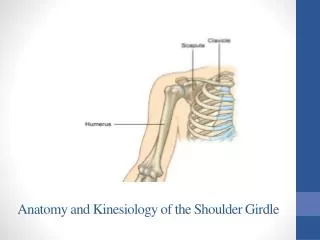
Chapter 22: The Shoulder Complex
Chapter 22: The Shoulder Complex. Jennifer Doherty-Restrepo, MS, LAT, ATC Academic Program Director, Entry-Level ATEP Florida International University Acute Care and Injury Prevention. Introduction. The shoulder is an extremely complicated region of the body


Chapter 22: The Shoulder Complex
E N D
Presentation Transcript
Chapter 22: The Shoulder Complex Jennifer Doherty-Restrepo, MS, LAT, ATC Academic Program Director, Entry-Level ATEP Florida International University Acute Care and Injury Prevention
Introduction • The shoulder is an extremely complicated region of the body • Joint with a high degree of mobility, but, not without compromising stability • Involved in a variety of overhead activities relative to sport • Susceptible to a number of repetitive and overused type injuries
Functional Anatomy • Great mobility, limited stability • Round humeral head articulates with flat glenoid • Rotator cuff and long head of the biceps provide dynamic stability during overhead motion • Supraspinatus compresses the humeral head • Other rotator cuff muscles depress the humeral head Integration of the capsule and rotator cuff • Scapula stabilizing muscles also provide dynamic stability • Relationship with the other joints of the shoulder complex and the G-H joint is critical
Prevention of Shoulder Injuries • Proper physical conditioning is key • Sport-specific conditioning • Strengthen through a full ROM • Warm-up should be used before explosive arm movements are attempted • Contact and collision sport athletes should receive proper instruction on falling • Protective equipment • Proper mechanics
Specific Injuries • Clavicular Fractures • Etiology • MOI = fall on outstretched arm, fall on tip of shoulder, or direct impact • Occurs primarily in middle third • Signs and Symptoms • Athlete supports arm, head tilted towards injured side with chin turned away • Clavicle may appear lower • Palpation reveals pain, swelling, deformity, and point tenderness
Clavicular Fractures (continued) • Management • Closed reduction - sling and swathe immediately • Refer for X-ray • Immobilize with brace for 6-8 weeks • After removal of brace, rehabilitation includes: • Joint mobilizations • Isometric exercises • Use of a sling for 3-4 weeks • May require surgical treatment
Specific Injuries • Scapular Fractures • Etiology • MOI = direct impact or force transmitted up through humerus • Signs and Symptoms • Pain during shoulder movement • Swelling and point tenderness • Management • Sling immediately and refer for X-ray • Use sling for 3 weeks then begin PRE exercises
Specific Injuries • Fractures of the Humerus • Etiology • MOI = direct impact, force transmitted up through humerus, or fall on outstretched arm • Proximal fractures occur due to direct blow • Dislocations occur due to fall on outstretched arm • Epiphyseal fractures are more common in young athletes and occur due to direct blow or indirect blow traveling along long axis of humerus
Specific Injuries • Fractures of the Humerus (continued) • Signs and Symptoms • Pain, swelling, point tenderness, decreased ROM • Management • Immediate application of splint • Refer for X-ray • Treat for shock
Specific Injuries • Acromioclavicular Sprain • Etiology • MOI = direct blow (from any direction) or upward force from the humerus • Graded from 1 - 6 according to severity of injury • Signs and Symptoms • Grade 1 - point tenderness, pain with movement • No disruption of AC joint • Grade 2 - tear or rupture of AC ligament, pain, point tenderness, and decreased ROM (abd/add) • Partial displacement of lateral end of clavicle
Acromioclavicular Sprain (continued) • Signs and Symptoms • Grade 3 - rupture of AC and CC ligaments • AC joint separation • Grade 4 - posterior dislocation of clavicle • Grade 5 – rupture of AC and CC ligaments, tearing of deltoid and trapezius attachments, gross deformity, severe pain, decreased ROM • Grade 6 - displacement of clavicle behind the coracobrachialis
Acromioclavicular Sprain (continued) • Management • Ice, sling and swathe • Referral to physician • Grades 1 – 3: non-operative treatment • 1 - 2 weeks of immobilization • Grades 4 – 6: surgery required • Aggressive rehab is required for all AC sprains • Joint mobilizations, flexibility exercises, and PRE exercises should occur immediately • Progress as tolerated – no pain and no additional swelling • Padding and protection may be required until pain-free ROM returns
A: Grade 1 • B: Grade 2 • C: Grade 3 • D: Grade 4 • E: Grade 5 • F: Grade 6
Specific Injuries • Glenohumeral Joint Sprain • Etiology • MOI = forced abduction and/or external rotation; or a direct blow • Signs and Symptoms • Pain during movement • Especially when re-creating the MOI • Decreased ROM • Point tenderness
Specific Injuries • Glenohumeral Joint Sprain (continued) • Management • RICE for 24-48 hours • Sling • After hemorrhaging subsides, modalities may be utilized along with PROM and AROM exercises to regain full ROM • When full ROM achieved without pain, PRE exercises can be initiated • Must be aware of potential development of chronic conditions (instability)
Specific Injuries • Acute Subluxations and Dislocations • Etiology • Subluxation = excessive translation of humeral head without complete separation from joint • Anterior dislocation = results from an anterior force on the shoulder with forced ABD and ER • Posterior dislocation = results from forced ADD and IR, or, falling on an extended and internally rotated shoulder
Specific Injuries • Acute Subluxations and Dislocations (continued) • Signs and Symptoms • Anterior dislocation - flattened deltoid; prominent humeral head in axilla; arm carried in slight ABD and ER rotation; moderate pain and disability • Posterior dislocation - severe pain and disability; arm carried in ADD and IR; prominent acromion and coracoid process; limited ER and elevation
Acute Subluxations and Dislocations (continued) • Management • Sling and swathe and refer for reduction • Immobilize for 3 weeks following reduction • Perform isometrics while in sling • After immobilization period, begin PRE exercises as pain allows • Protective bracing when return to play
Specific Injuries • Shoulder Impingement Syndrome • Etiology • Mechanical compression of supraspinatus tendon, subacromial bursa, and long head of biceps tendon due to decreased space under coracoacromial arch • MOI = overhead repetitive activities • Exacerbating factors • Laxity and inflammation • Postural mal-alignments • Kyphosis and/or rounded shoulders
Shoulder Impingement Syndrome (continued) • Signs and Symptoms • Diffuse pain • Increased pain with palpation of subacromial space • Decreased strength of external rotators compared to internal rotators • Tightness in posterior and inferior capsule • Positive impingement and empty can tests
Specific Injuries • Rotator cuff tear • Etiology • Occurs near insertion on greater tuberosity • Involve supraspinatus or rupture of other rotator cuff tendons • Partial or complete thickness tear • Full thickness tears usually occur in athletes with a long history of rotator cuff pathology • Generally does not occur in athlete under age 40 • MOI = acute trauma or impingement • Signs and Symptoms • Pain and weakness with shoulder ABD and IR • Point tenderness
Rotator cuff tear (continued) • Management • NSAID’s and analgesics • Modalities • Electrical stimulation for pain • Ultrasound for inflammation • Restore appropriate mechanics by strengthening rotator cuff to depress and compress humeral head to restore subacromial space • Severe cases may require rest, immobilization, and surgery
Specific Injuries • Thoracic Outlet Compression • Etiology • Compression of brachial plexus, subclavian artery and vein • Due to • 1) decreased space between clavicle and first rib, • 2) scalene compression, • 3) compression by pectoralis minor, or • 4) presence of cervical rib
Thoracic Outlet Compression (continued) • Signs and Symptoms • Paresthesia, pain, sensation of cold, impaired circulation, muscle weakness, muscle atrophy, and radial nerve palsy • Positive anterior scalene test, costoclavicular test, and hyperabduction test • Management • Conservative treatment - correct anatomical condition through stretching (pec minor and scalenes) and strengthening (trapezius, rhomboids, serratus anterior, erector spinae)
Specific Injuries • Biceps Brachii Rupture • Etiology • Generally occurs near origin of muscle at bicipital groove • MOI = powerful contraction
Biceps Brachii Rupture (continued) • Signs and Symptoms • Audible snap with sudden and intense pain • Protruding bulge may appear near middle of biceps • Weakness with elbow flexion and supination • Management • Ice for hemorrhaging • Immobilize with a sling and refer to physician • Athletes will require surgery
Specific Injuries • Bicipital Tenosynovitis • Etiology • Ballistic activity involves repeated stretching of biceps tendon causing irritation to the tendon and sheath • MOI = repetitive overhead activities • Signs and Symptoms • Point tenderness over bicipital groove • Swelling, crepitus due to inflammation • Pain when performing overhead activities
Bicipital Tenosynovitis (continued) • Management • Rest, ice, and ultrasound to treat inflammation • NSAID’s • Gradual program of strengthening and stretching
Specific Injuries • Contusion of Upper Arm • Etiology • MOI = Direct blow • Signs and Symptoms • Transitory paralysis and decreased ROM • Management • RICE for at least 24 hours • Provide protection to prevent repeated episodes that could cause myositis ossificans • Maintain ROM
Rehabilitation of the Shoulder • Immobilization • Will vary depending on injury • Time in brace or splint are injury specific • Isometrics can be performed • ROM and strengthening are dictated by healing • General Body Conditioning • Maintain cardiovascular endurance through cycling, running, and walking