Reproductive System
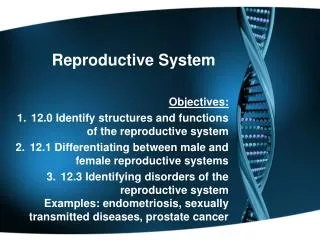
Chapter 18 A&P1 Tutor: Eleshia Howell. Reproductive System. The reproductive system is the only system that is not essential to the life of the individual (although its activities do affect other systems).

Reproductive System
E N D
Presentation Transcript
Chapter 18 A&P1 Tutor: Eleshia Howell Reproductive System (c) Eleshia Howell, 2012.
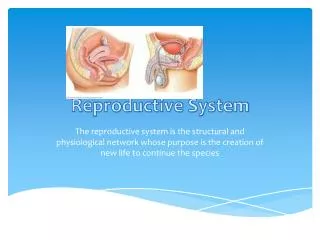
The reproductive system is the only system that is not essential to the life of the individual (although its activities do affect other systems). • This system ensures the continued existence of the human species – by producing, storing, nourishing and transporting functional male and female reproductive cells. (c) Eleshia Howell, 2012.
The ability to reproduce distinguishes living from non-living organisms • In human, the process occurs by sexual reproduction, in which the male & female organs differ anatomically as well as physically, and the new individual develops from the fusion of the two different sex cells. (c) Eleshia Howell, 2012.
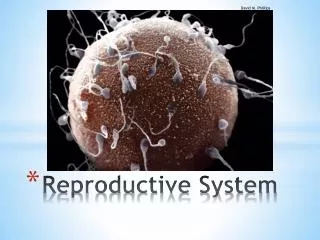
Adult males and females produce specialised reproductive germ cells, called gametes • Male gametes ~ spermatozoa • Female gametes ~ ova • They contain the genetic material (genes) on chromosomes, which pass inherited characteristics on to the next generation. (c) Eleshia Howell, 2012.
All other body cells have 46 chromosomes, arranged in 23 pairs....but gametes only contain 23 (one from each pair) • Gametes are formed by Meiosis – a process of cell reproduction that results in genetic diversity as the chromosomes “cross over” – producing 4 x daughter cells each with 23 chromosomes. (c) Eleshia Howell, 2012.
During fertilisation, a zygote is formed by the fusion of an ovum and a spermatozoon , and the full complement of chromosomes (46) is restored. • The zygote embeds itself in the uterine wall where it grows and develops over a 40 week gestation period. (c) Eleshia Howell, 2012.
Female Reproductive System FUNCTION: • Formation of ova • Reception of spermatozoa • Provision of suitable environments for fertilisation & foetal development • Parturition (childbirth) • Lactation (production of breast milk) • Female genitalia are both internal & external (c) Eleshia Howell, 2012.
Female reproductive organs, p438 (c) Eleshia Howell, 2012.
External Genitalia • Known collectively as the “vulva” • Consists of: • Labia Majora & Minora, • Clitoris • Vaginal orifice • Vestibule • Hymen • Vestibular glands (Bartholin’s Glands) (c) Eleshia Howell, 2012.
Female external genitalia p439 (c) Eleshia Howell, 2012.
Labia Majora~ • Are the two large folds forming the outer boundary of the vulva • Composed of skin, fibrous tissue and fat; contains large numbers of sebaceous glands • Anteriorly, they join in front of the symphysis pubis; posteriorly they merge with the skin of the perineum • At puberty, hair grows on the mons pubis as well as the lateral edges of the labia majora (c) Eleshia Howell, 2012.
Labia Minora~ • Two smaller folds between the majora, also containing numerous sebaceous glands • The cleft between the labia minora is the vestibule; the vagina, urethra and ducts of the greater Bartholin’s glands open into the vestibule. (c) Eleshia Howell, 2012.
Clitoris ~ • Is the female equivalent of the penis in males • Contains sensory nerve endings & erectile tissue • Has no reproductive significance (c) Eleshia Howell, 2012.
Hymen ~ • A thin layer of mucous membrane that partially occludes the opening of the vagina • It is normally incomplete to allow for the passage of menstrual flow; the size of the hymenal opening increases with age. • It can be “broken” via physical activity, insertion of tampons or sexual intercourse / vaginal penetration. (c) Eleshia Howell, 2012.
Vestibular Glands ~ • Or Bartholin’s Glands, are small pea-sized glands located on each side of the vaginal opening, with ducts leading into the vestibule and around the hymen • They secrete mucous to keep the vulva moist. (c) Eleshia Howell, 2012.
Perineum ~ • Is the area extending from the base of the labia minora to the anal canal. • It is roughly triangular shaped and consists of connective tissue, muscle and fat. • Provides attachment for the muscles of the pelvic floor. (c) Eleshia Howell, 2012.
Blood, Lymph & Nerve Supply • Arterial supply is from branches of the internal & external pudendal arteries, which branch off the internal iliac & femoral arteries respectively. • Venous drainage forms a small plexus that eventually leads into internal iliac veins. • Lymph drains into superficial inguinal nodes • The pudendal nerve innervates the external genitalia. (c) Eleshia Howell, 2012.
Internal Genitalia • Occupy the pelvic cavity and consist of: • Vagina • Uterus • Uterine tubes (fallopian tubes) x 2 • Ovaries x 2 (c) Eleshia Howell, 2012.
Vagina • A fibromuscular tube lined with stratified squamous epithelium, connecting the external and internal structures of the female reproductive system. • It is positioned obliquely upwards and backwards at approx 45° angle, between the bladder and rectum. • It is about 7.5cm in length at the anterior wall, 9cm long posterior wall. (c) Eleshia Howell, 2012.
The vagina is constructed of 3 layers: • Outer areolar tissue • Middle smooth muscle • Inner lining of stratified squamous epithelium that forms rugae • It has no secretory glands but the surface is kept moist by cervical secretions • pH is balanced between 4.9 – 3.5; acidity inhibits growth of most other micro-organisms. (c) Eleshia Howell, 2012.
Blood Supply, Lymph Drainage & Nerve Supply: • An arterial plexus is formed around the vagina from branches of uterine and vaginal arteries (from internal iliac arteries) • Venous plexus, in muscular wall, drains into internal iliac veins • Lymph drains into deep & superficial iliac nodes • PSN from sacral outflow, SN from Lumbar outflow, somatic sensory from Pudendal n. (c) Eleshia Howell, 2012.
Function of Vagina: • A receptacle for the penis during sexual intercourse • Provides an elastic passageway for baby to pass through during childbirth. (c) Eleshia Howell, 2012.
Uterus • A hollow, muscular, pear-shaped organ, flattened anteroposteriorly. It lies in the pelvic cavity, between the urinary bladder & rectum. • In most women, it leans forward (anteversion) and is bent forward (anteflexion), almost at right angles to the vagina. (c) Eleshia Howell, 2012.
When the body is upright, the uterus lies in an almost horizontal position. • It is about 7.5cm long, 5cm wide and its walls are about 2.5cm thick; weighs 30-40g. • The parts of the uterus are: • Fundus – dome shaped part at the top • Body – the main part, narrowest inferiorly where it is continuous with the cervix • Cervix – ‘neck’ of the uterus which protrudes into the anterior wall of the vagina. (c) Eleshia Howell, 2012.
The walls of the uterus are composed of 3 layers: • Perimetrium– is peritoneum, covering the fundus and body. Laterally, it forms the broad ligament, attaching the uterus to the sides of the pelvis. • Myometrium – thickest layer of smooth muscle, areolar tissue, blood vessels & nerves • Endometrium – consists of columnar epithelium containing mucus secreting tubular glands. It is divided functionally into two layers: (c) Eleshia Howell, 2012.
Endometrium.. • Functional layer – the upper layer, thick with blood vessels in the first half of menstrual cycle. This layer is shed if no fertilised egg present. • Basal layer – lies next to myometrium, is not shed, but fresh functional layer is regenerated from here during each menstrual cycle. (c) Eleshia Howell, 2012.
Blood Supply, Lymph Drainage & Nerve Supply are essentially the same as the vagina • The uterus is supported in the pelvic cavity by surrounding organs, muscles of the pelvic floor and ligament that suspend it from the walls of the pelvis. • Broad ligament • Round ligament • Uterosacral ligaments • Transverse cervical • Pubocervical fascia (c) Eleshia Howell, 2012.
Functions of the Uterus: • The menstrual cycle begins at puberty, under hypothalmic and anterior pituitary control, for the purpose of preparing the uterus to receive, nourish and protect a fertilised ovum • If an ovum is fertilised, the zygote embeds itself into the uterine wall, which grows and thickens to protect and nourish the embryo until the placenta is formed. (c) Eleshia Howell, 2012.
During pregnancy, the muscles of the uterus are prevented from contracting by high levels of progesterone, secreted by the placenta. At the end of pregnancy, oestrogen initiates uterine contractions, along with oxytocin, to promote labour (rhythmic contractions that forcefully expel the baby from the uterus, through the birth canal). (c) Eleshia Howell, 2012.
Uterine Tubes • Aka fallopian tubes, are about 10cm long and extend from the sides of the uterus, between the body and the fundus. • They lie in the upper free border of the broad ligament. • Their trumpet-shaped lateral ends end in finger-like projections called fimbriae, the longest of which is in close association with the ovary. (c) Eleshia Howell, 2012.
The tubes have an outer covering of peritoneum (the broad ligament), a middle smooth muscle layer and inner ciliated epithelial layer, bathed in mucous. • Blood, lymph and nerve supply is same as the uterus. • Their function is to move the ovum from ovary to uterus by peristalsis & ciliary movement. Fertilisation often occurs here. (c) Eleshia Howell, 2012.
Ovaries • These are the female gonads (glands producing sex hormones and the ova) • Lay in a shallow fossa on the lateral walls of the pelvis • About 2.5-3.5cm long, 2cm wide and 1cm thick • Each attached to upper part of the uterus by the ovarian ligament and part of the broad ligament known as mesovarium. (c) Eleshia Howell, 2012.
The ovaries have 2 layers of tissue: • Medulla – central portion consisting of fibrous tissue, blood vessels and nerves • Cortex – outer portion; has a framework of connective tissue covered by germinal epithelium. It contains ovarian follicles in various stages of maturity. During each menstrual cycle, one follicle matures, ruptures and releases its ovum into the peritoneal cavity (ovulation). (c) Eleshia Howell, 2012.
Arterial blood supply to the ovaries is via the ovarian arteries, which branch from the abdominal aorta just below the renal arteries • Venous drainage is posterior uterine plexus which drains into the inferior vena cava (R) and left renal vein • Lymph drainage goes into the lateral aortic and pre-aortic nodes • Nerve supply is same as uterus. (c) Eleshia Howell, 2012.
Functions of the Ovary: • The female gametes are developed and stored here • The hypothalamus and ant. Pituitary release gonadotrophins (FSH, LH) to mature and release an ovum • Ovaries also have endocrine functions, releasing hormones essential to the physiological changes during reproductive cycle (oestrogen and progesterone). (c) Eleshia Howell, 2012.
Puberty (female) • The age at which the internal reproductive organs reach maturity, usually between 12 -14 yrs of age ~ known as menarche and marks the beginning of childbearing period. • Menstrual cycle & ovulation begin • Breasts develop & enlarge • Pubic & axillary hair grows • Increase in height and widening of pelvis • Increased fat deposited in subcutaneous tissue, especially around hips and breasts (c) Eleshia Howell, 2012.
Menstrual Cycle • A series of events occurring regularly every 26-30 days throughout childbearing period of approx 36yrs. • The cycle consists of a series of changes taking place concurrently in the ovaries and uterine walls, stimulated by changes in blood hormone concentrations, all regulated by negative feedback mechanisms. (c) Eleshia Howell, 2012.
Menstrual Phase: • If an ovum is unfertilised, progesterone and oestrogen levels drop and the functional layer of the endometrium is shed. • Menstrual flow consists of endometrial cells, blood from the degenerating capillaries, secretions from the endometrial glands, and the unfertilised ovum. • oestrogen & progesterone stimulates FSH and LH levels and the next phase of cycle (c) Eleshia Howell, 2012.
Proliferative Phase: • An ovarian follicle is maturing, producing oestrogen, stimulating proliferation of the functional layer if the endometrium. • Endometrium thickens, becoming more vascular and rich in mucus secreting glands. • A surge in LH approx mid-cycle triggers ovulation. (c) Eleshia Howell, 2012.
Secretory Phase: • After ovulation, the ruptured follicle stimulates increased amounts of progesterone which causes the endometrium to become oedematous and the secretory glands produce increased amounts of watery mucous (believed to assist the passage of sperm through the uterus). There is a similar increase to mucous secretions in the tubes and cervical glands that lubricate vagina. (c) Eleshia Howell, 2012.
The period in which fertilisation can occur is relatively short ~ the ovum may only survive for about 8hrs and the capability of sperm fertilising the ovum may only be 24hrs (even though the sperm might survive for a number of days). • If the ovum is not fertilised, menstruation occurs and the cycle begins anew. (c) Eleshia Howell, 2012.
Observable changes that occur around the time of ovulation include: • Cervical mucous becomes thin, watery & elastic • Body temperature rises by a small amount • Abdominal discomfort • Breast engorgement / discomfort / sensitivity • Fluid retention • Mood / emotional fluctuations (c) Eleshia Howell, 2012.
Menopause • Usually occurs between 45-55 yrs of age, marking the end of childbearing period. • May occur suddenly or over a period of years, sometimes as long as 10yrs • Caused by a reduction in oestrogen levels as the number of functional ovarian follicles declines with age. Ovaries gradually become less responsive to gonadotrophins and ovulation & menstrual cycle eventually cease (c) Eleshia Howell, 2012.
Changes associated with menopause include: • Short term unpredictable vasodilation with flushing, sweating & palpitations • Shrinkage of the breasts • Axillary & pubic hair become sparse • Atrophy of the sex organs • Mood changes, irritability • Gradual thinning of skin • Loss of bone mass • Slow increase in blood cholesterol levels (c) Eleshia Howell, 2012.