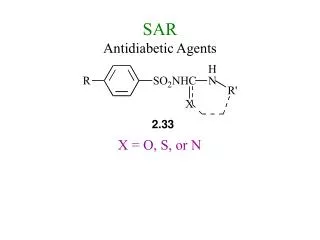
Antidiabetic Agents
Antidiabetic Agents. Dr. Florencia D. Munsayac. Cell Types. Approximate Percent of Islet Mass. Secretory Products. A cells (Alpha) . 20 . Glucagon Proglucagon. B cells (Beta). 75 . D cells (Delta). 3-5. Somatostatin. F cells (PP cells). <2. Pancreatic polypeptide.

Antidiabetic Agents
E N D
Presentation Transcript
Antidiabetic Agents Dr. Florencia D. Munsayac
Cell Types Approximate Percent of Islet Mass Secretory Products A cells (Alpha) 20 Glucagon Proglucagon B cells (Beta) 75 D cells (Delta) 3-5 Somatostatin F cells (PP cells) <2 Pancreatic polypeptide Insulin, C-peptide, proinsulin, islet amyloid polypeptide (IAPP) or amylin The Endocrine Pancreas 1 million islets of Langerhans
Different Forms of Diabetes Mellitus General – genetic and other factors not precisely defined Type 1 (Insulin-Dependent Diabetes Mellitus) Autoimmune type 1 DM type 1A) Non-autoimmune or idiopathic type 1 DM (type 1B) Type 2 (Non-insulin Dependent Diabetes Mellitus) Specific – defined gene mutations Maturity-onset diabetes of youth (MODY) MODY 1 hepatic nuclear factor 4α (HNF4A) gene mutations MODY 2 glucokinase (GCK) gene mutations MODY 3 hepatic nuclear factor 1α (TCF1) gene mutations MODY 4 insulin promoter factor 1 (IPF1) gene mutations MODY 5 hepatic nuclear factor 1β (HNF1β) gene mutations MODY 6 neurogenic differentiation 1 (NEUROD1) gene mutation MODY X unidentified gene mutation(s) Maternally inherited diabetes and deafness (MIDD) Mitochomdrial leucine tRNA gene mutations Insulin gene mutations Insulin receptor gene mutations Diabetes secondary to pancreatic disease Chronic pnacreatitis Surgery Tropical diabetes (chronic pancreatitis asst’d with nutritional and/or toxic factors) Diabetes secondary to other endocrinopathies Cushing’s disease Glucocorticoids administration Acromegaly Diabetes secondary to immune suppression Diabetes associated with genetic syndrome (Prader-Willi syndrome) Diabetes associated with drug therapy
Some Drugs That Cause Hypoglycemia or Hyperglycemia Drugs with Hypoglycemic Effects: Drugs with Hyperglycemic Effects: Beta-adrenergic receptor antagonists Epinephrine Salicylates Glucocorticoids Indomethacin Diuretics Naproxen Atypical antipsychotic Ethanol HIV-1 protease inhibitors Clofibrate Diazoxide ACE inhibitors Beta2 adrenergic agonists Li+ Ca++ channel blockers Theophyllin Phenytoin Ca++ Clonidine Bromocriptine H2-receptor blockers Mebendazole Pentamidine Sulfonamides Morphine Sulbactam-ampicillin Heparin Tetracycline Nalidixic acid Pyridoxine Sulfinpyrazone Pentamidine Marijuana Nicotine
Chemistry: * a small protein with molecular weight of 5808 * contains 51 amino acids * arranged in 2 chains ( A & B ) linked by disulfide bonds/bridges * stored crystals consisting of 2 atoms of zinc & 6 molecules of insulin * contain 8mg of insulin/human pancreas (=200 units)
Insulin secretion: -- respond to a variety of stimuli ( glucose, mannose, leucine, arginine & vagal activity)
Insulin Degradation: - 2 main organs: liver – 60% kidney – 35-40% - hydrolysis of the disulfide bonds glutathione insulin transhydrogenase (insulinase ) - half-life: 3-5 minutes Measurement of Circulating Insulin: - radioimmunoassay permits detecton of insulin in picomolar quantities - basal insulin values: 5-15uU/ml (30-90pmol/L) - peak rise: 60-90uU/ml (360-540pmol/L)
Transporters Tissues GlucoseKm (Mmo/L) Function GLUT 1 All tissues, esp.red cells, brain 1-2 Basal uptake of glucose; Transport across the BBB GLUT 2 B cells of pancreas; Liver; kidney; gut 15-20 Regulation of insulin release, other aspects of glucose homeostasis GLUT 3 Brain, kidney, placenta, other tissues < 1 Uptake into neurons, other tissues GLUT 4 Muscle, adipose 5 Insulin-mediated uptake of glucose GLUT 5 Gut, kidney 1-2 Absorption of fructose Effects of Insulin on its Targets A. Action of Insulin on Glucose Transporters:
B.Action of Insulin on Liver -inhibits hepatic glucose production (decreases gluconeogenesis & glycogenolysis) -stimulates hepatic glucose uptake C.Effect of Insulin on Muscle -stimulates glucose uptake -inhibits flow of gluconeogenic precursors to the liver (alanine, lactate & pyruvate) D.Effect of insulin on Adipose Tissue -stimulate glucose uptake (amount is small compared to muscle) - inhibits flow of gluconeogenic precursor to liver (glycerol) and reduces energy substrate for hepatic gluconeogenesis (non-esterified fatty acids)
A.Principal Types and Duration of Action 1.Short- and Rapid-acting insulins: =Regular insulin ( soluble crystalline zinc ) =Insulin lispro, Insulin aspart, insulin glulysine = Permit more physiologic prandial insulin replacement = Taken immediately before meal without sacrificing glucose control = With very fast onset (5-15 min, 10-20 min. & 30 minutes after SQ) and short duration (3-5 hours & 5-8 hours) = Peak serum values: 1 hour & 2 & 3 hours = The only type that should be administered intravenously = Useful in the management of diabetic ketoacidosis, surgery or during acute infection, and when the insulin requirement is changing rapidly
1.Intermediate-acting • a.LENTE INSULIN (insulin zinc suspension) • mixture of 30% semilente with 70% ultralente insulin provide a combination of relatively rapid absorption with sustained long action • b.NEUTRAL PROTAMINE HAGEDORN or Isophane Insulin • absorption & onset of action is delayed by combining appropriate amounts of insulin & protamine • 6 molecules of insulin per molecule of protamine • 3. Long-acting insulins • a.ULTRALENTE INSULIN (extended insulin zinc suspension) • b.PROTAMINE ZINC INSULIN SUSPENSION • they have slower onset and a prolonged peak of action • recommended dose be split into 2 or more doses • c. INSULIN GLARGINE • soluble, “peakless, ultra-long-acting insulin analog • designed to provide reproducible, convenient, background insulin replacement • has a slow onset of action (1-1.5 hours) • achieves a maximum effect after 4-5 hours and maintained for 11-24 hours or longer • given once a day
A Species of Insulin 1.Beef and pork insulins ØThe beef insulin differs by 3 amino acids, pork differs by 1 amino acid ØThe beef hormone is most antigenic 2. Human insulins Ø Less expensive, less immunogenic Ø Production by recombinant DNA techniques B.Purity of Insulin Ø Chromatography C.Concentration 100 units/ml, 500 units/ml
Insulin Delivery Systems A. Portable Pen Injectors Øto facilitate multiple SQ injections B.Continuous Subcutaneous Insulin Infusion Devices (CSII, Insulin Pumps) Øencouraged for individuals who are unable to obtain target control while on multiple injection regimens & where excellent glycemic control is desired, such as during pregnancy Øvelosulin (reg. insulin) & insulin aspart and lispro C.Inhaled Insulin Øhave a rapid route and a relatively short duration of action Øused to cover mealtime insulin requirements Øto correct high glucose levels
Factors that Affect Insulin Absorption: - site of injection: abdomen, buttock, anterior thigh, or dorsal arm - type of insulin - subcutaneous blood flow: massage, hot baths, or exercise - smoking - regional muscular activity at the site of the injection - volume & concentration of injected insulin - depth of injection Treatment With Insulin ØType 1 patients ØType 2 ØContraindication: advanced renal disease Elderly
Complications of Insulin Therapy • A.Hypoglycemia • 1.Mechanisms and diagnosis • Øresult from a delay in taking a meal • Øunusual physical exertion • Ødosage error • ØCM: tachycardia, palpitations, sweating, tremulousness, hunger, nausea, convulsion, coma • ØTreatment: glucose administration • Glucagons 1 mg SQ or IM • Honey or syrup • B.Immunopathology of Insulin Therapy • 1.Insulin allergy • Øan immediate type of hypersensitivity (IgE-antibodies) • ØTx: antihistamines, corticosteroids & desensitization • 2.Immune insulin resistance (IgG antibodies) • Ø+ circulating antibodies that neutralize the action of insulin to a small extent • ØTx: switching to a lesser antigenic purified insulin • C.Lipodystrophy at injection sites • corrected by avoidance of that specific injection site or with liposuction – hypertrophy
Oral Anti-diabetic Agents • 4 Categories: • Insulin secretagogues (sulfonylureas, meglitinides, • D-phenylalanine derivatives) • b.Biguanides • c.Thiazolidinediones • d.Alpha-glucosidase inhibitors
Insulin Secretagogues: • A.Sulfonylureas • Mechanism of Action: • Øto increase insulin release from pancreatic B cells • Sulfonylureas bind to S receptorinhibits efflux of K+depolarizationopens a voltage-gated Ca++ channelresults in Ca++ influx and the release of preformed insulin • reduction of serum glucagon concentrations • Chronic adm’n of sulfonylureas to type 2 diabetics reduces serum glucagon levels • potentiation of insulin action on target tissues
First Generation Sulfonylureas Tolbutamide: Øwell absorbed but rapidly metabolized in the liver Øduration of action: 6-12 hours Øelimination half-life: 4-5 hours Øtoxic reactions: skin rash hypoglycemia Ødrug interactions: dicumarol, phenylbutazone, sulfonamides Chlorpropamide: Øduration of action: up to 60 hours Øhalf-life: 32 hours Øslowly metabolized in the liver Ø20-30% is excreted unchanged in the urine ØSE: hypoglycemia, hyperemic flush, dilutional hyponatremia, transient leukopenia, thrombocytopenia, jaundice ØCI: hepatic & renal insufficiency ØDosage: 250mg daily Tolazamide: Øduration of action: 10-14 hours Ømore slowly absorbed Øhalf-life: 7 hours ØSE: hypoglycemia
Second Generation Sulfonylureas Glyburide: Ømetabolized in the liver Øshort plasma half-life Øduration of action: 10-24 hours ØSE: flushing, hypoglycemia ØContraindication: hepatic & renal insufficiency ØDosage: 5-10mg as single morning dose Glipizide: Øhas the shortest half-life: 2-4 hours Øduration of action: 10-24 hours Ø90% is metabolized in the liver Ø10% excreted unchanged in the urine ØSE: hypoglycemia ØContraindication: renal & hepatic insufficiency ØDosage: 5-20mg as a single dose, 30 minutes before breakfast Glimepiride: Øduration of action: 12-24 hours Øhalf-life: 5 hours Øavailable as once-daily dosing Øcompletely metabolized by the liver Ødosage: 1 mg daily
B. Meglitinides Repaglinide: Ømodulate B cell insulin release by regulating K+ efflux through the K+ channels Øno direct effect on insulin exocytosis Øpeak conc & peak effect: within 1 hour Øfast onset & duration of action (5-8 hrs.) Øhepatically cleared by CYP3A4 Øhalf-life: 1 hour Øindication: controlling postprandial glucose excursions ØDosage: 0.25-4 mg ØSE; hypoglycemia ØCaution: hepatic & renal impairment C. D-phenylalanine derivative Nateglinide: Østimulates very rapid and transient release of insulin from B cells through the closure of ATP-sensitive K+ channel Ømay suppress glucagons release early in the meal and result in less endogenous or hepatic glucose production Øhas minimal effect on overnight or fasting blood glucose levels Øingested just prior to meals Øabsorbed within 20 minutes after oral administration Øtime to peak concentration: < 1 hour Øhepatically metabolized by CYP2C9 & CYP3A4 Øhalf-life: 1.5 hours Øduration of action: < 4 hours ØSE: hypoglycemia but lowest of all the secretagogues
Biguanides Mechanism of action: -direct stimulation of glycolysis in tissues, with increased glucose removal from blood -reduced hepatic & renal gluconeogenesis -slowing of glucose absorption from the GIT, with increased glucose to lactate conversion by enterocytes -reduction of plasma glucagon levels Metabolism & Excretion: Metformin: Øhalf-life: 1.5-3 hours Øduration of action: 10-12 hours Ønot bound to plasma proteins Ønot metabolized Øexcreted by the kidneys as active compound Ømay impair the hepatic metabolism of lactic acid Clinical Uses: -refractory obesity whose BS is due to ineffective insulin action (insulin resistance syndrome) -use as in combination with sulfonylureas or thiazolidinediones in type 2 diabetics in whom oral monotherapy is inadequate -dosage: 500mg TID Toxic Effects: Øanorexia, nausea, vomiting, abdominal discomfort, diarrhea Øabsorption of B12 appears to be reduced during long-term therapy Containdications: Ørenal disease, alcoholism Øhepatic disease Ø chronic cardiopulmonary dysfunction
Thiazolidinediones ØAct to reduce insulin resistance ØPrimary action: nuclear regulation of gene involved in glucose and lipid metabolism and adipocyte differentiation ØAre ligands of peroxisome proliferator-activated receptor-gamma (PPAR-gamma) ØHave significant effects on vascular endothelium, the immune system, the ovaries and tumor cells ØIn diabetes, a major site of action is adipose tissue, where the drug promotes glucose uptake and utilization and modulate synthesis of lipid hormones or cytokines and other proteins involved in energy regulation ØAlso regulate adipocyte apoptosis & differentiation ØAre considered “euglycemics” ØHave a slow onset and offset of activity ØSE: hypoglycemia in combination Drop in triglyceride levels Slight rise in HDL & LDL cholesterol values Edema – fluid retention Anemia Dose-related weight gain (1-3 kg) ØCI: pregnancy Significant liver disease Heart failure
Pioglitazone: Ømay have PPAR-alpha as well as PPAR-gamma activity Øabsorbed within 2 hours of ingestion Ømetabolized by CYP2C8 and CYP3A4 to active metabolites ØDI: estrogen-containing oral contraceptives ØTaken once daily ØDosage: 15-30mg ØApproved as monotherapy or in combination with metformin, sulfonylureas, and insulin Rosiglitazone: Ørapidly absorbed and highly protein bound Ømetabolized in the liver by CYP2C8 & CYP2C9 Øadministered once or twice daily Ødosage: 4-8 mg Øapproved as monotherapy or in combination with biguanides & sulfonylureas
Alpha-Glucosidase Inhibitors - are competitive inhibitors of the intestinal alpha-glucosidases and reduce the postprandial digestion and absorption of starch and disaccharides--> lowering postmeal glycemic excursions (45-60mg/dl) and creating an insulin-sparing effect - members: acarbose & miglitol - taken in doses of 25-100 mg just prior to ingesting the first portion of each meal - both are absorbed from the gut - SE: flatulence, Diarrhea, Abdominal pain - CI: Chronic or inflammatory bowel disease, Renal impairment, Hepatic disease (acarbose)
End of Discussion God Bless...