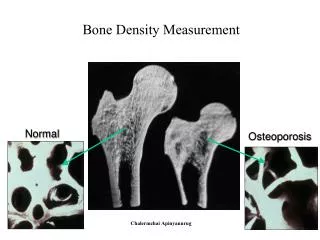
Normal Hemopoiesis
Normal Hemopoiesis. Ahmad Sh. Silmi Msc Haematology, FIBMS. Lifespan and production of blood cells. So our body is in a continuous dynamic and a very rapid cell turnover to be able to live. HOW ? It ’ s the Stem Cell !. HEMOPOIESIS: INTRO. Hemo : Referring to blood cells


Normal Hemopoiesis
E N D
Presentation Transcript
Normal Hemopoiesis Ahmad Sh. Silmi Msc Haematology, FIBMS
So our body is in a continuous dynamic and a very rapid cell turnover to be able to live. • HOW ? • It’s the Stem Cell !
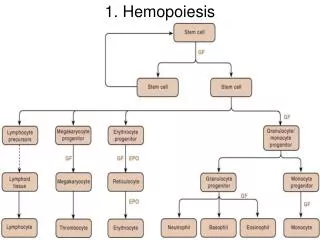
HEMOPOIESIS: INTRO Hemo: Referring to blood cells Poiesis: “The development or production of” The word Hemopoiesis refers to the production & development of all the blood cells: Erythrocytes:Erythropoiesis Leucocytes:Leucopoiesis Thrombocytes:Thrombopoiesis.
HEMOPOIESIS • Hemopoiesis depends on 3 important components: • the bone marrow stroma (Local control) • the hemopoietic stem and progenitor cells • the hemopoietic growth factors (Humoral control)
STEM CELL THEORY The dazzling array of all the blood cells are produced by thebone marrow. They all come from a single class of primitive mother cells called as: PLURIPOTENT STEM CELLS. These cells give rise to blood cells of: Myeloid series: Cells arising mainly from the bone marrow. Lymphoidseries: cells arising from lymphoid tissues.
STEM CELLS These cells have extensive proliferative capacity and also the: Ability to give rise to new stem cells(Self Renewal) Ability to differentiate into any blood cells lines(Pluripotency) They grow and develop in the bone marrow. The bone marrow & spleen form a supporting system, called the “hemopoietic microenvironment”
STEM CELLS: Types Pluripotent Stem cells: Has a diameter of 18 – 23 μ. Giving rise to: both Myeloid and Lymphoid series of cells Capable of extensive self-renewal. Myeloid Stem cells: Generate myeloid cells: Erythrocytes Granulocytes: PMNs, Eosinophils & Basophils. Thrombocytes. Lymphoid Stem cells: Giving rise only to: Lymphocytes: T type mainly.
Symmetric cell division Asymmetric cell division Self renewal of stem cells Stem cells divide asymmetrically Non-stem cells divide symmetrically
1 2 3 Rules of Normal Cell Proliferation Stem cellsself renew--immortal non-stem cells have finite life span
But also when it is required : Stem cells divide symmetrically to restore stem cell quantity Stem cells symmetric cell division
CLONAL HEMOPOIESIS MULTIPLICATION COMMITTMENT COMMITTED STEM CELL STEM CELL MULTIPLICATION COMMITTED STEM CELL CFU: COLONY FORMING UNIT
CLONAL HEMOPOIESIS: (Contd) COLONY FORMING UNIT (CFU) INTERMEDIATE BLAST CELLS MORPHOLOGICALLY RECOGNIZABLE MATURE BLOOD CELLS END CELLS: FINITE LIFE SPAN
Properties of stem cells Self renewal Hierarchy Extensive proliferative capacity Cell cycle status Surface Markers Interact with microenvironment
Stem Cell Progression Is Associated By Changes In: - Specific cell markers- Receptors - Adhesion molecules - Chromatin openness- Access to epigenetic transcription factors and loss of proliferative potential.
SITES OF HEMOPOIESIS • Yolk sac • Liver and spleen • Bone marrow • Gradual replacement of active (red) marrow by inactive (fatty) tissue • Expansion can occur during increased need for cell production
SITES OF HEMOPOIESIS Active Hemopoietic marrow is found, in children throughout the: Axial skeleton: Cranium Ribs. Sternum Vertebrae Pelvis • Appendicular skeleton: • Bones of the Upper & Lower limbs • In Adults active hemopoietic marrow is found only in: • The axial skeleton • The proximal ends of the appendicular skeleton.
Sites of Hemopoiesis Hemopoiesis starts as early as yolk sac development. 2-3 weeks after fertilization 3 layers are developed (ecto, meso, and endoderm) Hemoangioblast which is derived from the mesoderm
In the embryo • 2 week old embryo, hematopoiesis begins in yolk sac. • THE 1ST CELL TO BE PRODUCED IS erythrocytes • By 2 month old fetus, granulocyte and megakaryocyte production. • 4th month,lymphocytes production. • 5th month, monocytes produced.
CONTINUED….. • In the 3rd to 7th month of fetal life Hemopoietic stem cells will migrate to the liver and spleen, where hemopoiesis starts there and hemopoiesis is still mainly erythropoietic in nature, with minimal granulopoiesis
The bone marrow (BM) • The stem cells then migrate to the bone marrow (BM) where hemopoiesis starts and continue all over the life. In the bone marrow all types of blood cells are formed which include: • RBCS • Granulocytes: Neutrophils, Eosinophils, Basophils • Lymphocytes • Monocytes and macrophages • Platelets
Extramedullary Hemopoiesis • When required, yellow marrow can be replaced by red marrow. • Liver & spleen can aslo resumed. • This will multiply the production by 6. • Remark that Hemopoiesis within the marrow is called intramedullary or medullary hemopoiesis
Why hemopoietic cells reside in the bone marrow The stromal matrix plays an important role in presenting growth factors and nutrients to developing blood cells. The most immature cells have receptors which bind them to proteoglycan molecules on the matrix and to receptors on the stromal cells (i.e. macrophages, fibroblasts, fat cells and endothelial cells) There are lineage specific regions ( "niches" ) which provide the molecular basis for homing of transplanted stem cells. The unique supportive microenvironment stem cell niche - regulates proliferation and differentiation - supports survival and inhibits apoptosisSimilar principles apply to malignant stem cells in myeloid leukemias The sinusoids are lined with specialized endothelial cells which play an important role by producing factors which regulate growth anddifferentiation.
Interaction of stromal cells, growth factors and haemopoietic cells
Stromal Cells of BM • Endothelial cells • Fat cells • Fibroblasts • Lymphocytes • Macrophage
Haemopoietic growth factors The haemopoeitic growth factors are glycoprotein hormones that regulate the proliferation and differentiation of haemopoietic progenitor cells and the function of mature blood cells. T lymphocytes, monocytes, marcrophages and stromal cells are the major sources of growth factors except for erythropoietin, 90% of which is synthesized in the kidney and thrombopoietin, made largely in liver.
Haemopoietic growth factors Overview Regulate growth and differentiation -a family of glycoproteins with clinical utility-with different specificities-with different origins-bind to cognate receptors on progenitor cells-act locally or at a distance-regulate proliferation and differentiation-prevent apoptosis-enhance function of some end stage cells eg. GM-CSF enhances PMN function...., Adhesion molecules /integrins
Haemopoietic growth factors GM-CSF Granulocyte-Macrophage colony stimulating factor M-CSF Macrophage colony stimulating factor Erythropoietin Erythropoiesis stimulating hormone (These factors have the capacity to stimulate the proliferation of their target progenitor cells when used as a sole source of stimulation) Thrombopoietin Stimulates megakaryopoiesis
Haemopoietic growth factors Cytokines IL 1 (Interleukin 1) IL 3 IL 4 IL 5 IL 6 IL 9 IL 11 TGF-β SCF (Stem cell factor, also known as kit-ligand) Cytokines have no (e.g IL-1) or little (SCF) capacity to stimulate cell proliferation on their own, but are able to synergise with other cytokines to recruit nine cells into proliferation
Order of blood cell formation 1:STEM CELLS 2: Progenitor cells may be mutli-potential, bi-potential or uni-potential 3: Precursor cells, or also called maturing cells 4: Terminally differentiated cells Mature cells
Precursor cells Precursor cells Precursor cells Precursor cells
Stem Cells • Stem Cells: undifferentiated cells that give rise to all of the bone marrow cells. • Only 0.5% of all marrow nucleated cells. • Multipotential precursors. • High self-renewal – give rise to daughter stem cells that are exact replicas of the parent cell. • Not morphologically distinguishable At any time, the majority of stem cells (95%) are out of the cell cycle (they are in G0 mode/phase, also called quiescent). • The current phenotype is: CD34+CD38-Lin-HLA-DR-Rh123Dull
Progenitor cells of the BM • Stem cells which undergo differentiation. • Limited self-renewal ability. • Multipotential but Gradually they become unilineage or committed progenitor cell. • ~3% of total nucleated hematopoietic cells of bone marrow
Progenitor cells of the BM • Form colonies of cells in semisolid media in vitro – described as colony forming units (CFU). • CFU-GEMM (granulocytic, erythrocytic, monocytic,megakaryocytic,CFU-GM,CFU-Mk, etc. ) • Survival and differentiation of progenitor cells influenced by growth regulatory glycoproteins, called cytokines – include interleukins, colony stimulating factors
Morphology of stem cells and progenitor cells • Stem cells & progenitor cells are not recognized morphologically but all look like small mononuclear lymphocytes
Maturing blood cells 1- Majority of cells (>95%) 2- lose adherence receptors, become deformable. 3- migrate through cytoplasm of lining endothelial cell to enter sinusoids. 4. Platelets are the exception. Megakaryocytes form part of the sinusoidal wall. They form long processes of proplatelets which fragment into nascent platelets.