Coryneform bacteria, listeria and erysipelothrix
580 likes | 3.26k Vues
Coryneform bacteria, listeria and erysipelothrix. Corynebacterium sp. Listeria monocytogenes Erysipelothrix rhusiopathiae. Corynebacteria. Significant Corynebacterium species C. xerosis C. pseudodiphtheriticum C. pseudotuberculosis C. jekeium C. ulcerans Rhodococcus equi

Coryneform bacteria, listeria and erysipelothrix
E N D
Presentation Transcript
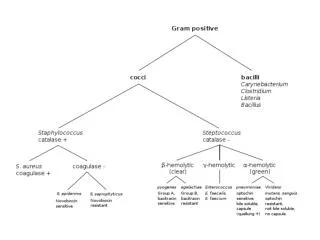
Coryneform bacteria, listeria and erysipelothrix Corynebacterium sp. Listeriamonocytogenes Erysipelothrixrhusiopathiae
Corynebacteria • Significant Corynebacterium species • C. xerosis • C. pseudodiphtheriticum • C. pseudotuberculosis • C. jekeium • C. ulcerans • Rhodococcus equi • Arcanobacterium haemolyticum
Corynebacterium Species • General characteristics • Found as free-living saprophytes in fresh and salt water, in soil and in the air • Members of the usual flora of humans and animals(often dismissed as contaminants) • Often called “diphtheroids” • Corynebacterium diphtheriae isthe most significant pathogen • Other species may cause infections in the immunocompromised hosts
Corynebacterium Species:General Characteristics • Morphology • Gram-positive, non–spore-forming rods • Arrange in palisades:“L-V” shape; “Chinese characters” • Pleomorphic: “club-ends” or coryneform • Beaded, irregular staining
C. diphtheriae: Agent of Diphtheria • Toxigenic Corynebacterium diphtheriae • Worldwide distribution but rare in places where vaccination programs exist • Exotoxin, Diphtheria toxin, as the virulence factor • Not all C. diphtheriae strains produce toxin • Toxin is produced by certain strains • Toxin is antigenic
Toxigenic Corynebacterium diphtheriae • Toxin consists of two fragments • A: Active fragment • Inhibits protein synthesis • Leads to cell/tissue death • B: Binding • Binds to specific cell membrane receptors • Mediates entry of fragment A into cytoplasm of host cell
Clinical Forms of Diphtheria • Respiratory • Acquired by droplet spray or hand to mouth contact • Non-immunized individuals are susceptible • Non-respiratory • Systemic • Skin and cutaneous forms
C. diphtheriae: Causative Agent of Diphtheria • Respiratory disease–diphtheria • Incubation period–2 to 5 days • Symptoms: sore throat, fever, malaise • Toxin is produced locally, usually in the pharynx or tonsils • Toxin causes tissue necrosis, can be absorbed to produce systemic effects • Forms a tough grey to white pseudomembrane which may cause suffocation
C. diphtheriae: Causative Agent of Diphtheria • C. diphtheriae pseudomembrane • WBC + organism
Clinical Infections: Non-Respiratory Disease • Systemic infections • Toxin is absorbed in the blood stream and carried systemically • Affects the kidneys, heart, and nervous system • Death occurs due to cardiac failure • Cutaneous form • More prevalent in the tropics • Infections occur at the site of minor abrasions • Maybe superinfected with Streptococcus pyogenes and/or Staphylococcus aureus
Treatment • Infected patients treated with anti-toxin and antibiotics • Anti-toxin produced in horses • Antibiotics have no effect on circulating toxin, but prevent spread of the toxin • Penicillin drug of choice
Laboratory Diagnosis • Microscopic morphology • Gram-positive, non–spore-forming rods, club-shaped, can be beaded • Appear in palisades and give "Chinese letter" arrangement • Produce metachromatic granules or “Babes’ Ernst” bodies (food reserves) which stain more darkly than remainder of organism Corynebacterium diphtheriae gram stain
Laboratory Diagnosis:Cultural Characteristics • Loeffler's slant or Pai's slant—Used to demonstrate pleomorphism and metachromatic granules ("Babes’ Ernst bodies“) • Growth on Serum Tellurite or modified Tinsdale exhibits brown or grayish→ to black halos around the colonies Tellurite: tellurium dioxide (TeO2).
Laboratory Diagnosis:Cultural Characteristics • Blood agar plae (BAP) 24-48 hours at 37oC small, grey translucent colonies • Small zone of b- hemolysis also s een
Laboratory Diagnosis • Identification • Confirm identification by fermentation reactions(glucose +) • Catalase positive • Urease negative • Non-motile
Laboratory Diagnosis • Toxigenicity testing • Elek test • Immunodiffusion test • Organisms are streaked on media with low Fe content to maximize toxin production. • Identification of C.diphtheriae does NOT mean the patient has dipheria. Must show the isolate produces the toxin. protease peptone agar + serum (horse or bovine) 1 and 4 positive
C. diphtheriae • Treatment: antitoxin • Prevention: DPT immunization
C. jekeium • Clinical Infections • Septicemia • Meningitis • Pulmonary disease • Populations Affected • Immunosuppressed • IV drug users
C. jekeiumColony Morphology • Isolation & identification • BAP: 48-72 hours at 35oC in ambient air or 5% CO2 small, gray-white colony, nonhemolytic • Gram stain: pleomorphic, club-shaped gram positive rod arranged in V forms or palisades
C. jekeiumLab Diagnosis • Identification • Nitrate reduction= negative • Urea= negative • Sucrose= negative • Glucose= positive
C. jekeium • Susceptibility testing • Exhibits resistance to multiple antibiotics • Susceptible to vancomycin
Listeria monocytogenes:General Characteristics • Gram-positive, non–spore-forming rods • Only human pathogen in genus • Widespread in nature • Known to infect a wide variety of animals • Human exposure is limited; direct or indirect • Transient colonization occurs without disease
Listeriamonocytogenes:Clinical Infections • Adults • Septicemia/meningitis in the compromised/elderly • Mild flu-like syndrome in pregnant women could be fatal to fetus • Ingestion of contaminated food • Neonatal • Early onset from intrauterine transmission results in sepsis; high mortality rate • Late onset manifests as meningitis; lower mortality rate
Listeria monocytogenes: • Virulence Factors • Hemolysin ( Listeriolysin O)- damages macrophage • Catalase • Superoxide dismutase • Phospholipid C • P60 surface protein- induces phagocytosis thru adhesion and penetration
Laboratory Diagnosis: L. monocytogenes • Identification • Microscopic morphology • Gram Positive non–spore-forming coccobacillary, pairs or short chains • Colony Morphology • Grows well on blood agar; colonies produce a narrow zone of hemolysis similar to Group B Streptococcus • Small, round and translucent
Laboratory Diagnosis: L. monocytogenes • Grows well at 0.5° C to 45° C • Because of this temperature range, especially the cooler end of the range, this organism grows well in refrigerated products, such as cream, cheese, deli meats, etc. • Can sometimes be isolated after “cold enrichment” (hold broth at 4° C for several weeks and subculture)
Laboratory Diagnosis: L. monocytogenes • Identification • Catalase positive • Motility: • Motile at 25o C; "umbrella" type → • Tumbling motility in hanging drop preparations (this can be seen on Gram Stain Tutor at www.medtraining.org) “Umbrella” motility pattern (Left) typical for L. monocytogenes
Laboratory Diagnosis: L. monocytogenes • Identification • CAMP test • Produces a “block” type of hemolysis in contrast to “arrow”-shape produced by Group B Streptococcus CAMP test with Listeria monocytogenes Positive CAMP test for Group B Streptococcus
Differentiating Characteristics betweenL. monocytogenes and Other Gram Positive Bacteria
Erysipelothrix rhusiopathiae:General characteristics • Gram positive, non–spore-forming, pleomorphic rods (can produce long filaments) • Distributed in nature • Can cause disease in animals (swine, turkey, sheep); swine is the main reservoir • Humans acquire the infection through occupational exposure, such as cuts & scratches (fish handlers, animal products)
Erysipelothrix rhusiopathiae:Clinical Infections • Erysipeloid • Self-limiting localized infection at the site of inoculation • Produces painful swelling, usually on the hands or fingers • Heals within 3 to 4 weeks • Endocarditis • May occur in those who have had valve replacements • Disseminated infections may occur, but rarely
Laboratory Diagnosis:Erysipelothrix rhusiopathiae • Microscopic Morphology • Pleomorphic, gram-positive thin rods that may form long filaments, may be arranged singly, in short chains, or in a V shape
Laboratory Diagnosis: Erysipelothrix rhusiopathiae • Identification • Catalase negative • CO2 is required • Distinguishing characteristic: Production of H2S on TSI • Microaerophilic • Nonmotile • Test tube brush growth in semisolid motility media
Laboratory Diagnosis: Erysipelothrix rhusiopathiae • Colony Morphology • Grows on blood or chocolate agar—colonies may appear gray or translucent, pinpoint with alpha hemolysis or nonhemolytic
Treatment: Erysipelothrix rhusiopathiae • Penicillin, cephalosporin, erythromycin
Characteristics of Corynebacterium, Listeria, and Erysipelothrix
Lactobacillus • Widely distributed in nature • Normal flora of mouth, GI tract and female genital tract • Treat with pencillin plus an aminoglycoside • resistant to vancomycin (helps in diagnosis) • Clinical Infections • Bacterial vaginosis • Bacteremia, endocarditis, meningitis (rare)
Lactobacillus • Microscopic Morphology • Long, slender gram positive pleomorphic bacilli • Non-spore forming • Colony Morphology • Microaerophilic • SBA: pinpoint, α- hemolytic colonies • Lab Diagnosis • Catalase negative