RESPIRATORY DISORDERS
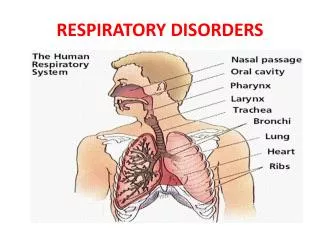
RESPIRATORY DISORDERS. The respiratory system. Nose H+M Larynx M+H Lungs H+D The upper respiratory tract includes: the nose & nasal cavities, the paranasal sinuses, the pharynx and the larynx The lower respiratory tract includes: the trachea and the lungs (bronchi, bronchioles and alveoli).

RESPIRATORY DISORDERS
E N D
Presentation Transcript
The respiratory system • Nose H+M • Larynx M+H • Lungs H+D • The upper respiratory tract includes: the nose & nasal cavities, the paranasal sinuses, the pharynx and the larynx • The lower respiratory tract includes: the trachea and the lungs (bronchi, bronchioles and alveoli)
THE RESPIRATORY SYSTEM • The temperament of the respiratory system ensures that: • The air breathed in from the external environment is cleared of harmful or irritant material-dust particles, pollen, fungal spores and bacteria. • The temperature of the incoming air is close to that of the respiratory tract, so preventing shock. • The humidity of the incoming air is adjusted in order to prevent dehydration of the body.
Humans possess a number of paranasal sinuses, divided into subgroups that are named according to the bones within which the sinuses lie: the maxillary sinuses, also called the maxillary antra and the largest of the paranasal sinuses, are under the eyes, in the maxillary bones. the frontal sinuses, superior to the eyes, in the frontal bone, which forms the hard part of the forehead. the ethmoid sinuses, which are formed from several discrete air cells within the ethmoid bone between the nose and the eyes. the sphenoid sinuses, in the sphenoid bone at the centre of the skull base under the pituitary gland.
THE PARANASAL SINUSES • a sinus is an air filled cavity in the bone. The paranasal sinuses are the four pairs of sinuses within the bones of the face and skull. They are situated near the nasal cavities or the ears.
Paranasal sinuses • They have four main functions: • To lighten the bones of the skull • To secrete mucus into the nasal passages • To act as speech resonators, giving a warm rich tone • To act as thermal insulators, so preventing cold inhaled air cooling surrounding structures.
Paranasal sinuses • also lined with a mucous membrane which contains goblet cells • Inflammation of the sinuses causes the mucous membrane to swell, so blocking the ostia (narrow passage or duct that connects the each sinus to the nasal cavities). This in turn prevents fluid from draining into the nasal cavity. This leads to blocked sinuses, a common disorder of the upper respiratory tract
THE NOSE (H+M) • Organ of smell • Acts to warm, moisten and filter incoming air before it enters the lung • internal nose made up of nostrils & nasal cavities. • The nasal cavities are separated from one another by the nasal septum, a vertical plate.
The nose • The nasal septum and the inside walls of the nasal cavities are covered with a very delicate mucous membrane. • This receives blood supply from a capillary network of blood vessels. This is prone to physical damage such as nose bleeds. • the nasal lining also contains a large number of goblet cells which secrete an excess of viscous fluid when inflamed or infected. (e.g. cold or flu)
THE TONSILS • Plays a relatively minor role in the immune system’s defence of the body against infection caused by bacteria, viruses and fungi. • Two pairs of lymphoid organs are found in the oropharynx: • Palatine tonsils- situated behind and below the fauces; these are the ones which are sometimes removed surgically. • Lingual tonsils- found at the base of the tongue. • Another pair of lymphoid organs are found in the nasopharynx: c) Nasopharyngeal tonsils- more familiar referred to as adenoids.
THE PHARYNX • the pharynx or throat is a muscular tube, extending from the base of the skull to the top of the oesophagus. • it serves as a passageway for both the respiratory & digestive tracts. • The pharynx carries air to & from the lungs via the trachea, & food and drink via the oesophagus and into the stomach. It is lined with a mucous membrane.
The pharynx • divided into three distinct sections: • The nasopharynx (upper section)- this lies just behind the opening of the throat. The nasopharynx has two openings linking the ears (the eustachian tubes) • The middle section; opposite the mouth is the oropharynx. This single opening linking with mouth is called the fauces. • The lower section is the laryngo-pharynx & this opens both the larynx and the oesophagus.
The larynx • The larynx , commonly called the "voice box," is a tube shaped structure comprised of a complex system of muscle, cartilage, and connective tissue.
THE LARYNX The larynx is suspended from the hyoid bone, which is significant in that it is the only bone in the body that does not articulate with any other bone. The framework of the larynx is composed of three unpaired and three paired cartilages. The thyroid cartilage is the largest of the unpaired cartilages, and resembles a shield in shape. The most anterior portion of this cartilage is very prominent in some men, and is commonly referred to as an "Adam's apple." The second unpaired cartilage is the cricoid cartilage, whose shape is often described as a "signet ring." The third unpaired cartilage is the epiglottis, which is shaped like a leaf. The attachment of the epiglottis allows it to invert, an action which helps to direct food and liquid into the oesophagus and to protect the vocal cords and airway during swallowing.Voice production is a complex action, and involves practically all systems of the body. Voice production begins with respiration (breathing). Air is inhaled as the diaphragm (the large, horizontal muscle below the lungs) lowers. The volume of the lungs expands and air rushes in to fill this space. We exhale as the muscles of the rib cage lower and the diaphragm raises, essentially squeezing the air out.
THE TRACHEA The trachea, or windpipe, is the bony tube that connects the nose and mouth to the lungs, and is an important part of the vertebrate respiratory system. When an individual breathes in, air flows into the lungs for respiration through the windpipe. Because of its primary function, any damage incurred to the trachea is potentially life-threatening.
The trachea • The trachea is made up of strong fibrous elastic (hyaline ) tissue, in which are embedded several C-shaped cartilage rings, making it semi-rigid so keeping it open and resistant to collapse. • The trachea divides into two branches at the level of the sternum: • the left bronchus and the right bronchus. This division takes place at a point called the carina.
BRONCHI AND BRONCHIOLES • The bronchi are the airways after the trachea which carry air to and from the lungs • the two bronchi have a structure similar to the trachea, but with the cartilage dispersed throughout the tubes, rather than in the form of rings. • The bronchi are very flexible and elastic & lined with mucous glands. • There also a large number of smooth muscle fibres present which allow changes to occur in the diameter of the bronchi.
Bronchi and bronchioles • the right bronchus is alot wider than the left one & more vertical. • The bronchi are lined with a special type of epithelium cells. • the bronchi divide repeatedly (as much as 20 times) forming smaller and smaller airways. • As they become smaller, the amount of cartilage decreases. • each bronchus divides into three small airways, called secondary or lobar bronchi. • Each of these goes to a specific lobe of the lung. • This repeated subdivision of the airways is called the bronchial or respiratory tree.
Bronchi and bronchioles • when the airways reach a diameter of around 1millimeter, they are known as bronchioles. • further division of the bronchial tree leads to the terminal bronchioles. • These in turn subdivide into a large number of the smallest and finest air passages, the respiratory bronchioles. These develop into the alveolar ducts
THE LUNGS (H+D) • The primary bronchi and the pulmonary blood vessels enter the lungs through an opening in the surface of the lung called the hilum. • The two lungs are the principle organs of respiration. • They are cone-shaped organs, occupying most of the thoracic cavity. • The lung tissue is soft and spongy, and has a great elasticity. • In children the lungs are pink in colour but with age they become darker and mottled as they are exposed to dust and chemicals in the environment.
The lungs • Each lung has: • An apex-which projects up into the base of the neck behind the clavicle • A base- with a concave surface, which rests on the diaphragm, the main respiratory muscle • A mediastinal surface- which rests against the various structures situated in the mediastinum. This is the central cavity between the two lungs. It holds the heart, the pulmonary blood vessels, various nerves and several lymph glands. • The lungs are enclosed in a continuous double membranous sac called the pleural sac.
CHRONIC COUGH • A cough that lasts for longer than 4-8 weeks is prolonged • TB OR NOT TB? • Consider a chest x-ray • The following differential diagnosis will be considered: Less than 3 weeks • Viral cold • Hay fever • Sinusitis More than 4 weeks and normal chest x-ray (non-smoker) • Post nasal drip • Asthma • COPD • ACE-inhibitors
CHRONIC COUGH Dyspnoea/ dry cough with abnormal chest x-ray • Left ventricular failure • HIV • Asthma • Alveolitis • Pleural disease • Pleural effusion Wet cough with foul smelling sputum • Bronchiectasis • Lung abscess • Chronic bronchitis
COUGHS (pertussis) • A dry cough is associated with a H+D frame, Pathway 1 • A wet cough is associated with a M+H frame, Pathway 2 • A cough is a self-protection mechanism which exists to clear the unwanted secretions and toxins from the lungs. • A cough may be the symptom of many disorders linked with the respiratory system i.e. Asthma, hay fever, cold, flu, pneumonia, pleurisy, TB, bronchitis, laryngitis, tonsillitis and occasionally organ related disorders such as the heart or liver. • Generally there are two main types of coughs- dry (non-productive) cough and wet (productive) cough. Discuss treatment in terms of the Tibb philosophy
PNEUMONIA • Infection of the lung tissue including the alveolar spaces and interstitial tissue. • Pneumonia: Inflammation of one or both lungs with consolidation. Pneumonia is frequently but not always due to infection. The infection may be bacterial, viral, fungal or parasitic. Symptoms may include fever, chills, cough with sputum production, chest pain, and shortness of breath. • Classification includes: • Community acquired • Nosocomial • Aspiration • Immunocompromised
PNEUMONIA Signs of pneumonia • Tachypnoea • Fever (however, fever may not be present in 30% of patients) • Herpes labialis (pneumococcus) • Consolidation (dull to percussion, increased viral load, bronchial breathing) • Nasal flaring Tests and treatment • Chest X-ray if indicated • Fluids, rest, antibiotics and hospitalization. Bronchopneumonia-this is a multifocal process involves the terminal bronchioles, which spreads segmentally causing patchy consolidation.
LOBAR PNEUMONIA CLINICAL FEATURES • Fever, rigors, pleuritic pain and cough with rust-coloured sputum • Tachypnoea, intercostal recession, flaring • Initially decreased air entry and creps on affected side may be present
LOBAR PNEUMONIA Later the classical signs of consolidation appear • Bronchial breathing • Increased vocal resonance • Dullness on percussion • A pleural friction rub may occasionally be heard • During resolution, the signs of consolidation are replaced by creps • However, in elderly patients or patients with lowered resistance such as diabetes or AIDS, the clinical picture will be less obvious. Suspect Pneumonia in any adult with a cough, raised respiratory rate, Pleuritic chest pain and who is ill, even though no chest signs are found on examination.
BRONCHOPNEUMONIA CLINICAL FEATURES The patient will be ill with: • Tachypnoea • Intercostal recession • Grunting • Tachycardia • Later scattered crepitations and wheezes appear, affecting one or more lobes • In adults diagnosis is suggested by early production of infected sputum, coarse crepitations and rhonchi • The presence of a cough in a neonate, even in the absence of other physical signs, is sufficient evidence to diagnose bronchopneumonia.
Bronchopneumonia In small infants, less than 2 months old, clinical features may be minimal. Bronchopneumonia should be suspected if there are any of the following: • A productive cough on history or examination • Any evidence of dyspnoea or grunting • Respiratory rate above 60/min • recession
BRONCHOPNEUMONIA Other causes of a raised respiratory rate in children High temperature • Check this by reducing the temperature • If the respiratory rate now drops, it was only due to pyrexia Acidosis (An abnormally high level of acid in the blood because the lungs are not working well) • This occurs particularly if the child has been given aspirin • This may have been given as aspirin or aspirin in another tablet e.g. Compral, Grandpa • Ask the escort about this • REFER Crying or exercise • This will also raise the respiratory rate • Recheck the respiratory rate when the child is quiet.
BRONCHOPNEUMONIA In infants 2-12 months • Chest signs are uncommon • The diagnosis of bronchopneumonia is suggested if • The respiratory rate is above 50/min • There is evidence of dyspnoea or recession • Flaring nostrils In small children 1-5 years • The diagnosis is often made if only a few of the above features are present. The following features are important • ill child • Fever • Dyspnoea and flaring • Respiratory rate above 40/min
BRONCHITIS • Bronchitis is a C+D to D+H imbalance. Pathologically it is the inflammation of the bronchi, the respiratory tubes that lead to the lungs. • There are two types of bronchitis, acute or chronic. • Acute bronchitis is usually caused by a sudden exposure to Cold weather/environment, excessive intake of C+D food & drink, dairy products, wheat products especially refined flour products and a sudden change in temperature from hot to cold or cold to hot.
Bronchitis • Chronic bronchitis results from frequent irritation of the lungs, such as from exposure to cigarette smoke or other noxious fumes, unhealthy environments, cold and dust etc. • As chronic bronchitis diminishes the exchange of oxygen and carbon dioxide in the lungs, the heart works harder in an attempt to compensate. • Over time, this can lead to pulmonary hypertension, enlargement of the heart and ultimately heart failure. • Usually a viral infection that does not require antibiotic therapy. • Bronchitis and pneumonia are often impossible to distinguish clinically.
Bronchitis • Antibiotics should be considered if: • The patient’s general condition is impaired or worsening • Fever continues for more than 1 week • Fever starts again after already having settled • The patient is immunocompromised.
BRONCHITIS • Cough is the most commonly observed symptom of acute bronchitis • Most patients have a cough for less than two weeks; however, 26% are still coughing after two weeks, and a few cough for six to eight weeks. SYMPTOMS • Cough • Sputum may be clear, white, yellow, green or even tinged with blood • Retrosternal discomfort (burning sensation due to “rawness” of bronchioles • sensation of tightness • Dyspnoea & wheezing • Symptoms may vary & may not all be present SIGNS • Fever • Not usually very ill patient • Coarse crackles which clear with coughing • Chest may be clear Discuss treatment as group discussion from TIBB perspective