Understanding the Cardiovascular System: Structure, Function, and Circulation
460 likes | 605 Vues
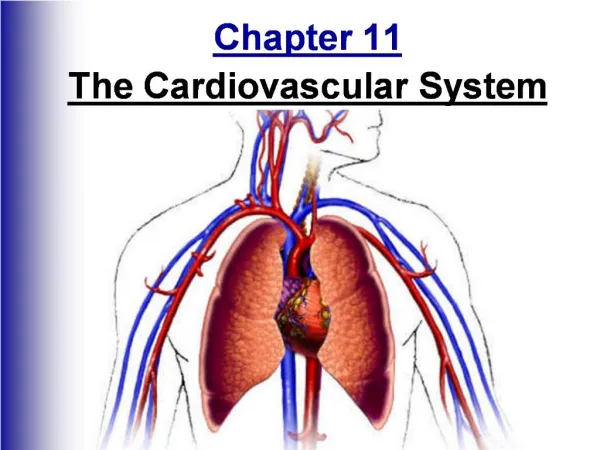
This chapter explores the cardiovascular system's key functions, primarily its role in transportation. Utilizing blood, it carries vital substances like oxygen, nutrients, and hormones throughout the body. The heart, situated in the thorax, consists of four chambers: two atria and two ventricles, governed by four essential valves to maintain proper blood flow. It analyzes heart anatomy, including the epicardium, myocardium, and endocardium, alongside the coronary arteries that nourish the myocardium. The chapter concludes by detailing the conduction system regulating heartbeats.

Understanding the Cardiovascular System: Structure, Function, and Circulation
E N D
Presentation Transcript
Chapter 11 The Cardiovascular System Biology 110 Tri-County Technical College Pendleton, SC
Functions of CV System • Major function is transportation • Using blood as transport vehicle, system carries oxygen, nutrients, cell wastes, hormones, and many other substances vital to homeostasis to and from cells • The force to move blood around the body provided by beating heart • Heart located in body thorax flanked by lungs
Have a heart… • More pointed apex pointed toward left hip & rests on diaphragm • Broader posterosuperior aspect, or base from which great vessels of body merge, points toward right shoulder and lies beneath the second rib
Coverings of the Heart • Enclosed by double sac of serous membane (pericardium) • Thin visceral pericardium (epicardium) hugs external surface of heart and is part of heart wall • Epicardium continuous at heart base with loosely applied parietal pericardium • Serous fluid (slippery lubricating) produced by serous pericardial membranes • Allows heart to beat almost frictionless environment as pericardial layers slide across each other
Walls of the Heart • Epicardium, Myocardium, Endocardium • Epicardium is thin visceral pericardium • Myocardium (middle layer) is composed of thick bundles of cardiac muscle twisted & whorled into ringlike arrangement • Myocardium that actually CONTRACTS • Endocardium (innermost) is thin, glistening sheet of endothelium that lines chambers • Continuous with lining of blood vessels entering and leaving heart
Heart Chambers • Four hollow chambers or cavities • Two atria and two ventricles—all lined with endocardium • Superior atria primarily receiving chambers • Inferior, thick-walled ventricles discharging chambers (actual pumps of heart • Septum dividing heart longitudinally referred to as interatrical and interventricular septum
Great Vessels of the Heart • Superior and inferior vena cavaright atria • Right ventriclepulmonary truckright and left pulmonary arterieslungs • O2 rich blood from lungs to heart4 pulmonary veins (pulmonary circuit)left atrialeft ventricleaortasystemic arteriesbody tissues (systemic circuit)
Heart Valves • Four valves whose general function is to prevent backflow of blood • Atrioventricular (AV) valves between atrial and ventricular chambers on each side • Left AV valve (bicuspid/mitral) has 2 cusps (flaps) & prevents backflow into left artium • Right AV valve (bicuspid) has 3 cusps & prevents backflow into right atrium • Pulmonary semilunar valve—right ventricle • Aortic semilunar valve—left ventricle
Blood Flow • From body into right atrium via vena cava • Right atriumright ventricle via tricuspid • Right ventriclelungs via pulmonary semilunar valve and pulmonary arteries • Lungsleft atrium via pulmonary veins • Left atriumleft ventricle via bicuspid • Left ventriclebody via aortic semilunar valve and aorta
Cardiac Circulation • Blood in heart does NOT nourish myocardium • Right and left coronary arteries responsible • Branch from base of aorta, encircle heart in atrioventricular groove • Anterior interventricular & circumflex arteries on left and posterior interventricular and marginal arteries on right compressed when ventricles contracting and fill when ventricle relax • Myocardium drained by several cardiac veins • Empty into coronary sinus (enlarged vessel on backside of heart • Coronary sinus empties into right atrim
Some Key Terms • Pericarditis-inflammation of pericardium often from decrease in amount of serious fluid • Pericardial layers bind and stick to each other • Forms painful adhesions interfering with heart movements • Valvular Stenosis-valve flaps become stiff (repeated bacterial infection of endocardium) • Forces heart to beat more vigorously than normal • Workload increases, heart weakens, and may fail
Key Terms, cont. • Myocardial infarction (heart attack or coronary)-myocardial cells NOT receiving adequate blood supply • Ischemic heart cells begin to die
Impulse Conduction • 2 types of controlling systems regulate • Nerves of ANS and intrinsic conduction system (nodal system) • ANS acts like “brakes” or “accelerator” depending on which division is activated • Intrinsic system composed of special tissue found no where else in body • Cross between nervous & muscle tissue • Causes depolarization in only ONE direction-from atria to ventricles
Impulse, cont. • Nodal system composed of sinoatrial (SA) node (right atrium); atrioventricular (AV) node(junction of atria & ventricles); AV bundles (bundle of His); Right and Left bundle branches (interventricular septum); and Purkinje fibers (within muscle of ventricular wall) • SA (Pacemaker) fires • Impulse spreads through atria to AV node • Atria contract
Impulse, III • AV node delays impulse preventing simultaneous atria/ventricle contraction • allows complete emptying of atria • Impulse conducted to AV bundle, bundle branches, and Purkinje fibers • Ventricles contract • Heart beats to internal rhythm but body can speed it up or slow it down • Vagus nerve <; Sympathetic fibers >
Heart Block • UNC, depolarization waves reach ventricles only through AV node • Damage to AV node can partially/totally release ventricles from control of SA node • Ventricles begin to beat at their own rate (which is much slower) some or all the time • This condition is called heart block
Three Key Terms • Ischemia is lack of adequate blood supply to heart muscle • May lead to fibrillation (rapid, uncoordinated shuddering of hear muscle) which makes heart useless as pump and major cause of death from heart attacks • Often followed by arrest • Bradycardia is heart rate substantially slower than normal (less than 60 beats per minute) • Tachycardia is rapid heartbeat (over 100 beats per minute) • May progress to fibrillation
Cardiac Cycle • Refers to events of ONE heartbeat • Average is 75 beats per minute so cycle normally about 0.8 seconds • Systole means heart contraction • Diastole means heart relaxation • Atria are in systole at same time and ventricles are in systole at the same time
Heart Sounds • Lub-Dup • First sound (lub) = closing of AV valves • Second sound (dup) caused by closing of semilunar valves at end of systole • Lub sound longer and louder; Dup tends to be short and sharp • Abnormal/unusual sounds called murmurs • Caused by turbulance of blood flow • Fairly common in children/elderly people
Sounds, cont. • Murmurs may indicate valve problem • If valve does NOT close tightly (incompetent), swishing will be heard as blood flows back through partially “open” valve • Distinct sounds also heard when blood flows turbulently through “stenosed” (narrowed) valves
Cardiac Output • CO is amount of blood pumped out by each side of heart • Actually each ventricle in ONE minute • Stroke volume is volume of blood pumped out by each ventricle with each heartbeat • SV >s as force of ventricular contraction >s • CO is PRODUCT of heart rate (HR) x stroke volume (SV); CO=HR x SV
Output, cont. • 75 beats/min x stroke volume of 70 ml/beat equals 5250 ml/min • Normal blood volume = ~5000 ml, entire blood supply passes through heart once each minute • SV regulated by many factors • > volume or speed of venous return >s SV & force of contraction • < volume or speed of venous return <s SV & force of contraction
Output, cont. • “Starlings law of the heart: more heart muscle is stretched, the stronger contraction • Critical factor “stretching” heart muscle is venous return • Insures volume of blood going out equals volume of blood coming in (vice-versa) • REGULATION of heart rate dependent of many factors
Output and Regulation, cont. • Heart rate can be changed temporarily by autonomic nerves • Sympathetic nerves stimulate SA and AV nodes and heart muscle itself to > rate • Parasympathetic nerves (vagus) slow and steady heart giving rest time during noncrisis • Epinephrine and thyroxine >s heart rate
Output & Regulation, cont. • Physical factors (age, gender, exercise, and body temperature) influence heart rate • Hypocalcemia (reduced levels of ionic calcium) depress the heart • Hypercalcemia (> levels of ionic calcium) causes prolonged contraction to point heart may stop entirely • Hypokalemia (reduced levels of ionic potassium causes feeble heart beat and abnormal rhythms appear • heatheart rate and coldheart rate
Congestive Heart Failure • Pumping efficiency depressed so circulation inadequate to meet tissue needs = congestive heart failure • One side can fail independently of the other • Left side fails = Pulmonary congestion occurs • vessels in lungs swells-fluid leaks-pulmonary edema-if untreated, person suffocates • Right side fails = Peripheral congestion occurs • blood backs up in systemic circulation-edema most noticeable in distal body parts (swollen feet, ankles, fingers) • Failure of one side puts strain on other side & eventually whole heart fails
Electrocardiogram (ECG) • Impulses cause electrical currents to pass through body • Can be detected by electrocardiograph • Three recognizable waves (P, QRS complex, & T) • P wave first and small-depolarization of atria before they contract • QRS complex is large wave-depolarization of ventricles; precedes their contraction • T-wave results repolarization of ventricles • Atrial repolarization normally hidden by QRS • May reveal heart problems: abnormal waves; changes in timing; fibrillation
Arterial Pulse • Expansion and recoil of artery occurring with each ventricle beat creates PULSE • Pulse rate = heart rate • Averages 70-80 per minute • Influenced by activity, postural changes, emotions • May be taken at any artery close to surface • Temporal, carotid, brachial, & radial most common
Blood Pressure… • Is pressure blood exerts against inner walls of blood vessels • Force that keeps blood circulating • USD, understood to mean pressure within large systemic arteries NEAR heart • Pressure highest in large arteries and <s thru pathway • Reaches 0 or negative at vena cava • Return dependent on valves in larger veins, milking activity of skeletal muscles, and pressure changes in thorax
Auscultatory Method for BP • Systemic arterial BP measured indirectly • System uses brachial artery of arm • Systolic pressure=pressure at peak of ventricular contraction • Diastolic pressure=pressure when ventricles are relaxed • “Normal” is 120/80 but range is 110-140/75-80 • Varies with age, weight, mood, race, activity, and posture
BP Math…or whatever • BP = cardiac output x peripheral resistance • Cardiac output increases, BP increases • Peripheral resistance increases; BP increases • Cardiac output decreases; BP decreases • Peripheral resistance decreases; BP decreases
Factoring the factors • Sympathetic division of ANS causes vasoconstriction >ing peripheral resistance which >s BP • Parasympathetic division of ANS causes vasodilation <ing peripheral resistance which <s BP • Kidneys help regulate BP by altering blood volume • Retain or excrete water • Also produce RENIN
Factors, cont. • If BP low, kidney cells release enzyme renin into blood • Renin triggers cascade of reactions that produce Angiotensin II which is potent vasoconstrictor • Vasoconstriction raises BP • AT II stimulates adrenal cortex to release Aldosterone (hormone that >s sodium ion reabsorption by kidneys • Water follows sodium ions thus blood volume and BP both rise
Enough of factoring, already.. • Epinephrine >s heart rate and BP • Nicotine >s BP by causing vasoconstriction • Alcohol/Histamine < BP by causing vasodilation • Diuretics cause kidneys to excrete more water which reduces blood volume thereby lowering BP • TOO much salthypertonic blood which absorbs water from tissues increasing blood volume and BP
The end of factoring…Yeah!! • TOO much fatsexcessive fats in blood • Makes blood more viscous and more difficult to pump • Peripheral resistance is increased which increases the blood pressure
Hypotension • Low BP = systolic < 100 mm Hg • Physical conditioning and/or health • Orthostatic hypotension = temporary drop in BP resulting in dizziness upon rising • May be slow reacting sympathetic NS and blood pooling in lower limbs reducing BP and blood delivery to brain • Chronic hypotension may be result of inadequate blood proteins, low viscosity, and/or low pressure
Hypertension • Sustained elevated arterial pressure of 140/90 or higher • Heart has to work against increased resistance and has to work HARDER • Myocardium enlarges; when strained beyond capacity to respond, weakens and becomes flabby • Causes small tears in endothelium of blood vessels that > progress of artherosclerosis
Hypertension, cont. • Most cases (90%+) are primary or essential which CANNOT be accounted for by any specific organic cause • Diet, obesity, heredity, race, stress involved • Treatment for hypertension • diuretics • vasodilators/beta blockers • ACE-inhibitors (inhibit renin) • Cardiac inhibitors (calcium channel blockers) • Lifestyle changes