Wound care
Wound care. Susie Pease Return to Practice (Nursing) School of Healthcare Studies The University of Leeds. Assessment. Assess individual wound environment Plan Implement Evaluate - Re-assess. Wound cleansing. Normasol Saline 0.9% - (Normal Saline) Room temperature

Wound care
E N D
Presentation Transcript
Wound care Susie Pease Return to Practice (Nursing) School of Healthcare Studies The University of Leeds
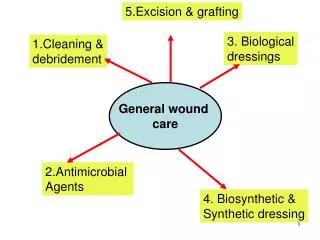
Assessment • Assess • individual • wound • environment • Plan • Implement • Evaluate - Re-assess
Wound cleansing • Normasol • Saline 0.9% - (Normal Saline) • Room temperature • Irrigate wound gently using syringe • Antiseptics rarely used • Tap water, bath, shower may be appropriate • DO NOT CLEAN WOUND UNLESS NECESSARY
Aseptic Technique • Cross infection must be prevented • The principles of asepsis should be followed • Ritualistic techniques are not necessary • Handwashing is vital
Characteristics of the ideal wound dressing (Bale and Morrison 1997) • Non - adherent • Impermeable to bacteria • Maintain high humidity • Thermally insulating • Non - toxic, non - allergenic • Comfortable and conformable • Protect from further trauma • Require infrequent changes
Low adherent dressing • Release • Low adherent rather than non- adherent • Provides some protection • Allows gaseous exchange • Free from particulate contamination • Does not provides a moist environment
Adhesive Island Dressings • Primapore / Cicaplaie • Non woven • Use on clean incisions or as secondary dressings • Little absorbent capacity • Do not use on granulating wounds • Do not stretch – can cause blistering
Hydrofibre Dressings • Aquacell • Soft non – woven fibre sheet or ribbon dressing • Can be used for acute and chronic wounds • Can absorb high amounts of exudate into fibres • When exudate is absorbed converts from soft conformable dressing to cohesive gel • Appears to reduce wound pain • Change when saturated or after 7 days
Vapour Permeable Film Dressings • Mefilm / Tegaderm • Provide a moist environment • Allows excess moisture to escape through the film • Impermeable to micro – organisms • Can be used as a primary or secondary dressing • Can be left in place for several days • Remove by releasing edge and stretching to release adhesive. • Opsite IV 3000 or Tegaderm HP – highly permeable to prevent moisture retention
Alginate Dressings • Kaltostat • Made from seaweed • Used as haemostatic dressing • On contact with exudate form a gel • Can be used for flat wounds or those which require packing • Irrigate with saline 0.9% if nec.before removal • Do not use where exudate is low
Charcoal / Odour Control Dressings • Carboflex / Clinisorb • Contains activated charcoal • Do not cut dressing – choose size larger than wound • Wound contact layer absorbs exudate • Non adhesive • Acts like a filter absorbing odour
Debridement • Surgical • Enzymatic – varidase • Chemical – hydrogen peroxide / EUSOL • Larva
Hydrogel Dressings • Aquaform • Suitable for sloughy/ necrotic wounds • Aids rehydration of necrotic tissue which helps debridement • Secondary dressing required
Foam Dressings • Allevyn / Trufoam / Transorbent • Provide a warm moist environment • Absorbent, use on moderate to heavily exuding wounds • Can be left in situ for 7 days depending on exudate
Hydrocolloid Dressings • Hydrocoll / Granuflex • Occlusive dressing • Provide ideal moist environment • Exudate absorbed & forms a gel • Used for treating necrotic, sloughy and granulating wounds • Can be left in situ for 7 days • “a week or til’ it leaks”
Impregnated dressings • Inadine (beware iodine sensitivity) • Contains 10% povidone iodine which is released directly into the wound • Use on contaminated or infected wounds • Can be left for 5 days • Jelonet (non-medicated paraffin tulle) • Granulating wounds – trauma on removal
Cavity Conforming • Cavi-Care (Silastic Foam) • Aquacell packing • Keep wound edges apart to allow healing by secondary intention • Foam dressings can be managed by patients • Aquacell ribbon requires nurse to change dressings
Polysaccharide Dressings • Debrisan / Iodosorb • Beads which absorb exudate • Form a gel • Provide a moist environment • Use in sloughy infected wounds • Remove gel with gentle irrigation • Require secondary dressing
Antimicrobials • Silver Sulphasalazine Cream (Flamazine) • Povidone Iodine Ointment • Aquacel Ag (silver impregnated Hydrofibre dressing) • Metronidazole Gel
Specialist bandages • Compression bandaging for the management of patients with venous leg ulcers • Paste bandages • Zinc paste with ichthammol • Zinc paste with calamine
New developments • Silicone dressings • Mepitel and Mepilex • Combination dressings • Versiva hydrocolloid, hydrofibre and foam filled • Growth factors – wound healing growth factors produced by many cells including platelets and macrophages
Prevention of Infection • Leave wound undisturbed unless signs of infection • Avoid ritualistic daily dressings • Observe principles of asepsis • Avoid communal use of equipment -scissors,tapes • Barrier Nursing if necessary • Antiseptics not used routinely • HANDWASHING
Summary • Modern wound dressings are designed to promote normal wound healing and allow: • Moist wound / dressing interface • Less frequent dressing changes • More comfort and less toxicity • Assessment of the needs of the individual patient is essential • Assessment, planning and evaluation should be documented and available
References and Bibliography • Bale S, Harding K & Leaper D (2000) An introduction to wounds. Emap Healthcare • Bale S & Jones V (1997) Wound Care Nursing A patient-centred approach. Bailliere Tindall • Bale S & Morrison M (1997) Wound Dressings. In: Morrison M, Moffat C, Bridel-Nixon J et al. A Colour guide to the Nursing Management of Chronic Wounds. Mosby, London.
References & Bibliography cont. • Dealey C (1999) The Care of Wounds. A Guide for Nurses. (2nd Edition) Blackwell Science. • Naylor W, Laverty D & Mallett J (2001) Handbook of wound Management in Cancer Care. Blackwell Science. • Winter G.D. (1962) Formation of the scab and the rate of epithelialisation of superficial wounds in the skin of the domestic pig. Nature, 193, 293 - 294