QOF- for beginners
QOF- for beginners. Revisiting the basics April 2007. What is it??. Quality & Outome Framework Links indicators of quality to method of funding general practice Not profit generating! Now amounts for up to third of all annual income Introduced in April 2004. What indicates quality??.


QOF- for beginners
E N D
Presentation Transcript
QOF- for beginners Revisiting the basics April 2007
What is it?? • Quality & Outome Framework • Links indicators of quality to method of funding general practice • Not profit generating! • Now amounts for up to third of all annual income • Introduced in April 2004
What indicates quality?? • Clinical • Administrative • Access • Development of IT • Practice Based Commissioning • Choose &Book
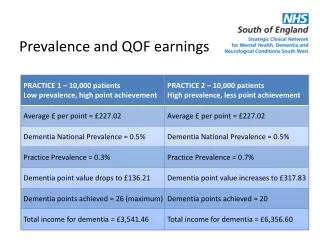
How is performance measured • Against targets of highest &lowest achievement on sliding scale of points • Points vary for each indicator • Lowest qualifying achievement usually 40%- highest 90-100%
Clinical areas • May just involve holding an electronic register • May have many indicators to meet for a specific patient/disease group • Some indicators apply to most or large portions of practice population e.g. smoking data or cervical cytology
CHD & Heart Failure Hypertension Atrial Fibrillation Stroke & TIA Hypothyroidism Dementia Depression Mental Health Learning Difficulty DM Chronic Kidney Disease Epilepsy Asthma COPD Cancer Palliative Care Obesity Ethnicity Clinical Areas
Administrative Areas • Policies & protocols • Medicines management • Education & meetings • Basic clinical data • Patient survey • Additional services
Balance of 1000 points • Clinical 655 • Holistic 20 • Organisational 181 • Additional 36 • Patient Experience 108
How is it measured • Submission written reports to PCT • Completion of on line template • Automatic extraction of data direct from system • Final data extracted on March 31st • To central site = QMAS • Calculates points from achievement – then calculates money • All subject to cross checking & audit by PCT
What does all this mean to running of the practice?? • Aiming for highest achievement is good for everyone • Generates lots of work/activity/appointment demand • System doesn’t run itself – needs constant attention
What have we got to help us?? • Protocols • Guidelines • Clinical audit • Reminders • Recall system • Exception reporting • Dedicated staff • BUT ONLY AS GOOD AS DATA PUT IN!!
Common pitfalls in data collection/recording • Read Coding • Losing track of patients with no or wrong recall • Forgetting the “all patients” data • Capturing outside data- knowing what is relevant & putting on our system in correct way • Ignoring yellow flags
Read Codes - 1 • Aim for Read Code formulary for every patient contact – clinical & administrative • Aim to use Codes that are straightforward and Contract-compatible • Use Guidelines • Use Keywords • Use Holding codes
Read Codes - 2 • Use Code at top of hierarchy • Do not use “H/o …” Codes • Do not use “PMH of …” • Remember Priorities • Use Recall buttons • Avoid multiple entries – some entries provoke “new diagnosis” time limits
Tricky clinical areas for data Entry of angina read code after 1st April 2003 requires something else to happen diagnostically Cardiological referral, EST, RA chest pain clinic Use holding codes until such an entry made. Beware new patients - summarisers CHD Heart failure Atrial Fibrillation Stroke/TIA
Entry heart failure read code has a diagnostic time limited requirement (after April 2006) Echocardiogram referral/result Use holding codes- again summarisers beware CHD Heart Failure Atrial fibrillation Stroke/TIA
Read code atrial fibrillation since requires something else to happen Requires ECG/cardiological referral ECG must be entered on guideline as different from usual way CHD Heart failure Atrial fibrillation Stroke/TIA
Entry stroke/TIA read code (after April 2006) requires something else to happen within Must have with it CT scan referral or result even if from secondary care 3months before or 12 months after Strokes need double coding- haemorrhagic or ischaemic CHD Heart failure Atrial fibrillation Stroke/TIA
Must have PHQ 9_with the read code Holding code otherwise until PHQ available Event type need to be changed from default of other to first ever Depression Mental health Epilepsy Diabetes
Lithium level after October Mental health review consists of evidence of physical check as well as specific indicators of mental health. Half doing a review is no help! Patients who DNA their planned review must be followed up within 14 days Depression Mental health Epilepsy Diabetes
Fit free needs to be positively entered in its own right If not fit free low threshold for using exemption Specific medication review Depression Mental health Epilepsy Diabetes
Miss no opportunity to ask for MA Do not enter a dip pos urine under proteinuria button Record every time patient asked/reminded to supply MA or go for retinal screening Depression Mental health Epilepsy Diabetes
Do not enter as read code based on eGFR alone especially at stage 3 Not necessarily changing antihypertensive on basis of CKD3 alone High use exemptions CKD Cancer Med revs
All conformed diagnosis must be identified from letters and coded/entered appropriately Episode type must be FIRST EVER Miss no opportunity for cancer care review CKD Cancer Med revs
Ensure no unused repeats remain on screen Every opportunity for med revs – careful how you do CKD Cancer Medication reviews