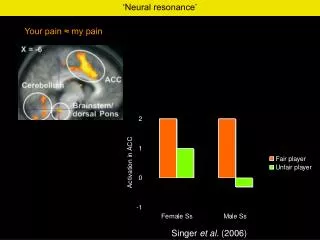
Orofacial Pain
Orofacial Pain. A relatively common symptom. Sources of orofacial pain include caries, periodontitis, neuropathic, and musculoskeletal conditions. Symptoms of pain may represent different phases of acute or chronic conditions.

Orofacial Pain
E N D
Presentation Transcript
A relatively common symptom. • Sources of orofacial pain include caries, periodontitis, neuropathic, and musculoskeletal conditions. • Symptoms of pain may represent different phases of acute or chronic conditions. • Based on NHIS data from 1989, survey participants representing 39 million adults reported experiencing at least one of five orofacial pain symptoms in the past 6 months: • tooth pain, • mouth sores, • jaw joint pain, • facial pain, • burning mouth (Lipton et al., 1993). http://drc.hhs.gov/report/pdfs/section10-orofacialpain.pdf
Orofacial pain is often divided into two categories.chronic and acute. • The National Center for Health Statistics generally uses a cut off point of 3 months to distinguish between acute and chronic pain. • Currently, there are no national data on orofacial pain for children. • Data sources other than the 1989 NHIS include studies on a population of elderly adults (65+) living in 10 northern Florida counties (Riley et al., 1998); studies of adults 45 and older, also located in northern Florida (Gilbert et al., 1997); a survey of adults in Toronto (Locker & Grushka, 1987); and studies on temporomandibular joint disorder, or TMD, reviewed by LeResche (1997). http://drc.hhs.gov/report/pdfs/section10-orofacialpain.pdf
What types of orofacial pain do we see? • Community • Macfarlane et al 2004 – n = 125 total 1510
Prevalence of selected pain conditions by poverty status: US adults, 18 years and over Adjusted for age SOURCE: Lethbridge-Cejku M, Rose D, Vickerie J. Summary health statistics for US Adults: National Health Interview Survey, 2004. National Center for Health Statistics.Vital Health Stat 10 (228). Hyattsville, MD 2006
Chronic Orofacial pain • The cost of chronic pain is estimated to be about $80 billion per year, 40% associated with orofacial pain (Israel & Scrivani, 2000; Friction & Schiffman, 1995). • The two most prevalent sources of chronic orofacial pain are temporomandibular joint disorder (TMD) and burning mouth syndrome. http://drc.hhs.gov/report/pdfs/section10-orofacialpain.pdf
Chronic Orofacial pain • TMD consists of jaw joint pain and dull facial pain in the temporomandibular joint and the muscles of mastication. Chronic TMD is estimated to affect from 3% to 12% of the U.S. population (Klausner, 1995). • Burning mouth syndrome is characterized as a burning, tender, or annoying sensation in the mouth with no apparent mucosal lesion. • In 1989, the prevalence of jaw joint pain, burning mouth, and dull facial pain in the U.S. population was 5.3%, 0.7%, and 1.5%, respectively. http://drc.hhs.gov/report/pdfs/section10-orofacialpain.pdf
Acute orofacial pain • Acute orofacial pain includes tooth pain and painful sores or irritations of the mouth. • Tooth pain is often caused by dental caries but may also be due to periodontal disease. • Tooth pain can interfere with work and social activities, promote anxiety, and result in economic costs.
Acute orofacial pain • Data from the 1989 NHIS Orofacial Pain Supplement indicate that the overall prevalence of tooth pain and of mouth sores in the United States was 13.6% and 8.4%, respectively. • The prevalence of tooth pain was higher among adults 20 to 64 years of age than among those 65 and older, those with lower education, poorer people, and those who visited a dentist within the past 12 months. (Vargas et al. 2000 and Lipton et al. 1993)
OROFACIAL PAIN in CANADA
Prevalence of orofacial pain in a sample of adults in the USA during a 6-month period (Lipton 1993)
Percentage of oral facial pain among adults in USA and Canada (Goulet et al., 1995; Lipton et al., 1993; & Ripley et al., 2001)
Proportion of subjects with no, mild, moderate and severe jaw pain reporting sleep problems, difficulty in opening and joint clicking in Quebec (Goulet et al., 1995)
OROFACIAL PAIN in Other studies
Pain “The subject’s conscious perception of modulated nociceptive impulses that generate an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage” (IASP definition, 1994)
History and Description of Pain • Compliant • Site of pain • What starts the pain • Duration of attack • Pain intensity • Quality of pain • When pain was first noted • When pain occurs
History Ex. of Orofacial Pain C. Characteristics of pain • Quality of pain • Behaviour of pain • Temporal • Frequency • Duration • Intensity • Concomitant symptoms • Flow of pain 1. Chief complaints A. Location of pain B. Onset of pain • Association with other factors • Progression
History Ex. of Orofacial Pain • E. Past consultation and/or treatment • F. Relationship to other complaints • 2. Past medical history • 3. Review of systems • 4. Psychological assessment 1. Chief complaints (cont.) D. Aggravating and alleviating factors • Physical modalities • Function and parafunction • Sleep disturbances • Medications • Emotional stress
Clinical Examination E. Cervical evaluation F. Balance and co-ordination 2. Muscle examination A. Pulpation • Pain and tenderness • Trigger points and pain referal 1. General examination A. Vital signs • Blood pressure • Pulse rate • Respiratory rate • Temperature B. Cranial nerve evaluation C. Eye evaluation D. Ear evaluation
Clinical Examination C. Oral structures • Mucogingival tissues • Teeth • Periodontium • Occlusion 4. Other diagnostic tests A. Imaging B. Laboratory tests C. Psychologic provocation tests 3. Masticatory evaluation A. Range of mandibular movement • Measurement • Pain B. Temoromandibular joint evaluation • Pain • Dysfunction
Characteristics of pulpal sensory fibres (Trowbridge and Kim, 1991)
Stress and Orofacial Pain
ENVIRONMENT BEHAVIOUR NERVOUS SYSTEM HOMEOSTASIS IMMUNE SYSTEM ENDOCRINE SYSTEM
BRAIN STRESS IL-1 CRH HIPPOCAMPUS HYPOTHALAMUS IMMUNE CELL PITUITARY ACTH ADRENAL GLAND glucocorticoids glucocorticoids
Signs and Symptoms of Stress • Physical Signs and Symptoms • Emotional Signs and Symptoms • Cognitive/Perceptual Signs and Symptoms • Behavioral Signs and Symptoms
1. Physical Signs and Symptoms of Stress increased heart rate; pounding heart; elevated blood pressure; sweaty palms; tightness of the chest, neck, jaw and back muscles; headache; diarrhea; constipation; urinary hesitancy; trembling, twitching;
1. Physical Signs and Symptoms of Stress stuttering and other speech difficulties; nausea; vomiting; sleep disturbances; fatigue; shallow breathing; dryness of the mouth or throat; susceptibility to minor illness, cold hands, itching; being easily startled; chronic pain and dysponesis
2. Emotional Signs and Symptoms of Stress • irritability, angry outbursts, hostility, • depression, jealously, restlessness, withdrawal, • anxiousness, diminished initiative, • feelings of unreality or overalertness, • reduction of personal involvement with others, lack of interest, tendency to cry,
2. Emotional Signs and Symptoms of Stress • being critical of others, self-deprecation, • nightmares, impatience, • decreased perception of positive experience opportunities, • narrowed focus, obsessive rumination, • reduced self-esteem, insomnia, • changes in eating habits and weakened positive emotional response reflexes
3. Cognitive/Perceptual Signs and Symptoms of Stress • forgetfulness, preoccupation, blocking, • blurred vision, errors in judging distance, • diminished or exaggerated fantasy life, reduced creativity, • lack of concentration, diminished productivity, • lack of attention to detail, • orientation to the past,
3. Cognitive/Perceptual Signs and Symptoms of Stress • decreased psychomotor reactivity and coordination, • attention deficit, disorganization of thought, • negative self-esteem, • diminished sense of meaning in life, • lack of control/need for too much control, • negative self-statements and negative evaluation of experiences
4. Behavioral Signs and Symptoms of Stress • increased smoking, • aggressive behaviors (such as driving), • increased alcohol or drug use, • carelessness, • under-eating, over-eating, • withdrawal, listlessness,
4. Behavioral Signs and Symptoms of Stress • hostility, • accident-proneness, • nervous laughter, • compulsive behavior and impatience
Memory Psyche Sensory Arousal Respiratory control Pituitary gland Sympathetic NS GI system Adrenal cortex Kidney Adrenal medulla Cardiovascular system Adrenaline Immune-Inflam response Electrolyte water control Haemostasis-fibrinolysis Metabolism Limbic system Metabolic and Haemostatic changes
ความเครียดกับโรคทางร่างกายความเครียดกับโรคทางร่างกาย • Stress ส่งผลให้มีการเพิ่มการหลั่งACTH, GH, PRL, beta-endorphine, ADH, insulin and glucagonACTH --> cortisol --> NE --> E • Stress stimulate sympathetic nervous systemCardiac Output, Stroke Volume, systolic Blood Pressure blood flow to muscle, skin blood glucose rate of blood coagulation
Cardiovascular responses • Increase Heart rate, Cardiac output, Blood pressure, muscle blood flow • ผู้ป่วยที่มีภาวะ hypertension, obesity, high fat dietStress --> cortisol or epihephine --> cholesterol --> coronary artery disease Arteriosclerosis Myocardial infarction Other
Gastrointestinal responses • อาหารติดคอ, ปวดท้อง, diarrhea, fullness, nausea หลังอาหารincrease gastric acid, mobility --> peptic ulcer • Respiratory responses Hyperventilation --> hypocapnea Cerebral vasoconstriction dizziness, confusion, paraesthesia, tetany Cooling --> trigger --> asthmatic attack