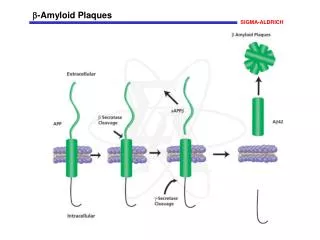
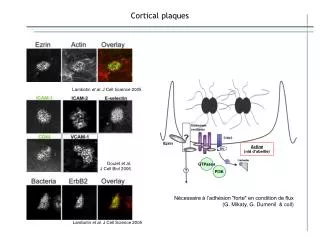
NON-SCALY PLAQUES
Group 2 Sy A, Sy J, Sydiongco, Tacata, Tady, Tamondong, Tan E, Tan G, Tan M, Tan S. NON-SCALY PLAQUES. SY, Aaron Keefe S. FIXED DRUG ERUPTION. FIXED DRUG ERUPTION. recur at the same site with each exposure to medications Six or fewer lesions occur, frequently one

NON-SCALY PLAQUES
E N D
Presentation Transcript
Group 2 Sy A, Sy J, Sydiongco, Tacata, Tady, Tamondong, Tan E, Tan G, Tan M, Tan S NON-SCALY PLAQUES
SY, Aaron Keefe S. FIXED DRUG ERUPTION
FIXED DRUG ERUPTION • recur at the same site with each exposure to medications • Six or fewer lesions occur, frequently one • May be present anywhere on the body, but half occur on the oral and genital mucosa
Clinical Features • Begins as a red patch • Evolves to an iris or target lesion identical to erythema multiforme that may eventually blister and erode • Lesions of genital and oral mucosa presents as erosions • Most lesions are 1 to several cm in diameter. • New lesions may be added with continiued /repeated ingestion of the medication.
Pathophysiology • Exact mechanism is unknown • Recent research suggests a cell-mediated process that initiates both the active and quiescent lesions. • Lesion contain intraepidermal CD8+ T-cells with the phenotypic markers of effector memory T-cells. • Skin-resident T-cells rapidly produce IFN-γon exposure to medication.
Histologic Features • An interface dermatitis occuring with intraepidermal and subepidermal vesicle formation, necrosis of keratinocytes and a mixed superficial and deep infiltrate of neutrophils, eosinophils, and mononuclear cells. • Stratum corneum is normal in acute stage. • Papillary dermal fibrosis and deep perivascular pigment incontinence are commonly present from prior episodes.
Etiologic Agents • Medications usually taken intermittently. • NSAIDS, esp. Pyrazole derivatives, Paracetamol, Naproxen, Oxicams, & Mefenamic Acid – predilection for the lips • Sulfonamides, Trimethoprim or the combination – resp. for majority of genital fixed drug eruptions
Possible Etiologic Agents Include: • Barbiturates • Tetracyclines • Phenolphthalein (in laxative) • Acetaminophen • Ceterizine • Celecoxib • Dextromethophan • Hydroxyzine • Lamotrigine • Phenylpropanolamine • Erythromycin • Chinese & Japanese herbs
Patch Testing • needed to determine which drug may be involved • Patch tests with various concentrations of the offending medication can reproduce the lesion on an affected but not unaffected skin. • Most useful in pyrazolone derivative-related reactions.
Nonpigmenting Fixed Drug Eruption • large, tender, often symmetrical eythematous plaques • Resolve completely within weeks. • Pseudoephedrine hydrochloride – most common cause • Baboon Syndrome – buttocks, groin, axilla
Treatment • Main goal - identify the causative agent and avoid it. • Lesions of fixed drug eruption resolve spontaneously with avoidance of the inciting drug.
Sy, Jamelle D. ERYSIPELAS
ERYSIPELAS St. Anthony’s fire /ignis sacer • an acute beta-hemolytic group A streptococcal infection of the skin involving the superficial dermal lymphatics • group B – perineal erysipelas
ERYSIPELAS • local redness, heat, swelling, & a highly characteristic raised, indurated border • PMN leukocytosis • skin lesions: transient hyperemia vesicles or bullae • legs and face are the most frequent sites affected
CELLULITIS Sydiongco, Paula
TACATA, Patricia TADY, Clarissa Marie URTICARIA
URTICARIA (HIVES) • characterized by wheals surrounded by a red halo orflare • severe itching, stinging or pricking • annular or polycyclicpattern clearing of central region and coalescence of lesions
URTICARIA (HIVES) • Subcutaneous swellings (angioedema) may accompany the wheals • target the gastrointestinal and respiratory tracts resulting in abdominal pain, coryza, asthma and respiratory problems.
COMMON TRIGGERS • Opiates • Polymyxin B • Tubocurarine • Aspirin and other NSAIDS • Tartrazine • Benzoate
Treatment • Acute Urticaria • Antihistamines Non-sedating Histamines pose a lower risk of psychomotor problem in adults. • Avoid the trigger if the cause can be identified • Systemic corticosteroids • For severe reactions, respiratory and cardiovascular support is essential. • Intubation and tracheotomy may be required.
Chronic Urticaria • Mainstay treatment: Antihistamines • Should be taken on a daily basis and not prescribed to be taken as needed • Second generation antihistamine produce less sedation in most patients • Second line treatment • Phototherapy • Calcium channel antagonist • Antimalarial medications • Methotrexate • Corticosteroids produce long term side effects • Local treatment • Tepid or cold tub baths • Topical camphor and menthol
Angioedema • Acute, evanescent, circumscribed edema • Area of predeliction: Eyelids, lips, lobes of ears, external genitalia, or mucous membranes of the mouth, tongue, or larynx • Swelling occurs in the lower layers of the skin or in the subcutaneous tissues • Frequently begins during night and is found on awakening • Two subtypes: Deep form Angioedema associated w/ C1 esterase inhibitor deficiency
Hereditary Angioedema (HAE) • Quincke edema • 2nd – 4th decade, Autosomal dominant inheritance • Swelling: Asymmetrical without urticaria or itching In subcutaneous tissues and abdominal organs mimicking surgical emergencies, and the upper airway (larynx) – life-threatening • Little response to antihistamines, epinephrine, or steroids • High mortality rate – death often caused by laryngeal edema • 3 phenotypic forms: Type I Type II Type III • Trigger factors: minor trauma, surgery, sudden changes in temperature, or sudden emotional stress
Acquired C1 Esterase Inhibitor Deficiency Usually occurs after 4th decade of life No family history • Not associated w/ pruritis or urticaria • Two subtypes: A. Acquired angioedema-I • Rare disorder associated with lymphoproliferative diseases • Treatment: Replacement of C1-EI with concentrates or FFP; antifibrinolytic agents; synthetic Danazol B. Acquired angioedema-II • Extremely rare disease • Treatment: Immunosuppresive therapy; Synthetic corticosteroids (temporarily effective); Plasmapheresis
Episodic Angioedema with Eosinophilia • Uncommon disorder w/ no underlying disease • Isolated facial edema • May occur with fever, weight gain, eosinoophilia and elevated eosinophil major basic protein • Treatment: administration of systemic steroidal medications, antihistamines, and IVG
Schnitzler Syndrome • Rare disorder • Combination of chronic, non-pruritic urticaria, fever of unknown origin, disabling bone pain, hyperostosis, increased erythrocyte sedimentation rate, and monoclonal IgM gammopathy • Age of onset: 29-77 years old; affects both sex • Effective therapy has not been determined • Bone pain and urticarial lesion respond to systemic corticosteroids