gingival enlargement
gingival enlargement

gingival enlargement
E N D
Presentation Transcript
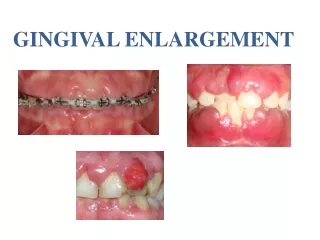
Gingival enlargement or gingival overgrowth Increase in the size of gingiva Old terminology gingival hyperplasia (not used more) Management depends on origin of enlargement Classified according to : Etiologic factors and pathologic change According to location and distribution According to the degree of enlargement
CLASSIFICATION Based on etiologic factors and pathologic changes I. Inflammatory Enlargement Acute Chronic II. Drug-induced enlargement • Conditioned enlargement • 1. Pregnancy 2. Puberty 3. Vitamin C deficiency 4. Plasma cell gingivitis 5. Nonspecific conditioned enlargement
CLASSIFICATION Systemic diseases causing gingival enlargement 1. Leukemia 2.Granulomatous diseases (Wegener's granulomatosis, sarcoidosis) Genetic gingival enlargement Hereditary gingival fibromatosis Neoplastic enlargement (gingival tumors) Benign tumors Malignant tumors False enlargement
Based on distribution localized or generalized . I- Localized A- Isolated” enlargements : limited to single or two teeth Sessile Pedunculated Tumor-like enlargements (e.g., fibroma/pyogenic granuloma). “ B-Regional” enlargements : around three or more teeth in one or multiple areas of the mouth (e.g., inflammatory enlargement associated with mouth breathing in maxillary anterior region). II- Generalized : Enlargement refers to involvement of gingiva adjacent to almost all the teeth (e.g., drug influenced gingival overgrowth
SEVERITY OF GINGIVAL ENLARGEMENT Degree 0 - No gingival enlargement Degree 1 - Enlargement located on interdental papilla Degree 2 - Enlargement involved papilla and marginal gingiva Degree 3- Enlargement that covers ¾ or more of the tooth crown (Bokenkamp, 1994, DeAngelo, 2007, Douzgou and Dallapicolla,2011).
1. INFLAMMATORY ENLARGEMENT Gingival abscess Periodontal abscess INFLAMMATORY
Inflammatory enlargement Most common form of gingival enlargement Chronic inflammatory response to local irritant associated with gingiva
Inflammatory enlargement • CLINICAL PICTURE • Smooth , edematousenlarged gingival tissue Ballooning of interdental papilla & marginal gingiva • appear bluish or deep red • Bleed easily • Localized / generalized • Discrete sessile or pedunculated • (tumor like mass) • Progress- slowly and painlessly • Pseudopockets • Occasionally, chronic inflammatory enlargement may also present as firm, resilient, pink and fibrotic enlargement
Treatment Non –surgical treatment Oral hygiene instructions Supra- and subgingival scaling followed by reevaluation at 4 weeks Correcting local factors Treating underlying systemic diseases and controlling predisposing conditions Surgical phase : Gingivectomyand gingivoplasty technique
Enlargements associated with systemic diseases or conditions Two mechanisms Conditioned enlargement Magnification of an existing inflammation initiated by dental plaque • Hormonal – Pregnancy , Puberty • Nutritional – Vitamin C deficiency • Allergic 4. Non specific conditioned Systemic disease causing enlargement Enlargement as manifestations of systemic diseases independently of presence of dental plaque Leukemia 2. Wegenersgranulomatosis
b. Enlargement in puberty • Male and female adolescents • Areas of plaque accumulation • Facial surface • Marginal and interdental Hormonal changes • Prevotellaintermedia & Prevotellanigrescens. After puberty – spontaneous reduction
a.Enlargement in pregnancy • Marginal , Interdental • Localized or generalized enlargement • Single or multiple tumor like masses Prevalence of 30% and even ranging up to 100% ETIOLOGY AND PATHOGENESIS : Hormonal changes (ESTROGEN AND PROGESTERON ) Subgingival microbiota – increase proportion of P. intermedia
Enlargementin Pregnancy CLINICAL FEATURES - Bright red or light purplish red color • Friable , smooth & shiny surface • Bleeding – spontaneously or on slight provocation • PLAQUE MUST PRESENT
2. Tumor like gingival enlargement Pregnancy tumor Not a neoplasm , it is an inflammatory response to bacterial plaque and modified patients condition localized, Tumor-like growth Most Common : labial aspect of the anterior maxillary region Etiology Local factors : Chronic trauma , irritation from calculus or restorations
CLINICAL FEATURES • Soft , friable , discrete mushroomlike or flattened • Doesn't invade underlying bone • Bleed easily • May have ulcerated surface • Painless unless its size and shape Treatment Removal of plaque and calculus Surgical excision and SRP Recurrence Spontaneous reduction – termination of pregnancy
c. Enlargement in vitamin C deficiency Scurvy Acute deficiency collagen degeneration , Modify response to plaque Clinical features • Bluish red , soft , friable smooth & shiny surface • edema • Haemorrhage– Spontaneous / slight provocation • Surface necrosis with pseudomembrane formation
MOUTH BREATHING The exact mechanism is not clear It is thought to be due to alternate wetting and drying of the gingival surface The gingiva appears red and edematous with diffuse shiny surface Affects Mainly the anterior maxillary gingiva Incomplete lip closure Short upper lip Class II malloclusion Proclined incisors Rhinitis
d. Plasma cell gingivitis Allergic in origin Clinical features Edematous and inflammed gingiva facial aspect of attached gingiva Bleeds easily Differs from plaque induced gingivitis(NO local factor) • HISTOPATHOLOGY • Epithelium – mild hyperplsia • Connective tissue – dense infiltrate of plasma cells
Systemic Disease That Cause Gingival Enlargement Leukemia: Malignant neoplasia of WBC precursors Acute myeloid leukemia Gingival enlargementd due to the massive infiltration of immature WBCs (leukemic cells) in the gingival connective tissue Clinically: it may mimic inflammatory origin. Localized OR Generalized Bluish red , shiny surface EASELY bleed (even spontaneously) Ulceration of gingiva • Secondary Inflammatory enlargement due to plaque accumulations
Leukemia: It can be associated with signs and symptoms of: Bone marrow failure, such as ecchymoses, Petechiae Night sweats, and lethargy Recent infections ( Candidal infection) Diagnosis can be made by a simple full blood count
Wegener’s Granulomatosis: “Strawberry gingivitis”, • Granulomatous disease • Acute necrotisingvasculitislesions of respiratory tract , nasal and oral defects Etiology • Unknown • Immunologically mediated tissue injury • Reddish-purple exophytic gingival swelling with patechialhaemorrhages, is a characteristic sign of Wegener’s granulomatosis. • Help in EARLY diagnosis of this potentially fatal condition, because they APEAR for a long time before multi-organ involvement occurs • At least two conditions to diagnose : • (1) ulcerative lesions of oral mucosa or nasal bleeding or inflammation; • (2) nodules, fixed infiltrates or cavities in chest radiograph; • (3) abnormal urinary sediment • (4) granulomatous inflammation on biopsy
Neoplastic Enlargement Benign tumors of gingiva Epulis Generic term refers to any solitary/discrete, pedunculated or sessile swellings of the gingiva with no histologic characterization of a particular lesion Fibrous epulis/peripheral fibroma Firm, pink, uninflammed mass Smooth surfaced Grow slowly Painless Pain may be associated due to secondary trauma
e. Nonspecific conditioned enlargement Pyogenicgranuloma Tumorlikemass , pedunculated Smooth surfaced , often ulcerated Reddish/bluish color mass are highly vascular Bleed readily Rapid grow within first few weeks and then slowly The mass may penetrate interdentally and present as bilobular (buccal and lingual) mass Bone not affected Painless
Gingival Cyst: Unusual cysts of odontogenic source Most common on : The labial attached gingiva of the mandibular Canine and premolar Presence of fluid may give them a bluish hue May cause resorption of the labial bone due to pressure Excisional biopsy is the best management for these lesions
Malignant lesions of gingiva Squamous cell carcinoma: • Most common malignant tumor of gingiva • Invasion to alveolar bone • 90% of all Oral cancer
Melanoma: From melanocytes Maxillary attached gingiva , Hard palate Rapid growth, early metastasis Infiltration into underlying bone Metastasis to lymph nodes
Genetic disorders associated with gingival enlargement Hereditary gingival fibromatosis Rare fibrotic gingival enlargement Autosomal dominant Fibroticfirm consistency pseudo-pockets localized or generalized It may present as a specific entity or as a part of syndrome (mental retardation, epilepsy) Diagnosis : Positive family history of gingival enlargement. Clinical picture It usually begins with the eruption of the primary or permanent dentition Buccal and lingual surfaces involved
Most Common Effects Diastema, spacing Malpositioningof teeth Prolonged retention of primary teeth Cover the dental crowns The alveolar bone is not affected unless periodontal diseases progressed
False enlargement Enlargement of bone subjacent to gingival area Gingival tissue appear normal Underlying osseous lesions Commonly Tori, Exostosis Also seen in Paget’s disease, Fibrous dysplasia, Cherubism,, Ameloblastoma, Osteoma and Osteosarcoma
Drug induced gingival enlargement Prevalence 50 % - phenytoin 30% - Cyclosporine 10% - Nifedipine
Characteristics Of Drug-induced Gingival Enlargement Higher prevalence in children Signs and symptoms are seen within 2-4 months of initiation of drug intake. The enlargement starts in the interdental papilla and eventually may involve marginal gingiva. Found in gingiva with or without bone loss but is not associated with attachment loss More prominent in maxillary and mandibular anteriors, may involve the gingiva around all teeth It will be absent in edentulous areas and will disappear in areas where teeth are extracted . Esthetic Problem Interfere masticatory function, speech, oral hygiene
Clinical features Gingival enlargement Without inflammation The enlargement looks like mulberry Shape lobulated surface Firm, fibrotic resilient Pink No bleeding on probing Enlargement with inflammation Increase in the size of existing enlargement and adds characteristic features of inflammatory enlargement Red or bluish red discoloration Increased bleeding tendency
Treatment Changing to alternate drug by physician Discontinuation of drug – spontaneous reduction Maintenance of good oral hygiene Plaque control , Mouthwashes Periodontal debridement Surgical excision of gingival overgrowth (gingivictomy)