Bronchopneumonia
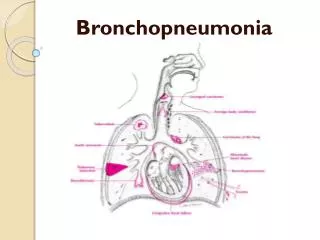
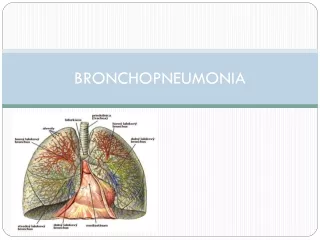
Bronchopneumonia. A type of pneumonia inflammation of the walls of the smaller bronchial tubes, with irregular areas of consolidation due to spread of the inflammation into the peribronchiolar alveoli and the alveolar ducts of the lungs


Bronchopneumonia
E N D
Presentation Transcript
A type of pneumonia • inflammation of the walls of the smaller bronchial tubes, with irregular areas of consolidation due to spread of the inflammation into the peribronchiolar alveoli and the alveolar ducts of the lungs • terminal bronchioles become clogged with mucopurulent exudate to form consolidated patches
usually a result of the spread of infection from the upper to the lower respiratory tract, most common caused by the bacterium Mycoplasmapneumoniae, Staphylococcus pyogenes, or Streptococcus pneumoniae. • The most common cause in infancy is the respiratory syncytial virus. • Bronchopneumonia pleural effusion, empyema, lung abscess, peripheral thrombophlebitis, respiratory failure, congestive heart failure, and jaundice.
Presenting signs and symptoms • High fever • Cough (initially unproductive to productive with sputum [yellow greenish]) • Tacypnea • Breath sounds – crackles, decrease breath sounds, rales • Chest pain • Retraction • Nasal flaring • Pallor to cyanosis • Irritability, restlessness, malaise, lethargy • Poor feeding • Gastrointestinal signs – Vomiting, Diarrhea, Abdominal pain • * can be the "non specific" symptoms such as irritability and decreased appetite or feeding without any specific respiratory or chest symptoms.
Nursing Management • Viral pneumonia • Symptomatically treated • Promote oxygenation (positioning, comfort, oxygen administration as order by paediatrician, postural drainage, • Antipyretic for fever • Strict I/O charting • Family support (FCC) • Bacterial pneumonia • Supportive and symptomatic • Antipyretic • Oxygenation (humidified via nasal or face mask) • Comfortable position • Antibiotic • Close observation for the respiratory status and other vital signs • Strict I/O charting (usually IVI) • Encourage fluid intake • Suction as to maintain patent airway (may use non-invasive suction device to suction his nares) • Nebulizer bronchodilator treatment may be prescribe depending on the child’s condition • Information giving to family and child accordingly • Enough rest and discourage vigorous activity (offer quite play)