Heart Failure 2013
E N D
Presentation Transcript
Definition • Inability of the heart to supply blood to meet metabolic demands of tissues resulting in inadequate tissue perfusion and volume overload
Heart Failure • Implies “biventricular failure” • Origin usually left sided • Left ventricle (LV)enlarges capacity, muscle size & shape = “ventricular remodeling” • LV weakens decreased ejection of blood, decreased stroke volume, decreased cardiac output
Incidence • 5 million cases • 660,000 new cases/year • Most common discharge diagnosis age >65
Causes of Heart Failure • Myocardial infarction • Pulmonary embolism (RV failure) • Cardiomyopathy (both RV & LV failure) • Mitral insufficiency (LV failure) • Aortic regurgitation/stenosis (LV failure) • Hypertension (LV failure) • Volume overload • Myocarditis • Infections/toxins
Mechanism of Failure • Decline in cardiac function decreased cardiac output • Drop in cardiac output decreased ejection fraction • Ejection Fraction= percentage of blood left ventricle pumps out with each beat • Normal= 55-70% • <40% = impaired function
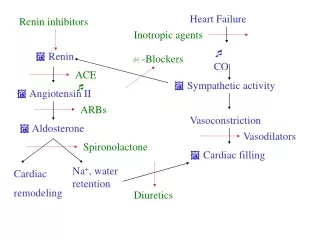
Inciting Event Increased myocardial demand Ventricular Remodeling Vasoconstriction (renin-angiotensisn) Decreased cardiac output Sodium & water retention (Aldosterone) Neurohormonal Activation Sympathetic increase in heart rate & contractility Increased intravascular volume Increased wall stress and afterload Chronic Congestive Failure
Etiology • Cardiac Output dependent on: • Preload: amount of blood in left ventricle (LV) • Afterload: pressure against which LV must eject • Contractility: strength of contraction • Coordination of contraction between atria/ventricles • Heart Rate: amount of time available for filling and emptying ventricles
Systolic Dysfunction“Poor Contraction” • Heart enlarges/does not contract normally • Decrease in muscle strength (thin walls) • Forward blood flow decreases systemic hypoperfusion • Stroke volume & ejection fraction decrease (EF<40%) • Pulmonary congestion
Diastolic Dysfunction“Impaired Filling” • Inability of the ventricle to fully relax • Increased pressure & volume in ventricle • Pressures back up to pulmonary veins pulmonary congestion • Stroke volume reduced • Echo: normal EF?, left atrial enlargement, pulmonary hypertension, heart wall abnormalities, right ventricular dilation
Clinical Manifestations • Left sided Failure (“Forward Failure”) • Blood backs into pulmonary veins & capillaries lung congestion • Dyspnea on exertion • Paroxysmal nocturnal dyspnea • Orthopnea • Pulmonary edema • Crackles • Cough • Tachycardia • S3, S4, systolic murmur • Insomnia, restlessness
Clinical Manifestations • Right Sided Failure (“Backward Failure”) • Elevated pressures & congestion in systemic veins & capillaries • Peripheral/Dependent edema • Weight gain • Liver congestion • Distended neck veins • Abnormal fluid in body cavities • Pleural, abdominal • Anorexia & nausea • Nocturia • Weakness
Assessment • History of symptoms • Limits of activity/response to rest • Peripheral pulses: quality, character • Inspect/palpate precordium for lateral displacement of point of maximum impulse • Sleeping patterns/sleep aids
Stages: American College of Cardiology/ American Heart Association
Management • Inotropes • Improve contractility, stroke volume, ejection fraction, cardiac output • Increase myocardial oxygen consumption • Dobutamine, milrinone, digoxin • Biventricular pacing: cardiac resynchroniztion therapy (CRT). Synchronizes LV systolic function so that LV walls contract at same time
Management • Reduction of Afterload • Decrease in resistance of blood, valves, blood vessels • Decreases work of left ventricle • Improved contractility, stroke volume, cardiac output • Angiotensin Converting Enzyme (ACE) inhibitors (captopril, enalapril) • Calcium Channel Blockers (nifedipine,verapamil) • Beta Blockers (metoprolol) • Angiotensin Receptor Blockers (ARBs) (valsartan, losartan)
Management • Reduction of Preload • Diuretic therapy • Loop Diuretics: lasix, bumex • Thiazide Diuretics: hydrochlorothiazide • Potassium Sparing: spironolactone, triamterene • Venodilators (nitroglycerin) • Fluid & sodium restriction
Interventions • Maintain adequate cardiac output • Physical/emotional rest • Evaluate for progression of left sided failure • Lowered systolic pressure • Narrowing of pulse pressure • Alterations in strong/weak pulsations • Auscultate heart sounds
Interventions • Improve oxygentation • Raise head of bed • Auscultate lung fields • Observe for respiratory distress • Small frequent feedings • Oxygen as needed
Interventions • Restore fluid balance • Diuretics • Strict I & o • Daily weight • Assess for weight fluctuations • *Include weight assessment in intershift report* • Observe for electrolyte depletion • Monitor for edema • Diet education
Complications • Intractable/refractory heart failure • Cardiac dysrhythmias • Myocardial failure • Digitalis toxicity • Pulmonary infarction • Pneumonia • Emboli
Core Measures • Evaluation of LV Function (EF) • Echo report • Cath report • Nuclear stress test
Core Measures • Adult Smoking Cessation • Heart failure patient with a history of smoking within the past year • ACEI or ARB presecribed at discharge • Left Ventricular ejection fraction (LVEF) <40%
Core Measure Exclusions • Patient refusal • Patient on LVAD • Patient <18 years of age • Transfer to acute care hospital • Comfort/Hospice care • Discharged to hospice • Expired • Left AMA • Patient involved in clinical trial
Patient Education • Disease process: pumping action • Signs & symptoms of recurrence • Weight gain • Swelling of ankles, feet, abdomen • Cough • Fatigue • Frequent urination at night • Review medications, activity, diet
Teach Back http://ruralhealth.uams.edu/health-literacy/teachback
References • Aherns, T., Prentice, D., & Kleinpell, R. (2011). Progressive care nursing certification. New York: McGraw Hill Medical. • Alspach, J. (2006). Core curriculum for critical care nursing. (6th ed., pp. 271-284). St Louis: Saunders Elsevier. • American Heart Associatin. (2005). Guideline update for the diagnosis and management of chronic heart failure in the adult. Circulation, 112, 154-235. • Aronow, W. (2006). Heart failure update. Geriatrics, 61(8), 16-20.