Spinal stenosis
New York DNS & Physical Therapy center is the first one in the niche to practise Dynamic Neuromuscular Stabilization therapy method in New York. Its professional medicine employees have more than 18 years of experience.


Spinal stenosis
E N D
Presentation Transcript
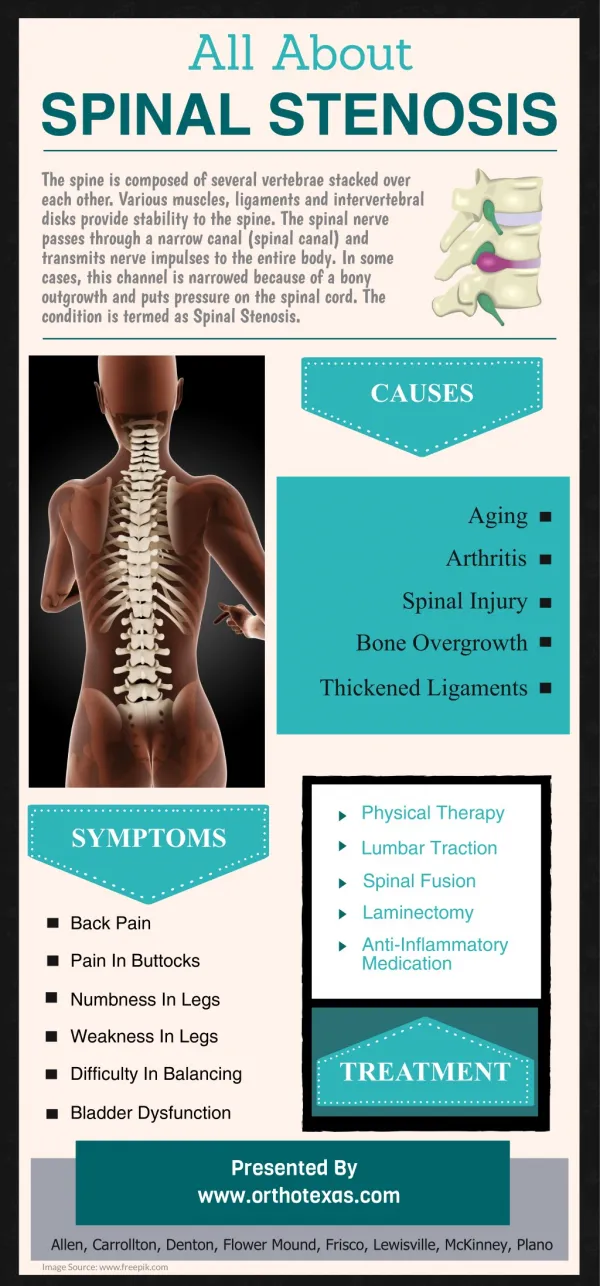
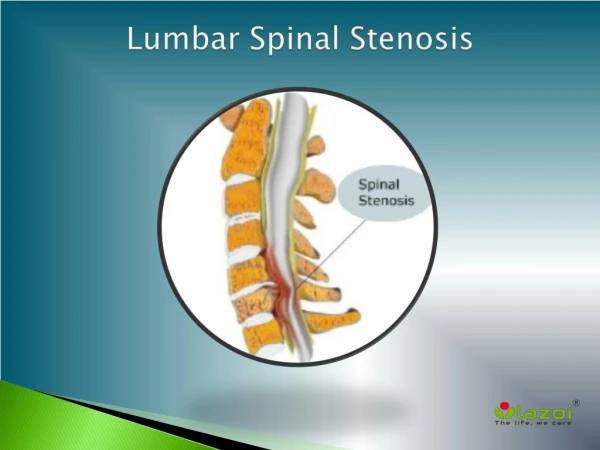
Spinal stenosis Definition Spinal stenosis is a narrowing of the open spaces within your spine, which can put pressure on your spinal cord and the nerves that travel through the spine to your arms and legs. Spinal stenosis occurs most often in the lower back and the neck. While spinal stenosis may cause no signs or symptoms in some people, other people may experience pain, tingling, numbness, muscle weakness, and problems with normal bladder or bowel function. Spinal stenosis is most commonly caused by wear-and-tear changes in the spine related to osteoarthritis. In severe cases of spinal stenosis, doctors may recommend surgery to create additional space for the spinal cord or nerves. Symptoms Many people have evidence of spinal stenosis on X-rays, but may not have signs or symptoms. When symptoms do occur, they often start gradually and worsen over time. Symptoms vary, depending on the location of the stenosis: ● In the neck (cervical spine). Cervical stenosis can cause numbness, weakness or tingling in a leg, foot, arm or hand. Tingling in the hand is the most common symptom, and many people also report problems with walking and balance. Nerves to the bladder or bowel may be affected, leading to incontinence. ● In the lower back (lumbar spine). Compressed nerves in your lumbar spine can cause pain or cramping in your legs when you stand for long periods of time or when you walk. The discomfort usually eases when you bend forward or sit down. When to see a doctor Make an appointment with your doctor if you have persistent pain, numbness or weakness in your back, legs or arms. Causes While some people are born with a small spinal canal, most spinal stenosis occurs when something happens to reduce the amount of space available within the spine. Causes of spinal stenosis may include: ● Overgrowth of bone. Wear and tear damage from osteoarthritis on your spinal bones can prompt the formation of bone spurs, which can grow into
the spinal canal. Paget's disease, a bone disease that usually affects adults, also can cause bone overgrowth in the spine. ● Herniated disks. The soft cushions that act as shock absorbers between your vertebrae tend to dry out with age. Cracks in a disk's exterior may allow some of the soft inner material to escape and press on the spinal cord or nerves. ● Thickened ligaments. The tough cords that help hold the bones of your spine together can become stiff and thickened over time. These thickened ligaments can bulge into the spinal canal. ● Tumors. Abnormal growths can form inside the spinal cord, within the membranes that cover the spinal cord or in the space between the spinal cord and vertebrae. ● Spinal injuries. Car accidents and other major trauma can cause dislocations or fractures of one or more vertebrae. Displaced bone from a spinal fracture may damage the contents of the spinal canal. Swelling of adjacent tissue immediately following back surgery also can put pressure on the spinal cord or nerves. Risk factors Most people with spinal stenosis have passed the age of 50. When younger people develop spinal stenosis, the cause is typically a genetic disease affecting bone and muscle development throughout the body. Complications Rarely, untreated cases of severe spinal stenosis may progress and cause permanent: ● Numbness ● Weakness ● Balance problems ● Incontinence ● Paralysis Preparing for your appointment If your family doctor suspects that you have spinal stenosis, he or she may refer you to a doctor who specializes in disorders of the nervous system (neurologist). Depending on the severity of your symptoms, you might also be referred to a spinal surgeon. What you can do Before the appointment, you might want to prepare a list of answers to the following questions:
● When did you first notice this problem? ● Has it worsened with time? ● Have your parents or siblings ever had similar symptoms? ● Do you have other medical problems? ● What medications or supplements do you take regularly? What to expect from your doctor Your doctor may ask some of the following questions: ● Do you have pain? Where is it? ● Does any position ease the pain or worsen it? ● Do you have any weakness, numbness or tingling? ● Do you feel clumsier lately? ● Have you had any difficulty controlling your bowel or bladder? ● What treatments have you tried already for these problems? Tests and diagnosis Spinal stenosis can be difficult to diagnose because its signs and symptoms resemble those of many age-related conditions. Imaging tests may be needed to help pinpoint the true cause of your signs and symptoms. Imaging tests These tests may include: ● X-rays. Using a small exposure to radiation, X-rays can reveal bony changes, such as bone spurs that may be narrowing the space within the spinal canal. ● Magnetic resonance imaging (MRI). In most cases, this is the imaging test of choice for diagnosing spinal stenosis. Instead of X-rays, an MRI uses a powerful magnet and radio waves to produce cross-sectional images of your spine. The test can detect damage to your disks and ligaments, as well as the presence of tumors. Most important, it can show pressure on the spinal cord or spinal nerves. ● CT myelogram. If you can't have an MRI, your doctor may recommend computerized tomography (CT), a test that combines X-ray images taken from many different angles to produce detailed, cross-sectional images of your body. In a CT myelogram, the CT scan is conducted after a contrast dye is injected. The dye outlines the spinal cord and nerves, and it can reveal herniated disks, bone spurs and tumors. Treatments and drugs
The type of treatment you receive for spinal stenosis may vary, depending on the location of the stenosis and the severity of your signs and symptoms. Medications To control pain associated with spinal stenosis, your doctor may prescribe: ● NSAIDs. Nonsteroidal anti-inflammatory drugs (NSAIDs) help relieve pain and reduce inflammation common to osteoarthritis. Some NSAIDs, such as ibuprofen (Advil, Motrin IB, others) and naproxen (Aleve), are available without prescription. ● Muscle relaxants. Medications such as cyclobenzaprine (Amrix, Fexmid) can calm the muscle spasms that occasionally occur with spinal stenosis. ● Antidepressants. Nightly doses of tricyclic antidepressants, such as amitriptyline, can help ease chronic pain. ● Anti-seizure drugs. Some anti-seizure drugs, such as gabapentin (Neurontin, Gralise, Horizant) and pregabalin (Lyrica), are used to reduce pain caused by damaged nerves. ● Opioids. Drugs that contain codeine-related drugs such as oxycodone (Percocet, OxyContin, others) and hydrocodone (Norco, Zohydro, others) can be habit-forming. Therapy It's common for people who have spinal stenosis to become less active, in an effort to reduce pain. However, that can lead to muscle weakness, which can result in more pain. A physical therapist can teach you exercises that may help: ● Build up your strength and endurance ● Maintain the flexibility and stability of your spine ● Improve your balance Steroid injections Your nerve roots may become irritated and swollen at the spots where they are being pinched. Injecting a corticosteroid into the space around that constriction can help reduce the inflammation and relieve some of the pressure. However, steroid injections don't work for everyone. And repeated steroid injections can weaken nearby bones and connective tissue, so only a few injections a year are suggested. Surgery Surgery may be considered if more conservative treatments haven't helped or if you're disabled by your symptoms.
The goal is to relieve the pressure on your spinal cord or nerve roots by creating more space within the spinal canal. Examples include: ● Laminectomy. The procedure removes the back part (lamina) of the affected vertebra. In some cases, that vertebra may need to be linked to adjoining vertebrae with metal hardware and a bone graft (spinal fusion) to maintain the spine's strength. ● Laminotomy. This procedure removes only a portion of the lamina, typically carving a hole just big enough to relieve the pressure in a particular spot. ● Laminoplasty. This procedure is performed only on the vertebrae in the neck. It opens up the space within the spinal canal by creating a hinge on the lamina. Metal hardware bridges the gap in the opened section of the spine. In most cases, these space-creating operations help reduce spinal stenosis symptoms. But some people's symptoms stay the same or get worse after surgery. Surgical risks include infection, a tear in the membrane that covers the spinal cord, a blood clot in a leg vein and neurological deterioration. Lifestyle and home remedies The following home treatments might help: ● Pain relievers. Over-the-counter medications such as ibuprofen (Advil, Motrin IB, others) and naproxen (Aleve) can help reduce pain and inflammation. ● Hot or cold packs. Some symptoms of cervical spinal stenosis may be relieved by applying heat or ice to your neck. ● Diet and nutrition. Losing excess weight can reduce load-bearing stress on the lumbar spine. ● Canes or walkers. In addition to providing stability, these assistive devices can help relieve pain by allowing you to bend forward while walking. What Is Spinal Stenosis? Spinal stenosis is a condition, mostly in adults 50 and older, in which your spinal canal starts to narrow. This can cause pain and other problems. Your spine is made up of a series of connected bones (or “vertebrae”) and shock-absorbing discs. It protects your spinal cord, a key part of the central nervous
system that connects the brain to the body. The cord rests in the canal formed by your vertebrae. For most people, the stenosis results from changes because of arthritis. The spinal canal may narrow. The open spaces between the vertebrae may start to get smaller. The tightness can pinch the spinal cord or the nerves around it, causing pain, tingling, or numbness in your legs, arms, or torso. There’s no cure, but there are a variety of nonsurgical treatments and exercises to keep the pain at bay. Most people with spinal stenosis live normal lives. Causes The leading reason for spinal stenosis is arthritis, a condition caused by the breakdown of cartilage -- the cushiony material between your bones -- and the growth of bone tissue. Osteoarthritis can lead to disc changes, a thickening of the ligaments of the spine, and bone spurs. This can put pressure on your spinal cord and spinal nerves. Other causes include: ● Herniated discs. If the cushions are cracked, material can seep out and press on your spinal cord or nerves. ● Injuries. An accident may fracture or inflame part of your spine. ● Tumors. If cancerous growths touch the spinal cord, you may get stenosis. ● Paget’s disease. With this condition, your bones grow abnormally large and brittle. The result is a narrowing of the spinal canal and nerve problems. Some people are born with spinal stenosis or diseases that lead to it. For them, the condition usually starts to cause problems between the ages of 30 and 50. Symptoms Spinal stenosis usually affects your neck or lower back. Not everyone has symptoms, but if you do, they tend to be the same: stiffness, numbness, and back pain.
More specific symptoms include: ● Sciatica. These shooting pains down your leg start as an ache in the lower back or buttocks. ● Foot drop. Painful leg weakness may cause you to “slap” your foot on the ground. ● A hard time standing or walking. When you’re upright, it tends to compress the vertebrae, causing pain. ● Loss of bladder or bowel control. In extreme cases, it weakens the nerves to the bladder or bowel. If you’re having symptoms, you might want to talk them over with your doctor. If you’re having a loss of bladder or bowel control, call your doctor at once. Diagnosis and Tests When you visit your doctor, she’s likely to ask you questions about your medical history. After that, she might order at least one of the following tests to figure out whether you have the condition: ● X-rays. These can show how the shape of your vertebrae has changed. ● Magnetic resonance imaging (MRI). By using radio waves, an MRI creates a 3-D image of your spine. It can show tumors, growths, and even damage to discs and ligaments. ● Computerized tomography (CT scan). A CT scan uses X-rays to create a 3-D image. With the help of a dye injected into your body, it can show damage to soft tissue as well as issues with your bones. Treatment Your doctor may start off with nonsurgical treatments. These might include: Medication: Common pain remedies such as aspirin, acetaminophen (Tylenol), ibuprofen (Advil, Motrin), and naproxen can offer short-term relief. All are available in low doses without a prescription. Other medications, including muscle relaxants and
anti-seizure medications, treat aspects of spinal stenosis, such as muscle spasms and damaged nerves. Corticosteroid injections: Your doctor will inject a steroid such as prednisone into your back or neck. Steroids make inflammation go down. However, because of side effects, they are used sparingly. Anesthetics: Used with precision, an injection of a “nerve block” can stop pain for a time. Exercise: You can improve your flexibility, strength, and balance with regular activity. Your doctor may recommend a physical therapist to help you. Assistive devices: You might get braces, a corset, or a walker to help you move about. Surgery Some people have severe cases. They struggle to walk or have issues with their bladder and bowel. Doctors may recommend surgery for these people. Procedures such as laminectomy and laminoplasty create space between the bones so inflammation can go down. Surgery carries its own risks. You should have a talk with your doctor about how much it can help, recovery time, and more before taking that step. Many patients also try nontraditional therapies, including chiropractic and acupuncture. Again, be sure your doctor knows if you’re trying a nontraditional approach. What You Can Do at Home Some things you can do to help ease symptoms of spinal stenosis include: ● Exercise. Think about moderation -- not 100 push-ups. Just take a 30-minute walk every other day. Talk over any new exercise plan with your doctor. ● Apply heat and cold. Heat loosens up your muscles. Cold helps heal inflammation. Use one or the other on your neck or lower back. Hot showers are also good.
● Practice good posture. Stand up straight, sit on a supportive chair, and sleep on a firm mattress. And when you lift heavy objects, bend from your knees, not your back. ● Lose weight. When you are heavier, there will be more pressure on your back. Spinal stenosis refers to a "choking" or compression of the spinal nerve roots or the spinal cord. There are two types of stenosis: lumbar stenosis and cervical stenosis. In the medical field, stenosis means the abnormal narrowing of a body channel. When combined with the word spinal, it defines a narrowing of the bone channel occupied by the spinal nerves or the spinal cord. Some people are born with a congenital form, but most develop spinal stenosis as part of the degenerative cascade. A few do not feel any effects of the narrowing, but as part of the aging process, most people will eventually notice radiating pain, weakness, and/or numbness secondary to the compression of the nerves or spinal cord. While the narrowing may occur at different parts of the spine, the symptoms of nerve compression are often similar. That is why specialists often will perform testing to determine the cause and location of the narrowing. Lumbar vs. Cervical Stenosis Lumbar Spinal Stenosis In lumbar stenosis, the spinal nerve roots in the lower back become compressed and this can produce symptoms of sciatica—tingling, weakness or numbness that radiates from the low back and into the buttocks and legs—especially with activity. Lumbar spinal stenosis often mimics symptoms of vascular insufficiency. Both conditions can cause claudication, which means leg pain with walking. If vascular studies identify normal blood flow, and there is confirmation of spinal stenosis on diagnostic testing, the symptoms are then called neurogenic claudication. In the classic description, people with spinal stenosis will describe an onset of leg pain, or weakness with walking, but with relief of symptoms with sitting. Many will also describe increased tolerance to walking when flexed forward, such as when walking while leaning forward on a shopping cart.
While lumbar spinal stenosis most often occurs at the L4-L5 and L3-L4 levels, it can occur any level in the spine. The degenerative cascade may eventually effect most of the vertebral segments of the lumbar spine. Cervical Stenosis Spinal stenosis pain in the neck is called cervical spinal stenosis. This condition means that there is potential compression of the spinal cord. Unfortunately, the spinal cord compression can lead to serious problems such as extreme weakness, or even paralysis. With cervical stenosis, anyone who develops signs of spinal cord compression (myelopathy) may need more invasive treatment, such as surgery. Thoracic stenosis can also occur, but is less common. The thoracic part of the spine is the middle/upper portion of the spine, and mainly consists of the vertebrae that are attached to the rib cage. This stable and strong part of the spine allows for minimal movement, which is why degenerative conditions such as spinal stenosis are less likely to develop. Spinal Stenosis and the Aging Spine Spinal stenosis is related to degeneration in the spine and usually will become significant in the 5th decade of life and extend throughout every subsequent age group. As it is a gradual process and rarely causes immediate symptoms, the subtle changes of spinal stenosis often result in a gradual decrease in physical activity, and a development of a more kyphotic or forward flexed posture. This gradual accommodation may be evident when looking at a series of oneself in pictures—over the course of several years—after around age 50. It is typical to start stooping forward more and become less active as effects of spinal stenosis increase. https://nydnrehab.com/what-we-treat/back-pain-and-neck-pain/spinesten/