Congestive Heart Failure
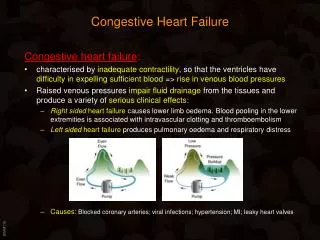
Congestive Heart Failure . Michele Ritter, M.D. Argy – February, 2007. Heart Failure . Results from any structural or functional abnormality that impairs the ability of the ventricle to eject blood ( Systolic Heart Failure ) or to fill with blood ( Diastolic Heart Failure ).

Congestive Heart Failure
E N D
Presentation Transcript
Congestive Heart Failure Michele Ritter, M.D. Argy – February, 2007
Heart Failure • Results from any structural or functional abnormality that impairs the ability of the ventricle to eject blood (Systolic Heart Failure) or to fill with blood (Diastolic Heart Failure).
Types of Heart Failure • Low-Output Heart Failure • Systolic Heart Failure: • decreased cardiac output • Decreased Left ventricular ejection fraction • Diastolic Heart Failure: • Elevated Left and Right ventricular end-diastolic pressures • May have normal LVEF • High-Output Heart Failure • Seen with peripheral shunting, low-systemic vascular resistance, hyperthryoidism, beri-beri, carcinoid, anemia • Often have normal cardiac output • Right-Ventricular Failure • Seen with pulmonary hypertension, large RV infarctions.
Causes of Low-Output Heart Failure • Systolic Dysfunction • Coronary Artery Disease • Idiopathic dilated cardiomyopathy (DCM) • 50% idiopathic (at least 25% familial) • 9 % mycoarditis (viral) • Ischemic heart disease, perpartum, hypertension, HIV, connective tissue disease, substance abuse, doxorubicin • Hypertension • Valvular Heart Disease • Diastolic Dysfunction • Hypertension • Coronary artery disease • Hypertrophic obstructive cardiomyopathy (HCM) • Restrictive cardiomyopathy
Clinical Presentation of Heart Failure • Due to excess fluid accumulation: • Dyspnea (most sensitive symptom) • Edema • Hepatic congestion • Ascites • Orthopnea, Paroxysmal Nocturnal Dyspnea (PND) • Due to reduction in cardiac ouput: • Fatigue (especially with exertion( • Weakness
Physical Examination in Heart Failure • S3 gallop • Low sensitivity, but highly specific • Cool, pale, cyanotic extremities • Have sinus tachycardia, diaphoresis and peripheral vasoconstriction • Crackles or decreased breath sounds at bases (effusions) on lung exam • Elevated jugular venous pressure • Lower extremity edema • Ascites • Hepatomegaly • Splenomegaly • Displaced PMI • Apical impulse that is laterally displaced past the midclavicular line is usually indicative of left ventricular enlargement>
Lab Analysis in Heart Failure • CBC • Since anemia can exacerbate heart failure • Serum electrolytes and creatinine • before starting high dose diuretics • Fasting Blood glucose • To evaluate for possible diabetes mellitus • Thyroid function tests • Since thyrotoxicosis can result in A. Fib, and hypothyroidism can results in HF. • Iron studies • To screen for hereditary hemochromatosis as cause of heart failure. • ANA • To evaluate for possible lupus • Viral studies • If viral mycocarditis suspected
Laboratory Analysis (cont.) • BNP • With chronic heart failure, atrial mycotes secrete increase amounts of atrial natriuretic peptide (ANP) and brain natriuretic pepetide (BNP) in response to high atrial and ventricular filling pressures • Usually is > 400 pg/mL in patients with dyspnea due to heart failure.
Chest X-ray in Heart Failure • Cardiomegaly • Cephalization of the pulmonary vessels • Kerley B-lines • Pleural effusions
Cardiac Testing in Heart Failure • Electrocardiogram: • May show specific cause of heart failure: • Ischemic heart disease • Dilated cardiomyopathy: first degree AV block, LBBB, Left anterior fascicular block • Amyloidosis: pseudo-infarction pattern • Idiopathic dilated cardiomyopathy: LVH • Echocardiogram: • Left ventricular ejection fraction • Structural/valvular abnormalities
Further Cardiac Testing in Heart Failure • Exercise Testing • Should be part of initial evaluation of all patients with CHF. • Coronary arteriography • Should be performed in patients presenting with heart failure who have angina or significant ischemia • Reasonable in patients who have chest pain that may or may not be cardiac in origin, in whom cardiac anatomy is not known, and in patients with known or suspected coronary artery disease who do not have angina. • Measure cardiac output, degree of left ventricular dysfunction, and left ventricular end-diastolic pressure.
Further testing in Heart Failure • Endomyocardial biopsy • Not frequently used • Really only useful in cases such as viral-induced cardiomyopathy
Classification of Heart Failure • New York Heart Association (NYHA) • Class I – symptoms of HF only at levels that would limit normal individuals. • Class II – symptoms of HF with ordinary exertion • Class III – symptoms of HF on less than ordinary exertion • Class IV – symptoms of HF at rest
Classification of Heart Failure (cont.) • ACC/AHA Guidelines • Stage A – High risk of HF, without structural heart disease or symptoms • Stage B – Heart disease with asymptomatic left ventricular dysfunction • Stage C – Prior or current symptoms of HF • Stage D – Advanced heart disease and severely symptomatic or refractory HF
Chronic Treatment of Systolic Heart Failure • Correction of systemic factors • Thyroid dysfunction • Infections • Uncontrolled diabetes • Hypertension • Lifestyle modification • Lower salt intake • Alcohol cessation • Medication compliance • Maximize medications • Discontinue drugs that may contribute to heart failure (NSAIDS, antiarrhythmics, calcium channel blockers)
Order of Therapy • Loop diuretics • ACE inhibitor (or ARB if not tolerated) • Beta blockers • Digoxin • Hydralazine, Nitrate • Potassium sparing diuretcs
Diuretics • Loop diuretics • Furosemide, buteminide • For Fluid control, and to help relieve symptoms • Potassium-sparing diuretics • Spironolactone, eplerenone • Help enhance diuresis • Maintain potassium • Shown to improve survival in CHF
ACE Inhibitor • Improve survival in patients with all severities of heart failure. • Begin therapy low and titrate up as possible: • Enalapril – 2.5 mg po BID • Captopril – 6.25 mg po TID • Lisinopril – 5 mg po QDaily • If cannot tolerate, may try ARB
Beta Blocker therapy • Certain Beta blockers (carvedilol, metoprolol, bisoprolol) can improve overall and event free survival in NYHA class II to III HF, probably in class IV. • Contraindicated: • Heart rate <60 bpm • Symptomatic bradycardia • Signs of peripheral hypoperfusion • COPD, asthma • PR interval > 0.24 sec, 2nd or 3rd degree block
Hydralazine plus Nitrates • Dosing: • Hydralazine • Started at 25 mg po TID, titrated up to 100 mg po TID • Isosorbide dinitrate • Started at 40 mg po TID/QID • Decreased mortality, lower rates of hospitalization, and improvement in quality of life.
Digoxin • Given to patients with HF to control symptoms such as fatigue, dyspnea, exercise intolerance • Shown to significantly reduce hospitalization for heart failure, but no benefit in terms of overall mortality.
Other important medication in Heart Failure -- Statins • Statin therapy is recommended in CHF for the secondary prevention of cardiovascular disease. • Some studies have shown a possible benefit specifically in HF with statin therapy • Improved LVEF • Reversal of ventricular remodeling • Reduction in inflammatory markers (CRP, IL-6, TNF-alphaII)
Meds to AVOID in heart failure • NSAIDS • Can cause worsening of preexisting HF • Thiazolidinediones • Include rosiglitazone (Avandia), and pioglitazone (Actos) • Cause fluid retention that can exacerbate HF • Metformin • People with HF who take it are at increased risk of potentially lethic lactic acidosis
Implantable Cardioverter-Defibrillators for HF • Sustained ventricular tachycardia is associated with sudden cardiac death in HF. • About one-third of mortality in HF is due to sudden cardiac death. • Patients with ischemic or nonischemic cardiomyopathy, NYHA class II to III HF, and LVEF ≤ 35% have a significant survival benefit from an implantable cardioverter-defibrillator (ICD) for the primary prevention of SCD.
Management of Refractory Heart Failure • Inotropic drugs: • Dobutamine, dopamine, milrinone, nitroprusside, nitroglycerin • Mechanical circulatory support: • Intraaortic balloon pump • Left ventricular assist device (LVAD) • Cardiac Transplantation • A history of multiple hospitalizations for HF • Escalation in the intensity of medical therapy • A reproducable peak oxygen consumption with maximal exercise (VO2max) of < 14 mL/kgper min. (normal is 20 mL/kg per min. or more) is relative indication, while a VO2max < 10 mL/kg per min is a stronger indication.
Acute Decompensated Heart Failure • Cardiogenic pulmonary edema is a common and sometimes fatal cause of acute respiratory distress. • Characterized by the transudation of excess fluid into the lungs secondary to an increase in left atrial and subsequently pulmonary venous and pulmonary capillary pressures.
Acute Decompensaated Heart Failure (cont.) • Causes: • Acute MI • Rupture of chordae tendinae/acute mitral valve insufficiency • Volume Overload • Transfusions, IV fluids • Non-compliance with diuretics, diet (high salt intake) • Worsening valvular defect • Aortic stenosis
Decompensated Heart Failure • Symptoms • Severe dyspnea • Cough • Clinical Findings • Tachypnea • Tachycardia • Hypertension/Hypotension • Crackles on lung exam • Increased JVD • S3, S4 or new murmur
Labs/Studies in Acute Decompensated Heart Failure • Chemistry, CBC • EKG • Chest X-ray • May consider cardiac enzymes • 2D-Echo
Decompensated Heart Failure • Treatment • Strict I’s and O’s, daily weights • Oxygen, mechanical ventilation if needed • Loop diuretics (Lasix!) • Morphine • Vasodilator therapy (nitroglycerin) • Nesiritide (BNP) – can help in acute setting, for short term therapy
Case # 1 • A 65-year old male with a history of hypertension, DM, CAD s/p MI and three-vessel CABG in 2002, presents with worsening dyspnea on exertion. He states that he occassionally has a dry cough, but denies any recent chest pain, fevers, N/V. Patient states that he usually can get up a flight of stairs if he stops half-way, but over the last several days, has not been able to climb them at all.
Case # 1 (cont.) • PMH: • CAD – MI and CABG in 2002 • Hypertension • Diabetes Mellitus • Hypothyroidism • Allergies: • NKDA • Outpatient Meds: • Synthroid • Metformin • Norvasc
Case # 1 (cont.) • Physical Exam: • 97.6, 168/72, 99, 28, 93% on RA • Gen: Alert and oriented x 3, breathing rapidly • CV: RRR, no murmurs; mod. JVD • Resp: Crackles throughout lungs • Abd.: soft, nontender, NABS • Ext: 2 + pitting edema bilaterally
Labs: Hgb: 13.5 WBC: 8 Platelets: 240 Sodium: 139 Potassium: 3.8 BUN: 18 Cr: 0.8 Trop. I – 0.01 CPK: 120 Case # 1 (cont.)
Case # 1 • What studies would you like to check in this patient? • What medications would you like to start/change? • What vital signs do you want to monitor?
Case # 2 • A 45-year old obese woman with diabetes mellitus is evaluated for a 1-month history of progressive shortness of breath. Two months ago, she had a flu-like illness with nausea, vomiting, and sweating. She has not followed up with a physician regularly. One of her siblings has “heart problems” and her mother died suddenly and unexpectedly at age 55 years.
Case # 2 • On examination her heart rate is 75/min and her blood pressure is 185/93 mm Hg. BMI is 32.9. Jugular venous pressure is mildly elevated. Lung examination reveals a few bibasilar crackles. Cardiac examination reveals regular rhythm, normal S1 and S2 and the presence of an S3. There is mild peripheral edema. An echocardiogram is significant for left ventricular hypertrophy and severely decreased systolic function (left ventricular ejection fraction, 20%) An electrocardiogram shows a previous anteroseptal MI.
Case # 2 • Which of the following is the most appropriate next diagnostic test? • Measurement of plasma BNP • Serum Protein Electrophoresis • Cardiac Stress Test • Cardiac catheterization • Endomyocardial biopsy