The Birth Process
The Birth Process. Mamie Guidera, CNM, MSN Carol O’Donoghue, CNM, MSN, MPH. Normal Labor and birth: Objectives . Introductions Physiologic labor and birth: the basics Phases of labor Birth video The P’s: Power, passageway, passenger, etc. Briefs:


The Birth Process
E N D
Presentation Transcript
The Birth Process Mamie Guidera, CNM, MSN Carol O’Donoghue, CNM, MSN, MPH
Normal Labor and birth: Objectives • Introductions • Physiologic labor and birth: the basics • Phases of labor • Birth video • The P’s: Power, passageway, passenger, etc. • Briefs: • American birth & (some of the) influences: • Where births take place • Cultural expectations of pain management • A word on Fetal Monitoring
Here’s the truth: Childbirth is not only a physiologic phenomenon, but a cultural/sociological experience. So before you walk onto the Labor Floor, ask yourself: • Where/how did you first learn about how a baby is born? What do you know about your own birth? • Who (family member, friends, healthcare provider) or what (your medical training, book, television show, movie) has influenced your perception of labor? What birth stories come to your mind first? • Is there such a thing as “good” pain? If you are an athlete, have you ever sought out physical discomfort? Why? • Have you ever been in pain? How did you deal with it? • What do you think is the role of the healthcare provider in birth?
Birth in the United States • Site of birth • Hospital • Birth Center • Home • Model of birth • Medical Model • Midwifery Model
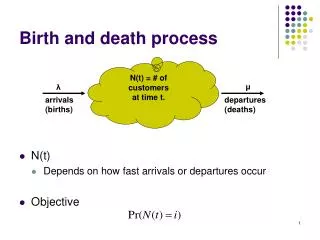
Stages of Labor • First stage: early, active, transition • Dilatation • Second stage • Pushing and birth • Third stage • Delivery of placenta • Fourth stage • Postpartum
Birth Video • Observe stages and phases of labor • Observe Maternal Behaviors!
True vs False Labor: Williams Obstetrics (22nd edition) True Labor: • Contractions occur at regular intervals • Intensity gradually increases • Discomfort is in the back and abdomen. • Cervix dilates. • Discomfort is not stopped by sedation • Contractions are irregular • Intensity remains the same • No cervical dilatation • Discomfort relieved by sedation
Length of first stage labor in healthy nulliparous and multiparous childbearing womenadapted from Albers L. (2007)bold = nullips, italics = multips
What are the signs and symptoms of impending labor? Bishop’s Score Position Consistency Effacement Dilatation Fetal station and part Importance of cervical status Physiological Preparation for Labor
Theoretical Maternal factors Progesterone Estrogen Oxytocin Prostaglandin Psyche Fetal factors Fetal cortisol Artificial Cervical exam Stripping of membranes Prostaglandins Artificial rupture of membranes Sex Nipple Stimulation Initiation of Labor
You tube!- dilatation and the cardinal movements http://www.youtube.com/watch?v=Xath6kOf0NE&feature=PlayList&p=6603A45DF81B89A9&index=38&playnext=2&playnext_from=PL • http://www.youtube.com/watch?v=Xath6kOf0NE&feature=PlayList&p=6603A45DF81B89A9&index=38&playnext=2&playnext_from=PL
Dilatation Effacement Cervix Station Contraction pattern Membranes Duration What are the characteristics of each? What are frequent maternal behaviors? Pain management? Early or Latent Phase, Active phase, Transition…
Woman/Fetus Power Passageway Passenger Position Psyche Providers/Support Persons: Patience Persistence Practice/ Pain Relief Psyche The Ps of Labor
Power: Influences • Uterine force • Nutrition and fluids • Rest/Fatigue
Passageway • Soft tissues • Cervix • Vagina • Perineum
Cervical Examination: examining the passageway • Dilatation • Effacement • Station • Position • Consistency • Presenting part • Status of membranes
Passenger • Size of passenger • Number of passengers • Position of passenger: • Presentation • Lie
Passenger • Descent • Fetal head journey through the pelvis until Crowning • Flexion • Fetal head tucks into chest • Important so that smallest diameter of head presents • May depend on pelvic type/shape
Passenger: Station • Engagement • AKA “dropping” or “lightening” • At the level of ischial spines = 0 station • Above ischial spines • -5 to -1 • -5 = unengaged • Below ischial spines • +1 to +5 • +5 = crowning
Passenger: Cardinal Movements • http://www.youtube.com/watch?v=Xath6kOf0NE&feature=PlayList&p=6603A45DF81B89A9&index=38&playnext=2&playnext_from=PL • Engagement – ischial spines • Descent Flexion Internal rotation- OT to OA • Extension Restitution- baby head realigns with body • External rotation • Expulsion – the body
Passenger: Position • The relationship of a site of the presenting part to the location on maternal pelvis • Examples: LOA, ROP, RMT, LSA, etc. • Asyncliticism: lateral deflection of the head with regards to the sagittal suture • Anterior or posterior
Position: Fetal and Maternal • Most common position for labor and birth? • Best position for labor and birth? • Worst position for labor and birth? • …..think mother and baby
Health care provider Support person(s) Family Friend Doula …let’s talk about this… Woman giving birth Knowledge Fear Support Trust Self Provider Beliefs, values, culture Psyche
From 10 cm to birth of baby Pushing or expulsion Contraction pattern Duration Second Stage of Labor
Perineal management (keep your hands off Mirror Ask mother to feel the baby’s head Stay focused on woman, not tasks Birth
Third Stage of Labor • Birth of the placenta • 5 to 30 minutes….or more • Signs of placental separation • Inspection • A word on Active Management of Third Stage • Pitocin and prevention of postpartum hemorrhage
Two Methods of Third Stage Management • Physiologic (“expectant”) management • Oxytocics are not used • Placenta is delivered by gravity and maternal effort • Cord is clamped after delivery of the placenta • Active Management • Oxytocic is given • [Cord is clamped] • Placenta delivered by controlled cord traction (CCT) with counter-traction on the fundus • Fundal massage after delivery of placenta
Part II: Reality & modern hospital birth: pain management, monitoring, interference with physiologic birth
Physiology of labor pain: First stage • Uterine contractions: • Myometrial ischemia Causes release of potassium, bradykinin, histamin, serotonin • Distention of lower uterine segments and cervix • Stimulates mechanorecoptors Impulses follow sensory-nerve fibers from paracervical and hypogastric plexus to lumbar sympathetic chain Enter dorsal horn of spinal cord at T10-12, L1
Pain pathways during labor: Late first and Second stage • Transition associated with greater nocioceptive input related to increased somatic pain from vaginal distention • Distention of vagina, perineum, pelvic floor, stretching of pelvic ligaments • Pain signal transmitted to spinal cord via S2-S4 (includes pudendal nerve)
Walking/Movement Hydrotherapy Back Rubs Birth Ball, toilet Maternal Preference Analgesia/ Anesthesia Others? Pain Management in Active Labor
One-on-One Labor Support: the evidence • If a doula was a drug, it would be considered unethical not to give it.” John Kennell, MD
Continuous Labor Support • Non-medical care by a trained person • Different definitions/criteria depending on studies: • “minimum of 80%” presence • presence “without interruption, except for toileting” • Various terms: doula, labor assistant, birth companion, monitrice • May refer to husband or untrained female companion