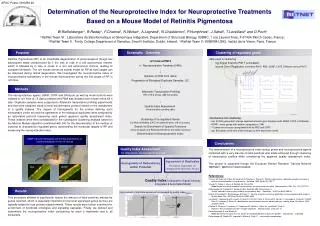
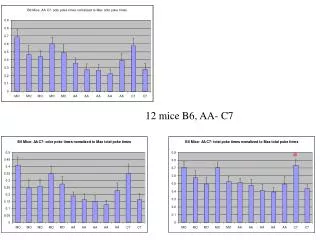
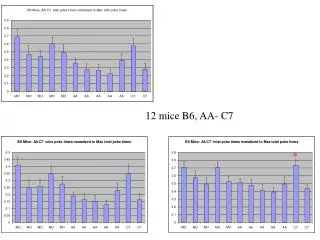
Group B6
Syphilis , Chlamydia and Gonorrhea : Bacteriology, Epidemiology, Pathogenesis, Clinical Manifestations, Diagnosis and Treatment. Group B6. Epidemiology - Syphilis. Epidemiology - Syphilis. Epidemiology - Syphilis. Epidemiology - Syphilis. Epidemiology - Syphilis. Epidemiology - Syphilis.

Group B6
E N D
Presentation Transcript
Syphilis, Chlamydia and Gonorrhea: Bacteriology, Epidemiology, Pathogenesis, Clinical Manifestations, Diagnosis and Treatment Group B6
Transmission - T. pallidum • “teeming with spirochetes” • Transmission • Sexually engaging a person with lesions • Mother Baby • In utero • Congenital syphilis
Pathogensis – T. pallidum 3-6 wks post-incubation
Pathogensis – T. pallidum Chancres resolve w/in wks even w/o treatment Some move directly to 2 syphilis Period in which organism replicates & spreads throughout body 4-10 wks after first signs of primary lesions If left untreated, can move to 3 syphilis Latent Period
2 Syphilis Sites of replication Lymph nodes, mucous membranes, liver, joints, muscle, skin • Spirochete replication dissemination • Manifestations(variable) • Malaise & Fever • Myalgias & Arthralgias • Lymphadenopathy • Rash & Lesions • Rash present on ENTIRE body (inc. palms & soles) • Lesions present in different stages (macular, papular, pustular) • Contains treponemes Condylomatalata gray/white lesions painless highly infectious warm/moist areas 2 syphilis will heal w/in weeks w/o treatment; if left untreated latent &/or 3 syphilis
Latent Syphilis • Early Latent Syphilis • Less than 1 yr after 2 syphilis • Relapse possible • PT may have relapse of 2 syphilis lesions/symptoms • CONTAGIOUS • Late Latent Syphilis • Less than 1 yr after 2 syphilis • No symptoms • Not as contagious PT is seropositive during latent phase, thus blood test is required for diagnoses. Latent stage may persist for years (10-20yrs); if left untreated 3 syphilis
3 Syphilis • Rare ~1/3 of untreated PTs • Slow, chronic inflammatory damage d/t to reaction of spirochetes in tissue • 3 categories • Gummatous syphilis • Cardiovascular syphilis • Neurosyphilis • Gummatous syphilis • Granulomatous lesions • Center = necrotic tissue • Form in (but not limited to) liver, bones, ski • Cardiovascular syphilis • Aneurysm formation in ascending aorta • Neurosyphilis • CNS invasion syphilitic meningitis • Damage to blood vessels in CNS meningovascular syphilis • Parenchymalneurosyphilis tabesdorsalis & general paresis
Clinical - Syphilis • Aka The Great Imitator • Primary syphilis characterized by a firm, round, small, PAINLESS, chancre • Usually a single lesion but there may be multiple • Occurs at the site where the treponeme invaded • The chancre lasts 3 to 6 weeks
Clinical - Syphilis • Secondary syphilis is characterized via a skin rash and mucous membrane lesions • Presents as rough, red/brownish spots on palms and soles • Other symptoms are fever, lymphadenopathy, myalgias, weight loss, and fatigue • These symptoms will disappear with or without treatment
Clinical - Syphyilis • Tertiary syphilis occurs many years after the secondary phase • Treponemes damage the brain, eyes, heart, vessels, bones, joints, and many internal organs • Patients may develop aortitis, hoarseness, Argyll Robertson’s pupil, gummas, and TabesDorsalis
Diagnosis – T. pallidum • Dark Field microscopy serology tests: • Fluorescent Treponemal Antibody Absorption (FTA-ABS) • Specific • Veneral Disease Research Lab (VDRL) • Nonspecific • detects reaginAb against cardiolipin
Diagnosis – T. pallidum • Serology • Non-treponemal antibodies • VDRL & PRP • Serology • Treponemal antibodies • FTA-ABS & MHA-TP
Treatment – T. pallidum • Drugs: • Benzathine penicillin G
Virulence Factors – Chlamydia • Intracellular organism • Downregulates MHC-I • LPS • Promotes inflammation via TLR-4 activation (inducing IL-1 & -8 secretion) • Prevents fusion of endosome with lysosome • Provides a “home” • Persistent state • Allows Chlamydia to persist in face of IFN-gamma • Nutrient up-take • Via Type 3 secretion system which serves as a “transport channel”
Clinical - Chlamydia • Clamydia trachomatis • A,B,C serotypes induce chronic infections and blindness due to follicular conjunctivitis • D,K serotypes cause urethritis/PID, ectopic pregnancy, neonatal pneumonia(staccato cough), or neonatal conjunctivitis • L1,L2,L3 result in lymphogranulomavenereum
Clinical - Chlamydia • Known as the silent STD since many are asymptomatic • Women may have burning upon urination or vaginal discharge • Untreated infections may lead to PID or ectopic pregnancy • Leading cause of pneumoniae and conjunctivitis in neonates
Clinical - Chlamydia • Men may have discharge from penis or burning upon urination • Rarely, Reiter’s syndrome may occur including arthritis, skin lesions, and inflammation of the eye and urethra
Diagnosis – C. trachomatis • Cell culture • Non-culture Direct Detection methods: • Direct Fluorescent Antibody tests (DFA) test) – direct at elementary bodies • Enzyme Immunoassays (EIA) • Nucleic Acid Hybridization Tests • Nucleic Acid Amplification Tests – most sensitive • Serologic Tests
Treatment – C. trachomatis • Drugs • Azithromycin • Ceftriaxone + Doxycycline = concurrent N. gonorrhea • Erythromycin (oral) = Neonates
Virulence Factors – N. gonorrhea • Adherence/Uptake • Pili • Opa proteins • Antigen variation/antigen phase variation • Porin 1 • Enzymes/Toxins • LOS • IgA protease
Pathogenesis – N. gonorrhea • Virulence Factors • Adherence/Uptake • Pili • Opa proteins • Antigen variation • Movement across cell • Porin 1 • Enzymes/Toxins • LOS • IgA protease
Clinical - Gonorrhea • Men may have burning upon urination and white, yellow, or green discharge • Painful or swollen testes may also occur as well as epidydimitis leading to infertility • Women are often asymptomatic but could experience burning upon urination • Untreated infections lead to PID in women and septic arthritis in both sexes • Pregnant women may also transmit gonorrhea to their baby via passage through birth canal resulting in blindness and joint infections
Diagnosis – N. gonorrhoeae • Nucleic acid amplification tests (NAAT) – most sensitive (PCR) • Nucleic acid hybridization test (co-infection Chlamydia) • Culture: Thayer Martin agar / chocolate agar • Gram stain: diplococci within neutrophils
Treatment – N. gonorrhoeae • Drugs: • Ceftriaxone + Azithromycin • Ceftriaxone + Doxycycline = concurrent Chlamydia • Erythromycin (eye gtts) = prophylaxis in neonates • Resistance: • Penicillin • Fluoroquinolones – Ciprofloxacin or Levofloxacin (Levaquin) • Vaccines: • NONE (varied pili antigens)
Antibiotic Resistance – N. gonorrhoeae • Beta-lactamases • Efflux pumps • Mutations: • Penicillin-binding proteins • DNA gyrase and topoisomerase • Porins
Q1 A 34-year-old male presents to your ofice with a painless penile ulcer several weeks after an episode of unprotected sexual intercourse.(bad luck?!) Which of the following is most useful in diagnosing Treponemapallidum infection in this patient? • Ulcer exudate microscopy after Gram staining • Ulcer exudate microscopy with darkfield illumination • Ulcer eudate cultures on enrichment media • Blood culture on differential media • Antitoxin detection in the serum