How much do you know, really?
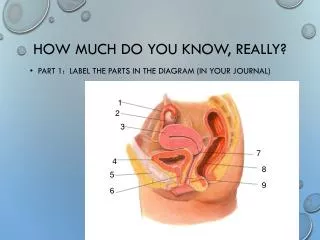
How much do you know, really?. Part 1: Label the parts in the diagram (in your journal). 1. 2. 3. 7. 4. 8. 5. 9. 6. Answers. Part 2: Given the terms, put them in order of the places for sperm development and ejaculation. Epididymis Seminiferous tubules Urethra Vas deferens.

How much do you know, really?
E N D
Presentation Transcript
How much do you know, really? • Part 1: Label the parts in the diagram (in your journal) 1 2 3 7 4 8 5 9 6
Part 2: Given the terms, put them in order of the places for sperm development and ejaculation • Epididymis • Seminiferous tubules • Urethra • Vas deferens
Answers • Seminiferous tubules • Epididymis • Vas deferens • urethra
Part 3: Match the term to the description A. Follicular Phase B. Ovulation C. Luteal Phase D. Menstruation • Egg passes through uterus without implantation. • Low estrogen levels cause hypothalamus to stimulate anterior pituitary to secrete FSH and LH. • Follicle ruptures and egg is released. • The period during which there is the greatest chance an egg will be fertilized.
Answers • D – Menstruation • A – Follicular Phase • B – Ovulation • C – Luteal Phase
Chapter 39 -- §3 & 4 Reproductive System
Reproductive System • Responsible for the formation of new individuals • If this system does not function properly the individual can still lead a healthy life • The most important system for the continuation of the species • Produces, stores and releases gametes • Zygote – the cell that results from the fusion of sperm and egg
Sexual Development • starts before baby is born • In the First6 Weeks • human male and female embryos are identical in appearance
Sexual Development -- con’t • 7th Week • primary reproductive organs begin to develop • testes – in males • produce testosterone • this causes development of male reproductive organs • ovaries – in females • produce estrogen • this causes development of female reproductive organs
After Birth • Gonads • produce small amounts of sex hormones that continue the development of reproductive organs
Puberty • period during which the reproductive system becomes fully functional (both male and female) • begins between ages 9 and 15, generally females start about 1 year earlier than males • begins when the hypothalamus signals the pituitary to produce more • FSH (follicle-stimulating hormone) and • LH (luteinizing hormone) which affect the gonads
Hormones • FSH (follicle stimulating hormone) and LH (luteinizing hormone) stimulate cells in the testes to produce testosterone • FSH and testosterone stimulate the development of sperm • The main function of the male reproductive system is to produce and deliver sperm
Parts testes – primary reproductive organs develop within the abdominal cavity
Scrotum sac of tissue into which the testes descend just before/after birth ● outside of the body cavity ● temperature is 1o-3oC lower than body temperature(37oC) which is necessary for proper sperm development
seminiferous tubules clusters of hundreds of tiny tubes within each testis • coiled and twisted together •location of sperm production
epididymis – comma-shaped structure in which sperm (which are produced in the seminiferous tubules) fully mature and are stored vas deferens – tube leading from the scrotum into the abdominal cavity urethra – tube leading to the outside of the body through the penis
Even More Parts seminal fluid – nutrient-rich fluid produced in three glands lining the reproductive tract 1) seminal vesicles 2) prostate 3) bulbourethral glands semen – combination of sperm and seminal fluid – between 50 and 130 million sperm per 1 mL of semen, or 2.5 million sperm per drop sperm – haploid reproductive cells that are produced by specialized cells in the testes undergoing meiosis
Parts of a Sperm head – contains highly condensed nucleus midpiece – region packed with mitochondria tail, or flagellum – propels cell forward acrosome – small cap on the head of the sperm that contains an enzyme that helps sperm penetrate the egg
Sperm Release • autonomic nervous system prepares organs to deliver sperm; • not completely voluntary • ejaculation – the process of ejecting sperm from the penis by the contraction of smooth muscle that lines the glands of the reproductive tract • 2 to 6 mL semen are released
Main Functions of the Female Reproductive System • To produce ova (eggs) and to prepare the female’s body to nourish a developing embryo
Ovaries • Primary reproductive organ in females; located in abdominal cavity • hypothalamus signals the pituitary to release FSH and LH which stimulates the ovaries to make estrogen • usually produces only one ovum (egg) each month
Egg Development • primary follicle – cluster of cells surrounding a single egg • helps the egg mature for release into the reproductive tract where it can be fertilized • 400,000 in each ovary • maturation – only about 400 eggs actually mature and are released in a lifetime • every 28 days, under the influence of FSH, an ovum completes meiosis
Ovulation • Release of egg from mature follicle • follicle breaks open and egg is swept from the surface of ovary into the opening of the Fallopian tube
More Parts • Fallopian tubes – fluid-filled tubes into which the ovum is swept • lined with ciliawhich help move ovum along • fertilization occurs here
uterus • Cavity into which the egg passes after a few days in the Fallopian tube • lined to receive a fertilized egg • the lining is shed if fertilization does not occur - menstruation
More Parts • cervix – opening to uterus from vagina • vagina – canal that leads from the uterus to outside of the body
The Menstrual Cycle Interaction of the endocrine and reproductive systems • takes about 28 days; mensis is Latin for “month” • regulated by hormones made by hypothalamus, pituitary gland, and ovaries; controlled by feedback mechanisms • egg is developed and released from ovary • uterus is prepared to receive fertilized egg
You will not be held accountable for details of the four phases…(Here they are, anyways)
Follicular Phase (approx. 10 days) • hypothalamus detects low levels of estrogen • hypothalamus releases a hormone to stimulate the pituitary gland • pituitary gland secretes FSH and LH • FSH and LH causes a follicle to develop to maturity • cells around the follicle enlarge and produce estrogen • increased level of estrogen causes the lining of the uterus to thicken (in preparation for receiving an egg)
Ovulation (3-4 days) • hypothalamus sends large amounts of releasing hormone to the pituitary gland • pituitary gland secretes FSH and LH • FSH and LH causes a follicle to rupture and release the mature egg into the fallopian tube
Luteal Phase • begins after egg is released • cells of ruptured follicle turn yellow and are called the “corpus luteum” • corpus luteum continue to release estrogen, but also begin to release progesterone • progesterone stimulates the growth and development of a blood supply and surrounding tissue of the lining of the uterus • first 2 days of luteal phase has the greatest chance of fertilization (10-14 days after completion of last menstrual cycle) • if the egg is fertilized, it begins to divide by mitosis • after several divisions, a ball of cells forms and implants itself in the lining of the uterus • within a few days of implantation, the uterus and embryo release hormones to keep the corpus luteum functioning for several weeks (allowing the lining of the uterus to develop)
Menstruation • If no fertilization occurs, 2 to 3 days after ovulation, the egg passes through the uterus without implanting • corpus luteum begins to disintegrate • less estrogen and less progesterone are released • decrease in estrogen levels cause the lining of the uterus to detach from the wall of the uterus • menstruation – discharge of the lining of the uterus and blood and unfertilized egg through the vagina • new cycle begins on the first day of menstruation
Sexually Transmitted Diseases (STDs) • Spread from one person to another during sexual intercourse. • syphilis – can be fatal • gonorrhea – can be easily spread • chlamydia – more than 3 million cases each year • caused by bacteria • females ages 15 to 19 show highest incidence • can cause infertility in females
Viral STDs • Cannot be treated with antibiotics. • Hepatitis B • Genital Warts • Genital Herpes • Aids • Best way to avoid STDs: Abstain from sex before marriage. • Next safest course: Use a latex condom (this is NOT 100% protection).
§39-4 Fertilization & Development • The penis generally enters the vagina to just below the cervix. • Sperm are released when semen is ejaculated • Sperm swim through the cervix, through the uterus and into the fallopian tubes.
If an egg is present, its chances of being fertilized by one of the hundreds of millions of sperm are good. • The sperm attaches to a binding site on the protective layer that surrounds the egg. • The acrosome of the sperm releases enzymes to break down the protective layer.
When one sperm enters the egg, the egg releases a chemical that coats its surface preventing other sperm from attaching (the acrosomal reaction). • The sperm nucleus (1N) enters the egg (1N). This is fertilization. • The fertilized egg is called a zygote.
Fallopian Tube 4 cells 2 cells Morula Zygote Fertilization Blastocyst Implantation Placenta Ovulation Ovary
Early Development • Zygote begins mitosis while in the Fallopian tube • morula – a solid ball of 64 cells that the embryo becomes, four days after fertilization • 3 stages of early development • Implantation • Gastrulation • Neurulation
Implantation • Occurs 6-7 days after fertilization. • Blastula connects itself to the wall of the uterus. • Differentiation begins • Cells begin to specialize due to the activation of certain genes.
Gastrulation • Process of cell migration which results in 3 cell layers (called Primary germ layers) • Ectoderm – develops into skin and nervous system. • Mesoderm – forms many internal tissues and organs • Endoderm – forms lining of the digestive system and many digestive organs.
Neurulaton • Development of the nervous system. • Some mesodermal tissues begins to become the notochord. • Notochord folds in on itself and creates the neural groove and two neural folds. • Neural folds move together to form the neural tube. This becomes the spinal cord, brain and rest of the nervous system develops.
Embryonic Membranes – Protect and Nourish Embryo • Amnion – develops into the amniotic sac which cushions and protects the embryo in the uterus. • Chorion – outermost membrane • Formed in third week • Chorionic villi – small finger-like projections on the outer surface of the chorion that extend into the uterine lining.
Placenta • Formed by the chorion and uterine lining. • Connection between mother and developing embryo. • Nutrients and oxygen in blood of mother diffuse into the embryo’s blood in the chorionic villi • Waste diffuses from the embryo’s blood into the mother’s blood. • Mother’s and embryo’s blood do not mix…they are separated by the placenta.
Placenta – continued • Placenta acts as an organ of respiration, nourishment and excretion. • Barrier to harmful or disease-causing agents. • Some agents can cross the placenta • HIV, German Measles (Rubella) • Some drugs can cross the placenta • Alcohol, medication, addictive substances
Development • 8 Weeks – embryo develops into a fetus. • 3 Months – most of major organ tissues are fully formed. • Umbilical cord is formed • Contains two arteries and one vein • Connects fetus to placenta • Fetus begins to move. • 8cm long with a mass of approx. 28 grams.