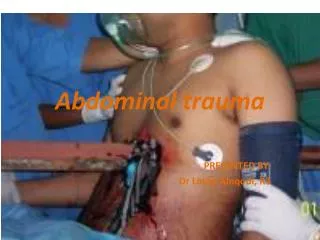
Abdominal Trauma
Abdominal Trauma. Dr. Roberts. Exterior Landmarks. Anterior Abdomen – transnipple line to inguinal ligament to symphysis pubis to ant. axillary line Flank – anterior to posterior axillary lines from 6 th intercostal space to iliac crest

Abdominal Trauma
E N D
Presentation Transcript
Abdominal Trauma Dr. Roberts
Exterior Landmarks • Anterior Abdomen – transnipple line to inguinal ligament to symphysis pubis to ant. axillary line • Flank – anterior to posterior axillary lines from 6th intercostal space to iliac crest • Back – posterior axillary line to posterior axillary line from the scapular tip to iliac crest
Internal Anatomy • Peritoneal Cavity – upper & lower parts; upper [diaphragm, liver, spleen, stomach, & trans colon]; lower [small bowel, ascend/descend/sigmoid colon, reproductive organs] • Pelvic Cavity – rectum, bladder, iliac vessels, reproductive organs • Retroperitoneal Space – aorta, inf vena cava, majority of duodenum, pancreas, kidneys, ureters, posterior portion of asc/descending colon *not sampled by DPL*
Mechanism of Injury: Blunt vs. Penetrating • Blunt: forces deform solid & hollow organs leading to rupture/bleeding/peritonitis • Shearing forces due to deceleration eg, liver/spleen at sights of ligamentous attachment • Spleen 55% > Liver 35%% > small bowel 10% & retroperitoneal hematoma 15%
Mechanism of Injury: Blunt vs. Penetrating • Penetrating: stab & low-velocity GSW inflict trauma by laceration/cutting; high-velocity GSW also transfer Kinetic Energy leading to cavitation/fragmentation • Stab wounds: Liver 40% > SB 30% > Diaphragm 20% > Colon 15% • GSW: SB 50% > colon 40% > Liver 30% > vascular structues 25%
Falls cause which type of injuries? • They produce hollow visceral injuries more commonly, and solid organ injuries less commonly. • They also produce retroperitoneal injuries associated with significant blood loss because force is transmitted up the axial skeleton.
Death from solid organ injury is due to what? • Acute Blood Loss
What organ is the most commonly injured in blunt abdominal trauma • Spleen
What is Kehr’s sign? • Kehr's sign is the occurrence of acute pain in the tip of the shoulder due to the presence of blood or other irritants in the peritoneum when a person is lying down and the legs are elevated. Kehr's sign in the left shoulder is considered a classical symptom of a ruptured spleen.
Are lower rib fractures important? • Yes! They should heighten clinical suspicion for splenic injury. • Remember that tachycardia, hypotension, and acute abdominal tenderness are the primary physical findings in abdominal trauma. • Repeat the abdominal exam frequently. A single finding is not specific for the diagnosis.
What is the problem with hollow visceral injuries? • They cause a combination of blood loss and peritoneal contamination.
What risk do head injuries, distracting injuries, and intoxicated patients run when they have abdominal trauma? • The risk of developing peritonitis due to a bowel perf. Peritoneal signs develop over time and this is why there is a need for repeat exams.
How long does it take for inflammation to develop after a perf? • 6-8 hours!
Retroperitoneal • SIP A DUCKS=SUPRARENAL GLI=IVC + BRANCHESP=PANCREAS HEAD • A=AORTA • D=DUODENUMU=URETERSC=CISTERNA CHYLI • K=KIDNEYS
Assessment • Hypotension – Expedite • Stable & no peritonitis – detailed evaluation • Detailed History • PE: inspect EVERYWHERE; Percuss/Palpate • GSW 90% have significant intraperitoneal injury • Stab wounds 30% significant intraperitoneal injury • Hypotension with GSW or stabbing with peritonitis = laparotomy • Pelvic Stability – compress ASIS with caution • Genitalia – blood @ meatus or ecchymoses @ scrotum/perineum suggests urethral tear • Rectum – sphincter tone, prostate, blood (Bowel Perf) • Vagina – blood? • Gluteal – penetrating injuries = 50% incidence of intraabdominal injury
What are the four modalities you can use to evaluate the abdomen? • Plain Films • FAST • DPL • CT scan
Plain films may help find free air or associated pelvic fractures.
What is DPL? What are the numbers? • DPL is used as a method of rapidly determining the presence of intraperitoneal blood • DPL is particularly useful if the history and abdominal examination of a patient who is unstable and has multisystem injuries is either unreliable (eg, head injury, alcohol, drug intoxication) or equivocal (eg, lower rib fractures, pelvic fractures, confounding clinical examination).
What is DPL? What are the numbers? • Abdominal exploration always is indicated if approximately 10 mL of blood is aspirated upon insertion of the peritoneal catheter (grossly positive) in the unstable patient. • If findings are negative, infuse 1 L of crystalloid solution (eg, lactated Ringer solution) into the peritoneum. Then, allow this fluid to drain by gravity, and ensure laboratory analysis is performed.
What is DPL? What are the numbers? • Presence of more than 100,000 RBC/mm3 or more than 500 WBC/mm3 is considered a positive finding.
What are DPL contraindications? • If they are going to surgery (absolute) • Advanced hepatic dysfunction, severe coagulopathies, previous abdominal surgeries, gravid uterus (relative)
FAST • Indications: • Change in sensorium (brain injury, ETOH or drug intoxication) • Change in sensation (spinal cord injury) • Injury to adjacent structures (lower ribs, pelvis or lumbar spine) • Prolonged loss of contact with patient anticipated, Lap-belt sign
What is the FAST scan, what are its indications? • Focused Assessment with Sonography in Trauma • Views • Perihepatic- Morisons pouch • Perisplenic • Pelvis • Pericardium • Use for trauma • Decision point, not diagnosis • should be “fast” • should not get in the way of definitive treatment or imaging
What is FAST and the numbers • FAST can identify free intraperitoneal fluid. • The sensitivity for solid organ encapsulated injury is moderate in most studies. • Hollow viscus injury rarely is identified; however, free fluid may be visualized in these cases.
What is FAST and the numbers? • FAST evaluation of the abdomen consists of visualization of: • 1) The pericardium (from a subxiphoid view), • 2) The splenorenal and the hepatorenal spaces (ie, Morison pouch), • 3) The paracolic gutters, • 4) The pouch of Douglas in the pelvis. The Morison pouch view has been shown the most sensitive, regardless of the etiology of the fluid.
What is FAST and the numbers? • Free fluid, generally assumed to be blood in the setting of abdominal trauma, appears as a black stripe (anechoic). • Free fluid in a hemodynamically unstable patient indicates the need for emergent laparotomy. • CT scan may further evaluate the stable patient with free fluid. • Sensitivity and specificity of these studies range from 85-95%.
Scan' em all and let God sort them out... • Tom’s “Paramedic Photo?”
Donut of Death? • CT scan often provides the most detailed images of traumatic pathology. • Transport only hemodynamically stable patients to the CT scanner. • The primary advantage of CT scanning is its high specificity and use for guiding nonoperative management of solid organ injuries.
Disadvantages to CT? • Drawbacks of CT scanning relate to the need to transport the patient from the trauma resuscitation area and the additional time required to perform CT scanning as compared to FAST or DPL. • The best CT imagery requires both oral and IV contrast.
Interventions • Gastric Tube: decompress stomach; blood = possible esophagus/stomach injury • Urinary Catheter: caution in unstable pelvic fx; blood at the meatus,; scrotal hematoma; perineal ecchymoses [Retrograde urethrogram]
Interventions • Urethrography: # 8 french catheter secured at meatus, then 15-20 mL of undiluted contrast with gentle pressure • Cystography: bulb syringe attached to a foley cath held 40 cm above the patient; 300mL of contrast infused until flow stops/patient has discomfort; AB/oblique/post drainage views • CT Cystogram a better test
Indications for laparotomy (celiotomy if you are a fancy surgeon) • Blunt trauma with hypotension & clinical evidence of bleeding • Blunt trauma with positive DPL or FAST • Hypotension with penetrating abdominal wound • GSW traversing the peritoneal cavity or visceral/vascular retroperitoneum • Evisceration • Bleeding from stomach, rectum, genitourinary tract & penetrating trauma • Presenting peritonitis • Free air, retroperitoneal air or ruptured hemidiaphragm in blunt trauma • CT demonstrating ruptured GI tract, intraperitoneal bladder, renal pedicle injury, severe visceral parenchymal injury after trauma
Specific Injuries • Diaphragm • Usually Lt hemidiaphram • Elevation or blurring of the hemidiaphragm, hemothorax, G tube in chest
Specific Injuries • Usually blunt trauma to the abdomen • Bloody gastric aspirate or retroperitoneal air; double contrast CT aids diagnosis
Specific Injuries • Small Bowel • Blunt trauma / seat belt sign / chance fracture • CT very sensitive • Pancreas • Double contrast CT may miss • Serum amylase may be normal initially • Rising amylase or pain mandates repeat CT or emergent ERCP
Specific Injuries • Liver Laceration Spleen Laceration
What are duodenal injuries most often associated with? • With high speed vertical or horizontal decelerating trauma. • Also associated with pancreatic injury. The classic case is a blow to the midepigastrium steering wheel, or bicycle handlebar.
What complication may arise with associated pancreatic injury?
On the abdominal plain film, mottled gas to the left of the spine is seen and resembles that of gas and feces in the transverse colon. CT through the same region shows a large gas collection in the lesser sac with fluid laterally, compatible with retroperitoneal abscess.
Tension gastrothorax complicating acute traumatic diaphragmatic rupture. • Remember that in most cases the only fining on CXR is blurring of the diaphragm or an effusion
What do we do in the E.R.? • ABC’s • Two large bore IV’s • O2 • Monitor • NG tube • Foley (unless suspect urethral injury) • Zosyn (3.375 g IV) • Admit! Unless superficial wounds do not reveal significant injury.
What are the organs most commonly injured by penetrating trauma to flank? • Liver, kidney, colon, duodenum, pancreas
Necrotizing fasciitis from gluteal stab & missed rectal injury!