Pressure Ulcer Prevalence
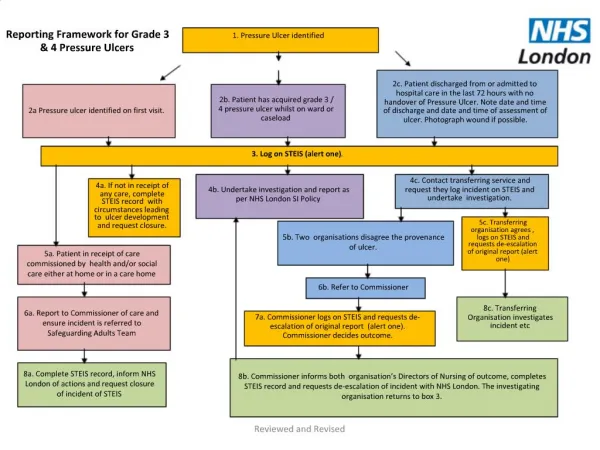
Pressure Ulcer Prevalence. Hospital Wide Monitoring & Management www.woundcarenurses.org Alex Khan RN BSN CWCN CFCN. Problem. According to Centers for Medicare & Medicaid (2010) more than 2.5 million people in the United States develop pressure ulcers annually.

Pressure Ulcer Prevalence
E N D
Presentation Transcript
Pressure Ulcer Prevalence Hospital Wide Monitoring & Management www.woundcarenurses.org AlexKhan RN BSN CWCN CFCN
Problem • According to Centers for Medicare & Medicaid (2010) more than 2.5 million people in the United States develop pressure ulcers annually. • Pressure ulcers cause pain, increased health risks such as; serious wound infections, mortality and increased health care utilization. • In-hospital mortality was also higher for pressure ulcer-related hospitalizations, death occurred in 11.6 percent of stays with pressures ulcers noted as a secondary diagnosis, (AHRQ, 2008). • The Centers for Medicare & Medicaid no longer provides reimbursement to hospitals to care for a patient who has acquired a pressure ulcer while under the hospital‘s care, (CMS, 2008).
Challenge Pressure ulcer prevention and prevalence presents an important challenge in acute and long term acute care hospitals. Pressure ulcer prevention requires an interdisciplinary and system wide approach to care. To accomplish this task; coordination between all disciplines, an organizational process and operational practices are needed. Therefore, pressure ulcer prevention and prevalence calls for a system focus to make needed changes.
Definition What is a Pressure Ulcer ? • Any lesion caused by unrelieved pressure resulting in damage of underlying tissue (AHCPR, 1994). • A pressure ulcer is localized injury to the skin and/or underlying tissue usually over a bony prominence, as a result of pressure, or pressure in combination with shear and/or friction (NPUAP, 2007).
Pressure Ulcer Stages The staging of pressure ulcers, as defined by national guidelines (NPUAP), allow for common understandings for healthcare professionals. • Stage I • Stage II • Stage III • Stage IV • Suspected Deep Tissue Injury (DTI) • Unstageable
Pressure Ulcer Causes • Immobility or limited mobility • Bowel & bladder incontinence • Shearing and friction injuries • Malnutrition or debility • Obesity • History of pressure ulcers • Dehydration • Contractures • Lack of compliance • Use of diapers / excess skin moisture
Current Practice • All patients are assessed for presence of pressure ulcers or wounds during the admission skin assessment completed by a Registered Nurse. • If a pressure ulcer / wound is identified during the admission assessment, it is categorized as “Community Acquired”. • If a pressure ulcer is identified during a daily nursing assessment but it was not identified & documented during the admission assessment, it is categorized as “Hospital Acquired”.
Current Practice • Based on the information entered by the registered nurse into the computer system, the hospital’s pressure ulcer prevalence percentage is calculated. • Pressure Ulcers are classified according to the National Pressure Ulcer Advisory Panel (NPUAP) guidelines. • Incidence of pressure ulcers is one of the Quality Indicator (QIs) reflecting hospital’s quality of care. Pressure ulcer prevalence data is utilized to measure quality of care delivered to the patients.
Issues With Current Practice • All Registered Nurses conducting admission assessments are not familiar with current NPUAP/CMS Pressure Ulcer Staging Guidelines. • Registered Nurse’s lack of wound care knowledge and training leads to inaccurate staging of pressure ulcers. • Inaccurately staged ulcers, as well as ulcers not identified during the admission assessment, produces inaccurate prevalence data. • Inaccurately staged ulcers can reflect high hospital acquired pressure ulcer rates.
Validation Survey A survey was developed to identify knowledge of nurses about staging of pressure ulcers. Each nurse completing the survey was required to identify & stage the pressure ulcers by observing the images of the ulcers. 50 Registered nurses were randomly selected to complete the survey. The following nurses completed the survey: 32 Registered Nurses with Bachelor of Nursing Degree 5 Registered Nurses with Master of Nursing Degree 1 Registered Nurse with Doctorate Degree 7 Registered Nurses with Associate Degree 5 Registered Nurses with Diploma
Survey PLEASE STAGE THE FOLLOWING PRESSURE ULCERS:
Validation Survey Results • 70% Nurses identified & staged 2 (2/6) pressure ulcers correctly. Stage I & Stage IV • 14% Nurses identified & staged 1 (1/6) pressure ulcer correctly. Stage IV • 8% Nurses identified & staged 3 (3/6) Pressure ulcers correctly. Stage I , Stage II & Stage IV • 4 Certified Wound Care Nurses were also asked to complete the survey and all 4 nurses identified & staged all 6 (6/6) pressure ulcers correctly (100%)
Survey Conclusion • Regardless of experience and educational background, all registered nurses do not have the competence and skill to identify wounds of different etiology, nor pressure ulcers of different stages. • Only registered nurses who receive specialized training in wound care and have experience in wound management and staging pressure ulcers are qualified to properly stage pressure ulcers.
Recommendations • Staff registered nurses to complete client’s skin assessment during the hospital admission process and every 24 hours. • If any skin issues identified other than intact or normal skin, a consult for wound care nurses would be placed. • Wound care nurses will be responsible for identification and management of wounds, staging of pressure ulcers and initiating additional consults for further work up, if necessary such as; Dermatology, Podiatry, Vascular Surgery, General Surgery etc. • Hospital’s Pressure Ulcer Prevalence percentage to be calculated from the assessment note completed by the certified wound care nurses.
Wound Care Nursing According to National Commission For Certifying Agency (NCCA) and the Accreditation Board for Specialty Nursing Certification (ABSNC), Wound Care Nursing is a nursing specialty, and the certification is the validation of knowledge, skills and expertise, which protects the public from unsafe and incompetent providers and distinguishes the healthcare facility for utilizing nurses expert in the management of wounds.
Wound Care Nurses Certified Wound care nurses are key health care team members who: • Accurately assess / stage patients wounds and provide critical documentation. • Implement cost-effective, evidence-based plan of care and develop strategies to prevent complications. • Collaborate with physicians in managing patients with wounds. • Provide education to medical, nursing and ancillary staff. • Educate and advocate for patients and their families.
Wound Care Nurses According to wound care certification board (WOCNCB), entry level Wound Care Nurse must possess following qualification in order to sit for certification exam: • Registered Nursing License • Bachelor’s Degree in Nursing • 1500 Clinical Hours in Wound Care • Completion of a Wound Care Training Program
Why Wound Care Nurses ? • According to some studies certified wound nurses provide safe and high quality care to patients and have a significant impact on the quality of care. • A secondary analysis from 652 hospitals showed that a 10% increase of certified baccalaureate nurses decreased the odds of inpatient 30-day mortality by 2% (Kendall-Gallager,2011).
Why Wound Care Nurses ? • A test of 460 Registered Nurses showed certified wound nurses scored significantly higher on a Pressure Ulcer Knowledge Test than non-certified RNs or RNs certified in other specialties (Zulkowski et al., 2007). • A retrospective analysis (Bolton et al., 2004) revealed that 78.5 percent of those patients treated by a board certified wound care nurse healed in comparison to the 36.3 percent of those treated by non-certified nurses.
Best Practice Model • Based on data collected and review of various studies, it is concluded that patients have improved outcomes when certified wound care nurses are involved in the assessment and treatment of their wounds from admission to discharge. • A change in current practice is required to ensure all patients with pressure ulcers and other wounds are seen by certified wound care nurses, for accurate classification, staging, recommending treatments and monitoring progress of all wounds. In addition,This practice will ensure that patients are receiving the best possible care that will lead to improved patient outcomes.
References • Agency for Health Care Policy and Research (AHCPR), U.S. Department of Health and Human Services, December 1994. Treating pressure sores. Consumer Version Clinical Practice Guideline Number 15 • Agency for Healthcare Research and Quality (2008) National healthcare quality & disparities report. (www.ahrq.gov) • Bolton, L., McNees, P., Van Rijswijk, L., De Leon, J., Lyder, C., Koba, L., (2004). Wound Healing Outcomes Using Standardized Assessment and Care in Clinical Practice. Journal Wound.Ostomy Continence Nursing, 31, 65-71. • Centers for Medicaide and medicare services (2008) Hospital program regulations. http://www.cms.gov/HospitalAcqCond/ • Kendall‐Gallagher, D., Blegen, M. (2009). Competence and Certification of Registered Nurses and Safety of Patients in Intensive Care Units. American Journal of Critical Care. 2009 Mar; 18(2):106‐116.
References • National Pressure Ulcer Advisory Panel (NPUAP) (2007). Pressure Ulcer Staging System Updated. http://www.npuap.org/pr2.htm • Wound, ostomy, and continence certification board (WOCNCB). www.wocncb.org • Zulkowski, K., Ayello E., Wexler, S. (2007). Certification & Education: Do They Affect Pressure Ulcer Knowledge in Nursing. Advance Skin Wound Care. 2007 Jan; 20(1):34‐8.