Background of NEMT in RI
Rhode Island Medicaid Non-Emergency Medical Transportation Program Rhode Island House Committee on Oversight March 23 rd , 2017. Background of NEMT in RI. Prior to State Transportation Broker Contract

Background of NEMT in RI
E N D
Presentation Transcript
Rhode Island Medicaid Non-Emergency Medical Transportation ProgramRhode Island House Committee on OversightMarch 23rd, 2017
Background of NEMT in RI • Prior to State Transportation Broker Contract • RIPTA provided non-Emergency Medical Transportation (NEMT) services between their Fixed Routes and Elderly Paratransit contracts. • RIPTA subcontracted with taxi companies • Highest level of service provided was wheelchair • Ambulance service coordinated through EOHHS • RIPTA invoiced State monthly for the services under the various categories for set amount per ride • Bus passes previously received at supermarket (LogistiCare assumed responsibility in December of 2014) • Changes Needed • CMS required Medicaid to contract with NEMT Broker to ensure transportation services met medical necessity criteria • Improved network coverage and better coordination of transportation services
Background of NEMT in RI State Broker Procurement Model • NEMT Broker Procurement completed in late 2013 • Five bids –successful vendor was LogistiCare • LogistiCare currently operates in 42 states Current LogistiCare Contract • Three year-fully capitated arrangement with actuarial set rates for Medicaid Population *Capitation payment is equal to the contracted member months estimates times the agreed upon contracted price per member. (Per Member Per Months) PMPMs currently for the SFY 17: Rite Care & Medicaid Expansion Populations at $7.07 Aged/Blind/Disabled population at $ 22.99 CNOM at $20.64. Elderly program has a fixed annual funding of $2.4 million. ** Estimates –Actual amounts based on number of members
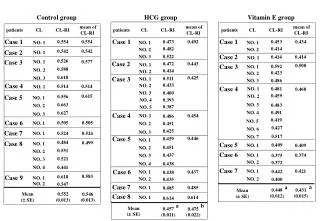
Medicaid NEMT Utilization *All other visits include: TANF Specialized Transportation for Medical Appointments, Physical Therapy, Physician Services, Psychiatry, Dental, Social Care Counseling and Eye Doctor
Non-Medicaid Elderly NEMT Utilization • * All other visits are: Eye Doctor, Radiation Treatment, Wound Care, Substance Abuse, Cardiac Rehab and Routine Services
EOHHS Oversight • EOHHS holds bi-weekly face-to-face meetings with LogistiCare to review operational, systems & financial functional areas, transportation provider network access, along with quality improvement activities. • EOHHS and LogistiCare work closely on a day-to-day basis to discuss any challenges (access, weather, etc.) that may have arisen. • LogistiCare employs 60 individuals locally for the Customer Representative Center, Quality Assurance and Mass Transit Units. • Training programs for transportation providers and LogistiCare’s staff are closely monitored. • EOHHS has an assigned team of individuals with various specialties to provide contract monitoring, and quality improvement & performance outcome oversight. • EOHHS is evaluating options to improve the quality of service for clients.
EOHHS Oversight • EOHHS and LogistiCare report to several external committees and/or multi-agency groups. • Currently report monthly to a meeting hosted by the Alliance for Better Long Term Care (last Wednesday of the Month) • The Lt. Governor’s Long Term Care Coordinating Council (Monthly). • Upon request the EOHHS & LogistiCare present to various groups as needed. • May 2016 – LogistiCare Outreach Meeting with SA MH Leadership Council RI • March 2016 – Training for Nurse Care Managers at Neighborhood Health Plan RI (Several multi sessions) • December 2015 – Transportation Outreach at Miriam Hospital (HIV Program) • April 2015 – Neighborhood Health Plan of RI Presentation • June 2014 – Transportation Outreach at RI Partnership for Home Care at Pocasset Bay (NW Links) • June 2014 – DEA sponsored the Academy training for “information and referral” specialists – Johnston Senior Center.
Complaint Data • Consistent with the provisions of its contract with EOHHS, LogistiCare tracks and manages complaints filed against its service delivery. • During this SFY16, LogistiCare logged 11,868 complaints in providing both Medicaid and non-Medicaid Elderly transportation services. • These complaints represent roughly 1% of all trip reservations made during this twelve month period.
Performance Standards • The State may hold back up to 2% of monthly payments if Broker’s performance falls bellow quality standards, including but not limited to the standards listed below: • To date, LogistiCare has substantially met these standards and EOHHS has not withheld monthly payment due to poor performance.
Deborah Florio Deputy Medicaid Director EOHHS • 401.462.0140 • Florio.deb@ohhs.ri.gov