Viral Hepatitis and HIV based on Centers for Disease Control information
220 likes | 718 Vues
Viral Hepatitis and HIV based on Centers for Disease Control information. IPPF Competencies Workshop, Mexico City, 28 July - 1 August 2008 Lynn Collins, Technical Advisor, HIV/AIDS, UNFPA. What is hepatitis?. Definition: inflammation of the liver Causes: toxins certain drugs

Viral Hepatitis and HIV based on Centers for Disease Control information
E N D
Presentation Transcript
Viral Hepatitis and HIVbased on Centers for Disease Control information IPPF Competencies Workshop, Mexico City, 28 July - 1 August 2008 Lynn Collins, Technical Advisor, HIV/AIDS, UNFPA
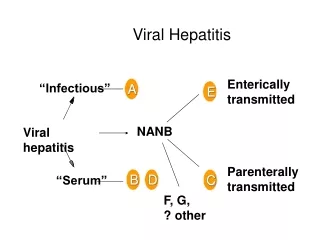
What is hepatitis? • Definition: inflammation of the liver • Causes: • toxins • certain drugs • some diseases • heavy alcohol use • bacterial and viral infections • Also the name of a family of viral infections that affect the liver; A,B,C,D, and E
Hepatitis A Virus (HAV) • Hepatitis A: an acute liver disease caused by the hepatitis A virus (HAV), lasting from a few weeks to several months. It does not lead to chronic infection. • Transmission: Ingestion of fecal matter, even in microscopic amounts, from close person-to-person contact or ingestion of contaminated food or drinks. • Vaccination: Hepatitis A vaccination is recommended for all children starting at age 1 year, travelers to certain countries, and others at risk.
Signs/symptoms (usually <2 mo.) Fever Fatigue Loss of appetite Nausea Vomiting Abdominal pain Dark urine Clay-colored bowel movements Joint pain Jaundice jaundice or elevated serum aminotransferase levels. Confirmation: a positive serologic test for IgM antibody to hepatitis A virus, or clinical case definition Person-to-person transmission through the fecal-oral route ingestion of something that has been contaminated with the feces of an infected person Most infections result from close personal contact with an infected household member or sex partner. Common-source outbreaks and sporadic cases also can occur from exposure to fecally contaminated food or water. Hepatitis A
Who is at increased risk for HAV? • Travelers to countries with high or intermediate endemicity of HAV • Men who have sex with men • Users of injection and non-injection illegal drugs • Persons with clotting factor disorders • Persons working with nonhuman primates susceptible to HAV infection
HAV • Incubation period 28 days (range: 15–50 days). • Survival outside the body for months, depending on the environmental conditions. The virus is killed by heating to 185 degrees F (85 degrees C) for one minute. Adequate chlorination of water kills HAV that enters the water supply. • Hepatitis A does not become chronic. • Reinfection not possible: IgG antibodies to HAV, which appear early in the course of infection, provide lifelong protection against the disease. • Prevention • by vaccination with the full, two-dose series – lasts 25 years in adults and at least 14–20 years in children • The safety of hepatitis A vaccination during pregnancy has not been determined; however, because the vaccine is produced from inactivated HAV, the theoretical risk to the developing fetus is expected to be low. • Because hepatitis A vaccine is inactivated, no special precautions need to be taken when vaccinating immunocompromised persons • Immune globulin is available for short-term protection (approximately 3 months) both pre- and post-exposure. Immune globulin must be administered within 2 weeks after exposure for maximum protection. • Good hygiene.
Vaccination candidates HAV • All children at age 1 year (i.e., 12–23 months). • Children and adolescents ages 2–18 who live in states or communities where routine hepatitis A vaccination has been implemented because of high disease incidence.. • Persons traveling to or working in countries that have high or intermediate rates of hepatitis A. • Men who have sex with men. Sexually active men (both adolescents and adults) who have sex with men should be vaccinated. Hepatitis A outbreaks among men who have sex with men have been reported frequently. • Users of illegal injection and noninjection drugs. During the past two decades, outbreaks of hepatitis A have been reported with increasing frequency among users of both injection and noninjection drugs (e.g., methamphetamine) in North America, Europe, and Australia. • Persons who have occupational risk for infection. Persons who work with HAV-infected primates or with HAV in a research laboratory setting should be vaccinated. No other groups have been shown to be at increased risk for HAV infection because of occupational exposure. • Persons who have chronic liver disease. Persons with chronic liver disease who have never had hepatitis A should be vaccinated, as they have a higher rate of fulminant hepatitis A (i.e., rapid onset of liver failure, often leading to death). Persons who are either awaiting or have received liver transplants also should be vaccinated. • Persons who have clotting-factor disorders. Persons who have never had hepatitis A and who are administered clotting-factor concentrates, especially solvent detergent-treated preparations, should be vaccinated.
Hepatitis B • Hepatitis B: a liver disease caused by the hepatitis B virus (HBV). It ranges in severity from a mild illness, lasting a few weeks (acute), to a serious long-term (chronic) illness that can lead to liver disease or liver cancer. • Transmission: Contact with infectious blood, semen, and other body fluids from having sex with an infected person, sharing contaminated needles to inject drugs, orfrom an infected mother to her newborn. • Vaccination: Hepatitis B vaccination is recommended for all infants, older children and adolescents who were not vaccinated previously, and adults at risk for HBV infection
Signs/symptoms (acute: several weeks to 6 months) Fever Fatigue Loss of appetite Nausea Vomiting Abdominal pain Dark urine Clay-colored bowel movements Joint pain Jaundice Persons with chronic HBV infection might be asymptomatic, have no evidence of liver disease, or have a spectrum of disease ranging from chronic hepatitis to cirrhosis or hepatocellular carcinoma (a type of liver cancer). Confirmation: a serologic testing HBV is transmitted through activities that involve percutaneous (i.e., puncture through the skin) or mucosal contact with infectious blood or body fluids (e.g., semen, saliva), including Sex with an infected partner Injection drug use that involves sharing needles, syringes, or drug-preparation equipment Birth to an infected mother Contact with blood or open sores of an infected person Needle sticks or sharp instrument exposures Sharing items such as razors or toothbrushes with an infected person HBV is not spread through food or water, sharing eating utensils, breastfeeding, hugging, kissing, hand holding, coughing, or sneezing. Hepatitis B
Who is at increased risk for HBV? • Infants born to infected mothers • Sex partners of infected persons • Sexually active persons who are not in a long-term, mutually monogamous relationship (e.g., >1 sex partner during the previous 6 months) • Men who have sex with men • Injection drug users • Household contacts of persons with chronic HBV infection • Healthcare and public safety workers at risk for occupational exposure to blood or blood-contaminated body fluids • Hemodialysis patients • Residents and staff of facilities for developmentally disabled persons • Travelers to countries with intermediate or high prevalence of HBV
HBV • Incubation period 90 days (range: 60–150 days) • Survival outside the body for 7 days • Acute infection ranges from asymptomatic or mild disease to — rarely — fulminant hepatitis. • Chronic HBV infection: • Approximately 25% of those who become chronically infected during childhood and 15% of those who become chronically infected after childhood die prematurely from cirrhosis or liver cancer, and the majority remain asymptomatic until onset of cirrhosis or end-stage liver disease. • The risk for chronic infection varies according to the age at infection and is greatest among young children. Approximately 90% of infants and 25%–50% of children aged 1–5 years will remain chronically infected with HBV. By contrast, approximately 95% of adults recover completely from HBV infection and do not become chronically infected.
HBV • Prevention • Vaccination with the full, two-dose series – lasts 23 years • Hepatitis B vaccine contains no live virus, so neither pregnancy nor lactation should be considered a contraindication to vaccination of women. On the basis of limited experience, there is no apparent risk of adverse effects to developing fetuses when hepatitis B vaccine is administered to pregnant women. • Larger doses or additional doses might also be necessary hemodialysis and immunocompromised persons and serologic testing is recommended 1–2 months after administration of the final dose of the primary vaccine series to determine the need for revaccination. Also for sex partners of persons with chronic HBV infection, and exposed infants • Need for booster doses not known for PLHIV • After a person has been exposed to HBV, appropriate prophylaxis, given as soon as possible but preferably within 24 hours, can effectively prevent infection. The mainstay of postexposure immunoprophylaxis is hepatitis B vaccine, but in certain circumstances the addition of HBIG will provide increased protection. • Treatment • For acute infection, no medication is available; treatment is supportive. • For chronic infection, several antiviral drugs (adefovir dipivoxil, interferon alfa-2b, pegylated interferon alfa-2a, lamivudine, entecavir, and telbivudine) are available. Persons with chronic HBV infection require medical evaluation and regular monitoring to determine whether disease is progressing and to identify liver damage or hepatocellular carcinoma.
Vaccination candidates HBV • All infants, beginning at birth • All children aged <19 years who have not been vaccinated previously • Susceptible sex partners of hepatitis B surface antigen (HBsAg)-positive persons • Sexually active persons who are not in a long-term, mutually monogamous relationship (e.g., >1 sex partner during the previous 6 months) • Persons seeking evaluation or treatment for a sexually transmitted disease • Men who have sex with men • Injection drug users • Susceptible household contacts of HBsAg-positive persons • Healthcare and public safety workers at risk for exposure to blood or blood-contaminated body fluids • Persons with end-stage renal disease, including predialysis, hemodialysis, peritoneal dialysis, and home dialysis patients • Residents and staff of facilities for developmentally disabled persons • Travelers to regions with intermediate or high rates of endemic HBV • Persons with chronic liver disease • Persons with HIV infection • All other persons seeking protection from HBV infection — acknowledgment of a specific risk factor is not a requirement for vaccination
Hepatitis C • Hepatitis C: a liver disease caused by the hepatitis C virus (HCV). HCV infection sometimes results in an acute illness, but most often becomes a chronic condition that can lead to cirrhosis of the liver and liver cancer. • Transmission: Contact with the blood of an infected person, primarily through sharing contaminated needles to inject drugs. • Vaccination: There is no vaccine for hepatitis C.
Signs/symptoms 70%–80% of people with acute hepatitis C do not have any symptoms. For those who do, they appear 6-7 weeks after exposure. Fever Fatigue Loss of appetite Nausea Vomiting Abdominal pain Dark urine Clay-colored bowel movements Joint pain Jaundice (yellow color in the skin or eyes) HCV is transmitted by: Sharing needles, syringes, or other equipment to inject drugs Needlestick injuries Being born to a HepC + mother Less commonly, a person can also get hepatitis C virus infection through: Sharing personal care items that may have come in contact with another person’s blood (razors or toothbrushes) Having sexual contact with a HepC+ person the risk of transmission from sexual contact is believed to be low. Risk increases for those who have multiple sex partners, have a sexually transmitted disease, engage in rough sex, or are living with HIV. More research is needed to better understand how and when hepatitis C can be spread through sexual contact. Hepatitis C virus is not spread by sharing eating utensils, breastfeeding, hugging, kissing, holding hands, coughing, or sneezing. It is also not spread through food or water. Hepatitis C
Who is at increased risk for HCV? • Current injection drug users • Past injection drug users, including those who injected only one time or many years ago • Recipients of donated blood, blood products, and organs • People who received a blood product for clotting problems made before 1987 • Hemodialysis patients or persons who spent many years on dialysis for kidney failure • People who received body piercing or tattoos done with non-sterile instruments • People with known exposures to the hepatitis C virus, such as • Healthcare workers injured by needlesticks • Recipients of blood or organs from a donor who tested positive for the hepatitis C virus • People living with HIV • Children born to mothers infected with the hepatitis C virus
HCV Incubation period 4–12 weeks (range: 2–24 weeks). Of every 100 people infected with the hepatitis C virus, about • 75–85 people will develop chronic hepatitis C virus infection; of those, • 60–70 people will go on to develop chronic liver disease • 5–20 people will go on to develop cirrhosis over a period of 20–30 years • 1–5 people will die from cirrhosis or liver cancer Approximately 15%–25% of people who get hepatitis C will clear the virus from their bodies without treatment and will not develop chronic infection. Experts do not fully understand why this happens for some people.
HCV Prevention • Clients should be informed about the low but present risk for transmission with sex partners. • Sharing personal items that might have blood on them, such as toothbrushes or razors, can pose a risk. • Cuts and sores on the skin should be covered to keep from spreading infectious blood or secretions. • Donating blood, organs, tissue, or semen can spread HCV to others. • HCV is not spread by sneezing, hugging, holding hands, coughing, sharing eating utensils or drinking glasses, or through food or water. • Patients may benefit from a joining support group. Treatment • Combination therapy with pegylated interferon and ribavirin is the treatment of choice. Treatment success rates are now being improved with the addition of polymerase and protease inhibitors to standard pegylated interferon/ribavirin combination therapy. • HCV-positive persons should be advised to avoid alcohol because it can accelerate cirrhosis and end-stage liver disease. • Viral hepatitis patients should also check with a health professional before taking any new prescription pills, over-the counter drugs (such as non-aspirin pain relievers), or supplements, as these can potentially damage the liver.
Who should be tested for HCV? • Persons who have ever injected illegal drugs, including those who injected only once many years ago • Recipients of clotting factor concentrates made before 1987 • Recipients of blood transfusions or solid organ transplants before July 1992 • Patients who have ever received long-term hemodialysis treatment • Persons with known exposures to HCV, such as • healthcare workers after needlesticks involving HCV-positive blood • recipients of blood or organs from a donor who later tested HCV-positive • All persons living with HIV • Patients with signs or symptoms of liver disease (e.g., abnormal liver enzyme tests) • Children born to HCV-positive mothers (to avoid detecting maternal antibody, these children should not be tested before age 18 months)
HIV and Hepatitis Hepatitis B and HIV • HBV) and HIV are bloodborne viruses transmitted primarily through sexual contact and injection drug use. Because of these shared modes of transmission, a high proportion of adults at risk for HIV infection are also at risk for HBV infection. • HIV-positive persons who become infected with HBVare at increased risk for developing chronic HBV infection. • Persons who are co-infected with HIV and HBV can have serious medical complications, including an increased risk for liver-related morbidity and mortality. • To prevent HBV infection in people living with HIV, hepatitis B vaccination is recommended Hepatitis C and HIV • HCV is a bloodborne virus transmitted through direct contact with the blood of an infected person. Thus, coinfection with HIV and HCV is common (50%–90%) among HIV positive injection drug users. • HCV infection progresses more rapidly to liver damage in people living with HIV. • HCV infection may also impact the course and management of HIV infection. • People living with HIV should be screened for HCV infection. • Injection drug users (IDUs) are at risk for HBV and HCV sharing needles and drug-preparation equipment. HAV outbreaks are believed to occur through both percutaneous and fecal-oral routes. IDUs should get vaccinated against hepatitis A and hepatitis B. Hepatitis, HIV, and MSM • Men who have sex with men (MSM) are at elevated risk for certain sexually transmitted diseases (STDs), including hepatitis A, hepatitis B, HIV/AIDS, syphilis, gonorrhea, and chlamydia. Despite the availability of safe and effective vaccines, many MSM have not been adequately vaccinated against viral hepatitis.
Hepatitis D • Hepatitis D: a serious liver disease caused by the hepatitis D virus (HDV) and relies on HBV to replicate. • Transmission: Contact with infectious blood, similar to how HBV is spread. • Vaccination: There is no vaccine for hepatitis D.
Hepatitis E • Hepatitis E: a serious liver disease caused by the hepatitis E virus (HEV) that usually results in an acute infection. It does not lead to a chronic infection. • Transmission: Ingestion of fecal matter, even in microscopic amounts; outbreaks are usually associated with contaminated water supply in countries with poor sanitation. • Vaccination: There is currently no FDA-approved vaccine for hepatitis E.