Bone Structure and Function
Bone Structure and Function. 5 Tissues found in a bone. Bone Cartilage Fibrous CT Blood Nerve. Regions of a Long Bone. Epiphysis: ends of a long bone Diaphysis: shaft of a long bone. Periosteum. Tough covering of a bone that is made of fibrous CT Helps form and repair bone tissue.


Bone Structure and Function
E N D
Presentation Transcript
5 Tissues found in a bone • Bone • Cartilage • Fibrous CT • Blood • Nerve
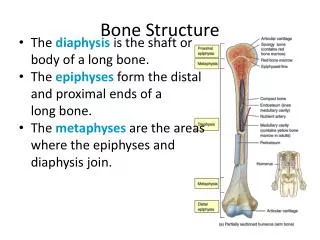
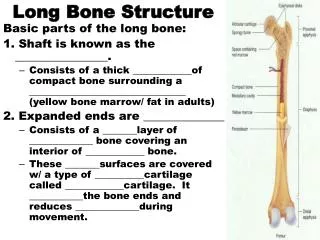
Regions of a Long Bone • Epiphysis: ends of a long bone • Diaphysis: shaft of a long bone
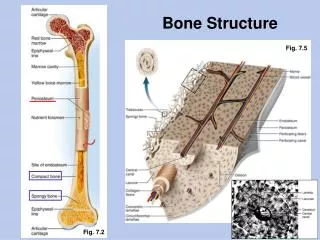
Periosteum • Tough covering of a bone that is made of fibrous CT • Helps form and repair bone tissue
Bone Features • Process: sites for tendons and ligaments to attach • Groove/opening: passageway for nerves and blood vessels • Depression: articulations of bones
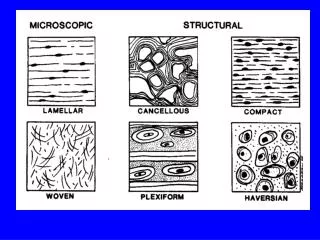
Diaphysis No spaces Tightly packed Epiphyses Branching bony plates with spaces Compact vs Spongy Bone
Medullary Cavities • Center of compact bone-diaphysis • Filled with marrow
Osteocytes • Bone cells
Lacunae • Bony chambers where bone cells are located
Osteonic Canals (Haversian Canals) • Open canal with bone cells around it
Canaliculi • small tubes in bone that contain cellular processes involved in communication
Collagen & Inorganic Salts • Collagen: gives bones strength and resilience • Inorganic salts: make bones hard and resistant to crushing
Osteon • Unit in bone composed of osteocytes and intercellular material aroun an osteonic canal • Many osteons cemented together form bone
Osteonic Canals • Contain 1-2 blood vessels (capillaries) and a nerve with loose CT
Perforating Canals (Volkmann’s) • Connect osteonic canals
Is Spongy bone composed of osteocytes? • Yes • Are they organized around osteonic canals? • No • How is spongy bone nourished? • Substances diffuse into canaliculi that lead to the surface
Bone forms by replacing CT:Two ways this occurs • Intramembranous bones originate between layers of CT (skull) • Endochondral bones begin as cartilage that is later replaced by bone
Development of intramembraneous bones: • 1. Develop from layers of CT at future bone sites • 2. CT cells enlarge and differentiate into osteoblasts (bone building cells) • 3. Osteoblasts within membrane layers form bone tissue • 4. Spongy bone forms • 5. Periosteum form from membrane tissue outside developing bone • 6. Osteoblasts on inside form compact bone over spongy bone
Development of Endochondral bones: • Develop from masses of hyaline cartilage • In the primary ossification center: 1. Cartilage grows athen begins to change 2. In the diaphysis-cartilage breaks down and disappears (periosteum is forming) 3. BV’s and osteoblasts invade disintegrating cartilage-spongy bone forms
Osteoblasts from periosteum deposit compact bone around the primary Os. Center • Epiphyses remain cartilaginous and continue to grow • In the Secondary Ossification Centers: 1. SOC’s appear in epiphyses-spongy bone forms in all directions 2. Band of cartilage between the POC and SOC’s is the epiphyseal disk (growth plate-site of mitosis) Calcium salts accumulate & matrix calcifies
Types of bone cells: • Osteoblasts-bone building cells • Osteocytes-bone cells formed rom osteoblasts
Osteoclasts • Large multinucleated cells that break down the calcified matrix by secreting an acid that dissolves calcified substances • Originate in bone marrow
Breaks in the epiphyseal disk of a young child: • May cause bone growth to stop or cause uneven growth
Osteoclast and osteoblast remodel bone throughout life by: • Osteoclast reabsorb bone tissue and osteoblast replace bone • These actions are contolled by hormones
Bone Cancer • Abnormal osteoclasts destroy bone tissue • However, prostate cancer stimulates osteoblasts activity which causes the formation of new bone
Fracture • Break in a bone
Hematoma • Blood clot
How bone heals • 1. BV’s rupture and hematoma forms • 2. Vessels in surrounding tissue dilate & swell (inflammation) • 3. Developing BV’s & osteoblast invade the hematoma and form spongy bone • 4. Fibroblasts produce firbocartilage
5. Phagocytes remove blood clot & dead or damaged cells • 6. Osteoclasts appear and reabsorb fragments • 7. Fibrocartilage fills the gap-forms a cartilage callus • 8. Cartilage callus is replaced by a bony callus • 9. Osteoclasts reshape the bone
4 main functions of bone • 1 shape & support • 2 protect • 3 body movement • 4 house marrow & salts
Hematopoiesis • Blood cell formation
After bones develop, blood cells are made in the • Liver • Spleen • Bone marrow
3 locations of marrow • Medullary cavity of long bones • Irregular spaces of spongy bone • Osteonic canals of compact bone
Red marrow forms: • Red blood cells • White blood cells • Platelets
Hemoglobin • Protein pigment that makes blood red • High affinity for oxygen
Yellow marrow • With age, yellow marrow replaces much of the red marrow • Yellow marrow stores fat and does not produce blood cells
6 locations of red marrow in adults • 1 spongy bone of skull • 2 ribs • 3 sternum • 4 clavicle • 5 vertebrae • 6 pelvis
Most calcium in bone tissue is in the form of • Calcium phosphate
Low blood calcium: • Stimulates osteoclasts to break down bone • When high-it stimulates osteoblasts to from bone tissue
Osteoporosis • Loss of bone and mineral content from bone • Bones develop spaces that fill with fibrous and fatty tissues
Factors that increase risk for osteoporosis: • 1 low calcium intake • 2 lack of physical exercise • 3 decrease in blood estrogen • 4 alcohol, cigarettes, genes
What can you do to reduce bone loss? • 1 1000-1500 mg of calcium daily • 2 exercise regularly • 3 estrogen replacement
Procedure for a bone marrow transplant involves: • 1 finding a match • 2 remove marrow (or stem cells) from donor • 3 destroy marrow of recipient • 4 insert donor marrow (stem cells)