Chapter 28: Skin Disorders
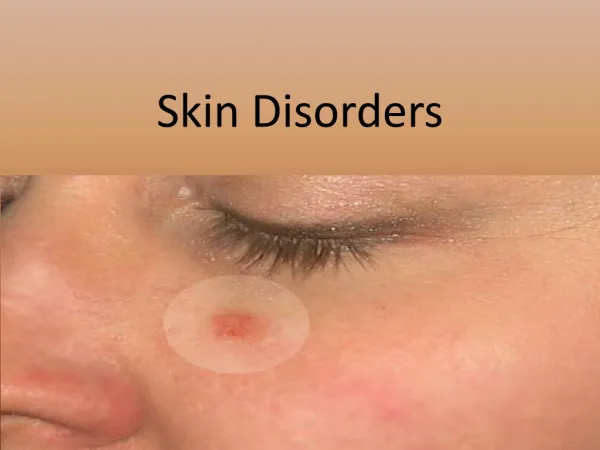
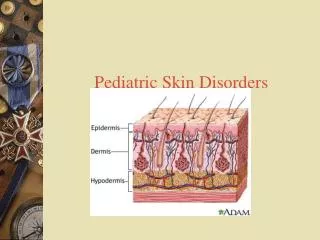
Chapter 28: Skin Disorders. Figure 28-1. Skin Lesions Defined. Skin pigment - melanin Variations may be due to anatomic, physiologic or pathophysiologic changes in skin blood flow Normal skin appearance Altered by external and internal factors Cellulitis

Chapter 28: Skin Disorders
E N D
Presentation Transcript
Chapter 28: Skin Disorders © 2011 McGraw-Hill Higher Education. All rights reserved.
Figure 28-1 © 2011 McGraw-Hill Higher Education. All rights reserved.
Skin Lesions Defined • Skin pigment - melanin • Variations may be due to anatomic, physiologic or pathophysiologic changes in skin blood flow • Normal skin appearance • Altered by external and internal factors • Cellulitis • Infectious inflammation of deep skin structures © 2011 McGraw-Hill Higher Education. All rights reserved.
Figure 28-3 © 2011 McGraw-Hill Higher Education. All rights reserved.
Figure 28-4 © 2011 McGraw-Hill Higher Education. All rights reserved.
Skin Trauma • Mechanical Forces that Cause Injury • Friction • Compression • Shearing • Stretching • Scraping • Tearing • Avulsing • Puncturing © 2011 McGraw-Hill Higher Education. All rights reserved.
Friction and Pressure Problems • Hyperkeratosis of the Hands and Feet • Etiology • Friction and pressure over bony protuberances • Painful when subcutaneous fat becomes inelastic • Sign and Symptoms • Thickening, of horny layer of skin, ovular, elongated and brown • Painful with pressure © 2011 McGraw-Hill Higher Education. All rights reserved.
Management • Avoid emery boards and pumice as the increase in friction will stimulate skin to produce added callus • Use moisturizer • Pair off callus with scalpel • Padding • Prevention • Cushioning devices; wearing 2 socks • Lubricants to reduce friction, shaving calluses • For calluses on hands, special gloves or protective gear © 2011 McGraw-Hill Higher Education. All rights reserved.
Blisters • Etiology • Result of a shearing force that produces a raised area that accumulates with fluid • Signs and Symptoms • Hot spot, sharp burning sensation, painful • Superficial area of skin raised with clear fluid • Prevention • Use of dust or powder or lubricant to reduce friction • Tubular socks, 2 pairs of socks if feet are sensitive or perspire excessively • Appropriate shoes that are broken in • Padding and lubricants © 2011 McGraw-Hill Higher Education. All rights reserved.
Management (intact blister) • Leave intact for 24 hours • Clean with antiseptic • Cut small incision to drain fluid (large enough that it won’t re-seal) • Note in some states this is considered a surgical technique, placing ATC in violation of certain practice acts • Prevent refilling with a pressure pad • Clean again with antiseptic • Use doughnut to prevent irritation • Monitor for infection, replace wet bandaging • Debridement can be performed when tenderness is gone © 2011 McGraw-Hill Higher Education. All rights reserved.
Management (open/torn blister) • Keep clean to avoid infection • Keep skin in place and apply non-adhering sterile dressing and padding • Monitor daily for infection • Management (denuded blister) • If blister is torn 1/2 inch or more remove skin flap • Clean and expose area, apply antiseptic with occlusive dressing • Second skin can be applied to raw area © 2011 McGraw-Hill Higher Education. All rights reserved.
Soft Corns and Hard Corns • Etiology • Caused by pressure of improperly fitting shoes and anatomic abnormalities • Soft corns are the result of pressure and perspiration, also associated with exostosis • Signs and Symptoms • Hard corns form on the tops of toes and tend to be painful and dry • Soft corns result in thickening of skin, white and sometimes painful (between 4th and 5th toes) • Prevention • Wear properly fitting shoes • Management • Surgical removal if painful • Padding; maintain clean dry feet; wear appropriate shoes © 2011 McGraw-Hill Higher Education. All rights reserved.
Excessive Perspiration (hyperhidrosis) • Etiology • Syrup-like perspiration, high in sodium chloride • Increases risk of other skin irritation • Makes adherence of bandages difficulty • Management • Use of astringent such as alcohol or an absorbent powder • Aluminum chloride or electric current can be used to treat condition © 2011 McGraw-Hill Higher Education. All rights reserved.
Chafing of Skin • Etiology • Occurs particularly in patients that are obese or heavy limbed • Result of friction and maceration of skin in climate of heat and moisture • Signs and Symptoms • Separation of keratin from granular layer of skin • Causes oozing wounds that crust and crack • Management • Clean area with soap and water and treat with medicated solution and hydrocortisone cream • Prevention • Keep skin dry, clean, and friction free • For the groin, soft, loose, cotton underwear is recommended © 2011 McGraw-Hill Higher Education. All rights reserved.
Xerotic (Dry) Skin • Etiology • Drying of skin due to exposure of cold, excessive bathing, decrease in humidity causing skin to lose water • Signs and Symptoms • Dry skin w/ variable redness and scaling; itching • Management • Prevent water loss and replace lost water • Bathe in tepid water, use moisturizer • If condition worsens, refer to physician © 2011 McGraw-Hill Higher Education. All rights reserved.
Ingrown Toenails • Etiology • Generally occurs in great toe • Nail grows laterally into skin • Result of lateral pressure from shoes, poor nail trimming, and repeated trauma © 2011 McGraw-Hill Higher Education. All rights reserved.
Signs and Symptoms • Pain and swelling • Penetrated skin becomes inflamed and purulent with lateral nail fold swollen and irritated • Management • Conservative management includes soaking the inflamed toe in warm water (20 minutes) • Place cotton under edge of nail to clear from skin • If chronic, remove wedge of nail and apply antiseptic compress until inflammation resides • Physician may take more aggressive approach • Prevention • Properly fitting shoes and socks are essential • Weekly toenail trimming (cut straight across) • Leave nail long enough to clear skin © 2011 McGraw-Hill Higher Education. All rights reserved.
Wounds • Abrasions • Scraping of skin against rough surface (top surface of skin is worn away) • Increased probability of infection due to exposure of dirt and foreign material • Clean and debride • Punctures • Direct penetration of skin with pointed object • Must be referred to physician © 2011 McGraw-Hill Higher Education. All rights reserved.
Lacerations • Object tears tissue, giving wound appearance of jagged edge (sometimes result of blunt trauma) • Presents environment susceptible to infection • Skin Incision • Smooth cut in skin - not jagged • Skin Avulsion • Skin torn away from body (should be placed in moist gauze w/in a plastic bag that is then immersed in cold water) • Transport to hospital with patient for possible reattachment © 2011 McGraw-Hill Higher Education. All rights reserved.
Skin Bruises • Result of blunt trauma; causes disruption of superficial blood vessels and results in black and blue discoloration • Treatment requires RICE to control hemorrhaging © 2011 McGraw-Hill Higher Education. All rights reserved.
Wound Management • All wounds must be assumed contaminated • Pay close attention to all universal precautions • Clean all wounds with soap and water to minimize infection • Apply a dressing with antiseptic (unless physician examination is necessary) • Lacerations and punctures should be treated by a physician • Use of occlusive dressings • Minimizes scab formation, perceived pain from exposed nerves, cost and time effective, provide adequate barrier • Antibiotic ointment used to prevent secondary infection (SEE TABLE 28-4 for added instruction) © 2011 McGraw-Hill Higher Education. All rights reserved.
If the wound is discharging serum (fluid) to dressing should be changed regularly • When drainage has stopped = no need for dressing • Wound should be cleaned with hydrogen peroxide or Betadine • Effective against bacteria and not harmful to fibroblasts • Antibacterial ointment should be used to limit bacterial growth and to prevent dressing from adhering to wound • Proper care = minimized inflammatory response with quick healing and reduced scarring © 2011 McGraw-Hill Higher Education. All rights reserved.
Suturing • Dependent on severity • Determined by physician • Are underlying tissues exposed or is there significant bleeding? • Should be put in as soon as possible • Within 12 hours following injury • Utilize fine suture material and minimal tightening • Limits additional damage, inflammation and scarring • Large areas or slow healing areas = larger material to be left in longer • Occasionally steri-strips or butterfly bandages will suffice © 2011 McGraw-Hill Higher Education. All rights reserved.
Alternative techniques involves use of skin adhesive/glue • Creates a bond across the wound edges allowing for appropriate healing • Can be used to replace small sutures • Seals out infection • Easy to use, provides water resistant protective coating • Long term cosmetic outcome is comparable to traditional repair methods © 2011 McGraw-Hill Higher Education. All rights reserved.
Athletic Training Clinic Practice in Wound Care • Use clean and sterile instruments • Clean hands thoroughly and use gloves • Sterilize in and around skin lesion • Use a non-medicated covering if athlete is to be sent for medical attention • Utilize butterfly bandage if suture not required • Avoid touching any part of sterile dressings that will contact the wound • Place medication on pad • Secure the dressing in place © 2011 McGraw-Hill Higher Education. All rights reserved.
Bacterial Infections • Bacteria are single celled micro-organisms • Spherical, doublets, and spirochetes • Staphylococcus • Gram positive bacteria that appears in clumps in skin and upper respiratory tract • Streptococcus • Chain bacteria often associated with systemic disease and skin infections • Bacillus • Spore forming, aerobic, and occasionally mobile • Can cause systemic damage © 2011 McGraw-Hill Higher Education. All rights reserved.
Methicillin-Resistant Staphylococcus Aureus (MRSA) • Etiology • Strains of staphylococcus bacteria that are resistant to some antibiotics • Often occurs in individuals that are already sick, in hospital and are ill, have open wounds, or burns • Can occur outside of hospital setting as well • Signs & Symptoms • Redness, swelling, tenderness of infection site • Some may carry MRSA and not exhibit symptoms • Management • Antibiotics (higher dose) provided intravenously • Treatment lasts several weeks © 2011 McGraw-Hill Higher Education. All rights reserved.
Impetigo Contagiosa • Etiology • Caused by A-beta-hemolytic streptococci, S aureus or combination of these bacteria • Spread through close contact • Signs and Symptoms • Mild itching and soreness followed by eruption of small vesicles and pustules that rupture and crust • Generally develops in body folds that are subject to friction • Management • Cleansing and topical antibacterial agents • Systemic antibiotics © 2011 McGraw-Hill Higher Education. All rights reserved.
Furuncles (Boils) • Etiology • Infection of hair follicle that results in pustule formation • Generally the result of a staph. infection © 2011 McGraw-Hill Higher Education. All rights reserved.
Signs and Symptoms • Pustule that becomes reddened and enlarged as well as hard from internal pressure • Pain and tenderness increase with pressure • Most will mature and rupture • Management • Care involves protection from additional irritation • Referral to physician for antibiotics • Keep patient from contact with other team members while boil is draining © 2011 McGraw-Hill Higher Education. All rights reserved.
Carbuncles • Etiology • Similar in terms of early stage development as furuncles • Signs and Symptoms • Larger and deeper than furuncle and has several openings in the skin • May produce fever and elevation of WBC count • Starts hard and red and over a few days emerges into a lesion that discharges yellowish pus • Management • Surgical drainage combined with the administration of antibiotics • Warm compress is applied to promote circulation © 2011 McGraw-Hill Higher Education. All rights reserved.
Folliculitis • Etiology • Inflammation of hair follicle • Caused by non-infectious or infectious agents • Moist warm environment and mechanical occlusion contribute to condition • Pseudofolliculitis (PFB) © 2011 McGraw-Hill Higher Education. All rights reserved.
Signs and Symptoms • Redness around follicle that is followed by development of papule or pustule at the hair follicle • Followed by development of crust that sloughs off with the hair • Deeper infection may cause scarring and alopecia in that area • Management • Management is much like impetigo • Moist heat is used to increase circulation • Antibiotics can also be used depending on the condition © 2011 McGraw-Hill Higher Education. All rights reserved.
Hidradenitis Suppurativa • Etiology • Primary inflammation event of the hair follicle resulting in secondary blockage of the apocrine gland • Signs and Symptoms • Begins as small papule that can develop into deep dermal inflammation • Management • Avoid use of antiperspirants, deodorants and shaving creams • Use medicated soaps and systemic antibiotics © 2011 McGraw-Hill Higher Education. All rights reserved.
Acne Vulgaris • Etiology • Inflammatory disease of the hair follicle and the sebaceous glands • Sex hormones may contribute • Signs and Symptoms • Present with whiteheads, blackheads, flesh or red colored papules, pustules or cysts • If chronic and deep = may scar • Psychological impact • Management • Topical and systemic agents used to treat acne • Sometimes the use endogenous hormones is required • Mild soaps are recommended © 2011 McGraw-Hill Higher Education. All rights reserved.
Paronychia and Onychia • Etiology • Caused by staph, strep and or fungal organisms that accompany contamination of open wounds or hangnails • Damage to cuticle puts finger at risk • Onychia is an infection of the nail bed itself, while paronychia involves the lateral nail fold • Signs and Symptoms • Rapid onset; painful with bright red swelling of proximal and lateral fold of nail • Accumulation of purulent material w/in nail fold • Management • Soak finger or toe in hot solution of Epsom salt 3 times daily • Topical antibiotics, systemic antibiotics if severe • May require pus removal through skin incision © 2011 McGraw-Hill Higher Education. All rights reserved.
Tetanus Infection (lockjaw) • Etiology • Acute infection of the CNS and muscles caused by tetanus bacillus • Bacteria enters through the blood and open wounds • Signs and Symptoms • Stiffness of the jaw and muscles of the neck • Muscles of facial expression produce contortion and become painful • Fever may become markedly elevated • Management • Treat in intensive care unit • Childhood immunization © 2011 McGraw-Hill Higher Education. All rights reserved.
Fungal Infections • Group of organisms that include yeast and molds which are usually not pathogenic • Grow best in unsanitary conditions with warmth, moisture and darkness • Infections generally occur in keratinized tissue found in hair, nails and stratum corneum • Dermatophytes (Ringworm fungi) • Cause of most skin, nail and hair fungal infections © 2011 McGraw-Hill Higher Education. All rights reserved.
Tinea of the Scalp (tinea capitis) • Signs and Symptoms • Ringworm of the scalp begins as a small papule that spreads peripherally • Appears as small grayish scales resulting in scattered balding • Easily spread through close physical contact • Management • Topical creams and shampoos are ineffective in treating fungus in hair shaft • Systemic antifungal agents are replacing older agents due to increased resistance • Some topical agents are used in conjunction © 2011 McGraw-Hill Higher Education. All rights reserved.
Tinea of the Body (tinea corporis) • Signs and Symptoms • Commonly involve extremities and trunk • Itchy red-brown scaling annular plaque that expands peripherally • Management • Topical antifungal cream © 2011 McGraw-Hill Higher Education. All rights reserved.
Tinea of the Nail (tinea unguium/ onychomycosis) • Signs and Symptoms • Fungal infection of the nail -- found commonly in those engaged in water sports or who have chronic athlete’s foot • Nail becomes thick, brittle and separated from its bed • Management • Some topical antifungal agents have proved useful • Systemic medications are most effective • Surgical removal of nail may be necessary if extremely infected © 2011 McGraw-Hill Higher Education. All rights reserved.
Tinea of the Groin (tinea cruris) • Etiology • Symmetric red-brown scaling plaque with snake-like border • Signs and Symptoms • Mild to moderate itching • May progress to secondary bacterial infection © 2011 McGraw-Hill Higher Education. All rights reserved.
Management • Treat until cured • Will respond to many of the non-prescription medications • Medications that mask symptoms should be avoided • Failure to respond to normal management may suggest a non-fungal problem (such as bacteria) and should be referred to a physician • May require additional topical medications and oral prescriptions © 2011 McGraw-Hill Higher Education. All rights reserved.
Athlete’s Foot (tinea pedis) • Etiology • Most common form of superficial fungal infection • Trichophyton species are most common cause of athlete’s foot • Webs of toes may become infected by a combination of yeast and dermatophytes • Signs and Symptoms • Extreme itching on soles of feet, between and on top of toes • Appears as dry scaling patch or inflammatory scaling red papules forming larger plaques • May develop secondary infection from itching and bacteria • Management • Topical antifungal agents and good foot hygiene © 2011 McGraw-Hill Higher Education. All rights reserved.
Candidiasis (Moniliasis) • Etiology • Yeast-like fungus that can produce skin, mucous membrane and internal infections • Ideal environment includes hot humid weather, tight clothing, and poor hygiene • Signs and Symptom • Infections w/in body folds • Presents as beefy red patches and possible satellite pustules • White, macerated border may surround the red area; deep painful fissures may develop at skin creases • Management • Maintain dry area • Use antifungal agents to clear infection © 2011 McGraw-Hill Higher Education. All rights reserved.
Tinea Versicolor • Etiology • Caused by a yeast • Appears commonly in areas in which sebaceous glands actively secrete body oils • Signs and Symptoms • Fungus produces multiple, small, circular macules that are pink, brown, or white • Commonly occur on chest, abdomen, and neck • Do not tan when exposed to sun and usually are asymptomatic • Management • Straightforward treatment - recurrences are common • Use selenium shampoo (Selsun) and topical econazole nitrate (or something similar) • When microorganism has been eradicated, re-pigmentation of the area will occur © 2011 McGraw-Hill Higher Education. All rights reserved.
Viral Infections • Ultramicroscopic organisms that require host cells to complete their life cycle • May stimulate cell chemically to produce more virus until host cell dies • Lies within bud-like structure that does not damage cell or virus, w/out causing infection • A number of skin infections are caused by viruses © 2011 McGraw-Hill Higher Education. All rights reserved.