Chronic Inflammatory Polyradiculoneuropathy (CIDP)
680 likes | 3.66k Vues
Chronic Inflammatory Polyradiculoneuropathy (CIDP). Outline. General Clinical Manifestations Diagnosis Treatment and prognosis. CIDP. Acquired, immune-mediated polyradiculoneuropathy

Chronic Inflammatory Polyradiculoneuropathy (CIDP)
E N D
Presentation Transcript
Outline • General • Clinical Manifestations • Diagnosis • Treatment and prognosis
CIDP • Acquired, immune-mediated polyradiculoneuropathy • Heterogeneous disorder with a wide range of clinical expression ranging from subacute to a progressive or relapsing-remitting course • Diagnosis is based on clinical symptoms and signs, electrodiagnostic studies, CSF examination, and other laboratory tests
CIDP: Clinical Manifestations • Demyelination • May be detected on nerve conduction studies or nerve biopsy • Multifocal demyelination is a diagnostic hallmark of CIDP, but distribution of demyelinative lesions varies among patients • Weakness • Characteristically, involves both proximal and distal muscles • Typically symmetric, but can begin asymmetrically • Sensory symptoms are common but motor symptoms usually predominate • Autonomic system dysfunction can occur
CIDP: Clinical Manifestations • Slow progressive course is seen in approximately 2/3 of cases • Children usually have a more precipitous onset of symptoms • Relapsing course with partial or complete recovery between recurrences is seen in approximately 1/3 of cases • Periods of worsening and improvement usually last weeks or months • Patients with a younger age of onset are said to have a higher frequency of relapsing course
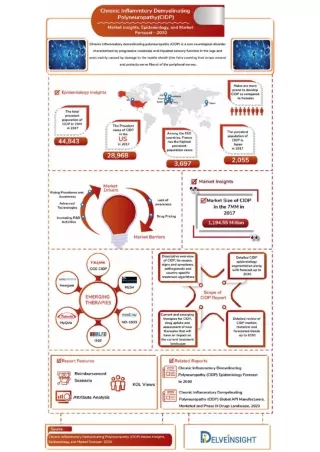
CIDP: Incidence • In one study, prevalence was estimated to range from 1-7.7 per 100,000 • These are likely underestimates, since the criteria to select cases were strict • CIDP accounted for 13% of patients seen in one neuromuscular center • Incidence increases with increasing age • Children are rarely affected
CIDP: Pathophysiology • In one study, CIDP occurred within a few weeks after an infectious event in 16% of the patients • Because of the insidious onset, documenting precipitating illnesses or events is very difficult • Both respiratory and gastrointestinal infections have been cited, but no causative organism has been identified • With Guillain-Barre syndome, the most common preceding infection is Campylobacter Bouchard et al. NEUROLOGY 1999;52:498–503
CIDP: Regional Variants • The classical phenotype that suggests CIDP is the presence of proximal and distal weakness, with large fiber sensory loss and areflexia • Few patients present with classic symtpoms • Some authors have suggested subclassifications based on the clinical phenotype in order to aid in diagnosis and treatment • Currently these subclasses are not thought to be distinct diseases
Lewis-Sumner syndrome Distal acquired demyelinating sensory neuropathy and sensory CIDP Multifocal demyelinating neuropathy with persistent conduction block Distal CIDP Sensory CIDP ANTI-MAG (Myelin Associated Glycoprotein) Neuropathy CIDP with Hypertrophic nerves Subacute demyelinating polyneuropathy Chronic Inflammatory demyelinating neuropathies CIDP: Regional Variants
CIDP: Associated Conditions • Most frequently CIDP is an idiopathic illness • Has been known to occur with several conditions • In these cases, the associated condition is included in the main diagnosis to separate those cases from the idiopathic variety • Example: “CIDP with HIV infection”
CIDP: Associated Conditions • HIV infection • Mild lymphocytic pleocytosis and increased gamma globulin level in the CSF are seen frequently • Hodgkin lymphoma • Associated neuropathy is not caused by direct infiltration of the peripheral nerves but is a consequence of the autoimmune cascade that occurs with this disease, but the mechanism is not completely clear • Paraproteinemias and/or plasma cell dyscrasias
CIDP: Associated Conditions • CIDP is seen with monoclonal gammopathies (eg MGUS), most frequently gammopathy of immunoglobulin M (IgM) • Evidence suggests that CIDP with IgM MGUS has specific clinical and electrophysiologic characteristics • Usually predominance of distal weakness with sensory symptoms greater than motor • Multiple sclerosis • Reports describe CNS white matter changes in patients with CIDP • Whether a true association exists between CIDP and multiple sclerosis remains unclear
CIDP: Associated Conditions • Systemic lupus erythematosus • Chronic active hepatitis (B or C) • CIDP associated with hepatitis should be differentiated from cryoglobulinemic vasculitis • The latter causes either symmetric distal sensorimotor polyneuropathy or mononeuropathy multiplex but on pathologic examination shows wallerian degeneration and not the segmental demyelination seen in CIDP
CIDP: Associated Conditions • Inflammatory bowel disease • CIDP has been described in association with Crohn disease and other inflammatory bowel conditions, although no direct correlation between the two afflictions is known • The mechanism of development of CIDP is presumed to be an autoimmune abnormality that is also causing the primary problem in inflammatory bowel disease, although the details are not known
CIDP: Associated Conditions • Diabetes mellitus • Increasing evidence supports the suggestion that some patients with diabetes who have severe neuropathy or unusually progressive neuropathy may have CIDP superimposed on their diabetic disorder • Diabetes may predispose patients to CIDP • Pregnancy • Known to worsen CIDP • Worsening usually occurs in the third trimester or in the postpartum period
CIDP: Monitoring and Prognosis • Sometimes difficult to assess the activity of a chronic neuropathy • Nerve biopsy can be used to detect active nerve lesions and inflammatory infiltrates • Axonal loss has more long-term prognostic impact than active demyelination or inflammatory infiltrates in demyelinating disorders of the peripheral and central nervous systems
CIDP: Diagnosis • The diagnosis of CIDP is typically based on the clinical presentation, absence of other causes of the neuropathic syndrome, and results of electrodiagnostic studies • Presence of increased cerebrospinal fluid (CSF) protein and demyelinating changes on nerve biopsy are supportive of the diagnosis, but these are not always present
CIDP: Diagnosis • Because of the clinical heterogeneity and the lack of a diagnostic test, various diagnostic criteria have been proposed • In one series of patients all of whom had proximal and distal weakness and in whom 95% of patients had improvement with treatment, only 30% had the classic triad of slow nerve conduction velocity, elevated CSF protein and demyelination on nerve biopsy
American Association of Neurology: Criteria • Developed criteria for the identification of patients with CIDP for research studies • Pathologic criteria • Electrophysiologic criteria: Require 3 demyelinating range abnormalities (either slow conduction velocity, prolonged distal motor latencies or F wave latencies or conduction block) in 2 nerves • Criteria are not sensitive and may miss more than 50 % of patients with CIDP • Specificity approaches 100% • Majority of patients seen in clinical practice fail to meet all of the criteria
Laboratory Studies: CSF • Protein level is increased significantly in 80% of patients • Usually between 50 and 200 mg/dL, but can be higher • 10% of patients also have mild lymphocytic pleocytosis (<50 cells) and increased gamma globulin (usually associated with HIV infection) • CBC, sedimentation rate, antinuclear antibody, biochemistry profile, and serum and urine immunoelectrophoresis are necessary to exclude important associated systemic disorders
CIDP: EMG • Critical test to determine whether the disorder is truly a peripheral neuropathy and whether the neuropathy is demyelinating • Findings of a demyelinating neuropathy • Multifocal conduction block or temporal dispersion of compound muscle action potential • Prolonged distal latencies • Variable conduction slowing to less than 70% of normal • Absent or prolonged F wave latencies • As the disease progresses, patients tend to develop secondary axonal degeneration
CIDP: Peripheral nerve biopsy • Indications • Patients in whom the diagnosis is not completely clear • Cases where other causes of neuropathy (eg, hereditary, vasculitic) cannot be excluded • Caes where profound axonal involvement is observed on EMG • Some experts recommend biopsy for most patients prior to initiating immunosuppressive therapy
CIDP: Histologic Findings • Interstitial and perivascular infiltration of the endoneurium with inflammatory T cells and macrophages with local edema • Evidence exists of segmental demyelination and remyelination with occasional onion bulb formation, particularly in relapsing cases • Some evidence of axonal damage also is observed, with loss of myelinated nerve fibers • The inflammatory infiltrate with neutrophil infiltration is observed in only a minority of patients
CIDP: Histology • Note the decreased density of nerve fibers (arrows) • Demyelinated fibers (D) • Fibers undergoing active macrophagemediated demyelination (M) Bouchard, et al. NEUROLOGY 1999;52:498–503
CIDP: Therapy • Prednisone, IVIg and plasmapheresis have all been demonstrated to be effective in controlled clinical trials • In one study, response was seen to at least 1 of these 3 main therapies in 66% of patients • Only 1/3 of patients have a sustained remission after initial treatment and most require ongoing treatment • Early treatment is advisable to prevent axonal loss and motor neuron loss which leads to functional decline • May be irreversible
CIDP: Therapy • A positive therapeutic response is measured by improvement or stabilization of previously documented progressive weakness, sensory loss, or ataxia • In responsive patients, treatment is continued until maximal improvement or stabilization is achieved, at which point it can be tapered or discontinued • If there is further deterioration or a relapse, the therapy can be re-instituted • Patients with chronic progressive disease require maintenance therapy, although tapering the treatment can be re-attempted periodically to determine continued need
CIDP: Therapy • Prednisone • First line therapy • Agents used for refractory patients • Cyclosporine (Sandimmune, Neoral) • Cyclophosphamide (Cytoxan) • Azathioprine (Imuran) • Mycophenolate (CellCept)
CIDP: Therapy • Neuropathic pain • Antiepileptics • Carbamazepine (Tegretol) • Gabapentin (Neurontin) • Tricyclic antidepressants • Amitriptyline (Elavil)
CIDP: Plasmapheresis • Several controlled studies confirmed benefit • Proposed mechanism • Removal of antibodies and complement components that are responsible for immune-mediated damage of peripheral nerves • Has been shown to have similar efficacy as IVIg in treatment of CIDP
CIDP: Plasmapheresis • Treatment regimens • Not standardized due to a lack of controlled studies • Common regimen • 3 plasma exchanges per week for first 2 weeks • Additional treatment is determined by clinical response
IV Ig • Solution composed mostly of heterogenous human IgG but also small amounts of IgA and IgM • Proposed mechanism of action • IVIg contains random set of antibodies that would neutralize immune factors, causing damage to peripheral nerve in CIDP • Activates complement cascade and provides multitude of antibodies capable of neutralization of many microorganisms, toxins, viruses, and presumably autoantibodies
IV Ig • Used in infectious diseases to provide immediate passive immunity in situations in which time constraints do not allow development of active immunity via vaccination • Also used to treat multiple immune-mediated conditions, such as idiopathic thrombocytopenic purpura, GBS, and myasthenia gravis
CIDP: IV Ig • Several studies showed significant benefit in CIDP • Useful alternative to plasmapheresis • On average, improvement seen by day 10 and continues through day 42 • Serum half-life is approximately 21-29 days • Patients usually require repeated treatments every few weeks or months to maintain remission or treat recurrences
CIDP: Prognosis • The outcome of CIDP is difficult to predict owing to the variety of clinical patterns and evolution • If left untreated, it can become disabling, with loss of ability to ambulate, work, or function independently
References • “Acquired demyelinating neuropathy”. Brain. 119. 257–270. • Ad Hoc Subcommittee of the American Academy of Neurology, AIDS Task Force (1991). “Research criteria for diagnosis of chronic inflammatory demyelinating polyradiculoneuropathy (CIDP)”. Neurology. 41. 617–618.
References • Bouchard, et al. “Clinicopathologic findings and prognosis of chronic inflammatory demyelinating polyneuropathy”.Neurology. February (1 of 1). 1999. 52. 498-503. • Kuwabara, S, et al. “Distribution patterns of demyelination correlate with clinical profiles in chronic inflammatory demyelinating polyneuropathy”. Journal of Neurology Neurosurgery and Psychiatry. 2002. 72. 37-42. • Latov N. “Diagnosis of CIDP”. Neurology. 59. S2–S6.