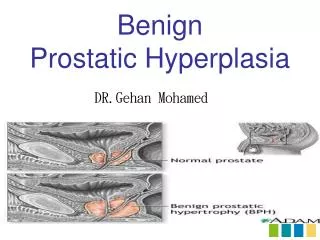
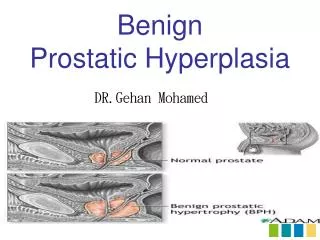
Benign Prostatic Hyperplasia (Nodular Hyperplasia)
Benign Prostatic Hyperplasia (Nodular Hyperplasia). - Is an extremely common abnormality of men by the age of 40, and its frequency rises progressively with age, reaching 90% by the eighth decade of life.

Benign Prostatic Hyperplasia (Nodular Hyperplasia)
E N D
Presentation Transcript
Benign Prostatic Hyperplasia (Nodular Hyperplasia) - Is an extremely common abnormality of men by the age of 40, and its frequency rises progressively with age, reaching 90% by the eighth decade of life. - Is characterized by proliferation of bothstromal and epithelial elements, with resultant enlargement of the gland and, in some cases, urinary obstruction.
- Direct cause of BPH remains incompletely understood, however, excessive androgen-dependent growth of stromal and glandular elements has a central role. - BPH does not occur in males castrated before the onset of puberty or in men with genetic diseases that block androgen activity.
- Dihydrotestosterone (DHT), the ultimate mediator of prostatic growth, is synthesized in the prostate from circulating testosterone by the action of the enzyme 5α-reductase, type 2. - DHT binds to nuclear androgen receptors, which regulate the expression of genes that support the growth and survival of prostatic epithelium and stromal cells.
- Although testosterone can also bind to androgen receptors and stimulate growth, DHT is 10 times more potent. - Clinical symptoms of lower urinary tract obstruction caused by prostatic enlargement may also be exacerbated by contraction of prostatic smooth muscle mediated by α1-adrenergic receptors.
MORPHOLOGY - BPH always occurs in the inner, transitional zone of the prostate. - The affected prostate is enlarged, typically weighing between 60 and 100 g, and contains many well-circumscribed nodules - The nodules may appear solid or contain cystic spaces,corresponding to dilated glandular elements
- The urethra is usually compressed by the hyperplastic nodules, often to a narrow slit. - In some cases, hyperplastic glandular and stromal elements lying just under the epithelium of the proximal prostatic urethra may project into the bladder lumen as a pedunculated mass, producing a ball-valve type of urethral obstruction.
Microscopically - The hyperplastic nodules are composed of variable proportions of proliferating glandular elements and fibromuscularstroma. - The hyperplastic glands are lined by tall, columnar epithelial cells and a peripheral layer of flattened basal cells - The glandular lumina often contain inspissated, proteinaceoussecretory material known as corpora amylacea.
Clinical Features - Occur in only about 10% of men with pathologic evidence of BPH. - Because BPH preferentially involves the inner portions of the prostate, the most common manifestations are related to lower urinary tract obstruction, often in the form of a.Difficulty in starting the stream of urine (hesitancy)
b. Intermittent interruption of the urinary stream while voiding. c. urinary urgency, frequency, and nocturia, all indicative of bladder irritation. Note: - The presence of residual urine in the bladder due to chronic obstruction increases the risk of urinary tract infections.
- In some affected men, BPH leads to complete urinary obstruction, with resultant painful distention of the bladder and, in the absence of appropriate treatment, hydronephrosis - Initial treatment is pharmacologic, using targeted therapeutic agents that inhibit DHT formation (Finestride) or that relax smooth muscle by blocking alpha adrenergic blockers (Flomax). - Various surgical techniques are reserved for severely symptomatic cases recalcitrant to medical therapy.
Carcinoma of the Prostate - Adenocarcinoma of the prostate occurs mainly in men older than 50 years of age. - It is the most common form of cancer in men, - Over the past several decades, there has been a significant drop in prostate cancer mortality. - This relatively favorable outcome is related in part to increased detection of the disease through screening but how effective screening is at saving lives is controversial.
- prostate carcinoma commonly is found incidentally at autopsy in men dying of other causes, and many more men die with prostate cancer than of prostate cancer. - It is not currently possible to identify the tumors that will be "bad actors" with certainty; thus, while some men are no doubt saved by early detection and treatment of their prostate cancers, it is equally certain that others are being "cured" of clinically inconsequential tumors
PATHOGENESIS 1. Androgens are of central importance. - Cancer of the prostate does not develop in males castrated before puberty, indicating that androgens somehow provide the cellular context, within which prostate cancer develops. - This dependence on androgens extends to established cancers, which often regress for a time in response to surgical or chemical castration
- Tumors resistant to anti-androgen therapy often acquire mutations that permit androgen receptors to activate the expression of their target genes even in the absence of the hormones. - Thus, tumors that recur in the face of anti-androgen therapies still depend on geneproducts regulated by androgen receptors for their growth and survival
2. Heredity – - There is an increased risk among first-degree relatives of patients with prostate cancer. - Incidence of prostatic cancer is uncommon in Asians and highest among blacks and is also high in Scandinavian countries. - A number of genetic variants that are associated with increased risk, including
1. a variant near the MYConcogene on chromosome 8q24 that appears to account for some of the increased incidence of prostate cancer in males of African descent. 2. in white American men, the development of prostate cancer has been linked to a susceptibility locus on chromosome 1q24-q25.
3. Environment - plays a role, as evidenced by the fact that in Japanese immigrants to the United States the incidence of the disease rises (although not to the level seen in native-born Americans). -Also, as the diet in Asia becomes more Westernized, the incidence of clinical prostate cancer in this region of the world appears to be increasing. However, the relationship between specific dietary components and prostate cancer risk is unclear.
4. Acquired somatic mutations, a. One class of somatic mutations is gene rearrangements that create fusion genes consisting of the androgen-regulated promoter of the TMPRSS2 gene and the coding sequence of ETS family transcription factors (the most common being ERG).
b. TMPRSS2-ETS fusion genes occur in approximately 40% to 50% of prostate cancers; it is possible that unregulated increased expression of ETS transcription factors interfere with prostatic epithelial cell differentiation. c. other mutations commonly lead to activation of the oncogenic PI3K/AKT signaling pathway; of these, the most common are mutations that inactivate the tumor suppressor gene PTEN, which acts as a brake on PI3K activity.
MORPHOLOGY - Most carcinomas detected clinically are not visible grossly. - More advanced lesions appear as firm, lesions with ill-defined margins that infiltrate the adjacent gland On histologic examination, - Most lesions are moderately differentiated adenocarcinomas that produce well-defined glands.
1. The glands typically are smaller than benign glands 2. Are lined by a single uniform layer of cuboidal or low columnar epithelium, lacking the basal cell layer seen in benign glands 3. In contrast with benign glands, malignant glands are crowded together and characteristically lack branching and papillary infolding. 4.The cytoplasm of the tumor cells ranges from pale-clear (as in benign glands) to a distinctive amphophilic (dark purple) appearance
5. Nuclei are enlarged and often contain one or more prominent nucleoli 6. Pleomorphism is not marked. 7. Mitotic figures are uncommon. 8.With increasing grade, irregular or ragged glandular structures, cribriform glands, sheets of cells, or infiltrating individual cells are present.
- In approximately 80% of cases, prostatic tissue removed for carcinoma also harbors presumptive precursor lesions, referred to as high-grade prostatic intraepithelial neoplasia (HGPIN).
Clinical Features - A minority of carcinomas are discovered unexpectedly during histologic examination of prostate tissue removed by transurethral resection for BPH. - Some 70% to 80% of prostate cancers arise in the outer (peripheral) glands and hence may be palpable as irregular hard nodules on digital rectal examination.
- However, most prostate cancers are small, nonpalpable, asymptomatic lesions discovered on needle biopsy performed to investigate an elevated serum prostate-specific antigen (PSA) level - Because of the peripheral location, prostate cancer is less likely than BPH to cause urethral obstruction in its initial stages. - Locally advanced cancers often infiltrate the seminal vesicles and periurethral zones of the prostate
and may invade the adjacent soft tissues, the wall of the urinary bladder, or (less commonly) the rectum. - Bone metastases, particularly to the axial skeleton, are frequent late in the disease and typically cause osteoblastic (bone-producing) lesions that can be detected on radionuclide bone scans. - The poor sensitivity and specificity of prostate imaging studies limit their diagnostic utility for the detection of early prostate cancer
- The PSA assay is the most important test used in the diagnosis and management of prostate cancer but suffers from a number of limitations. - PSA is a product of prostatic epithelium and is normally secreted in the semen, it is a serineprotease whose function is to cleave and liquefy the seminal coagulum formed after ejaculation
- In most laboratories, a serum PSA level of 4 ng/mL is the cutoff between normal and abnormal, although some guidelines designate values above 2.5 ng/mL as abnormal. - Although PSA screening can detect prostate cancers early in their course, many prostate cancers are slow-growing and clinicallyinsignificant, requiring no treatment
- One limitation of PSA is that while it is organ-specific, it is not cancer-specific. - BPH, prostatitis, prostatic infarcts, instrumentation of the prostate, and ejaculation also increase serum PSA levels. - Conversely, 20 to 40% of patients with organ-confined prostate cancer have a PSA value of 4.0 ng/mL or less.
- The percentage of free PSA (the ratio of free PSA to total PSA) is lower in men with prostate cancer than in men with benign prostatic diseases. - Once cancer is diagnosed, serial measurements of PSA are of great value in assessing the response to therapy. - For example, a rising PSA level after radical prostatectomy or radiotherapy for localized disease is indicative of recurrent or disseminated disease.
- The most common treatments for clinically localized prostate cancer are radical prostatectomy and radiotherapy. - The prognosis after radical prostatectomy is based on the pathologic stage, margin status, and Gleason grade. - The Gleason grade, clinical stage, and serum PSA values are important predictors of outcome after radiotherapy.
- Because many prostate cancers follow an indolent course, active surveillance ("watchful waiting") is an appropriate approach for older men, patients with significant comorbidity, or even some younger men with low serum PSA values and small, low-grade cancers. - Advanced metastatic carcinoma is treated by androgen deprivation, effected either by orchiectomy or by administration ofsynthetic agonists of luteinizing hormone-releasing hormone. .
(LHRH), which in effect achieve a pharmacologic orchiectomy - Although antiandrogen therapy induces remissions, androgen-independent clones eventually emerge, leading to rapid disease progression and death.