YELLOW FEVER
YELLOW FEVER. EPIDEMIOLOGY 1. YF is an acute haemorrhagic fever caused by the YF virus - an RNA virus which belongs to the genus of FLAVIVIRUSES. (arbovirus) 2 forms are known:

YELLOW FEVER
E N D
Presentation Transcript
YELLOW FEVER DR (MRS) M.B. FETUGA
EPIDEMIOLOGY 1 • YF is an acute haemorrhagic fever caused by the YF virus - an RNA virus which belongs to the genus of FLAVIVIRUSES. (arbovirus) • 2 forms are known: -Urban form: Direct man-to-man transmission by the Aedes aegypti mosquitoes which breed in pots and cans around houses. -Jungle form: Zoonotic infection of monkeys found in the tropical rain forests. Acquired through the bites of Aedes africanus and A. simpsoni which transmit the virus from the infected monkeys to man. DR (MRS) M.B. FETUGA
EPIDEMIOLOGY 2 YF circulates zoonotically as three genotypes: type I and IIA in West & Central Africa, respectively and type IIB in South America. Present-day African epidemics are primarily urban. In areas where outbreaks of urban YF are common, most cases involve children because many adults are immune. Transmission in West Africa is highest during the peak of the rainy season, from July to October. DR (MRS) M.B. FETUGA
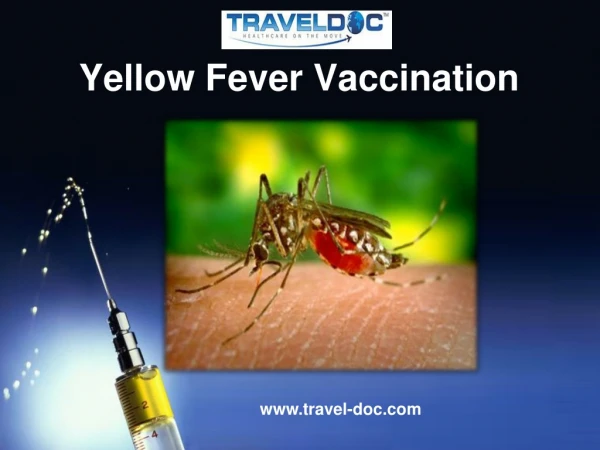
TRANSMISSION • The infection is acquired by the bite of infected mosquitoes. • 1-2 weeks in the mosquito before it is capable of transmitting the virus • The virus replicates in the local LNs, enters the blood (10ry viraemia) • Then deposited in the liver, spleen, kidney, bone marrow and lymph glands. • After a short interval during which the virus persists in these organs and replicates, the virus appears in the blood again -(20ry viraemia) DR (MRS) M.B. FETUGA
PATHOGENESIS 1 • Pathological changes include: • Swelling of hepatocytes followed by coagulative necrosis in the midzone of the liver lobule. • Formation of Councilman bodies (hyaline, irregular, eosinophilic masses) • Similar cellular damage occur in other organs. DR (MRS) M.B. FETUGA
PATHOGENESIS 2 • KIDNEYS: Acute tubular necrosis & Renal failure. • HEART: Myocardial fiber degeneration and fatty infiltration. • BRAIN: Oedema and petechial hemorrhages. • LIVER: Direct injury results in impaired ability to carry out its functions of biosynthesis and detoxification. This is the central pathogenic event of YF. Hemorrhage is thought to result from decreased synthesis of vitamin K–dependent clotting factors and DIC. DR (MRS) M.B. FETUGA
CLINICAL FEATURES1 • Incubation period 3 - 6 days. • Studies that children experience a milder disease than adults • Most cases are abortive (inapparent) and are missed. Xterised by a flu-like syndrome - fever, headache) that is easily passed as viral URTI. DR (MRS) M.B. FETUGA
CLINICAL FEATURES 2 • Classic form: -Sudden onset of fever, headache, myalgia, arthralgia, anorexia, nausea, vomiting, conjunctival injection, flushing of face & neck, bradycardia and reddening of the tongue at the tip and edges with foul breath occur early in the illness. Brief period of remission occurs. DR (MRS) M.B. FETUGA
CLINICAL FEATURES 3 6 – 24 hrs later: Reappearance of fever, vomiting, epigastric pain, jaundice, dehydration, GIT & other hemorrhages especially hematemesis. Albuminuria, hypotension, signs of renal failure, delirium, convulsions, and coma. Death may occur between the 7th and 10th days. Fatality rate in severe cases – close to 50%. Survivors of the acute phase of illness may succumb to renal failure or myocardial damage. DR (MRS) M.B. FETUGA
LABORATORY • Viral culture • Serology: Rising titres of anti-YF antibodies • FBC: Leukopenia, thrombocytopaenia • Clotting profile: Prolonged clotting, prothrombin, and partial thromboplastin times • LFT: Hyperbilirubinemia; elevated serum transaminases; • Serum E&U: Azotaemia • Urinalysis: Albuminuria • RBS: Hypoglycemia may be present in severe cases • ECG: Bradycardia and ST-T changes. DR (MRS) M.B. FETUGA
LABORATORY • Necropsy: Liver biopsy -Coagulative necrosis of hepatocytes in the midzone -Microvascular fatty degeneration -Minimal inflammation -Eosinophilic degeneration of hepatocytes (Councilman bodies –confirm the diagnosis DR (MRS) M.B. FETUGA
LABORATORY • Kidneys- Acute tubular necrosis • Heart- Myocardial fibre degeneration & fatty infiltration • Brain- Oedema & petechial hemorrhage • Hematologic- DIC & ↓vit K- factors DR (MRS) M.B. FETUGA
DIFFERENTIAL DIAGNOSIS • Severe malaria • Septicaemia • Hepatitis • Dengue • Marburg-Ebola • Leptospirosis DR (MRS) M.B. FETUGA
MANAGEMENT • There is no specific treatment for YF. • Since patients are viraemic during the febrile phase of the illness, it is necessary to isolate YF patients e.g. using mosquito nets. • Supportive treatments include (1) Control fever thro’ tepid sponging and paracetamol (2) Vigorous IV fluid replacement of losses (3) Correct acid-base imbalance (4)Avoid drugs that are metabolized by the liver or toxic to the liver, kidney, or CNS. • Prompt correction of bleeding disorders with FRESH WHOLE BLOOD. • Dialysis for ARF. DR (MRS) M.B. FETUGA
PREVENTION • YF 17D vaccine - live, attenuated vaccine. Administered as a single 0.5-mL subcutaneous injection at 9 months in the NPI schedule. (Safe) • Confers life-long immunity. • YF vaccine should not be administered to persons with symptomatic immunodeficiency diseases and those on immunosuppressants. • Small risk of encephalitis after vaccination in children younger than 9 months. DR (MRS) M.B. FETUGA