Blood
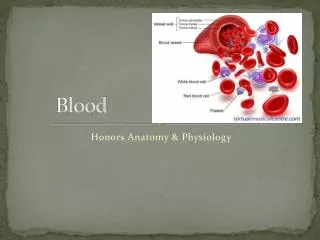
Blood. Introduction. Blood, a type of connective tissue, is a complex mixture of cells, chemicals, and fluid. Blood transports substances throughout the body, and helps to maintain a stable internal environment. The blood includes red blood cells, white blood cells, platelets, and plasma.

Blood
E N D
Presentation Transcript
Introduction • Blood, a type of connective tissue, is a complex mixture of cells, chemicals, and fluid. • Blood transports substances throughout the body, and helps to maintain a stable internal environment. • The blood includes red blood cells, white blood cells, platelets, and plasma.
Red Blood Cells • Red blood cells (erythrocytes) are biconcave disks that contain one-third oxygen-carrying hemoglobin by volume. • When oxygen combines with hemoglobin bright red oxyhemoglobin results. • Deoxygenated blood (deoxyhemoglobin) is darker. • RBCs discard their nuclei during development and so cannot reproduce or produce proteins.
RBC Production, Control & Counts • Red blood cell production occurs in the red bone marrow after birth. • The average life span of a red blood cell is 120 days. • The number of RBCs is a measure of the blood’s oxygen-carrying capacity.
Dietary Factors Affecting RBC Production • Vitamins B12 and folic acid are needed for DNA synthesis, so they are necessary for the reproduction of all body cells • Iron is needed for hemoglobin synthesis. • A deficiency in red blood cells or quantity of hemoglobin results in anemia.
White Blood Cells • White blood cells (leukocytes) help defend the body against disease. • Five types of WBCs are in circulating blood and are distinguished by size, granular appearance of the cytoplasm, shape of the nucleus, and staining characteristics. • The types of WBCs are the granular neutrophils, eosinophils, and basophils, and the agranular monocytes and lymphocytes.
Functions of White Blood Cells • Neutrophils and monocytes are phagocytic, with monocytes engulfing the larger particles. • Eosinophils moderate allergic reactions as well as defend against parasitic infections. • Basophils migrate to damaged tissues and release histamine to promote inflammation and heparin to inhibit blood clotting. • Lymphocytes are the major players in specific immune reactions and some produce antibodies.
White Blood Cell Counts • A differential WBC count can help pinpoint the nature of an illness, indicating whether it is caused by bacteria or viruses. • Leukocytosis occurs after an infection when excess numbers of leukocytes are present; leukopenia occurs from a variety of conditions, including AIDS.
Blood Plateletes • Platelets help repair damaged blood vessels by adhering to their broken edges.
Blood Plasma • Plasma is the clear, straw-colored fluid portion of the blood. • Plasma is mostly water but contains a variety of substances. • Plasma functions to transport nutrients and gases, regulate fluid and electrolyte balance, and maintain a favorable pH.
Blood Plasma – Gases & Nutrients • The most important blood gases are oxygen and carbon dioxide. • The plasma nutrients include amino acids, monosaccharides, nucleotides, and lipids.
Plasma Electrolytes • Plasma electrolytes are absorbed by the intestine or are by-products of cellular metabolism. • They include sodium, potassium, calcium, magnesium, chloride, bicarbonate, phosphate, and sulfate ions. • Some of these ions are important in maintaining osmotic pressure and pH of the plasma.
Hemostasis • Hemostasis refers to the stoppage of bleeding. • Following injury to a vessel, three steps occur in hemostasis: blood vessel spasm, platelet plug formation, and blood coagulation.
Blood Coagulation • Once a blood clot forms, it promotes still more clotting through a positive feedback system. • After a clot forms, fibroblasts invade the area and produce fibers throughout the clots. • A clot that forms abnormally in a vessel is a thrombus; if it dislodges, it is an embolus.
Blood Groups and Transfusions • After mixed success with transfusions, scientists determined that blood was of different types and only certain combinations were compatible.
Antigens and Antibodies • Clumping of red blood cells following transfusion is called agglutination. • Agglutination is due to the interaction of proteins on the surfaces of red blood cells (antigens) with certain antibodies carried in the plasma. • Only a few of the antigens on red blood cells produce transfusion reactions. • These include the ABO group and Rh group.
ABO Blood Group • Type A blood has A antigens on red blood cells and anti-B antibodies in the plasma. • Type B blood has B antigens on red blood cells and anti-A antibodies in the plasma. • Type AB blood has both A and B antigens, but no antibodies in the plasma. • Type O blood has neither antigen, but both types of antibodies in the plasma.
ABO Blood Group Cont. • Adverse transfusion reactions are avoided by preventing the mixing of blood that contains matching antigens and antibodies. • Adverse reactions are due to the agglutination of red blood cells.
Rh Blood Group • The Rh factor was named after the rhesus monkey. • If the Rh factor surface protein is present on red blood cells, the blood is Rh positive; otherwise it is Rh negative. • There are no corresponding antibodies in the plasma unless a person with Rh- negative blood is transfused with Rh- positive blood; the person will then develop antibodies for the Rh factor. • Erythroblastosis fetalis develops in Rh- positive fetuses of Rh-negative mothers but can now be prevented.
Introduction • The cardiovascular system consists of the heart, and vessels, arteries, capillaries and veins. • A functional cardiovascular system is vital for supplying oxygen and nutrients to tissues and removing wastes from them.
Structure of the Heart • The heart is a hollow, cone-shaped, muscular pump within the thoracic cavity. • Size and Location of the Heart • The average adult heart is 14 cm long and 9 cm wide. • The heart lies in the mediastinum under the sternum; its apex extends to the fifth intercostal space. • The pericardium encloses the heart.
Wall of the Heart • The wall of the heart is composed of three distinct layers. • The outermost layer, the epicardium, is made up of connective tissue and epithelium; it houses capillaries along with coronary arteries. It is the same as the visceral pericardium. • The middle layer called myocardium consists of cardiac muscle and is the thickest layer of the heart wall. • The inner endocardium is smooth and is made up of connective tissue and epithelium, and is continuous with the endothelium of major vessels joining the heart.
Heart Chambers and Valves • The heart has four internal chambers: two atria on top and two ventricles below. • Atria receive blood returning to the heart and have thin walls and ear-like auricles projecting from their exterior. • The thick-muscled ventricles pump blood to the body.
Heart Chambers and Valves cont. • A septum divides the atrium and ventricle on each side. Each also has an atrioventricular (A-V) valve to ensure one way flow of blood. • The right A-V valve (tricuspid) and left A-V valve (bicuspid or mitral valve) have cusps to which chordae tendinae attach. • Chordae tendinae are, in turn, attached to papillary muscles in the inner heart wall that contract during ventricular contraction to prevent the backflow of blood through the A-V valves.
Heart Chambers and Valves cont. • The superior and inferior vena cavae bring de-oxygenated blood from the body to the right atrium. • The right ventricle has a thinner wall than does the left ventricle because it must pump blood only as far as the lungs, compared to the left ventricle pumping to the entire body.
Heart Chambers and Valves cont. • At the base of the pulmonary trunk leading to the lungs is the pulmonary valve, which prevents a return flow of blood to the ventricle. • The left atrium receives blood from four pulmonary veins. • The left ventricle pumps blood into the entire body through the aorta, guarded by the aortic valve that prevents backflow of blood into the ventricle.
Path of Blood through the Heart • Blood low in oxygen returns to the right atrium via the venae cavae and coronary sinus. • The right atrium contracts, forcing blood through the tricuspid valve into the right ventricle.
Path of Blood through the Heart • The right ventricle contracts, closing the tricuspid valve, and forcing blood through the pulmonary valve into the pulmonary trunk and arteries. • The pulmonary arteries carry blood to the lungs where it can rid itself of excess carbon dioxide and pick up a new supply of oxygen.
Path of Blood through the Heart • Freshly oxygenated blood is returned to the left atrium of the heart through the pulmonary veins. • The left atrium contracts, forcing blood through the left bicuspid valve into the left ventricle. • The left ventricle contracts, closing the bicuspid valve and forcing open the aortic valve as blood enters the aorta for distribution to the body.
Blood Supply to the Heart • The first branches off of the aorta, which carry freshly oxygenated blood, are the right and left coronary arteries that feed the heart muscle itself. • Branches of the coronary arteries feed many capillaries of the myocardium.
Blood Supply to the Heart cont. • The heart muscle requires a continuous supply of freshly oxygenated blood, so smaller branches of arteries often have anastomoses as alternate pathways for blood, should one pathway become blocked. • Cardiac veins drain blood from the heart muscle and carry it to the coronary sinus, which empties into the right atrium.
Heart Actions • The cardiac cycle consists of the atria beating in unison (atrial systole) followed by the contraction of both ventricles, (ventricular systole) then the entire heart relaxes for a brief moment (diastole).
Cardiac Cycle • During the cardiac cycle, pressure within the heart chambers rises and falls with the contraction and relaxation of atria and ventricles. • When the atria fill, pressure in the atria is greater than that of the ventricles, which forces the A-V valves open. • Pressure inside atria rises further as they contract, forcing the remaining blood into the ventricles.
Cardiac Cycle cont. • When ventricles contract, pressure inside them increases sharply, causing A-V valves to close and the aortic and pulmonary valves to open. • As the ventricles contract, papillary muscles contract, pulling on chordae tendinae and preventing the backflow of blood through the A-V valves.
Heart Sounds • Heart sounds are due to vibrations in heart tissues as blood rapidly changes velocity within the heart. • Heart sounds can be described as a "lubb-dupp" sound. • The first sound (lubb) occurs as ventricles contract and A-V valves are closing. • The second sound (dupp) occurs as ventricles relax and aortic and pulmonary valves are closing.
Blood Vessels • The blood vessels (arteries, arterioles, capillaries, venules, and veins) form a closed tube that carries blood away from the heart, to the cells, and back again.
Arteries and Arterioles • Arteries are strong, elastic vessels adapted for carrying high-pressure blood. • Arteries become smaller as they divide and give rise to arterioles. • The wall of an artery consists of smooth muscle and connective tissue. • Arteries are capable of vasoconstriction as directed by the sympathetic impulses; when impulses are inhibited, vasodilation results.