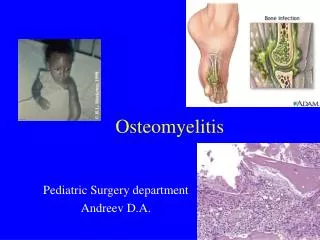
Microbiology of Vertebral Osteomyelitis and Implications on Empiric Therapy
Microbiology of Vertebral Osteomyelitis and Implications on Empiric Therapy. Abbye Clark, BS University of South Carolina School of Medicine. IDweek 2017 Abstract #65531. Disclosures. The authors have no financial disclosures. Background.

Microbiology of Vertebral Osteomyelitis and Implications on Empiric Therapy
E N D
Presentation Transcript
Microbiology of Vertebral Osteomyelitis and Implications on Empiric Therapy Abbye Clark, BS University of South Carolina School of Medicine IDweek 2017 Abstract #65531
Disclosures • The authors have no financial disclosures
Background • Common organisms implicated in vertebral osteomyelitis (VO) include: • Staphylococcus aureus, coagulase-negative Staphylococcusspp., Streptococcusspp., and Enterobacteriaceae • The management of VO includes empiric antibiotics while clinical cultures are being processed • McHenry MC. Clin Infect Dis. 2002 • Weissman S. Scand J Infect Dis. 2014 • Gouliouris TJ. AntimicrobChemother 2010 • Berbari EF. Clin Infect Dis. 2015
Aims of Study • Develop institutional guidelines for empiric therapy of VO based on: • Local epidemiology and microbiology • Risk factors for VO due to gram-negative bacilli
Methods: Study Design • A retrospective cohort of hospitalized subjects ≥18 years, diagnosed with VO from 08/01/2010 to 08/31/2015 at Palmetto Health hospitals in Columbia, SC, USA • ICD-9 codes corresponding to VO, discitis, spondylodiscitis, paravertebral abscess, and sacroilitis
Methods: Criteria • Inclusion criteria • VO confirmed if 2/3 for the following accompanied ICD-9 code: • Clinical symptoms • Imaging suggestive of VO • Positive cultures from bloodstream or vertebral region biopsy • Exclusion criteria • Absence of VO on chart review • Presence of sacral decubitus ulcer adjacent to VO
Methods: Statistical Analysis • Multivariate logistic regression was used to identify the risk factors of VO due to gram-negativeinfection
Results: Associated Abscesses • 113 (75%) subjects had at least one associated abscess
Results: Microbiology • 121 (81%) subjects had positive cultures
Results: VO with Hardware In Situ • 14 subjects had VO with Hardware In Situ (HAVO) • 12 subjects had positive cultures • 11/12 (92%) were due to gram-positive bacteria
Limitations • Retrospective, single center study • Too few gram-negative bacilli affected power of predictive model • Fewer than recommended number of samples taken at the time of biopsy
Conclusions • Predominance of VO due to gram-positive bacteria (86% overall) • 84% in native VO • 92% in presence of hardware • Cancer, diverticular disease and injection drug use were associated with increased risk of VO due to gram-negative bacilli
Implications for Clinical Practice • IV vancomycin monotherapy may be reasonable for empiric therapy in non-critically ill patients while awaiting Gram stain and clinical culture results • Addition of gram-negative coverage to vancomycin may be justified in critically-ill patients or those with specific risk factors
Acknowledgments Study Team: • Neha Sharma, BS • Sharon Weissman, MD • Majdi Al-Hasan, MD • Caroline Derrick, PharmD • KamlaSanasi-Bhola, MD
Microbiology of Vertebral Osteomyelitis and Implications on Empiric Therapy Questions? Contact: Abbye Clark, BS Abbye.Clark@uscmed.sc.edu