Ulcerative Colitis Mini Case Study
Ulcerative Colitis Mini Case Study. Krista Blackwell Sodexo Mid-Atlantic Dietetic Internship January 6, 2014. Overview. Ulcerative Colitis MNT in IBD Case Study History and Physical Medication and Labs Assessment Diagnoses Goals and Intervention Monitoring and Evaluation Education

Ulcerative Colitis Mini Case Study
E N D
Presentation Transcript
Ulcerative ColitisMini Case Study Krista Blackwell Sodexo Mid-Atlantic Dietetic Internship January 6, 2014
Overview • Ulcerative Colitis • MNT in IBD • Case Study • History and Physical • Medication and Labs • Assessment • Diagnoses • Goals and Intervention • Monitoring and Evaluation • Education • Article Review • Resources
Ulcerative Colitis • A form of IBD that effects the colon and rectum • Causes: Genetic, environment, and “irritant” • Inflammatory and abnormal immune response • Dx made with sigmoidoscopy
Side Effects • Protein losses • Electrolyte disturbances • Dehydration • Anorexia • Malabsorption • Altered GI transit • Increased secretions • Diarrhea • Fever • Weight loss • Anemia • Food intolerances • Malnutrition • GI and/or rectal bleed • Growth failure
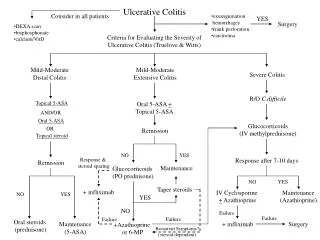
MNT in IBD • Goals: Reduce inflammation, alleviate symptoms, correct dehydration and nutritional deficiencies • Individualized treatment • Acute phase/ flare up: Low-fiber • Remission: High protein (1.0-1.5 g/kg), nutrient-dense diet, 2 quarts of water daily
MNT in IBD • Avoid: Diarrhea-causing foods, extreme temperatures, carbonated beverages, alcohol, caffeine, spicy foods, lactose • Small frequent meals, eat slowly and chew well • MVI with minerals: Thiamine, Vit E, iron, zinc, Ca, K, folic acid
Case Study: History and Physical • CP is a 26 year old female • PMHx: Dx with ulcerative colitis in 2011 • CP reported having multiple episodes of bloody diarrhea • Distended abdomen and abdominal cramping • NKA
Chief Complaint • Nov. 2nd: CP presented with bloody bowel movements and fatigue, was put under observation and given Solu-Medrol and prednisone and d/c Nov. 3 • Nov. 6th: CP vomited her first dose of prednisone • Nov. 9th: Early this morning, CP had one bloody BM an hour and presented to the ED and was admitted to SGAH for further evaluation and monitoring
Medical Diagnoses • Ulcerative Colitis (Dx in 2011) • Rectal bleeding • Hemorrhage of the anus and rectum • Hypokalemia • Anemia
Social History • CP is a 26 year-old Caucasian female • Lives at home in Rockville, MD with her parents • Manager at GAP • Works long hours • Limited access to food
Anthropometric Data • Ht: 157cm (62”) • Wt 11/9/13: 46.5 kg (102.3lb) • Wt 11/3/13: 53.6 kg (118lb) • UBW: 50kg (110lb) • IBW: 50 kg (110lb) • %IBW: 93% • % wt change: 5% wt loss over 1 week • BMI: 18.86
Nutrition Assessment • Diet Order: Clear Liquid • Intake: Fair • Risk Level: Moderate • Reason for visit: Diet Education • Summary of visit • 8lb wt loss since last hospital admission on 11/3 • Pt’s nausea subsided, able to consume clear liquid diet and the doctor will be advancing her to full liquids • Tries to drink adequate fluids, usually about 3-4 bottles of water a day • No BM since hospital admission • Provided pt with diet education for ulcerative colitis/ inflammatory bowel disease
Nutrition Prescription • Estimated Energy Needs: 1388-1500kcal • (MSJ 1.2-1.3) • Estimated Protein Needs: 38-47g (0.8-1.0 g/kg) • Estimated Fluid Needs: 1500 mL (1mL/kcal) • Micronutrient Needs: MVI with minerals
Nutrition Diagnoses • Nutrition Diagnoses I: Involuntary weight loss R/T ulcerative colitis AEB 5% wt loss over 1 week • Diagnoses II: Food and nutrition-related knowledge deficit R/T lack of prior exposure to nutrition-related information AEB no formal prior education while experiencing acute colitis symptoms
Goals • Pt consume adequate energy intake: At least 75% of meals within the next 3-4 days. • Pt maintain current weight and prevent further weight loss • Patient to demonstrate knowledge of diet guidelines through menu selections prior to discharge
Interventions • Nutrition Education: Provided pt with information about a low fiber diet for the next few weeks and how to slowly reincorporate fiber into the diet • Food and Nutrition Delivery/ Meals and Snacks: As tolerated and as medically feasible, suggest advancing to a low fiber diet • MVI with minerals
Monitoring and Evaluation • Monitor po intake • Monitor pt’s wt trends • RD to monitor understanding of information presented
Discharge Summary • Discharged Nov. 13 • Diagnoses: • Ulcerative Colitis flare • Rectal bleeding secondary to ulcerative colitis flare: Diarrhea and rectal bleed resolved • Anemia, which is stable • Acute dehydration • Hypokalemia, which is resolved • Discharge medications: Prednisone and protonix • Pt to follow up with GI doctor in 2 days
Nutrition Care in Adult IBD Nutrition Issues in Gastroenterology, June 2012Authors: Amar S. Naik and Nanda Venu • Nutrition Assessment • Identifying deficiencies and malnourished pts • Goals • Diet in IBD • Common Deficiencies: Fe, Zinc, Mg, Vit B12, Folate, Vit D and Ca • Omega 3s • Enteral and Parenteral Nutrition
Remission Induction and Maintenance Effect of Probiotics on Ulcerative Colitis: A meta-analysis World Journal of Gastroenterology, April 2010Authors: Li-Xuan Sang, Bing Chang, Wen-Liang Zhang, Xiao-Mei Wu, Xiao-Hang Li, Min Jiang • Aim: To evaluate the induction of remission and maintenance effects of Probiotics for UC • 13 randomized controlled trials from MEDLINE, EMBASE, Cochrane Controlled Trials Register • Evaluates probiotic’s curative effects for treating UC based on existing random control trials
Remission Induction and Maintenance Effect of Probiotics on Ulcerative Colitis: A meta-analysis • Results: Further research is needed including variations of bacterial species, applied dosage, treatment timing, and course of treatment • Results were not consistent
Resources • Mahan, K.., Escott-Stump, S, Raymond, J. Krause’s Food and the Nutrition Care Process. 3rd ed. Elsevier Saunders. 2012 • Width, Mary; Reinhard, Tonia. The Clinical Dietitian’s Essential Pocket Guide. Lippincott Williams & Wilkins. 2009. • Naik, Amar S., Venu, Nanda. “Nutrition Care in Adult Inflammatory Bowel Disease.” Nutrition Issues in Gastroenterology, series #106. June 2012. • Sang, Li-Xuan., Chang, Bing., Zhang, Wen-Liang., Wu, Xiao-Mei., Li, Xiao-Hang., Jiang, Min. “Remission induction and maintenance effect of probiotics on ulcerative colitis: A meta-analysis”. World Journal of Gastroenterology. April 2010.