Kidney Exchange
470 likes | 492 Vues
Kidney Exchange. 4 th Barcelona Economics Lecture Hospital Clinic, Barcelona 8 November 2004. Roth, Alvin E., Tayfun Sönmez, and M. Utku Ünver, “ Kidney Exchange ,” Quarterly Journal of Economics , 119, 2, May, 2004, 457-488. ____ “ Pairwise Kidney Exchange ,” June 2004.

Kidney Exchange
E N D
Presentation Transcript
Kidney Exchange 4th Barcelona Economics LectureHospital Clinic, Barcelona 8 November 2004
Roth, Alvin E., Tayfun Sönmez, and M. Utku Ünver, “Kidney Exchange,” Quarterly Journal of Economics, 119, 2, May, 2004, 457-488. ____ “Pairwise Kidney Exchange,” June 2004. _____ “The Importance of Three Way Kidney Exchange,”in preparation
ProposalNew England Center for Kidney Donor Exchange Presented to the ROTC September 20, 2004 (Approved!) Frank Delmonico, MD (NEOB and MGH) Susan Saidman, PhD (MGH Histocompatibility Lab) Al Roth, PhD (Prof. of Economics & Business Admin, Harvard) Tayfun Somnez, PhD (Dept. of Economics, Koc University Utku Unver, PhD (Dept. of Economics, Koc University
On Saturday I gave a companion talk as the Pareto Lecture, at a conference of economic theorists • In that talk I emphasized some of the theoretical issues that arise in designing a Kidney Exchange. • Today I’ll speak more of practical issues, and how those shape what can be done (and what kind of theory is needed).
Economists As Engineers • In recent years, game theorists have become usefully involved in the design of markets. • See e.g. Roth and Peranson (1999), Roth (2002,medical labor markets) Wilson (2002, electricity markets), Abdulkadiroğlu and Sönmez (2003, schools), Milgrom (2004, auctions), Niederle and Roth (2004, gastroenterologist labor market) • A certain amount of humility is called for: successful designs most often involve incremental changes to existing practices, both because • It is easier to get incremental changes adopted, rather than radical departures from preceding practice, and • There may be lots of hidden institutional adaptations and knowledge in existing institutions, procedures, and customs.
Kidney transplants • There are over 60,000 patients on the waiting list for cadaver kidneys in the U.S. • In 2003 there were over 8,500 transplants of cadaver kidneys performed in the U.S. (and over 2,000 in Spain, which has one of the most effective cadaver organ donation systems in the world) • In the same year, about 3,500 patients died while on the waiting list. • In 2003 there were also over 6,000 transplants of kidneys from living donors in the US, a number that has been increasing steadily from year to year. • (I don’t know the local statistics, but I understand that the Hospital Clinic is one of the places at which live donor transplants are done here.)
Live-donor transplants are much less organized than cadaver transplants • The way such transplants are typically arranged is that a patient identifies a willing donor and, if the transplant is feasible, it is carried out. • Otherwise, the patient remains on the queue for a cadaver kidney, while the donor returns home. • Recently, however, in a small number of cases, additional possibilities have been utilized: • Paired exchanges: exchanges between incompatible couples • Indirect exchanges: an exchange between an incompatible couple and the cadaver queue
Baltimore Center Carries Out Triple-Swap TransplantsAugust 2, 2003, New York Times “The triple-swap kidney transplant operation was announced in a news conference today at the Johns Hopkins Comprehensive Transplant Center, which said it believed that this was the first time three simultaneous kidney transplants have been performed… “Months in the making, the exchange was the only way all three recipients could have received a kidney, the lead surgeon, Dr. Robert A. Montgomery, said, because of tissue, blood or antibody incompatibilities among the donors and their originally designated recipients.” • Johns Hopkins has recently hired a paired kidney exchange coordinator to facilitate further exchanges
How might more frequent and larger-scale kidney exchanges eventually be organized? • Building on existing practices in kidney transplantation, we consider how exchanges might be organized to produce efficient outcomes, providing consistent incentives (dominant strategy equilibria) to patients-donors-doctors. • Why are incentives/equilibria important? (becoming ill is not something anyone chooses…) • But if patients, donors, and the doctors acting as their advocates are asked to make choices, we need to understand the incentives they have, in order to know the equilibria of the game and understand the resulting behavior. • Experience with the cadaver queues make this clear…
Incentives: liver transplants Chicago hospitals accused of transplant fraud 2003-07-29 11:20:07 -0400 (Reuters Health) CHICAGO (Reuters) – “Three Chicago hospitals were accused of fraud by prosecutors on Monday for manipulating diagnoses of transplant patients to get them new livers. “Two of the institutions paid fines to settle the charges. ‘By falsely diagnosing patients and placing them in intensive care to make them appear more sick than they were, these three highly regarded medical centers made patients eligible for liver transplants ahead of others who were waiting for organs in the transplant region,’ said Patrick Fitzgerald, the U.S. attorney for the Northern District of Illinois.” • These things look a bit different to economists than to prosecutors: it looks like these docs may simply be acting in the interests of their patients…
Incentives and efficiency:Neonatal heart transplants • Heart transplant candidates gain priority through time on the waiting list • Some congenital defects can be diagnosed in the womb. • A fetus placed on the waiting list has a better chance of getting a heart • And when a heart becomes available, a C-section might be in the patient’s best interest. • But fetuses (on Mom’s circulatory system) get healthier, not sicker, as time passes and they gain weight. • So hearts transplanted into not-full-term babies may have less chance of surviving. Michaels, Marian G, Joel Frader, and John Armitage [1993], "Ethical Considerations in Listing Fetuses as Candidates for Neonatal Heart Transplantation," Journal of the American Medical Association, January 20, vol. 269, no. 3, pp401-403
Kidney Matching • Two genetic characteristics play key roles: • ABO blood-type: There are four blood types A, B, AB and O. • Type O kidneys can be transplanted into any patient; • Type A kidneys can be transplanted into type A or type AB patients; • Type B kidneys can be transplanted into type B or type AB patients; and • Type AB kidneys can only be transplanted into type AB patients. • So type O patients are at a disadvantage in finding compatible kidneys.
2. Tissue type or HLA type: • Combination of six proteins, two of type A, two of type B, and two of type DR. • Prior to transplantation, the potential recipient is tested for the presence of antibodies against HLA in the donor kidney. The presence of antibodies, known as a positive crossmatch, significantly increases the likelihood of graft rejection by the recipient and makes the transplant infeasible.
Goals of a structured method of direct kidney exchange • Assemble a database of incompatible patient-donor pairs. (Right now, the incompatible donors are largely lost.) • Identify which exchanges are possible, and which sets of exchanges make best use of available donor kidneys • allow not only for paired-exchange but also other forms of exchange such as a three-way exchange.
Some relevant economics papers • Shapley, Lloyd and Herbert Scarf (1974), “On Cores and Indivisibility,” Journal of Mathematical Economics, 1, 23-37. • Roth, Alvin E. and Andrew Postlewaite (1977), “Weak Versus Strong Domination in a Market with Indivisible Goods,” Journal of Mathematical Economics, 4, 131-137. • Roth, Alvin E. (1982), “Incentive Compatibility in a Market with Indivisible Goods,” Economics Letters, 9, 127-132. • Atila Abdulkadiroğlu and Tayfun Sönmez [1999] House allocation with existing tenants. Journal of Economic Theory 88, 233-260.
DONOR KIDNEY EXCHANGE FOR INCOMPATIBLE RECIPIENTS • by Francis L. Delmonico, MD 1, Paul E. Morrissey, MD 1, George S. Lipkowitz, MD 2, Jeffrey S. Stoff, MD 1, Jonathan Himmelfarb, MD 1, William Harmon, MD 1, Martha Pavlakis, MD 1, Helen Mah 1, Jane Goguen 1, Richard Luskin 1, Edgar Milford, MD 1 and Richard J. Rohrer, MD 1. 1, New England Organ Bank, Newton, MA and 2, LifeChoice Donor Services, Windsor, CT. • Reports two live donor exchanges (4 recipients) and 8 list paired exchanges (16 recipients) from 2001-02.
House allocation • Shapley & Scarf [1974] housing market model: n agents each endowed with an indivisible good, a “house”. • Each agent has preferences over all the houses and there is no money, trade is feasible only in houses. • Gale’s top trading cycles (TTC) algorithm: Each agent points to her most preferred house (and each house points to its owner). There is at least one cycle in the resulting directed graph (a cycle may consist of an agent pointing to her own house.) In each such cycle, the corresponding trades are carried out and these agents are removed from the market together with their assignments. • The process continues (with each agent pointing to her most preferred house that remains on the market) until no agents and houses remain.
Theorem (Shapley and Scarf): the allocation x produced by the top trading cycle algorithm is in the core (no set of agents can all do better than to participate) • When preferences are strict, Gale’s TTC algorithm yields the unique allocation in the core (Roth and Postlewaite 1977).
Theorem (Roth ’82): if the top trading cycle procedure is used, it is a dominant strategy for every agent to state his true preferences. • The idea of the proof is simple, but it takes some work to make precise. • When the preferences of the players are given by the vector P, let Nt(P) be the set of players still in the market at stage t of the top trading cycle procedure. • A chain in a set Nt is a list of agents/houses a1, a2, …ak such that ai’s first choice in the set Nt is ai+1. (A cycle is a chain such that ak=a1.) • At any stage t, the graph of people pointing to their first choice consists of cycles and chains (with the ‘head’ of every chain pointing to a cycle…).
Cycles and chains Cycles and chains i
The cycles leave the system (regardless of where i points), but i’s choice set (the chains pointing to i) remains, and can only grow i
Paired kidney exchanges similarly seek the gains from trade among patients with willing donors, but (with the recent Johns Hopkins 3-pair exchange being a notable exception) mostly among just two pairs. • In the context of kidney exchange, if we consider exchange only among patients with donors, the properties of the housing market model essentially carry over unchanged (as long as donor preferences coincide with those of their intended recipient). • However donors (unlike houses) have preferences. So all parts of a live-donor exchange are done simultaneously, to avoid incentive problems.
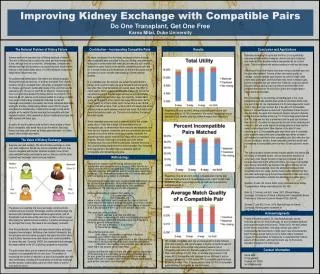
How big are the welfare gains? • Theory show us how to go from inefficient to efficient procedures, but it doesn’t tell us how big the gains are likely to be. • For that we turn to computational simulations, using data on the mismatch frequencies, patient demographics, etc. • We first consider unrelated donor-patient pairs. (About 25% all living-donor transplants were in this category in 2001.)
Patient and Donor Characteristics • Population: Caucasian ESRD patient population between 18 and 79 years of age in the U.S. Renal Data System (USRDS). • Blood-type and age distribution: Distributions for new ESRD waitlist patients recorded between January 1995 and April 2003 in the USRDS database. • Gender distribution: Data recorded between 1992 and 2001. • HLA distribution: The distribution reported in Zenios [1996] using the USRDS registration data for years between 1988 and 1991. • We assume that all HLA proteins and blood type are independently distributed following Zenios [1996].
Simulated patient preferences • Preferences are determined using the graft survival analysis of Mandal et. al. [2003]. We assume that the preferences of each patient depends on the donor age and the number of HLA mismatches. Using the graft survival analysis of Mandal et. al. [2003], MRS is determined as • 5.14 years of younger donor age per each additional HLA mismatch for patients younger than 60 years of age, and • 5.10 years of younger donor age per each additional HLA mismatch for patients older than 59 years of age
How about actual patient populations? • While the simulated results look good, they are drawn from general patient distributions. • Actual patient populations will consist of incompatible patient-donor pairs. • Patients who are already known to be incompatible with one donor may be much harder to match…e.g. they are more likely to be highly sensitized
MGH Dataset (constructed by Susan Saidman) • MGH patients w/ incompatible (ABO or XM) donor(s) • Data included • ABO type of patient & donor • HLA type of patient & donor • Most recent class I and II PRAs • Called abs or safe antigens • Relationship of donor to recipient • Reason donor was incompatible • If donor not HLA typed, HLA types were assigned from list of UNOS deceased donors • 44 patients and 68 donor/patient pairs • 23 O; 13 A; 6 B; 2 AB
Note that • The initial screening and computer match identifies potentially compatible donor and recipient pairs • A crossmatch will always be required before pair can be confirmed to be compatible • Extensive antibody screening of patients and careful identification of all antibody specificities by a sensitive and specific method can help prevent unexpected positive crossmatches
Summary of analysis of MGH dataset • If only two wayexchanges allowed • 8 patient-donor pairs in the dataset can potentially exchange kidneys (2 ABO-O; 3 ABO-A; 3 ABO-B) • If three way exchanges allowed • 11 patient-donor pairs in the dataset can potentially exchange kidneys (3 ABO-O; 3 ABO-A; 4 ABO-B; 1 ABO-AB) • There is also a possible five way exchange • Allows 12 patient-donor pairs to potentially exchange kidneys • But logistics currently not practical
Discussion of the Computational Results • The computational results (for both the simulated data and the MGH data) suggest that adoption of the TTC mechanism will significantly improve the utilization rate of potential living-donor kidneys. • But under the TTC mechanism, average/maximal sizes of exchanges grow as the population grows. For large populations of patient-donor pairs, some of the efficient exchanges may be impractically large.
Suppose exchanges involving more than two pairs are impractical? • Our New England surgical colleagues have 0-1 (feasible/infeasible) preferences over kidneys. • Initially, exchanges may be restricted to pairs. (see also Bogomolnaia and Moulin (2004) • This involves a substantial welfare loss compared to the unconstrained case • But it allows us to tap into some elegant graph theory for constrained efficient and incentive compatible mechanisms.
Pairwise matchings and matroids • Let (V,E) be the graph whose vertices are incompatible patient-donor pairs, with mutually compatible pairs connected by edges. • A matching M is a collection of edges such that no vertex is covered more than once. • Let S ={S} be the collection of subsets of V such that, for any S in S, there is a matching M that covers the vertices in S • Then (V, S) is a matroid: • If S is in S, so is any subset of S. • If S and S’ are in S, and |S’|>|S|, then there is a point in S’ that can be added to S to get a set in S.
Pairwise matching with 0-1 preferences • All maximal matchings match the same number of couples. • If patients have priorities, then a “greedy” priority algorithm produces the efficient (maximal) matching with highest priorities. • Any priority matching mechanism makes it a dominant strategy for all couples to • accept all feasible kidneys • reveal all available donors • So, there are efficient, incentive compatible mechanisms in the constrained case also.
Summary There are several potential sources of increased efficiency from assembling a database of incompatible pairs (aggregating across time and space), including • More couple exchanges • longer cycles of exchange, instead of just pairs If longer cycles of exchange aren’t (initially) feasible, constrained efficient matches can still be achieved with good incentive properties
Why 3-way exchanges add so much • Example: Consider a population of 9 incompatible patient donor pairs consisting of • O-A, O-B (difficult to match O patients) • A-B, A-B, B-A (more A-B than B-A pairs) • A-A, A-A, A-A (odd number of A-A pairs) • B-O (scarce O donor) • 3 two-way exchanges are possible: 6 transplants • (A-B,B-A); (A-A,A-A); (B-O,O-B) • If three-way exchanges are also feasible: 8 transplants • (A-B,B-A); (A-A,A-A,A-A); (B-O,O-A,A-B)
Four-way exchanges add less • In connection with blood type (ABO) incompatibilities, 4-way exchanges add less, but make additional exchanges possible when there is a (rare) incompatible patient-donor pair of type AB-O. • (AB-O,O-A,A-B,B-AB) is a four way exchange in which the presence of the AB-O helps three other couples… • Incompatibilities involving positive cross matches may sometimes generate larger exchanges, but it appears that these are relatively rare
Summary (for surgeons):What do the economists bring to the table? • To arrange exchanges efficiently in a population of patients with incompatible donors, there are distributional issues, not just issues of medical compatibility. • For example, consider four incompatible patient-donor pairs P1, P2, P3, P4, and suppose pairwise exchanges are possible between P1 and P2; P2 and P3, and P1 and P4. • Then the exchange P1-P2 results in two transplantations, but the exchanges P1-P4 and P2-P3 results in four.
Summary (for economists) • As game theorists start to take a more active role in practical market design, we have to deal with constraints, demands, and situations different than those that arise in the simplest theoretical models of mechanism design • Here we address some of the issues that have come up as we try to help surgeons implement an organized exchange of live-donor kidneys • Not only do these issues appear to allow satisfactory practical solutions, they suggest new directions in which to pursue the underlying theory.