the lab. Ascorbic acid, cephalosporins etc.,
Blood Urea Nitrogen • BUN increases in volume depleted states due to reabsorption in the proximal tubules and in the collecting ducts. • BUN can be high with out RF. Hypercatabolic states, protein loading, steroids etc., • BUN can be low even with RF Severemalnourishment, liver disease, low protein diet etc.,
Types of ARF • ARF • ARF/CKD • Anuric (<50ml of urine output/day) • Oliguric (<400 ml/day) • Non-oliguric (>400 ml/day)
Etiology of ARF • Prerenal Renal hypoperfusion, no structural damage to the kidneys, Cr normalizes in 24-72 hours with correction of hypoperfused state. • Post-renal Obstruction to the urine flow, either unilateral/bilateral, intra-ureteral or extra-ureteral or bladder neck or intra-pelvis (renal pelvis). • Intra-renal Damage or inflammation within the kidney, may be primary renal or part of systemic disease.
ACEI and ARB associated ARF These medications cause ARF where angiotensin is playing a major crucial protective role in maintaining GFR by constricting the glomerular efferent arteriole. • Volume Depletion • B/L Renal artery stenosis • CHF • Diuretic use • Cirrhosis etc.,
NSAIDs associated ARF • Vasomotor in nature. • In the presence of conditions with increased renal vasoconstrictor activity like CHF, Cirrhosis, Nephrotic Syndrome, Sepsis, Volume depletion, HTN, CKD, DM, Anaesthesia etc., • No RF seen in Euvolemic conditions with normal kidney, liver and cardiac functions.
Postrenal ARF • Intra Ureteral Stones, Clots, Pyogenic debris, Sloughed papillae in analgesic nephropathy, sickle cell disease etc., • Extra Ureteral Malignancy, Retroperitoneal fibrosis, accidental ligation etc., • Bladder neck/Urethral BPH, Prostate Ca, Bladder Ca, Autonomic neuropathy with urinary retention, Urethral stricture, Blood clots/bladder stones.
Intrarenal ARF • Vascular • Glomerular • Interstitial • Tubular
Vascular causes of Intrarenal ARF • Large and Medium size vessels Renal artery thrombosis or emboli Renal vein thrombosis Polyarterial nodosa • Small vessel disease Atheroembolic phenomenon Microangiopathies like TTP, HUS, HELLP and malignant HTN.
Nephritis Hematuria Proteinuria (1-2gm/d) ARF May present as Rapidly progressive Glomerulonephritis Renal Biopsy to diagnose Nephrosis Massive proteinuria(>3gm/d) Minimal hematuria Uncommon to present as ARF Renal Biopsy needed to diagnose. Glomerular causes of Intrarenal ARF
Focal/diffuse edema and infiltration of the renal interstitium with inflammatory cells. Interstitial causes of Intrarenal ARF
Ischemia induced Shock Hemorrhage Sepsis Trauma Pancreatitis Nephrotoxin induced Drugs like IV contrast, Aminoglycosides, Ampho B, pentamidine, Acyclovir, Ehtylene Glycol etc., Endogenous Toxins in the case of Rhabdomyolysis, Hemolysis, uric acid nephropathy Tubular causes of Intrarenal ARF, Acute Tubular Necrosis
Epidemiology of ARF • Community acquired ARF seen in 1% of all hospitalized patients on admission.50% of those patients have underlying CKD. • Development of ARF in hospitalized patients is common and carries independent mortality risk. • In patients with normal renal function, the incidence of ARF is about 5%. • In patients with underlying CKD, the incidence is about 16%
Epidemiology of ARF Hospital acquired ARF • 40% is due to ATN • 15% related to medication associated ARF. • 10% due to contrast induced nephropathy. • AIDS associated ARF account for 5%.
Mortality associated with ARF • ICU associated ARF along with respiratory failure requiring hemodialysis, the mortality is >90%. • ICU associated ARF with out respiratory failure or hemodialysis, it is 72% • Non-ICU renal failure associated mortality is around 32%.
Evaluation of ARF • Careful History and tabulation of data including u.o, weights, vitals, medications etc.,. • Physical Examination findings including signs of vol. depletion etc., • Urinalysis • Urinary indices(Urine sodium, creatinine, FeNa, FeUrea etc.,)
Prerenal High SpGr No proteinuria/hematuria U.Na <20 U.Cr/P.Cr >40 U.Osm >500 FeNa <1% FeUrea <35% ATN Sp Gr 1.010 Variable proteinuria U.Na >40 U.Cr/P.Cr <20 U.Osm <350 FeNa >1% FeUrea >50% Urinary Indices
Urinalysis and Urine Sediment • UA positive for heme and proteinuria seen in Glomerular and Interstitial renal failure. • Urine eosinophils are seen in AIN, Atheroembolic disease etc., • Urine sediment positive for red cell casts seen in Glomerulonephritis. • UA bland in Post Renal ARF.
Laboratory Data • Peripheral eosinophilia in AIN, Atheroembolic disease. • Hypocomplementemia seen in SLE, MPGN, Atheroembolic disease etc., • Elevated ESR seen in Atheroembolic disease. • Serologies positive in glomerular diseases, like ANA, ANCA, Anti GBM, Hepatitis, HIV • Elevated LDH seen in RVT.
Laboratory Data (contd) • Thrombocytopenia with microangiopathic hemolysis seen in TTP, HUS etc., • Low Haptoglobin, High retic count seen in microangiopathic states. • Schistocytes (red cell fragmentation). • CPK, uric acid levels etc., to evaluate for rhabdomyolysis, uric acid nephropathy. • Evidence of hepatic insufficiency in diagnosing hepatorenal syndrome.
Imaging Ultrasound • Useful in Post renal ARF. • Early obstruction may not show significant hydronephrosis. • External obstruction encasing the whole urinary system may not show hydronephrosis, for e.g., retroperitoneal fibrosis. • U/S doppler useful in diagnosing Renal vein thrombosis.
Imaging (contd) CT scan • Useful for detecting stones, location of the obstruction, Tumours etc., Isotope renography • To evaluate the function significance of obstruction. • Done with lasix and Mag3 isotope for evaluatine obstruction.
Imaging (contd) Cystoscopy and Retrograde Pyelography • To evaluate patients with high clinical suspicion of obstruction esp., in unique cases of calculi, pyogenic debris, blood clots, bladder cancer etc., Renal Angigraphy • In emergent cases of anuria with suspicion of renal embolization.
Renal Biopsy • Only in patients with no clear etiology. • In patients with active urinary sediment (RBCs, red cell casts etc., ) • RPGN (rapidly progressive glomerulonephritis). • Refractory ATN with out recovery despite no further renal insults. • Acute Interstitial nephritis.
Management of ARF • Volume repletion with isotonic fluids to improve renal perfusion pressures in prerenal states. • CVP/ PAWP monitoring. • Supportive measures for sepsis with pressors, antibiotics etc., • Colloidal substances like blood products in hemorrhagic shock. • Management of heart failure by improving cardiac output.
Management (contd) • Drugs need to be dosed according to the renal clearance. • Electrolyte and acid base correction. • Renal diet, if K+ high. • Diuretics in overt fluid overload states. • Foley catheterization in bladder neck obstruction/prostatic obstruction.
Management (contd) • Avoid nephrotoxic agents like Contrast dye, NSAIDs, Aminoglycosides etc., • Also avoid ACEI/ARB unless the underlying problem is decompensated heart failure. • Nutritional support with parenteral or enteral feeding.
Management (contd) Renal replacement therapy Modes of dialysis: • IHD (Intermittent Hemodialysis) Quick removal of solutes over 3-4 hours, possible hemodynamic instability. ICU, hypotensive patients are probably not the best candiadtes for this type of HD. • CRRT (Continuous renal replacement therapy). Modality of choice in critically ill patients.
Management (contd) • Vascular access needed for Hemodialysis. • Peritoneal dialysis uncommonly used for managing ARF • It may be used in locations where IHD or CRRT are not available.