Rheumatoid Arthritis
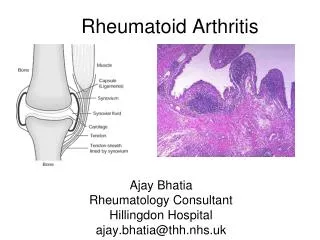
Rheumatoid Arthritis. Dr Jaya Ravindran Consultant Rheumatologist Walsgrave Hospital. RHEUMATOID ARTHRITIS. Background Chronic erosive symmetrical arthritis (extra-articular features) 1% population 2-3X more common in women Peak age onset 3rd to 5th decade


Rheumatoid Arthritis
E N D
Presentation Transcript
Rheumatoid Arthritis Dr Jaya Ravindran Consultant Rheumatologist Walsgrave Hospital
RHEUMATOID ARTHRITIS Background • Chronic erosive symmetrical arthritis (extra-articular features) • 1% population • 2-3X more common in women • Peak age onset 3rd to 5th decade (Macgregor et al 1998 in Klippel and Dieppe Rheumatology) • Erosions occur early in disease (Fuchs et al 1989 J Rheumatol)
RHEUMATOID ARTHRITIS Background • Functional decline - 10 years work disability 40-60% • (Jantti et al 1999 Rheumatol) • Premature mortality comparable to coronary artery disease and Hodgkin’s lymphoma • (Pincus et al 1994 Ann Intern Med) • Economic burden £1.3 billion /year in UK • Early treatment works and RA responds better, earlier • (Munroe et al 1998 Ann Rheum Dis)
REFER EARLY! Who and when to refer (In theory) • ARA 1987 Revised Criteria for the classification of Rheumatoid arthritis • At least 4 criteria must be filled • Morning stiffness > 1 hour > 6 weeks • Arthritis of 3 or more joints PIP, MCP, wrist elbow, knee, ankle, MTP > 6 weeks • Arthritis of hand joints wrist, PIP, MCP > 6 weeks • Symmetric arthritis at least one area > 6 weeks • Rheumatoid nodules • Positive Rheumatoid factor • Radiographic changes
REFER EARLY! In practice • Anyone with > 3 inflamed joints with symptoms > 6 weeks • At presentation • rheumatoid factor negative in 60% • normal x-rays in 50% • no acute phase in 60% • (Green et al 2002 Collected reports on the Rheumatic diseases) • Atypical presentations - polymyalgic, palindromic, monoarthritis
Useful Baseline Investigations • ESR/PV/CRP • FBC • U&E/LFT • RhF (CCP) • ANA • Urine dip • Radiology (Hands and Feet) • (Synovial fluid analysis)
Clinical spectrum Articular • PIP, MCP, wrists, elbows, shoulders, knees, ankles, MTP • C-Spine • DIP usually spared • Early changes • fusiform swelling PIP, MCP and wrist swelling
Clinical spectrum Articular • Later deformities • Swan neck & Boutonniere • Z-shaped thumb • Ulnar deviation (MCP) • Volar subluxation (wrist) • Later deformities • Hammer, overlapping and claw toes • Splayfoot, valgus deviation (MTP) • MTP head subluxation • pes planus, valgus hindfoot
Clinical spectrum • C/spine • atlantoaxial subluxation • subaxial disease • Myelopathy • Tenosynovitis and tendon rupture
Extra-articular • 40% patients • Sero-positive • Nodules • Systemic • weight loss, low-grade fever, lymphadenopathy, fatigue • Ocular • Keratoconjunctivitis sicca • scleritis (scleromalacia perforans) • episcleritis • Pulmonary • Alveolitis and lung fibrosis, • nodules • pleural effusions • BOOP • Caplans
Extra-articular • Cardiac • Carditis, conduction disturbances, coronary arteritis • Vasculitis • ischaemia and infarction (eg leg ulcers, mononeuritis multiplex) • Felty’s syndrome • Amyloidosis • nephrotic syndrome, cardiac, malabsorption • Anaemia • chronic disease & drugs • Osteoporosis
Management of RA Multidisciplinary • Effective in RA • Vliet Vlieland et al 1997 Br J Rheumatol • GP, rheumatologist, nurse specialist, PT, OT, podiatrist, orthotist, surgery • Education - team, leaflets, resources from organisation/support groups • OT – activities of daily living, equipment and adaptations, splinting • PT – dynamic exercise therapy and hydrotherapy • Podiatry and orthotics – insoles, shoes, intervention for callosities
Management of RA Surgery • Joint arthroplasty • Tendon repair • Synovectomy • C/spine stabilisation
DMARDs (adapted from BSR 2000 and ARC 2002 guidelines) • Monotherapy used in majority of patients • Combination therapy and use of steroids • evidence less clear-cut and perhaps reserved for poor responders/aggressive disease • Steroids - bridge therapy’ • Onset of action 6 weeks to few months • Monitoring – “joint” responsibilty • GP / Rheumatologist / patient • local / national guidelines / shared cared monitoring cards • trends important
Toxicity Bone marrow toxicity • Thrombocytopenia, leucopenia or pancytopenia • WBC<4 (neut<2) • Plts<150 • Sorethoat, mouth ulcers, flu-like illnesses, bleeding, bruising • Isolated anaemia very rare and tends to be due to other causes. • Methotrexate, sulphasalazine, gold, azathioprine, penicillamine, cyclosporin, leflunomide, cyclophosphamide, chlorambucil
Toxicity Liver toxicity • Raised ALP common in active RA and by itself does not usually suggest liver toxicity • >2 X increase in AST or ALT or unexplained falling albumin • Methotrexate, sulphasalazine, azathioprine, cyclosporin, leflunomide
Toxicity Renal toxicity and hypertension • >1+ blood and/or protein • quantify proteinuria (gold, penicillamine) • >30% rise in creatinine (cyclosporin) • hypertension (leflunomide, cyclosporin)
Toxicity Other • Mucocutaneous and GI • Pulmonary – dry cough and dyspnoea • MTX, SSZ, gold
Biologics • TNF alpha blockade • NICE guidelines • Infections esp TB • ?Malignancy • Others eg MS,CCF