TOPIC 8 Digestive System
Biology 221 Anatomy & Physiology II. TOPIC 8 Digestive System. Chapter 18 pp. 651-677. E. Lathrop-Davis / E. Gorski / S. Kabrhel. Digestive System Functions. The digestive system: provide nutrients in usable form; and removes unusable wastes from the body. Digestive System Overview.

TOPIC 8 Digestive System
E N D
Presentation Transcript
Biology 221 Anatomy & Physiology II TOPIC 8Digestive System Chapter 18 pp. 651-677 E. Lathrop-Davis / E. Gorski / S. Kabrhel
Digestive System Functions The digestive system: • provide nutrients in usable form; and • removes unusable wastes from the body.
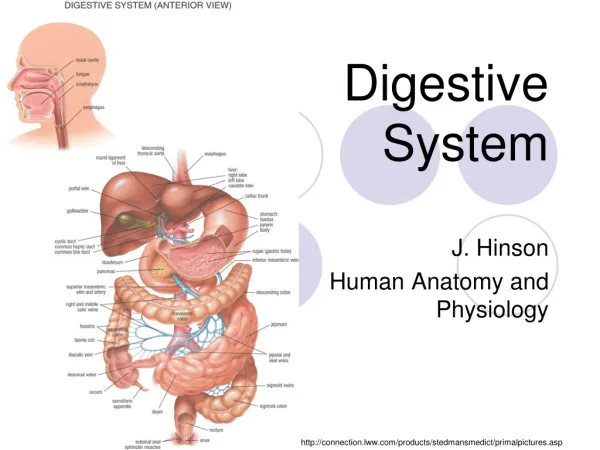
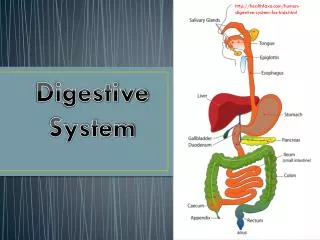
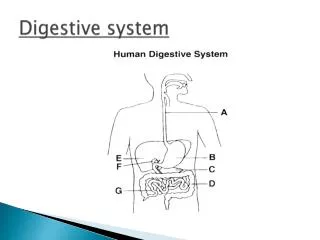
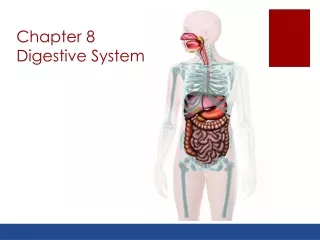
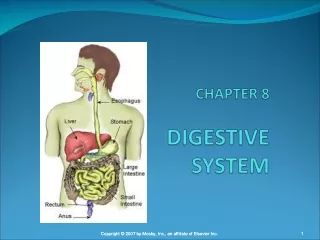
Digestive System Overview There are two main groups of organs: • The alimentary canal (also known as the gastrointestinal or GI tract) is the tube through which food passes. • The GI tract is responsible for digestion and absorption of food. • Organs of the GI tract include the mouth, pharynx, esophagus, stomach, small intestine, and large intestine. Fig. 24.1, p. 888
Digestive System Overview • Accessory organs are organs, glands and structures which aid digestion but not part of GI tract itself. • Accessory organs include the teeth, tongue, salivary glands, pancreas, liver, and gall bladder. Fig. 24.1, p. 888
Processes of Digestion There are 6 main processes involved in digestion: • Ingestion is the entrance of food and drink into the mouth. • Mechanical digestion is the physical breakdown into smaller pieces. • Propulsion is movement of materials through the gut. • Chemical digestion is the breakage of bonds in molecules to form smaller compounds. • Absorption is the uptake of nutrients from lumen (if it’s not absorbed, it’s not usable). • Defecation is the removal of indigestible material (like cellulose) Fig. 24.2, p. 889
Peritoneum • The peritoneum is a serous membrane. • The parietal peritoneum lines the abdominal cavity. • Organs posterior to the parietal peritoneum are retroperitoneal. • The visceral peritoneum (also called the serosa) covers surfaces of most abdominal organs. • Mesenteries are a double layer of peritoneum extending from the body wall to certain digestive organs • Intraperitoneal organs are ones found in the mesentaries. See also Fig. 24.5, p. 891 Fig,. 24.30, p. 929
Peritoneum • The peritoneal cavity is the fluid-filled “space” between the visceral and parietal peritoneum. • Peritonitis is any inflammation of the peritoneum. It makes movement within the gut more difficult and painful. See also Fig. 24.5, p. 891 Fig,. 24.30, p. 929
Splanchnic Circulation Arteries serving the digestive organs are branches of the abdominal aorta. • The celiac trunk is the first branch of the abdominal aorta. It is very short; gives rise to: • hepatic artery, which serves the liver, gall bladder, stomach, and duodenum; • left gastric artery serving the stomach and inferior esophagus; and the • splenic artery serving the spleen, stomach, and pancreas. Fig. 20.22, p. 761 Fig. 20.22, p. 759
Splanchnic Circulation • The superior mesenteric artery supplies the small intestine and most of large intestine, and the pancreas. • The inferior mesenteric artery serves the large intestine. Fig. 20.22, p. 761 Fig. 20.22, p. 759
Hepatic Circulation: Hepatic portal system • The hepatic portal system consistes of veins draining digestive organs and carrying nutrient-rich blood to the liver. • The gastric veindrains the stomach. • The superior mesenteric veindrains the small intestine. • The splenic veindrains spleen. • The inferior mesenteric vein drains the large intestine and empties into the splenic vein. • Venous blood from the hepatic portal system mixes with arterial blood (from the hepatic artery) in liver. Fig. 20.27, p. 771
Hepatic Circulation: Hepatic Veins • drain venous blood from liver into inferior vena cava Fig. 20.27, p. 771
Mucosa • The mucosa is the mucous membrane lining the gut. • The mucosa consists of: • an epithelial lining; • a lamina propria of areolar connective tissue; and • the muscularis mucosae of smooth muscle. http://www.usc.edu/hsc/dental/ghisto/gi/d_1.html
Mucosa: Epithelium • Type of tissue comprising the epithelium varies depending on location. • Stratified squamous epithelium is found in mouth, esophagus and anal canal where abrasion is likely. • Simple columnar epithelium is found in stomach and intestines where secretion and absorption are important. • The epithelium secretes mucus, digestive enzymes, and hormones. • It provides an intact barrier to protect against entry of bacteria. http://www.usc.edu/hsc/dental/ghisto/gi/d_15.html http://www.usc.edu/hsc/dental/ghisto/gi/c_2.html
Mucosa: Lamina Propria • The lamina propria is a ayer of areolar connective tissue. • Blood capillaries nourish epithelium, absorb and transport digested nutrients. • Lymphatic capillaries provide drainage for interstitial fluid and transport fats to the venous circulation. http://www.usc.edu/hsc/dental/ghisto/gi/d_60.html
Mucosa: Muscularis Mucosae • The muscularis mucosae consists of smooth muscle. • It is used for local movement and to hold mucosa in folds (small intestine) http://education.vetmed.vt.edu/Curriculum/VM8054/Labs/Lab19/EXAMPLES/Exileum.htm
Submucosa • The submucosa is dense connective tissue superficial to the mucosa. • It is highly vascularized with many lymphatic vessels. • Lymph nodules help protect against diseases. • MALT, or mucosa-associated lymphatic tissue, is common especially in the small intestine (as Peyer’s Patches) and large intestines. http://education.vetmed.vt.edu/Curriculum/VM8054/Labs/Lab19/EXAMPLES/Exileum.htm
Muscularis Externa (Muscularis) • The mucularis consists of two layers in most organs (3 in stomach). • The circular layer runs around the tube. • The longitudinal layer runs the length of the tube. • Peristalsis moves material through gut by alternating contraction of circular and longitudinal muscle. • Segmentation is a series of ring-like contractions that help mix material with digestive enzymes in small intestine Fig. 24.3, p. 890
Serosa • The visceral peritoneum, or serosa, is composed of simple squamous epithelium (mesothelium) with areolar CT. • The adventitia is a dense connective tissue covering without epithelium. It is found around the esophagus. • Retroperitoneal organs have both a serosa (of parietal peritoneum) and adventitia (on the side abutting body wall).
Enteric Nervous System Intrinsic nerve plexuses consist of enteric neurons. • Enteric neurons are able to act independently of central nervous system. • They communicate with each other to control GI activity. • There are two main enteric plexuses. • The submucosal nerve plexus regulates glands in submucosa and smooth muscle of muscularis mucosae. • The myenteric nerve plexus regulates activity of muscularis externa (with aide of submucosal nerve plexus).
Central Nervous System Control • Enteric nerve plexuses linked to CNS by visceral afferent (sensory) fibers • The digestive system receives motor input from the sympathetic and parasympathetic divisions of the autonomic nervous system. • Parasympathetic outflow generally increases activity. • Sympathetic outflow generally decreases activity.
Mouth (Oral Cavity) • The oral oriface is the anterior opening. • The mouth is continuous posteriorly with the oropharynx. • The lips and cheeks keep food in oral cavity. • There ar three layers of tissue in the mouth wall: • the mucosa (stratified squamous epithelium); • the submucosa; and • the muscularis externa, which consists of skeletal muscle for voluntary control.
Mouth: Palate • The palate separates the oral and nasal cavities and is why you can chew and breath at the same time. • The hard palate consists of the palatine process of maxilla and the palatine bones. • The soft palate is composed of muscle only. • It prevents food from entering nasopharynx during swallowing. • The uvula is the part that hangs down in middle. Fig. 24.7, p. 895
Mouth: Arches • The palatoglossal arch anchors the soft palate to the tongue. • The palatopharyngeal arch anchors the soft palate to the wall of the oropharynx. • The fauces refers to the area between these arches. The palatine tonsils are located in the fauces. Fig. 24.7, p. 895
Mouth: Tongue • The lingual tonsil sits at base of tongue and protects against invasion by bacteria (see Topic 5 - Lymphatic System). • Taste buds contain receptors for taste. They are scattered over the tongue in papillae. Fig. 24.8, p. 896
Mouth: Tongue • The tongue forms a bolus, or ball, of food, making it easier to swallow. • The tongue also keeps the food between the teeth. • Muscles are served by the Hypoglossal (XII) nerve (see A&P I Unit VI). • Intrinsic muscles within tongue (not attached to bone) allow the tongue to change shape for swallowing and speech. • Extrinsic muscles attach to bone or the soft palate and alter tongue position (protrusion, retraction, side-to-side). Fig. 24.7, p. 895
Salivary Glands • The salivary glands produce saliva. • There are two groups of salivary glands: • The intrinsic glands (or buccal glands) lie within the oral cavity. • The3 pairs of extrinsic glands (see A&P I Unit VI for innervation) lie outside the cavity. They are: • the parotid glands (connected to oral cavity by parotid duct; mumps is a viral infection of the parotid glands); • the sublingual glands; and • the submandibular glands. Fig. 24.9, p. 897
Saliva • Mucus cells in the salivary glands are less common than serous cells and produce mucus to lubricate the food. • Serous cells produce a watery saliva that is composed mostly (97-99.5%) of water. • This saliva is slightly acidic (pH ~ 6.8). • It contains several types of solutes including: • electrolytes (ions such as Na+, K+, Cl-, PO4=, HCO3-), • metabolic wastes (urea, uric acid), and • proteins.
Salivary Proteins Salivary proteins include: • mucin, the glycoprotein portion of mucus that lubricates oral cavity; • lysozyme, which has antibacterial properties; • IgAantibodies that prevent antigens from attaching to the mucus membrane; • defensins secreted by neutrophils that act as local antibiotic and chemotatic agents when the mucosa is damaged; and • salivary amylase, which begins starch hydrolysis.
Control of Salivation • The sympathetic division of the ANS either: • stimulates production of mucin-rich saliva, or • inhibits salivation altogether at high levels. • The parasympathetic division of ANS stimulates activity. • Chemoreceptors (excited most by acidic substances) and baroreceptors (excited by mechanical stimuli) send messages to the salivatory nuclei in pons and medulla. This results in increased parasympathetic motor output. • Parasympathetic motor output results in increased salivation.
Control of Salivation • The salivary nuclei are also under psychological control, wherein they respond to visual and olfactory stimuli, even thoughts of food, by increasing parasympathetic output. • Salivary nuclei are also stimulated by irritation to the lower GI tract. • Parasympathetic nerves that stimulate salivation are the: • the facial, which goes to the submandibular and sublingual salivary glands; and • the glossopharyngeal, which goes to the parotid salivary glands.
Teeth • Teeth lie in the alveoli of the mandible and maxilla (see A&P I axial skeleton lab). • Primary dentition refers to the 20 deciduous teeth (also called milk or baby teeth). • The roots are absorbed as the permanent teeth grow in causing the baby teeth to fall out. Fig. 24.10, p. 899
Teeth Permanent dentition refers to the 32 adult teeth. Each jaw contains: • 4 Incisors (central and lateral) • 2 Canines (eyeteeth) • 4 Bicuspids = premolars • Molars • 2 first molars • 2 second molars • 2 third molars, which are also called wisdom teeth, and may become impacted as they grow in. When this happens they are surgically removed. Fig. 24.10, p. 899
Tooth Structure • The crown is the part visible above the gum line. It is covered by enamel (the hardest substance in body) with dentin under it. • The neck is the area between the crown and the root. • The root has no enamel; its dentin is under the cementum. • Cementum is calcified connective tissue covering the dentin of root. It attaches the root to the periodontal ligament which anchors tooth into the alveolus. • The pulp cavity houses blood vessels and nerves that enter or leave via the apical foramen in the root canal (narrowed end of the cavity). Fig. 24.11, p. 900
Pharynx • Only oropharynx and laryngopharynx are involved in digestion (nasopharynx is only respiratory). • The pharynx is lined with nonkeratinized stratified squamous epithelium to protect against abrasion. • Mucus-producing glands in submucosa produce mucus that lubricates food. • Skeletal muscle in the wall responds to somatic reflexes to move food quickly past laryngopharynx. • There is no serosa or adventitia around the pharynx.
Esophagus • The esophagus runs from the laryngopharynx through the mediastinum to the stomach. • All 4 tissue layers are present in its wall. • The mucosa consists of stratified squamous epithelium. • The submucosa consists of dense irregular connective tissue with mucus-secreting esophageal glands. http://www.usc.edu/hsc/dental/ghisto/gi/c_2.html
Esophagus • The muscularis changes muscle type as it goes down. • The top 1/3 is skeletal muscle • The middle 1/3 is a mix of skeletal and smooth muscle. • The bottom 1/3 is smooth muscle. • The adventitia is the dense connective tissue covering of the esophagus. http://www.usc.edu/hsc/dental/ghisto/gi/d_8.html http://www.usc.edu/hsc/dental/ghisto/gi/d_3.html
Structures Associated with the Esophagus • The upper esophageal sphincter controls movement of material from pharynx into esophagus. • The esophageal hiatus is the opening in the diaphragm that allows the esophagus to pass from the thoracic cavity into the abdominal cavity. • The gastroesophageal (cardiac) sphincter is a thickening of smooth muscle at the inferior end of the esophagus. • It is aided by diaphragm in closing the bottom of the esophagus. • This helps prevent reflux of acidic gastric juice.
Esophageal Disorders • Heartburn results from a failure of the lower esophageal sphincter to close completely allowing acidic gastric juice into esophagus. • Hiatus hernia refers to the protrusion of the superior portion of stomach above diaphragm through the esophageal hiatus. • An esophageal ulcer is an erosion of the esophageal wall due to chronic reflux of stomach acid. An ulcer represents a chemical burn to the esophageal wall.
Digestive Processes in Mouth, Pharynx and Esophagus • Ingestion is taking food into the mouth. • Mechanical digestion in the mouth consists of mastication by teeth (with aid of tongue) and formation of a bolus. • Chemical digestion of carbohydrates starts with salivary amylase produced by the salivary glands. • Amylase breaks starch and glycogen into smaller fragments (including maltose [disaccharide] if left long enough, which is why a cracker starts to taste sweet if left in the mouth). • Activity of salivary amylase continues until it reaches acid environment of the stomach.
Digestive Processes in Mouth, Pharynx and Esophagus • Absorption in the mouth, pharynx and esophagus is almost nil with the exception of some drugs, such as nitroglycerine. • Movement of food in these areas includes deglutition (swallowing) and peristalsis through the esophagus. • Deglutition moves food from oral cavity to stomach. • The process is voluntary in the oral cavity (buccal phase) and reflexive in the pharynx. • Think About It: What is the importance of having deglutition be reflexive in the pharynx? • Peristalsis occurs and is involuntary where smooth muscle is found. Fig. 24.13, p.904
Stomach: Gross Anatomy • The cardiac region (cardia) is the first area into which the food goes. • The fundus is a temporary storage area at the upper left of the stomach. • The body is the main portion of the stomach. • The greater curvature runs along the inferior surface of the stomach; • the lesser curvature, along the upper surface. • The pyloric regionis the distal portion leading into the small intestine. • The pyloric sphinctercontrols movement of chyme into small intestine. Fig. 24.14, p. 905
Stomach: Gross Anatomy • Arterial blood is supplied by the gastric arteries and the splenic artery. (See 20.22, p. 758) • Venous blood is drained by the gastric veins, which empty into the splenic vein or directly into the hepatic portal vein. http://medlib.med.utah.edu/WebPath/GIHTML/GI194.html http://medlib.med.utah.edu/WebPath/GIHTML/GI194.html Fig. 24.14, p. 905
Stomach Histology • The mucosa consists of simple columnar epithelium. • The muscularis mucosae throws mucosa into folds called rugae. • The submucosaconsists of connective tissue. • The muscularis has 3 layers that allow it to create mixing waves in addition to peristalsis. The three layers are from outside to inside: • the longitudinal layer; • the circular layer; and • the oblique layer . • The serosa covers the stomach. http://www.gutfeelings.com/STOMACH.HTML Fig. 24.14, p. 905
Microscopic Anatomy • The surface of the epithelium is composed mainly of goblet cells that secrete mucus. • Gastric pits are downward extensions of the epithelium. • Tight junctions between epithelial cells prevent acidic gastric juice from reaching underlying layers. • Gastric pits contain gastric glands which secrete gastric juice. Four types of cells are present. Fig. 24.15, p. 906 http://www.usc.edu/hsc/dental/ghisto/gi/d_15.html
Gastric Pit Cells • Mucous neck cells secrete bicarbonate-rich mucus • Parietal (oxyntic) cells secrete: • HCl ( which is buffered by bicarbonate rich mucus to protect the mucosa); and • intrinsic factor (which is essential to absorption of Vit. B12 by small intestine). • Chief (zymogenic) cells secrete: • pepsinogen (inactive form of the protease pepsin for protein hydrolysis); and • minor amounts of lipases (which hydrolyze lipids).
Gastric Pit Cells • Enteroendocrine cells release hormones and hormone-like products into the lamina propria where they are picked up by blood and carried to other digestive organs. • Gastrin is generally stimulatory. • Histamine stimulates H+ secretion. • Somatostatin is generally inhibitory.
Digestive Processes in Stomach • Mechanical digestion in the stomach is the result of mixing waves, which help break food into smaller particles. • Chemical digestion in the stomach produces chyme with a pH of about 2. • Acid (HCl) secreted by parietal cells breaks some bonds and activates pepsinogen into pepsin. • Pepsin hydrolyses proteins and is produced as pepsinogen by chief cells. • Think About It: What would happen if pepsin were activated in the gastric pit? • Rennin is a protease secreted in children that acts on milk proteins.
Digestive Processes in Stomach • Movementin the stomach includes: • mixing waves that mix food with acid and enzymes; and • peristalsis that moves material through stomach and into small intestine. • Absorption is limited to lipid soluble substances such as: • alcohol, • aspirin, and • some other drugs.
Regulation of Gastric Secretion Gastric secretion is controlled by the autonomic nervous system and hormones. • Hormonal control is accomplished by locally secreted hormones. • Gastrin from the stomach stimulates secretion. • Somatostatin, gastric inhibitory protein (GIP), and cholecystokinin from the small intestine inhibit secretion. Somatostatin is also produced by the stomach itself. See Fig. 24.16, p. 910
Regulation of Gastric Secretion • Neural control is accomplished by the ANS and local enteric nerve reflexes. • Autonomic control starts in the CNS. • The parasympathetic division works through the Vagus (X) nerve and stimulates activity. • The sympathetic division works through thoracic spinal nerves and inhibits activity. • Local enteric nerve reflexes are based on distension of the stomach or duodenum. • Distension of the stomach stimulates gastric activity • Distension of the duodenum inhibits gastric activity. See Fig. 24.16, p. 910